
- < Previous
Home > Schools & Departments > HE > SOSE > Health Sciences Program > Faculty Publications > 38

Health Sciences Faculty Publications
Stressors and coping strategies in the new normal: a case study of teachers in a higher education setting.
Janine Marie Balajadia , Ateneo de Manila University Maria Micole Veatrizze Dy , Ateneo de Manila University Lukas Pariñas , Ateneo de Manila University Christine Leila Taguba , Ateneo de Manila University Alessandra Grace Tan , Ateneo de Manila University Maxine Therese Tuazon , Ateneo de Manila University Jerome Patrick Uy , Ateneo de Manila University Genejane M. Adarlo , Ateneo de Manila University Follow
Document Type
Conference Proceeding
Publication Date
When governments restricted holding in-person classes to contain the spread of COVID-19, many higher education institutions turned to digital technology to continue the education of their students. This abrupt change in the delivery of teaching and learning posed pedagogical and technological challenges to the teachers. And as governments have gradually allowed the return of students to physical classrooms with the decline in COVID-19 cases and the rollout of vaccines, teachers must adapt once more to a different arrangement for teaching and learning. Using the Job Demands-Resources Model as a theoretical framework, this case study examined the stressors (i.e., job demands) encountered by teachers in a higher education setting as students have returned to physical campuses. It also explored their coping strategies (i.e., job resources) that helped them adjust to the demands of using a different arrangement for teaching and learning in the new normal. Thematic analysis of responses to open-ended questions in a survey of 100 teachers in an institution of Catholic higher education in the Philippines showed demands related to teaching as a job and other competing concerns were brought up as stressors when in-person classes resumed after two years of fully online teaching. It also revealed seeking social support, focusing on teaching and research, and practicing self-care as their ways of coping with the demands of the new normal. Findings from this study can contribute to policies that can cater to faculty development.
Recommended Citation
Balajadia, J. M., Dy, M. M. V., Pariñas, L., Taguba, C. L., Tan, A. G., Tuazon, M. T., Uy, J. P., Adarlo, G. (2023). Stressors and Coping Strategies in the New Normal: A Case Study of Teachers in a Higher Education Setting. In N. Callaos, J. Horne, B. Sánchez, M. Savoie (Eds.), Proceedings of the 17th International Multi-Conference on Society, Cybernetics and Informatics: IMSCI 2023, pp. 92-98. International Institute of Informatics and Cybernetics. https://doi.org/10.54808/IMSCI2023.01.92
Since February 28, 2024
Advanced Search
- Notify me via email or RSS
- Collections
- Libraries & Archives
- Ateneo Journals
- Disciplines
Author Corner
- Why contribute?
- Getting started
- Working with publishers and Open Access
- Copyright and intellectual property
- Contibutor FAQ
About Archium
- License agreement
- University website
- University libraries
Home About Help My Account Accessibility Statement
Privacy & Data Protection Copyright
Advertisement
A Qualitative Study of How Adolescents’ Use of Coping Strategies and Support Varies in Line With Their Experiences of Adversity
- Original Paper
- Open access
- Published: 01 March 2022
- Volume 52 , pages 177–203, ( 2023 )
Cite this article
You have full access to this open access article

- Emily Stapley ORCID: orcid.org/0000-0003-2935-4438 1 ,
- Sarah Stock 1 ,
- Jessica Deighton 1 &
- Ola Demkowicz 2
8378 Accesses
7 Citations
8 Altmetric
Explore all metrics
Adolescence is associated with a rise in the incidence of mental health issues. Thus, the factors, processes, and contexts that protect and promote positive mental health in adolescence are of key interest to policymakers.
Our aim was twofold: First, to explore the coping strategies and sources of support that adolescents identify as protective (or not) in the face of difficulty over a three-year period; second, to examine how and why this may vary in line with the levels of adversity that they report experiencing in life.
Participants were attending schools in England implementing a mental health prevention programme called HeadStart. 93 semi-structured interviews were conducted with 31 adolescents (age 11–12 at the outset of the study; 58% female) once per year over three years. The interviews were analysed using thematic analysis.
Six coping strategy themes (e.g., ‘Disengaging from problems’) and five support themes (e.g., ‘Parents as a source of comfort and advice’) were derived from the interviews. The types, quality, and consistency of reported coping strategies and support varied in line with whether adolescents were experiencing higher or lower levels of adversity in life over time, and according to the resources that they had available within their physical and social contexts.
Conclusions
Our findings underscore the importance for mental health prevention programmes of bolstering both individual-level coping strategies and the resources available within adolescents’ environments to help them to manage adversity.
Similar content being viewed by others

Resilience in adolescence during the COVID-19 crisis in Canada

SALaMA study protocol: a mixed methods study to explore mental health and psychosocial support for conflict-affected youth in Detroit, Michigan
An exploratory mixed-method descriptive analysis of youth coping during the first wave of the covid-19 pandemic in quebec.
Avoid common mistakes on your manuscript.
Adolescence is a period of major life change, characterised by physical transformations, psychological and cognitive development, and changes to peer and family relationships (Blakemore, 2012 ). Adolescence is also associated with a rise in the incidence of mental health issues, with the latest statistics in the UK indicating that among 11- to 16-year-olds, 17.6% had a diagnosable mental disorder in 2020, as compared to 14.4% of 5- to 10-year-olds (Vizard et al., 2020 ). It has been calculated that the cost of ‘late intervention’ to combat the problems that young people experience, such as mental disorders, is nearly £17 billion (Chowdry & Fitzsimons, 2016 ). Therefore, developing effective early intervention programmes, and ascertaining the factors, processes, and contexts that protect and promote adolescent wellbeing and positive mental health, is of key interest for policymakers seeking to prevent the onset of mental health issues in adolescence.
Researchers have distinguished between protective factors, which are associated with positive outcomes in the face of risk and adversity, and promotive factors, which are associated with positive outcomes generally (Masten & Barnes, 2018 ). The study of such factors features prominently in research seeking to explain why some individuals show resilience in the face of trauma, adversity, and risk, whereas others show poorer outcomes (e.g., Luthar, 2015 ; Masten & Barnes, 2018 ). Resilience can be broadly defined as the complex and dynamic process of adaptation to adversity (Luthar, Cicchetti, & Becker, 2000 ; Masten, 2014 ; Ungar, 2012 ), though we note that there are various subtleties and variations in how resilience can be understood (for an overview, see Southwick, Bonanno, Masten, Panter-Brick, & Yehuda, 2014 ).
Recent theory and research in this area has increasingly focused upon the embedded nature of resilience, whereby adaptation is facilitated through interactions between the individual and aspects of their ecological environment. For example, Ungar ( 2008 ) has defined resilience as a process whereby individuals navigate towards the resources to sustain their wellbeing that are available to them within their physical and social contexts. Thus, rather than putting the onus solely on the individual’s ability to cope, this definition underscores the role of both the individual and their environment in promoting wellbeing (Ungar, Brown, Liebenberg, Cheung, & Levine, 2008 ). Similarly, Masten ( 2021 ), advocating for a systemic perspective on resilience, has argued that the degree to which young people are able to respond adaptively in the face of disaster depends on the resilience of the interconnected systems around them, including family, school, community, and policy. Such definitions are underpinned by Bronfenbrenner’s ( 1979 ) ecological systems theory, which emphasises the role in child development of the child’s interaction with the interrelated, nested systems around them (Ungar, Ghazinour, & Richter, 2013 ).
Following early pioneers in the study of resilience (e.g., Garmezy, 1974 , 1985 ), researchers have tended to distinguish between three broad categories of protective factors: individual factors, such as effective coping skills or high self-esteem; family factors, such as a positive caregiver-child relationship or family climate; and environmental or community factors, such as prosocial peers or a positive school environment (e.g., Eriksson, Cater, Andershed, & Andershed, 2010 ; Fritz, de Graaff, Caisley, van Harmelen, & Wilkinson, 2018 ; Olsson, Bond, Burns, Vella-Brodrick, & Sawyer, 2003 ). Thus, the concepts of coping and social support have prominence within the study of protective factors. Coping can be defined as the “constantly changing cognitive and behavioral efforts to manage specific external and/or internal demands that are appraised as taxing or exceeding the resources of the person” (Lazarus & Folkman, 1984 , p.141), and social support as the resources that the individual’s social network provides to help them to handle difficulties (Cohen, 2004 ).
Research investigating protective factors has often been quantitative in design. For instance, numerous studies have examined what factors protect young people in the face of adversity (e.g., Askeland et al., 2020 ; Eriksson et al., 2010 ), which factors reduce the likelihood of young people developing mental health issues (e.g., Fritz et al., 2018 ; Fritz, Stochl, Goodyer, van Harmelen, & Wilkinson, 2020 ), which factors predict resilience following trauma (e.g., Lai, Lewis, Livings, La Greca, & Esnard, 2017 ; Masten, 2021 ), and in what ways the impact of protective factors varies by the level of adversity experienced (e.g., Bowen, Lee, & Weller, 2007 ; Kassis, Artz, Scambor, Scambor, & Moldenhauer, 2013 ). However, quantitative research in this area has been criticised for its lack of attention to how, why, and when particular factors, or combinations of factors, may be more or less protective for young people from their own perspectives and in their own words (Eriksson et al., 2010 ; Ungar, 2003 ). Qualitative research designs are well suited for answering such questions, including offering greater nuance in understanding the complex protective processes that are ecologically embedded within each individual’s world.
Previous qualitative studies have explored young people’s identification of the protective factors and processes that contribute to resilience in the context of academic attainment (e.g., Chee, 2019 ; Morales, 2008 ), economic disadvantage (Smokowski & Reynolds, 1999 ), and specific mental health difficulties (e.g., Everall, Altrows, & Paulson, 2006 ; Las Hayas et al., 2016 ), as well as young people’s ways of coping with adversity or stress in daily life (e.g., Stapley, Demkowicz, Eisenstadt, Wolpert, & Deighton, 2020a ; Ungar et al., 2008 ). For example, through interviews with 13 young adults in Canada who overcame suicidality in adolescence, Everall et al. ( 2006 ) identified four domains of resilience: (a) social processes - having consistent, supportive relationships with others (such as family members, peers, teachers, and professionals); (b) emotional processes - being aware of and able to express feelings; (c) cognitive processes - gaining new perspectives and having a sense of control; and (d) taking action with purpose and specific goals in mind. In another Canadian study, Ungar et al. ( 2008 ) identified seven experiences that 19 adolescents described as enhancing their mental health, which they each had varying access to within their environments: material resources; supportive relationships; a desirable sense of self; a sense of power and control; cultural traditions; a meaningful role within the community; and feeling part of something bigger.
By illuminating protective factors and processes, and exploring how and why they may vary by context, resources, or the level of adversity experienced, qualitative research findings can inform the development of interventions seeking to bolster young people’s resilience and prevent the onset of mental health issues (Eriksson et al., 2010 ; Luthar, 2015 ). For instance, Ungar, Hadfield, and Ikeda ( 2018 ) interviewed 85 adolescents in Canada, who had different levels of exposure to risk and varying access to resilience-promoting resources (e.g., a supportive adult), about their experiences of service use. They found that adolescents at higher risk and with low resilience voiced a preference for professional support with more relaxed boundaries, such as contact outside of official therapy time, implying that this type of therapeutic relationship may be a protective factor for these adolescents (Ungar et al., 2018 ). On the other hand, adolescents with high resilience and at low risk described less need for professional support in general due to the social capital that they already had in their lives, implying that the social support networks that these adolescents already have access to may be protective enough without additional therapeutic support (Ungar et al., 2018 ).
Given the rising rates of mental health issues among adolescents in the UK (Vizard et al., 2020 ), recent UK government policy has moved towards schools being key sites from which to deliver interventions to promote wellbeing and prevent the onset of mental health issues (Department of Health and Social Care & Department for Education, 2018 ). The significant proportion of time that young people spend in school means that schools can reach a much wider range of young people than clinical services and can overcome barriers associated with attending clinical services, such as travel, timing, and cost issues (Masia-Warner, Nangle, & Hansen, 2006 ). As studies of resilience are inevitably contextually situated because what is experienced as protective in one context may not be available or seen as adaptive in another (Ungar, 2008 ), there is a need for qualitative research specifically in a UK context to explore the factors and processes that young people find to be protective in the face of difficulties in life, including how, why, and in what circumstances these may vary. Such findings can then be used to inform the development of effective school-based prevention and early intervention programmes to meet a range of needs.
Consequently, in the current study, we sought to build on existing understanding in this area by taking a qualitative approach to inquiry and exploring the factors, processes, and contexts (with a focus on the concepts of coping and social support) that are deemed protective from adolescents’ own perspectives and in their own words, within the setting of a school-based mental health prevention programme in the UK. Specifically, our study sought to address the following aims using qualitative methods: (1) To explore the coping strategies and sources of support that adolescents identify as protective (or not) in the face of difficult situations and feelings over a three-year period; (2) To examine how and why this may vary in line with the levels of adversity that they report experiencing in life.
Research Design
We used an interpretive, qualitative research design to explore, through semi-structured interviews, young people’s lived experiences of and perspectives on problems and difficulties in daily life, coping strategies, and accessing or receiving support both from formal sources, including professionals, and informal sources, including family and friends. Our analysis primarily draws on Braun and Clarke’s ( 2006 , 2021 ) guidance for conducting thematic analysis and is underpinned by a critical realist epistemological perspective. This takes the view that while there is a real world that exists independently of our perceptions and constructions of it, our understanding of it is a construction from our own point of view (Maxwell, 2010 ). This means that we see our analysis of the data as being an interpretation of participants’ reality, which we have constructed from our own perspectives, contexts, and views of the world. We are experienced researchers in the child and adolescent mental health research field, currently working in the context of evaluating interventions seeking to enhance young people’s resilience, mental health, and wellbeing, to learn about what helps to manage and prevent mental health difficulties.
Setting for the Study
HeadStart is a six-year, school-based, mental health prevention programme, which launched in 2016 in six local authorities in England. The aim of HeadStart is to promote resilience, wellbeing, and positive mental health through the delivery of a range of preventive and early intervention approaches seeking to boost young people’s coping strategies and environmental resources (Evidence Based Practice Unit, 2018 , 2019 ). A five-year qualitative longitudinal study is being conducted to explore young people’s experiences of HeadStart and, in doing so, examine the role and place of HeadStart more broadly within young people’s perspectives on coping and receiving support. Young people were invited to take part in the study by school staff or HeadStart staff if they had already received support from HeadStart by the first timepoint of the study or if they were identified as likely to receive it in future. To date, 82 interviews with the same cohort of young people have been conducted at Time 1 (2017 or 2018), 78 at Time 2 (2018 or 2019), and 55 at Time 3 (2019). Data collection in 2020 (Times 3 and 4) was paused due to Covid-19 restrictions.
Ethical Considerations
Ethical approval for this study was granted by the University College London (UCL) Research Ethics Committee (ID number 7963/002). As all participants were under the age of 16, written informed consent was sought from the young people’s parents/carers and written assent to take part and for the publication of their anonymised data was sought from the young people at the outset of the study. It was made clear in study information sheets that participation was voluntary, and that participants could withdraw at any time without consequence. Participants received a £10 voucher after each interview as a thank you for taking part. To protect participant confidentiality, interview transcripts were anonymised (e.g., with names of people and places removed).
Participants
A subsample of 31 participants from the wider qualitative longitudinal study sample was selected for inclusion in the present study. The subsample represented nine secondary schools across four of the HeadStart areas. Demographic information about the subsample can be seen in Table 1 . All 31 participants had taken part in Time 1, 2 and 3 interviews, yielding a total subset of 93 interviews. 25 participants from the wider study sample were excluded from the subsample as they were missing interviews at Time 2 or 3. Given our study’s focus on adversity, 14 participants were excluded because they did not discuss coping strategies and support in the context of experiencing any mental health difficulties, family strain, or bullying, nor did they not report receiving any targeted support from HeadStart at Time 1. Targeted (indicated or selective) support is offered to select students, including those with mild or subclinical symptoms of a mental disorder or those with experience of particular risk factors, such as parental mental health issues (Campbell, 2004 ; Werner-Seidler, Perry, Calear, Newby, & Christensen, 2017 ). 12 participants from one HeadStart area were excluded because they were up to two years younger (age 9–10 years) than the majority of the young people (age 11–12 years) at Time 1, thus they did not align with our study’s focus on adolescence.
Data Collection
The interviews were conducted by four members of the research team (including the first and last authors). The interviews took place in a private room at participants’ schools. Where possible, the same researcher interviewed each participant at all three timepoints. All interviews were audio recorded and transcribed verbatim. The interviews in our subsample ranged in length from 20.47 to 60.05 min at Time 1 ( M = 40.3, SD = 9.86), 21.39 to 68.43 min at Time 2 ( M = 38.05, SD = 12.95), and 22.55 to 63.23 min at Time 3 ( M = 41.83, SD = 11.16).
The interview schedule developed by the research team was semi-structured, which meant that while there were core questions asked by the researcher in each interview, the conversation around these key areas was led by participants’ responses. Core interview questions asked about participants’ experiences of and perspectives on coping with problems and difficult situations or feelings in life, including strategies that they drew on and social and professional support that they accessed (and their opinions on this). At Times 2 and 3, the interview schedule also asked about any changes over time in relation to topics raised previously. For example, ‘You mentioned when I met with you last year that you were having arguments with your friends, how are your friendships this year?’.
Reflexivity
Reflexivity is a means for the researcher to critically engage with their role in the research process, including remaining self-aware and cognizant of their own influence on the research and in turn how the research may be affecting them (Probst, 2015 ). The research team designed an interview reflection tool to facilitate interviewers in debriefing following each interview. Reflections were audio-recorded and discussed further with the research team lead (the first author) when the interviewer deemed this to be helpful. The intention was to provide a space for interviewers to offload their immediate thoughts and feelings following each interview, and to encourage them to develop their interview skills through reflecting on their technique in each interview.
We reflect that our approach to data collection and analysis is inevitably influenced by our own understanding and experiences of the research area. For instance, our approach to asking young people about their experiences of coping and support was influenced by our theoretical grounding as researchers within systemic theories of resilience. Thus, in each interview, we specifically explored young people’s experiences within the context of key systems, including family, peers, and school. We also recognise that our approach to data collection and analysis is influenced and limited by our own understanding and experiences of the world, including sociodemographic differences between ourselves and the young people, such as in terms of age, ethnicity, and gender identity. For example, the age gap between ourselves and participants, in conjunction with the interviews taking place on school premises, could have reinforced hierarchical structures inherent in schools (Ozer, Newlan, Douglas, & Hubbard, 2013 ), and thus inhibited participants from speaking openly in their interviews about their experiences and opinions. Therefore, we endeavoured at each interview to establish a secure, non-hierarchical space for the young people to speak to us in, emphasising confidentiality (unless any safeguarding issues arose), young people’s right to withdraw at any time, and that there were no right or wrong answers. Our interview schedules were also developed in conjunction with young people to ensure that the questions were meaningful to and understood by our target audience.
Data Analysis
To address our study aims, our analysis sought to answer two research questions sequentially: (1) What helps adolescents to manage difficult situations and feelings over a three-year period? (2) How does ‘what helps’ vary depending on the level of adversity that adolescents report experiencing in their lives over time?
To answer the first research question, a hybrid deductive/inductive thematic analysis was conducted by the first and second authors using NVivo (version 12) to identify the coping strategies and sources of support that participants reported drawing on at Times 1, 2, and 3. An existing thematic framework of young people’s coping behaviour was used to facilitate this, which was derived through an earlier inductive thematic analysis, guided by Braun and Clarke’s ( 2006 ) methodology, of all 82 interviews conducted at Time 1 with the young people taking part in the wider qualitative longitudinal study (see Stapley et al., 2020a ). The framework consisted of the following main themes: Activities and strategies; Disengaging from problems; Standing up for yourself; Acceptance of problems; Social support; HeadStart support; Other professional support; Hiding feelings or problems (Stapley et al., 2020a ).
We used this existing framework to guide our coding of the interviews in the present study, but also renamed and restructured themes, and created new themes, as necessary to best reflect the Time 1, 2, and 3 interview data. The coding process involved collating relevant transcript extracts under each theme. For instance, a new subtheme of ‘Support from boyfriends or girlfriends’ was developed from coding participants’ Time 2 and 3 interviews and included within a new main theme of ‘Support from close and trustworthy friends’. ‘Hiding feelings or problems’ ceased to be a main theme in the present study, as it became apparent when exploring the data across all three timepoints that this was typically spoken about in relation to particular groups of people, principally parents, friends, and school staff. Thus, in our study, participants’ references to finding it difficult to talk to or hiding problems or feelings from others have been captured as relevant when describing their experiences and perceptions of support from these groups.
To answer the second research question, an inductive thematic analysis was conducted, again by the first and second authors using NVivo (version 12), guided by the six steps outlined by Braun and Clarke ( 2006 , 2021 ): becoming familiarised with the data; systematically coding the data or applying descriptive labels to transcript extracts; collating similar codes (labels) to generate initial themes; developing and reviewing themes; refining and giving names and definitions to themes; and the report. The interviews were re-coded in NVivo to develop new themes, which this time delineated the difficult situations and feelings that participants reported experiencing at Times 1, 2, and 3.
Braun and Clarke ( 2021 ) take a reflexive approach to thematic analysis, which can be distinguished from codebook or coding reliability approaches to thematic analysis. We view our analysis as primarily reflexive, but at times reflecting elements more akin to a codebook approach. Our use of an existing thematic framework, for example, when answering our first research question perhaps more closely reflects a codebook approach, whereby the themes were developed using the Time 1 dataset and then used to guide our analysis of the Time 2 and 3 datasets, with refinements made as necessary in light of new data. By contrast, the analysis process for our second research question took an entirely open and bottom-up approach to both coding and theme development, which aligns more closely with a reflexive approach.
The first and second authors worked together throughout the analysis for both research questions to code the data and develop themes, using a collaborative approach to facilitate rich, in-depth engagement with the data (Braun & Clarke, 2019 ), and to ensure that our interpretations remained grounded within the data. However, we did not seek to assess interrater reliability during our analysis, thus our analysis was not aligned with a coding reliability approach to thematic analysis. This is because, in line with Braun and Clarke’s ( 2021 ) reflexive approach, we view researcher subjectivity as a “resource for knowledge production which inevitably sculpts the knowledge produced, rather than a must-be-contained threat to credibility” (p. 334–335), thus interrater reliability is not seen as a marker for quality of analysis.
Braun and Clarke ( 2021 ) also distinguish between themes defined as patterns of shared meaning organised by a central concept, which is a core part of their reflexive approach, and themes defined as summaries of participant responses in relation to particular topics within the data, which is more aligned with a codebook approach. Researchers taking a reflexive approach to thematic analysis need to justify their use of the latter (Braun & Clarke, 2021 ). Due to the large volume of data that we were working with and our aim of drawing relatively broad, concrete comparisons between groups of participants, we reflect that some of our themes align more closely with what Braun and Clarke ( 2021 ) describe as ‘shared-topic’ themes (e.g., ‘Varying trajectories of HeadStart and other professional support’), rather than ‘shared-meaning’ themes (e.g., ‘Disengaging from difficulties’).
As the final step in our analysis, by examining the transcript content coded to each theme delineating the difficult situations and feelings that each participant reported experiencing at each timepoint, participants were then divided into three groups by the first and second authors, each representing a different level of adversity. The three groups were: Group A - participants who reported that their levels of difficulty in life had improved or were manageable by Time 3; Group B - participants who reported experiencing some ongoing difficulties and some areas of improvement by Time 3; Group C – participants who reported that their levels of difficulty had deteriorated or were hard to manage by Time 3. The authors initially separately allocated each participant to one of the three groups and then checked each other’s allocations, with discussion of any instances of disagreement until agreement was reached.
Table 2 ; Fig. 1 show the difficult situations and feelings reported by participants in each of the three groups at any timepoint.
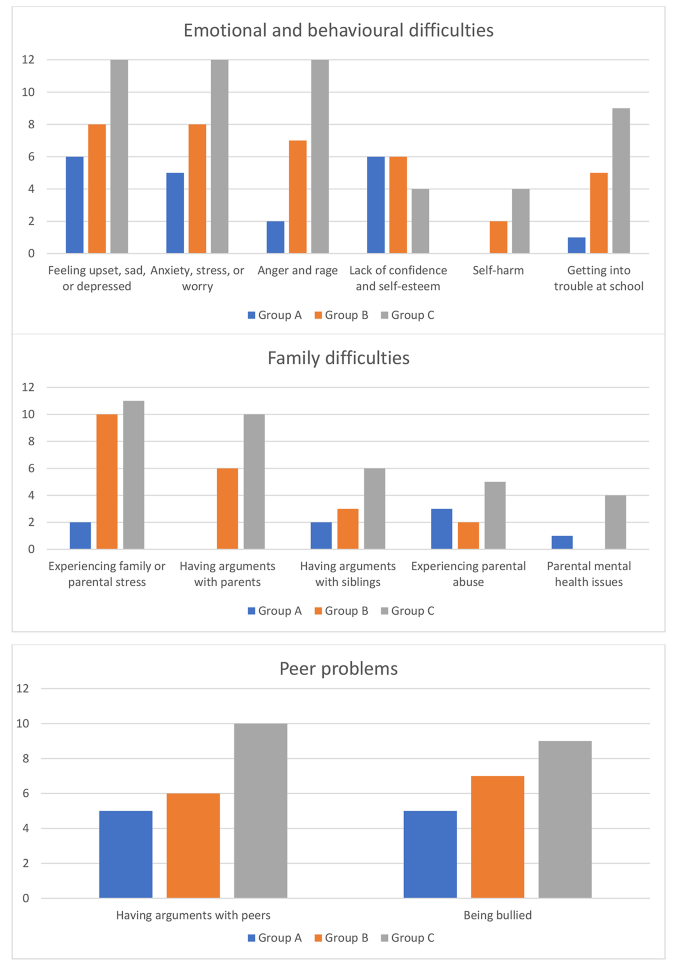
Frequencies ( N ) of participants in each group who reported experiencing particular difficult situations and feelings at any timepoint
As can be seen in Table 2 ; Fig. 1 , comparatively high proportions of participants across the three groups reported experiencing feelings of sadness and anxiety, as well as experiences of being bullied at any timepoint. However, Group C contained the highest proportions of participants who reported experiencing difficulties with anger, self-harm, arguments with parents and/or siblings, parental abuse, parental mental health issues (such as depression), getting into trouble at school, and arguments with peers. By contrast, the highest proportion of participants who reported lacking in confidence and self-esteem could be seen in Group A. Groups B and C contained the highest proportions of participants who reported experiencing some form of family or parental stress (such as animosity between parents or family financial difficulties) at any timepoint.
Table 3 ; Fig. 2 present the coping strategies and sources of support (organised in terms of individual-, family-, and environment-level protective factors and processes) that participants across the three groups reported drawing on at two or more timepoints to manage difficulties in life. Reports at two or more timepoints was considered a proxy for participants’ consistency in usage of specific coping strategies and sources of support over time. Previous quantitative longitudinal research has identified stability in adolescents’ reports of using particular coping strategies over at least a two-year period (Valiente, Eisenberg, Fabes, Spinrad, & Sulik, 2015 ).
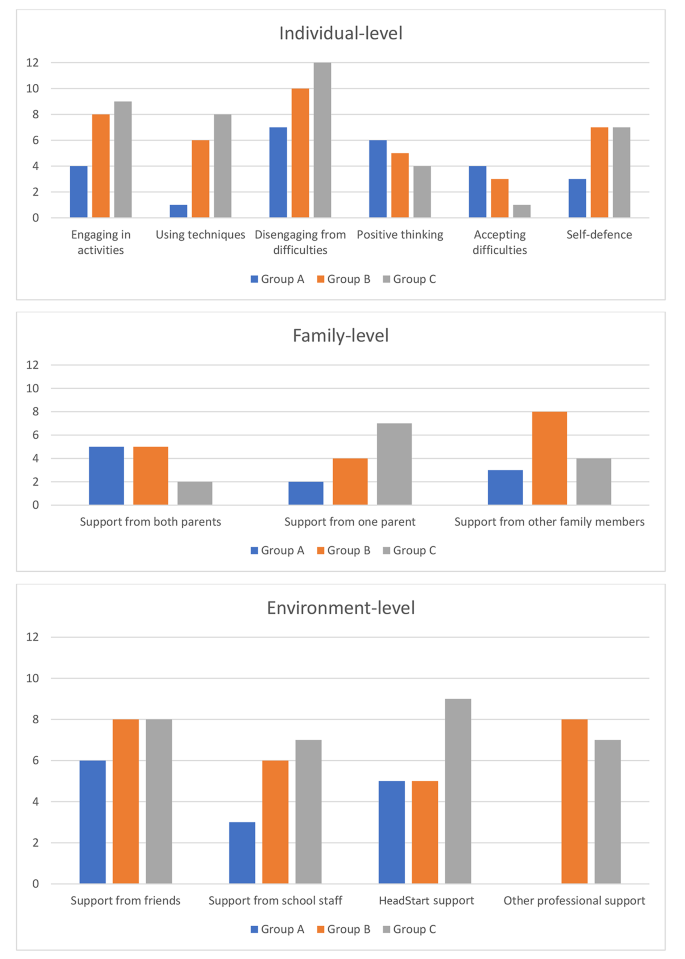
Frequencies ( N ) of participants in each group who reported drawing on particular coping strategies and sources of support at two or more timepoints. (Note. Current or historic targeted support received from HeadStart or other professionals (e.g., CAMHS is shown as reported at any timepoint by participants)
Individual-level Factors and Processes
Engaging in activities.
Participants described engaging in different activities (e.g., playing video games, drawing, and playing football) to take their mind off their problems, have fun, or relax: “When I’m thinking about the worries and when I’m, like, drawing, it’s, like, makes me a lot, like, do you know, thinking about the worries, it makes them go somewhere else” (Group A, Time 2). The prevalence of this theme, in terms of references at two or more timepoints, was higher in Groups B (73%) and C (75%) than Group A (50%).
However, participants in Groups B and C also reported that engaging in activities did not always help. Reasons for this included that some problems (such as a grandparent dying) can make you feel so sad that engaging in an activity does not help, some activities (e.g., boxing) can make you feel angrier instead of calmer, and some activities (e.g., eating comfort food) are not necessarily good for you: “I realised me doing boxing has made me more angry and then, then when people are annoying me, then I know that I have the power to do something” (Group C, Time 3).
Using Techniques
Participants described using different techniques or specific strategies (e.g., deep breathing techniques, stress balls, and counting to 10), sometimes suggested by a professional, to try to regulate their emotions: “ When I was clicking my fingers I always… I just, when I got nervous or I got angry or something like that, I feel like that calmed me down” (Group C, Time 3). The prevalence of this theme, in terms of references at two or more timepoints, was higher in Groups B (55%) and C (67%) than Group A ( N = 13%).
Yet, participants in Groups B and C also reported limitations in the efficacy of strategies, such as forgetting to take deep breaths to manage their anger in the heat of the moment. Participants in Groups B (18%) and C (33%) also mentioned engaging in self-harm as a coping strategy at various points in their lives. However, self-harm was only identified as a current coping strategy by the third timepoint by participants in Group C: “[My sister] just tells me I’m an idiot, (chuckles) and I need to stop doing it” (Group C, Time 3).
Disengaging from Difficulties
Almost all participants across the three groups described instances at two or more timepoints when they had dealt with problems by deliberately disengaging from them, such as through distracting themselves, forgetting problems, choosing to put problems out of their mind, or ignoring the existence of problems and individuals who were upsetting them (e.g., bullies): “I just try my best to not listen to them and just ignore them” (Group A, Time 2).
Positive Thinking
Participants described engaging in positive thinking in the face of difficulty, including trying to see the positive side of difficult situations, thinking positive thoughts to cheer themselves up, and persevering and not giving up: “Make something happy out of it or just think about generally something that makes you happy and then like… sort of like post the angry feelings out with the happy feelings” (Group B, Time 1). The prevalence of this theme, in terms of references at two or more timepoints, was highest in Group A (75%), as compared to Groups B (45%) and C (33%).
Accepting Difficulties
Participants described how over time they had become used to difficult situations or had simply accepted the existence of particular aspects of life that they found hard, which could eventually make such situations less stressful and easier to handle: “I was really shy, and like, I was scared to talk to other people, I kind of got used to it and, like, I’m not as shy anymore” (Group A, Time 3). This theme also included participants’ references to waiting for problems or difficult feelings to pass or ‘blow over’. The prevalence of this theme, in terms of references at two or more timepoints, was higher in Groups A (50%) and B (27%) than Group C ( N = 8%).
Self-defence
Participants described situations (principally arguments with friends, family members, or teachers) at two or more timepoints that in their view required them to challenge unwanted behaviour from others or defend themselves (verbally or physically): “I ain’t just going to stand there and have everyone call me a wimp when they hit me, and I don’t hit them back. I’m just going to stand there and hit them back” (Group B, Time 1). The prevalence of this theme was higher in Groups B (64%) and C (58%) than Group A (38%).
Family-level Factors and Processes
Parents as a source of comfort and advice.
Participants in Group A often referred to both of their parents (63%) as being a supportive presence in their lives: “The first people I would go to are my parents if there was a problem. Which is really good, and they would give me their honest opinion” (Group A, Time 2). This included feeling able to and wanting to talk to their parents about their problems, with reference to their parents making them feel better, giving them advice, or helping them to see another perspective or reach a solution. Similarly, 45% of participants in Group B described both of their parents, at two or more timepoints, as being a source of support, comfort, and advice in difficult situations. A higher proportion of participants in Group C identified one of their parents (58%), usually their mother, as being a supportive presence in their lives, as opposed to both parents (17%). This parent was described as being a source of advice and comfort.
Parents at Arms-length
Only a minority (25%) of Group A participants perceived one parent as being a more prominent source of support than the other at two or more timepoints. Both of these participants self-identified as female and described feeling more able to talk to their mothers about problems than their fathers, who they felt may not understand their problems to the same degree that their mothers would: “If it’s to do with girls or problems at school, I probably wouldn’t necessarily speak to [my dad] about it but sometimes, I do” (Group A, Time 2). Similarly, participants in Group B (36%) who described one parent as being a more prominent source of support than the other indicated that they had a closer relationship with one parent (usually their mother). By contrast, the other parent for participants in Group C was often seen as being a source of difficulty in their lives or as less available to talk to (such as because they were busy or they did not live with them), and so was considered to be a less suitable source of support for these reasons.
Participants in Group B also described instances of not always feeling able to, not always wanting to, or hesitating to talk to their parents about their problems. For instance, if they thought that they might worry or upset their parents, if their parents were not available to talk to, if they thought that a problem was not major enough to warrant talking to their parents about, or if, in general, they preferred trying to resolve problems on their own first. Similarly, participants in Group C described finding it hard to speak to their parents about some issues, such as feeling sad or having low self-esteem, because, for example, they felt that their parents did not understand what they were going through.
My mum is always like, ‘Toughen up’. I literally can’t and like I don’t know what to say to my mum when she says to me, ‘Toughen up’, when she’s like, ‘You need to stop crying, you need to grow up’, and I don’t know if I can. (Group C, Time 3)
Other Family Members as a Supportive Presence
Participants also described drawing on support from other members of their families. The prevalence of this theme, in terms of references at two or more timepoints, was higher in Group B (73%) than Groups A (38%) and C (33%). There were participants in all three groups who saw their siblings (and also, in a small number of cases, their cousins) as ‘having their back’ and as being someone to talk to about problems and seek advice from because, for example, they had had similar experiences to each other: “If there’s any problems with me, like, s- I, I could talk to [my sister]. And like, she’ll listen. Like, I’ll, I can trust her […] she won’t, like, tell my mum if I don’t want her to” (Group B, Time 2). In terms of support from extended family, participants across the three groups most often referred to their grandmother as a source of support, describing them as another person to talk to about problems and seek advice from, in the absence of or in addition to parental support. Participants in Groups B and C also described their pets as being a source of comfort and as cheering them up when they were feeling sad, worried, or angry.
Environment-level Factors and Processes
Support from close and trustworthy friends.
Similar proportions of participants across Groups A (75%), B (73%), and C (67%) described at two or more timepoints how their friends (including, for a minority, boyfriends or girlfriends) were a source of support in times of difficulty. Friends were referred to as cheering you up, standing up for you in arguments or against bullies, and being someone to talk to and receive relatable advice from, for example for problems that your parents would not understand. However, while trust in family members was more implicit, there were participants across all three groups who mentioned having specific or close friends whom they trusted more than others to keep their problems confidential: “I have one friend […] she’s like really… we talk about everything. When I told, when I say something to her, it then doesn’t come out anyone’s mouth” (Group B, Time 3).
School Staff as a Double-edged Sword
Higher proportions of participants in Groups B (55%) and C (58%), as compared to Group A (38%), reported drawing on or being given support, when needed, from school staff (teachers and/or pastoral care staff) at two or more timepoints. Participants in Group A primarily described school staff as mediating in situations of bullying or arguments with peers, and felt that particular school staff members were supportive or were there for them to talk to if they needed to. However, Group A participants also reported that generally they felt more comfortable seeking support from family and friends, although they would consider talking to a school staff member if a problem was really serious: “If we’re talking about like school, no, not really, because um I just feel like that’s, that’s not what I do, that’s not how I deal with things. Like, I, I, I’d rather go to my friends or my mum” (Group A, Time 3).
Participants in Group B similarly described school staff as intervening in difficult situations with peers, and also described seeking support from specific school staff members if they were upset or if they wanted someone to talk to. However, Group B participants also mentioned times when school staff had not always been able to provide effective support. For instance, school staff were not always available to talk to about problems, they did not always listen or take action, or they could not always be trusted to keep problems confidential. Talking to a teacher about issues with peers could also result in you being labelled as a ‘snitch’, which was not helpful: “If I do tell on the people who do it, they w- they will A, start calling me a snitch, and B, start making fun of [me] even more” (Group B, Time 1).
Participants in Group C described having arguments with and feeling blamed by teachers, but also described instances when they had been given support by particular members of school staff, including seeing them as someone to speak to about difficult family situations, bullying, or managing anger. However, Group C participants also described times when they had struggled to trust school staff, including having an awareness that there may be consequences of speaking to school staff (such as an investigation happening), worries about teachers forming an opinion of you, and experiences of or anticipation of not feeling understood by school staff: “I find it a bit difficult to tell teachers because I know that their policy is obviously they can’t tell pupils, but they can tell like people if it’s a major problem like anyone [is] in danger” (Group C, Time 3).
Varying Trajectories of HeadStart and Other Professional Support
Group C contained the highest proportion of participants who reported receiving targeted support from HeadStart at any timepoint (75%), followed by Group A (63%) and Group B (45%). On the other hand, Group B contained the highest proportion of participants who reported receiving current or historic support from other professionals (outside of HeadStart) at any timepoint (73%), followed by Group C (58%) and Group A ( N = 0).
At Time 1, four participants in Group A reported meeting with a peer mentor (an older student at school). They described the positive impact of this type of HeadStart support, including learning coping strategies, having someone relatable to talk to, and boosting their confidence. At Time 2, none of these participants reported still being in receipt of peer mentoring. Three had been offered additional HeadStart support (such as involvement in co-producing their area’s programme). However, one had decided not to take part as none of her friends had signed up this year, another’s support had stopped because of school staff strikes, and the other participant’s support had never begun. One participant in Group A mentioned receiving HeadStart support for the first time at Time 2 (counselling). At Time 3, no participants in Group A reported receiving any HeadStart support: “I just stopped it because I didn’t think I’d need it anymore” (Group A, Time 3).
At Time 1, four participants in Group B reported receiving HeadStart support, including one-to-one (peer mentoring or counselling) and small group-based support (psychoeducational sessions or co-production meetings). They described receiving useful advice about coping with being bullied and handling difficult feelings (such as anger and anxiety), enjoying being involved in HeadStart, and finding it helpful to have someone to speak to about their worries.
They give some really good ad- advice, like when we was learning about worrying and stress, there was like some stuff that we can do to like help deal with that, and then things that we do, like, that are maybe bad and like how we can stop that like happening, and like a better way to cope with it. (Group B, Time 1)
At Times 2 and 3, only one participant in Group B was still receiving HeadStart support. This participant reported feeling more confident and less anxious as a result, but also felt that some of their group sessions had been disrupted by other students misbehaving. Two participants in Group B did not feel at Times 2 and 3 that they needed support from HeadStart anymore, as they were feeling better. However, two other participants (one of whom also described receiving ongoing support from a professional at CAMHS to manage her anxiety across Times 1, 2, and 3, and the other of whom mentioned seeing a school counsellor at Time 2) stated that they would like to receive support from HeadStart again at Time 2. One of these participants still felt the same at Time 3, whereas the other felt that they did not need any support from HeadStart by Time 3.
Two participants did not report receiving support from HeadStart at any timepoint, but did mention taking medication to manage attention deficit hyperactivity disorder (ADHD) across Times 1, 2, and 3. Five participants also described historic contact with social services, counselling, and/or therapy to manage such issues as school-related stress or difficult family situations. Four of these participants identified aspects of this support that had been unhelpful, such as finding it boring, finding it hard to talk about difficult feelings or situations, or having their trust betrayed. Only one of these participants stated that his therapy had had a positive impact on his levels of worry and stress at the time. However, he also said that he would not necessarily want to receive therapy again.
Nobody wants to be the person who’s, like, gone to therapy three years in a row. And um ‘cause I don’t want to miss school as well because last time I had to go to therapy I, I, I missed a lot of school. (Group B, Time 2)
At Time 1, five participants in Group C reported receiving one-to-one (peer mentoring) or small group-based HeadStart support (psychoeducational sessions or co-production meetings). Participants described getting things off their chests through talking to others about their problems, and learning how to manage their worries and anger. One of these participants also reported receiving ongoing small group and one-to-one support from HeadStart support workers across Times 2 and 3. However, the other four participants reported no longer receiving HeadStart support at Time 2 because it had ended or because they had not found it helpful.
Of the latter four participants, one participant did not report receiving any HeadStart support at Time 3 either. Another reported receiving HeadStart support again at Time 3 in the form of co-production meetings, as well as having contact with social care and a school counsellor, which he described as limited in its utility. The remaining two participants described receiving support from statutory CAMHS, social care, and/or a counsellor instead of HeadStart at Time 2. Both felt that this support was more helpful. By Time 3, one of these participants was still receiving ongoing counselling, and the other had stopped receiving support from statutory CAMHS, but had been referred to another form of small group-based HeadStart support at school.
Why do you think the CAMHS course has been more helpful than [HeadStart]? They explained it more in detail and like, I don’t know. Talking to like other people with ADHD and stuff and I found than better than. ‘Cause like not really much people has ADHD in this school. (Group C, Time 2)
Two participants in Group C reported receiving HeadStart support for the first time at Time 2 (counselling). For one of these participants, this support had continued at Time 3, although with a new counsellor, as her previous counsellor at Time 2 had not managed to help her. For the other participant, this support (which had also included therapeutic work with her parents) had ended by Time 3. However, both of these participants also mentioned receiving support from statutory CAMHS in relation to feelings of anxiety, depression, and self-harm at Time 3.
[My previous counsellor] couldn’t cope with the situation. It was too hard for her to deal with because, she, she, she was too young […] like, she couldn’t help, she didn’t know what to do with it. Um, and that’s why we had to go with a different person. (Group C, Time 2)
Two participants in Group C reported receiving HeadStart support (e.g., online counselling) for the first time at Time 3. One of these participants also mentioned receiving professional support at Time 1 for ADHD. The other participant mentioned historic contact with social care at Time 2 and current support from social care at Time 3. This participant described having recently been referred to a youth worker by her social worker for additional emotional support, which she felt had been helpful.
Our sample consisted of adolescents who were attending schools in England implementing a mental health prevention programme, HeadStart. Within our sample, we identified three groups of participants: those who reported that their levels of difficulty in life had improved or were manageable by the third year of the study (Group A); those who reported experiencing some ongoing difficulties and some areas of improvement (Group B); and those who reported that their levels of difficulty had deteriorated or were hard to manage (Group C). Young people who reported experiencing higher and/or persistent levels of difficulty in life over time, as compared to their counterparts, more often described using such coping strategies as self-defence and self-harm, referred to limitations in the efficacy of particular activities and strategies, voiced reasons why they were reluctant or unable to seek support from their parents, perceived limitations in support from school staff, and reported more mixed experiences of support from professionals, in terms of the timing of support and their perceptions of its efficacy. This aligns with findings from a previous qualitative study conducted to examine change over the first two years of HeadStart in young people’s experiences of difficulties and support, drawing on the wider qualitative longitudinal study sample of 78 participants (Stapley, Eisenstadt, Demkowicz, Stock, & Deighton, 2020b ). This study found that young people who described having more difficult experiences in general over the two-year period were more likely to report having sources of support characterised by uncertainty or ambiguity (Stapley et al., 2020b ).
The findings of the current study also reflect previous quantitative findings, which have similarly identified variation in the incidence and impact of protective factors according to the level of adversity that young people are experiencing (e.g., Fergusson, Lynskey, & Horwood, 1996 ; Kassis et al., 2013 ). However, our qualitative findings also add to this previous quantitative research by showing when, how, and why particular factors and processes may be more or less protective from the perspective of young people who are experiencing varying levels of adversity. For instance, in previous research, friendships have been found to mitigate against the negative effects of bullying (Kendrick, Jutengren, & Stattin, 2012 ), and family adversity (Criss, Pettit, Bates, Dodge, & Lapp, 2002 ). Yet, while comparatively high proportions of participants across all three groups in our study referred to their friends as a source of support in times of difficulty, the proportion of participants who also described having arguments with their friends was highest in Group C. This could suggest that the quality of support may influence the level of protection that it can offer. Indeed, high quality friendships, defined in terms of perceptions of supportiveness, have been found to predict lower levels of future victimisation by bullies (Kendrick et al., 2012 ).
Quality may also be relevant when considering the limitations in the efficacy of particular coping strategies that participants in Groups B and C reported, as well as the use of self-harm as a coping strategy in a minority of cases. The coping strategy of positive thinking, on the other hand, employed by a majority of participants in Group A, has been identified in previous research as being an individual-level protective factor implicated in promoting young people’s resilience (Masten & Barnes, 2018 ), and as an adaptive coping strategy (Losoya, Eisenberg, & Fabes, 1998 ; Zimmer-Gembeck & Skinner, 2011 ). Yet, disengagement or withdrawal from problems has been found in previous studies to be associated with poorer mental health outcomes (e.g., (Seiffge-Krenke, 2004 ; Seiffge-Krenke & Klessinger, 2000 ). By contrast, our findings indicate that this is a strategy that the majority of young people engage in, regardless of their levels of difficulty in life (see also Stapley et al., 2020a ). Perhaps this alternatively reflects previous findings from the emotion regulation literature that the use of distraction can enhance adolescents’ levels of positive affect and reduce their levels of negative affect, which may be a solution in the short-term (Wante, Van Beveren, Theuwis, & Braet, 2018 ).
While parental support was drawn on by young people in all three groups in our study, the majority of participants in Group C cited one parent, rather than both, as a source of support, with the non-supportive parent described as less available to talk to because for example, they were busy, they did not live together, or they were a source of difficulty in their lives. By contrast, the majority of participants in Group A referred to both of their parents as being a supportive presence in their lives. Previous qualitative studies have similarly highlighted the importance, from young people’s perspectives, of familial support in protecting against adversity or promoting recovery from mental health issues (e.g., Las Hayas et al., 2016 ; Smokowski & Reynolds, 1999 ). Indeed, close caregiver-child relationships have frequently been identified as a key family-level protective factor for young people in the face of adversity (Masten, 2021 ). The higher levels of familial stress reported by young people in Groups B and C, as compared to Group A, may explain the differences in the levels of familial support that they reported. For example, previous research has identified a negative association between interparental conflict and parental emotional support provision for young people (Riggio, 2004 ).
In terms of support from HeadStart, 61% of participants reported receiving some form of targeted HeadStart support by the end of the three-year period of our study: three-quarters of participants in Group C, just under half of Group B, and just under two-thirds of Group A. In Groups A and B, the majority of participants reported receiving support from HeadStart at Time 1 only. By contrast, in Group C, participants described a range of interactions with HeadStart, with some participants only reporting receiving support at one timepoint and others reporting receiving multiple forms of support across or at different timepoints. Our findings suggest that more long-term, regular, or sustained preventive intervention may be needed for young people who are experiencing higher levels of difficulty in life (see also Stapley et al., 2020b ), such as those within Groups B and C, with perhaps more ‘light touch’ engagement for those experiencing less difficulty over time, such as those within Group A. The latter reflects Ungar et al.’s ( 2018 ) finding that adolescents with high resilience and low risk describe less need for professional support in general, potentially due to the social support that they already have.
School staff nominations are often a starting point for the identification of students for targeted interventions (Campbell, 2004 ). However, research has shown that teachers have less accuracy in identifying young people with emotional problems, compared to behavioural problems (e.g., Cunningham & Suldo, 2014 ; Splett et al., 2020 ), and with moderate or subclinical levels of symptoms, compared to severe (Splett et al., 2019 ). This could offer a potential explanation for why just under 50% of participants in Group B, for example, reported ever receiving HeadStart support, and why, for participants in Group C, the timing of their interactions with HeadStart varied. Thus, instating a regular wellbeing and mental health symptom check-in (such as using standardised self-report outcome measures) with young people each school year, and at the end of support interventions, could help to ensure that young people are offered additional support as and when it is needed (Humphrey & Wigelsworth, 2016 ; Stapley et al., 2020b ).
On the other hand, it is possible that some participants were offered support and chose not to engage with it. Indeed, participants in Groups B and C identified both positive elements and limitations of the HeadStart and professional support that they had received, and described ways in which school staff could be supportive, but also voiced concerns about trusting school staff, or instances of not feeling listened to or understood by school staff. Previous qualitative studies of young people’s help-seeking behaviour have similarly identified young people’s perceptions of issues around school staff trustworthiness and availability as barriers to help-seeking (Helms, 2003 ; Lindsey & Kalafat, 1998 ). Such concerns could thus present a barrier to young people’s engagement with preventive interventions led by trained school staff or implemented within a school setting. Therefore, reviews of evaluations of existing programmes have highlighted the important role that a programme component focusing on promoting a supportive school environment or ethos can have in maximising engagement with and the effectiveness of school-based prevention and early intervention programmes (Weare & Nind, 2011 ).
Training in coping and problem-solving skills is often a key component in psychological interventions (Horwitz, Opperman, Burnside, Ghaziuddin, & King, 2016 ). Some of the coping strategies that participants described appear to align with treatment components across a range of evidence-based prevention and treatment approaches; for instance, positive thinking echoes aspects of cognitive restructuring activities within cognitive behavioural therapy (CBT) approaches (Clark, 2013 ). Yet, interventions that primarily aim to effect change at the level of the individual may have more limited efficacy for those who are experiencing high levels of contextual stress. Indeed, higher levels of family dysfunction have been found to predict poorer mental health treatment outcomes for adolescents (Phillips et al., 2000 ). This could explain why participants in Group C, approximately 90% of whom reported experiencing various sources of familial stress, were experiencing difficulties with their mental health and relationships by Time 3, despite 75% of them reporting receipt of HeadStart support by that point. Thus, following a review of resilience research, Luthar ( 2015 ) concluded that to maximise the potential for success, resilience-enhancing interventions should focus on invoking change in both the child and in their wider environment. For instance, the UK-based Thrive Framework is a needs-based approach to mental health and wellbeing support, which “provides a set of principles for creating coherent and resource-efficient communities of mental health and wellbeing support for children, young people and families” (Wolpert et al., 2019 , p.2).
In a review of school-based mental health services, Rones and Hoagwood ( 2000 ) found that effectiveness was associated with multi-component programmes that targeted the ecology of the child, such as through involving parents (e.g., in parenting skill development sessions) and teachers (e.g., in classroom management techniques training). Similarly, in a systematic review, Weare and Nind ( 2011 ) found that the involvement of parents was cited in multiple reviews as a key ingredient in school-based preventive interventions. However, only one participant in our study mentioned receiving a HeadStart intervention that involved therapeutic work with their parents. Thus, particularly for young people who are experiencing higher levels of adversity in life (e.g., familial strain), our findings suggest that mental health prevention programmes like HeadStart could benefit from placing emphasis on implementing interventions that seek to effect change and boost the resources available within young people’s wider contexts, as well as within young people themselves. This reflects theories of resilience that emphasise the role of the individual’s connections and relationships with external systems in promoting resilience, as well as their own capacity to cope (e.g., Masten & Barnes, 2018 ; Ungar et al., 2008 ).
Strengths and Limitations
Our study illuminates the different coping strategies and sources of support that adolescents experiencing varying levels of adversity in life view as protective (or less so) in relation to handling difficult situations and feelings over a three-year period – and why. A limitation of our study relates to the transferability of our findings. Most notably, our sample consisted of adolescents who were identified and invited to take part by school staff or HeadStart staff, based on current or potential future engagement in some aspect of HeadStart. Thus, our findings may overlook wider experiences, including those experiencing adversity without the school’s awareness, whose experiences of coping and social support may well be different. Similarly, there may be individuals who declined to take part, and we do not know how their experiences relate to those reported here.
Furthermore, our sample includes only those who chose to take part in all three interviews over the three-year period of the study. We do not know whether additional themes would be identified from interviews with adolescents who were unable to take part in all three interviews, such as if they had moved to a different school and were uncontactable by the research team. It is possible that the latter may be those who are experiencing particularly high levels of adversity. In terms of demographic information, we note that the majority of our sample identified themselves as being from a White ethnic background. Future research would benefit from an emphasis on sociodemographic representativeness in sampling, including direct exploration of how ethnicity may play a role in the protective factors and processes identified by adolescents in the UK. We note too that our findings are by nature specific to England, but may nevertheless offer value to researchers in other countries when considered in conjunction with research specific to their locality.
The findings solely reflect participants’ reports of experiences of difficulties in life, coping, and engagement with support that they remembered to or chose to share in their interviews. While every effort was made to help participants to feel comfortable and secure in the interview situation, including building rapport during each interview and ensuring where possible that the same researcher interviewed the same participant across all three timepoints, some participants may have felt less comfortable about sharing their experiences with a stranger, or sharing experiences that might have led to them feeling upset or embarrassed in their interviews (Docherty & Sandelowski, 1999 ). Lack of reference in an interview is not an objective indication that a participant definitely did not draw on a particular coping strategy or support source. For this reason, we did not seek to explore change over time in the minutiae of young people’s usage of particular coping strategies and support. Participants were also not explicitly asked about change over time in relation to each individual coping strategy and source of support mentioned in each interview.
The interview questions focused on participants’ experiences of coping and seeking or receiving support over each year of the study. Thus, it is important to note that while a broad range of protective factors have been identified in resilience research, including for example ‘skilled parenting’ and ‘connections with well-functioning communities’ (Masten & Barnes, 2018 ), our study focused specifically on the types of coping strategies and sources of support that young people report as being protective in the face of difficulty, as this was the focus of the interviews. In addition, there were a minority of problems (e.g., physical health issues) and sources of support (e.g., support from adults outside of the family and school) that were referenced so infrequently and by such a small number of participants that they were not included in our final list of themes.
Participants were grouped in our analysis based on their subjective experiences of the levels of difficulty in their lives that they were experiencing by the third timepoint of the study. We are unable to report objectively on the levels of mental health difficulties that would meet clinical thresholds within our sample. However, we reflect on the possible circularity of grouping participants in this way, in that individuals with higher levels of mental health concerns may be more likely to perceive situations as stressful or notice stressful aspects of their environment, or individuals experiencing more stressful situations or situated within a more stressful environment may be more likely to experience higher levels of mental health concerns.
Our findings add to previous research by showing that the types, quality, and consistency of reported coping strategies and support, as described by adolescents in a UK context, varies in line with whether adolescents report experiencing higher or lower levels of adversity in life over time, and according to the resources that they have available within their physical and social environments. Future research in this area could qualitatively explore the additional factors and processes, both internal and external to the individual, beyond coping strategies and sources of support, that adolescents in this context describe as protective, and examine how these may also vary in line with the level of adversity experienced. Future research could also seek to further disentangle the differences between the presence and quality of different support sources and coping strategies as protective factors. Understanding the specific support and coping processes that are perceived to be most helpful by adolescents could indicate important areas for intervention.
Our findings suggest that more long-term, regular, or sustained early intervention may be needed for young people experiencing higher levels of difficulty in life. School staff and practitioners implementing regular reviews with young people regarding their support needs and preferences could help to ensure that young people receive timely support that is best suited to their needs. This aligns with a needs-based approach to providing support for young people’s mental health and wellbeing. Finally, for maximum effectiveness with young people who are experiencing high levels of contextual adversity, preventive interventions could benefit from being multi-component, such as incorporating family, school, and individual elements to boost the resources available within young people’s wider contexts, as well as within young people themselves.
Availability of Data and Material
Access to data is restricted to the HeadStart Learning Team to comply with the study’s ethical approval. Materials (e.g., interview schedules) are available upon request to the corresponding author.
Code Availability
Not applicable.
Askeland, K. G., Bøe, T., Breivik, K., la Greca, A. M., Sivertsen, B., & Hysing, M. (2020). Life events and adolescent depressive symptoms: Protective factors associated with resilience. PLoS ONE , 15(6 June), https://doi.org/10.1371/journal.pone.0234109
Blakemore, S. J. (2012, March). Development of the social brain in adolescence. Journal of the Royal Society of Medicine . https://doi.org/10.1258/jrsm.2011.110221
Bowen, N. K., Lee, J. S., & Weller, B. E. (2007). Social Environmental Risk and Protection: Implications for Practice in Elementary Schools Social Environmental Risk and Protection: A Typology with Implications for Practice in Elementary Schools . Retrieved from https://academic.oup.com/cs/article/29/4/229/552358
Braun, V., & Clarke, V. (2006). Using thematic analysis in psychology. Qualitative Research in Psychology , 3(2), 77–101. https://doi.org/10.1191/1478088706qp063oa
Article Google Scholar
Braun, V., & Clarke, V. (2019, August 8). Reflecting on reflexive thematic analysis. Qualitative Research in Sport, Exercise and Health . Routledge. https://doi.org/10.1080/2159676X.2019.1628806
Braun, V., & Clarke, V. (2021). One size fits all? What counts as quality practice in (reflexive) thematic analysis? Qualitative Research in Psychology , 18(3), 328–352. https://doi.org/10.1080/14780887.2020.1769238
Bronfenbrenner, U. (1979). The Ecology of Human Development . Cambridge, MA: Harvard University Press
Google Scholar
Campbell, M. A. (2004). Identification of “at-risk” students for prevention and early intervention programs in secondary schools. Australian Journal of Guidance and Counselling , 14(1), 65–77
Chee, W. (2019). “Lose at the Starting Line, Win at the Finishing Line”: The Narratives Behind Beating Academic Adversity. Social Indicators Research , 145(2), 741–753. https://doi.org/10.1007/s11205-017-1574-8
Clark, D. A. (2013). Cognitive restructuring. In S. G. Hofmann (Ed.), The Wiley Handbook of Cognitive Behavioural Therapy (pp. 1–22). John Wiley & Sons Ltd
Cohen, S. (2004). November). Social relationships and health. American Psychologist . https://doi.org/10.1037/0003-066X.59.8.676
Chowdry, H., & Fitzsimons, P. (2016). The Cost of Late Intervention: EIF Analysis 2016. Retrieved from https://www.eif.org.uk/report/the-cost-of-late-intervention-eif-analysis-2016 [October, 2021]
Criss, M. M., Pettit, G. S., Bates, J. E., Dodge, K. A., & Lapp, A. L. (2002). Family Adversity, Positive Peer Relationships, and Children’s Externalizing Behavior: A Longitudinal Perspective on Risk and Resilience .Child Development (Vol. 73)
Cunningham, J. M., & Suldo, S. M. (2014). Accuracy of teachers in identifying elementary school students who report at-risk levels of anxiety and depression. School Mental Health: A Multidisciplinary Research and Practice Journal , 6(4), 237–250. https://doi.org/10.1007/s12310-014-9125-9
Department of Health and Social Care & Department for Education (2018). Government Response to the First Joint Report of the Education and Health and Social Care Committees of Session 2017–2019 on Transforming Children and Young People’s Mental Health Provision: A Green Paper. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/728902/HESC_Print__3_.pdf
Docherty, S., & Sandelowski, M. (1999). Focus on Qualitative Methods Interviewing Children . Research in Nursing & Health (Vol. 22)
Eriksson, I., Cater, Å., Andershed, A. K., & Andershed, H. (2010). What we know and need to know about factors that protect youth from problems: A review of previous reviews. Procedia - Social and Behavioral Sciences (5 vol., pp. 477–482). Elsevier Ltd. https://doi.org/10.1016/j.sbspro.2010.07.127
Everall, R. D., Altrows, K. J., & Paulson, B. L. (2006). Creating a Future: A Study of Resilience in Suicidal Female Adolescents. Journal of Counseling & Development , 84(4), 461–471. https://doi.org/10.1002/j.1556-6678.2006.tb00430.x
Evidence Based Practice Unit. (2018). What are HeadStart interventions focusing on to improve mental health in 10 to 16-year-olds? . London: EBPU. https://www.ucl.ac.uk/evidence-based-practice-unit/sites/evidence-based-practice-unit/files/headstart-heads-up-012019.pdf
Evidence Based Practice Unit. (2019). What are local HeadStart partnerships doing to support the mental health of children and young people aged 10 to 16? . London: EBPU. https://www.ucl.ac.uk/evidence-based-practice-unit/sites/evidence-based-practice-unit/files/headstart-heads-up-022019.pdf
Fergusson, D. M., Lynskey, M. T., & Horwood, L. J. (1996). Factors Associated with Continuity and Changes in Disruptive Behavior Patterns Between Childhood and Adolescence .Journal of Abnormal Child Psychology(Vol. 24)
Fritz, J., de Graaff, A. M., Caisley, H., van Harmelen, A. L., & Wilkinson, P. O. (2018). A Systematic Review of Amenable Resilience Factors That Moderate and/or Mediate the Relationship Between Childhood Adversity and Mental Health in Young People. Frontiers in Psychiatry , 9 . https://doi.org/10.3389/fpsyt.2018.00230
Fritz, J., Stochl, J., Goodyer, I. M., van Harmelen, A. L., & Wilkinson, P. O. (2020). Embracing the positive: an examination of how well resilience factors at age 14 can predict distress at age 17. Translational Psychiatry , 10(1), https://doi.org/10.1038/s41398-020-00944-w
Garmezy, N. (1974). The study of competence in children at risk for severe psychopathology. In E. J. Anthony, & C. Koupernik (Eds.), The Child in his Family: Children at Psychiatric Risk (pp. 77–97). John Wiley & Sons
Garmezy, N. (1985). Stress-resistant children: The search for protective factors. In J. E. Stevenson (Ed.), Recent Research in Developmental Psychopathology: Journal of Child Psychology and Psychiatry Book Supplement, No. 4 (pp. 213–233). Oxford: Pergamon
Helms, J. L. (2003). Barriers to Help Seeking among 12th Graders. Journal of Educational and Psychological Consultation , 14(1), 27–40. https://doi.org/10.1207/S1532768XJEPC1401_02
Horwitz, A. G., Opperman, K. J., Burnside, A., Ghaziuddin, N., & King, C. A. (2016). Youth suicide. In M. Rom, & Korin (Eds.), Health Promotion for Children and Adolescents (pp. 125–144). New York: Springer Science + Business Media
Chapter Google Scholar
Humphrey, N., & Wigelsworth, M. (2016). Making the case for universal school-based mental health screening. Emotional and Behavioural Difficulties , 21(1), 22–42. https://doi.org/10.1080/13632752.2015.1120051
Kassis, W., Artz, S., Scambor, C., Scambor, E., & Moldenhauer, S. (2013). Finding the way out: A non-dichotomous understanding of violence and depression resilience of adolescents who are exposed to family violence. Child Abuse and Neglect , 37(2–3), 181–199. https://doi.org/10.1016/j.chiabu.2012.11.001
Kendrick, K., Jutengren, G., & Stattin, H. (2012). The protective role of supportive friends against bullying perpetration and victimization. Journal of Adolescence , 35(4), 1069–1080. https://doi.org/10.1016/j.adolescence.2012.02.014
Lai, B. S., Lewis, R., Livings, M. S., Greca, L., A. M., & Esnard, A. M. (2017). Posttraumatic Stress Symptom Trajectories Among Children After Disaster Exposure: A Review. Journal of Traumatic Stress , 30(6), 571–582. https://doi.org/10.1002/jts.22242
Las Hayas, C., Padierna, J. A., Muñoz, P., Aguirre, M., Gómez del Barrio, A., Beato-Fernández, L., & Calvete, E. (2016). Resilience in eating disorders: A qualitative study. Women and Health , 56(5), 576–594. https://doi.org/10.1080/03630242.2015.1101744
Lazarus, R. S., & Folkman, S. (1984). Stress, Appraisal, and Coping . New York, NY: Springer
Lindsey, C. R., & Kalafat, J. (1998). Adolescents’ views of preferred helper characteristics and barriers to seeking help from school-based adults. Journal of Educational and Psychological Consultation , 9(3), 171–193. https://doi.org/10.1207/s1532768xjepc0903_1
Losoya, S., Eisenberg, N., & Fabes, R. A. (1998). Developmental issues in the study of coping. International Journal of Behavioral Development , 22(2), 287–313. https://doi.org/10.1080/016502598384388
Luthar, S. S. (2015). Resilience in development: A synthesis of research across five decades. In D. Cicchetti, & D. J. Cohen (Eds.), Developmental psychopathology: Risk, disorder, and adaptation (pp. 739–795). John Wiley
Luthar, S. S., Cicchetti, D., & Becker, B. (2000). The construct of resilience: A critical evaluation and guidelines for future work. Child Development , 71(3), 543–562. https://doi.org/10.1111/1467-8624.00164
Masia-Warner, C., Nangle, D. W., & Hansen, D. J. (2006). Bringing evidence-based child mental health aervices to the schools: General issues and specific populations. Education & Treatment of Children , 29(2), 165–172
Masten, A. S. (2014). Ordinary Magic: Resilience in Development . Guilford Press
Masten, A. S. (2021). Resilience of children in disasters: A multisystem perspective. International Journal of Psychology , 56(1), 1–11. https://doi.org/10.1002/ijop.12737
Masten, A., & Barnes, A. (2018). Resilience in Children: Developmental Perspectives. Children , 5(7), 98. https://doi.org/10.3390/children5070098
Maxwell, J. A. (2010). A Realist Approach for Qualitative Research . SAGE
Morales, E. E. (2008). Academic Resilience in Retrospect: Following Up a Decade Later. Journal of Hispanic Higher Education , 7(3), 228–248. https://doi.org/10.1177/1538192708317119
Olsson, C. A., Bond, L., Burns, J. M., Vella-Brodrick, D. A., & Sawyer, S. M. (2003). Adolescent resilience: a concept analysis . Journal of Adolescence (Vol. 26). Retrieved from www.elsevier.com/locate/jado
Ozer, E. J., Newlan, S., Douglas, L., & Hubbard, E. (2013). “Bounded” Empowerment: Analyzing Tensions in the Practice of Youth-Led Participatory Research in Urban Public Schools. American Journal of Community Psychology , 52(1–2), 13–26. https://doi.org/10.1007/s10464-013-9573-7
Phillips, S. D., Hargis, M. B., Kramer, T. L., Lensing, S. Y., Taylor, J. L., Burns, B. J., & Robbins, J. M. (2000). Toward a level playing field: Predictive factors for the outcomes of mental health treatment for adolescents. Journal of the American Academy of Child and Adolescent Psychiatry , 39(12), 1485–1495. https://doi.org/10.1097/00004583-200012000-00008
Probst, B. (2015). The eye regards itself: Benefits and challenges of reflexivity in qualitative social work research. Social Work Research , 39(1), 37–48. https://doi.org/10.1093/swr/svu028
Riggio, H. R. (2004). Parental marital conflict and divorce, parent-child relationships, social support, and relationship anxiety in young adulthood. Personal Relationships , 11, 99–114
Rones, M., & Hoagwood, K. (2000). School-based mental health services: A research review. Clinical Child and Family Psychology Review , 3, 223–241
Seiffge-Krenke, I. (2004). Adaptive and maladaptive coping styles: Does intervention change anything? European Journal of Developmental Psychology , 1(4), 367–382. https://doi.org/10.1080/17405629.2004.11453396
Seiffge-Krenke, I., & Klessinger, N. (2000). Long-Term Effects of Avoidant Coping on Adolescents’ Depressive Symptoms .Journal of Youth and Adolescence(Vol. 29)
Smokowski, P. R., & Reynolds, A. J. (1999). Resilience and Protective Factors in Adolescence: An Autobiographical Perspective From Disadvantaged Youth .Journal of School Psychology (Vol. 37)
Southwick, S. M., Bonanno, G. A., Masten, A. S., Panter-Brick, C., & Yehuda, R. (2014). Resilience definitions, theory, and challenges: Interdisciplinary perspectives. European Journal of Psychotraumatology , 5, 25338. DOI: https://doi.org/10.3402/ejpt.v5.25338
Splett, J. W., Garzona, M., Gibson, N., Wojtalewicz, D., Raborn, A., & Reinke, W. M. (2019). Teacher Recognition, Concern, and Referral of Children’s Internalizing and Externalizing Behavior Problems. School Mental Health , 11(2), 228–239. https://doi.org/10.1007/s12310-018-09303-z
Splett, J. W., Raborn, A., Brann, K., Smith-Millman, M. K., Halliday, C., & Weist, M. D. (2020). Between-teacher variance of students’ teacher-rated risk for emotional, behavioral, and adaptive functioning. Journal of School Psychology , 80, 37–53. https://doi.org/10.1016/j.jsp.2020.04.001
Stapley, E., Demkowicz, O., Eisenstadt, M., Wolpert, M., & Deighton, J. (2020a). Coping with the stresses of daily life in England: A qualitative study of self-care strategies and social and professional support in early adolescence. The Journal of Early Adolescence , 40(5), 605–632. doi: https://doi.org/10.1177/0272431619858420
Stapley, E., Eisenstadt, M., Demkowicz, O., Stock, S., & Deighton, J. (2020b). Learning From Young People in HeadStart: A Study of Change Over Time in Young People’s Experiences of Difficulties and Support . London: EBPU
Ungar, M. (2003). Qualitative Contributions to Resilience Research. Qualitative Social Work , 2(1), 85–102. https://doi.org/10.1177/1473325003002001123
Ungar, M. (2008). Resilience across cultures. British Journal of Social Work , 38(2), 218–235. https://doi.org/10.1093/bjsw/bcl343
Ungar, M. (Ed.). (2012). The Social Ecology of Resilience: A Handbook of Theory and Practice . Springer Science + Business Media. https://doi.org/10.1007/978-1-4614-0586-3
Ungar, M., Brown, M., Liebenberg, L., Cheung, M., & Levine, K. (2008). Distinguishing differences in pathways to resilience among Canadian youth. Canadian Journal of Community Mental Health , 27(1), 1–13. https://doi.org/10.7870/cjcmh-2008-0001
Ungar, M., Ghazinour, M., & Richter, J. (2013, April). Annual research review: What is resilience within the social ecology of human development? Journal of Child Psychology and Psychiatry and Allied Disciplines . https://doi.org/10.1111/jcpp.12025
Ungar, M., Hadfield, K., & Ikeda, J. (2018). Adolescents’ experiences of therapeutic relationships at high and low levels of risk and resilience. Journal of Social Work Practice , 32(3), 277–292. https://doi.org/10.1080/02650533.2017.1384999
Valiente, C., Eisenberg, N., Fabes, R. A., Spinrad, T. L., & Sulik, M. J. (2015). Coping Across the Transition to Adolescence: Evidence of Interindividual Consistency and Mean-Level Change. Journal of Early Adolescence , 35(7), 947–965. https://doi.org/10.1177/0272431614548068
Vizard, T., Sadler, K., Ford, T., Newlove-Delgado, T., McManus, S., Marcheselli, F. ... Cartwright, C. (2020). Mental Health of Children and Young People in England, 2020: Wave 1 Follow up to the 2017 Survey. Retrieved from https://files.digital.nhs.uk/AF/AECD6B/mhcyp_2020_rep_v2.pdf [February 2022]
Wante, L., Van Beveren, M. L., Theuwis, L., & Braet, C. (2018). The effects of emotion regulation strategies on positive and negative affect in early adolescents. Cognition and Emotion , 32(5), 988–1002. https://doi.org/10.1080/02699931.2017.1374242
Weare, K., & Nind, M. (2011). Mental health promotion and problem prevention in schools: What does the evidence say? Health Promotion International , 26 (SUPPL. 1). https://doi.org/10.1093/heapro/dar075
Werner-Seidler, A., Perry, Y., Calear, A. L., Newby, J. M., & Christensen, H. (2017, February 1). School-based depression and anxiety prevention programs for young people: A systematic review and meta-analysis. Clinical Psychology Review . Elsevier Inc. https://doi.org/10.1016/j.cpr.2016.10.005
Wolpert, M., Harris, R., Hodges, S., Fuggle, P., James, R., Wiener, A. … Munk, S. (2019). THRIVE Framework for System Change . London: CAMHS Press
Zimmer-Gembeck, M. J., & Skinner, E. A. (2011). Review: The development of coping across childhood and adolescence: An integrative review and critique of research. International Journal of Behavioral Development , 35(1), 1–17. https://doi.org/10.1177/0165025410384923
Download references
Acknowledgements
We are indebted to the young people who generously shared their experiences with us.
With thanks to other members of the HeadStart Learning Team (Mia Eisenstadt, Rosa Town, Alisha O’Neill, and Parise Carmichael-Murphy) for their vital role in the collection, management, and analysis of data used to inform our research publications.
With thanks also to our colleagues in the National Institute for Health Research (NIHR) Children and Families Policy Research Unit (Ruth Gilbert, Kevin Herbert, Tanya Lereya, and Sarah Cattan) for their helpful feedback on earlier drafts of this paper.
HeadStart is a six-year, £67.4 m National Lottery funded programme set up by The National Lottery Community Fund, the largest funder of community activity in the UK. The interview data analysed in this study were collected as part of the Learning Team’s national evaluation of HeadStart, funded by The National Lottery Community Fund. The views expressed are those of the author(s) and not necessarily those of The National Lottery Community Fund.
This study was funded by the National Institute for Health Research (NIHR) Policy Research Programme. ES was also partly supported by the NIHR ARC North Thames. The views expressed are those of the author(s) and not necessarily those of the NIHR or the Department of Health and Social Care.
Author information
Authors and affiliations.
Evidence Based Practice Unit (EBPU), Anna Freud National Centre for Children and Families and University College London (UCL), 4-8 Rodney Street, N1 9JH, London, England
Emily Stapley, Sarah Stock & Jessica Deighton
Manchester Institute of Education, The University of Manchester, Manchester, England
Ola Demkowicz
You can also search for this author in PubMed Google Scholar
Contributions
ES conceived of the study, led on in its design, coordination, and data collection and analysis, and drafted the manuscript; SS participated in the study design and data analysis, and contributed to the drafting of the manuscript; JD led on the acquisition of funding, participated in the study design and coordination, and contributed to the drafting of the manuscript; OD participated in data collection and analysis, and contributed to the drafting of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Correspondence to Emily Stapley .
Ethics declarations
Conflicts of interest/competing interests.
The authors have no relevant financial or non-financial interests to disclose.
Consent to Participate and for Publication
As all participants were under the age of 16, written informed consent was sought from the young people’s parents/carers and written assent was sought from the young people themselves for them to take part and for the publication of their anonymised data.
Ethics Approvals
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards. Ethical approval for this study was granted by the University College London (UCL) Research Ethics Committee (ID number 7963/002).
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ .
Reprints and permissions
About this article
Stapley, E., Stock, S., Deighton, J. et al. A Qualitative Study of How Adolescents’ Use of Coping Strategies and Support Varies in Line With Their Experiences of Adversity. Child Youth Care Forum 52 , 177–203 (2023). https://doi.org/10.1007/s10566-022-09682-0
Download citation
Received : 09 June 2021
Revised : 22 December 2021
Accepted : 09 February 2022
Published : 01 March 2022
Issue Date : February 2023
DOI : https://doi.org/10.1007/s10566-022-09682-0
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Adolescence
- Qualitative
- Find a journal
- Publish with us
- Track your research
- Research article
- Open access
- Published: 15 July 2021
How have people been coping during the COVID-19 pandemic? Patterns and predictors of coping strategies amongst 26,016 UK adults
- Meg Fluharty 1 &
- Daisy Fancourt 1
BMC Psychology volume 9 , Article number: 107 ( 2021 ) Cite this article
27k Accesses
51 Citations
6 Altmetric
Metrics details
Individuals face increased psychological distress during the COVID-19 pandemic. However, it’s unknown whether choice of coping styles are influenced by COVID-19 in addition to known predictors.
Data from 26,016 UK adults in the UCL COVID-19 Social Study were analysed from 12/4/2020 15/5/2020. Regression models were used to identify predictors of coping styles (problem-focused, emotion-focused, avoidant, and socially-supported): model 1 included sociodemographic variables, model 2 additionally included psychosocial factors, and model 3 further included experience of COVID-19 specific adverse worries or events.
Sociodemographic and psychosocial predictors of coping align with usual predictors of coping styles not occurring during a pandemic. However, even when controlling for the wide range of these previously known predictors specific adversities were associated with use of specific strategies. Experience of worries about finances, basic needs, and events related to Covid-19 were associated with a range of strategies, while experience of financial adversities was associated with problem-focused, emotion-focused and avoidant coping. There were no associations between coping styles and experiencing challenges in meeting basic needs, but Covid-19 related adversities were associated with a lower use of socially-supported coping.
Conclusions
This paper demonstrates that there are not only demographic and social predictors of coping styles during the COVID-19 pandemic, but specific adversities are related to the ways that adults cope. Furthermore, this study identifies groups at risk of more avoidant coping mechanisms which may be targeted for supportive interventions.
Peer Review reports
The coronavirus (COVID-19) pandemic has had diverse negative psychological effects globally. Individuals have experienced a wide range of adversities due to the virus, including those relating to the virus itself (such as experiencing illness oneself, concerns for friends and family, and bereavement), financial adversities (including loss of work or income, and inability to pay bills), and challenges in meeting basic needs (such as accessing sufficient food, medicine, and safe accommodation) [ 1 ]. Recent research has highlighted substantial increases in mental illness and loneliness during the COVID-19 pandemic [ 2 , 3 ]. Whilst some of these experiences reflect those reported during previous pandemics [ 4 ], COVID-19 is causing greater concern due to the global scale, heavy lockdown measures implemented, and long time scale predicted [ 5 ].
As a large proportion of the global population has experienced some form of psychological distress during the pandemic, there have been calls for more research exploring factors that help to buffer against or exacerbate experiences [ 6 ]. This is particularly important given there are projected long-lasting effects of the COVID-19 pandemic alongside limited mental health resources available [ 7 ]. However, there were inequalities in those who were more likely to be negatively affected by pandemic-related stressors, with certain groups including younger adults, women, people from Black Asian Minority Ethic (BAME) groups, and people living alone experiencing poor mental health [ 4 ]. Differences in mental health responses are likely be influenced by differences in individuals’ use of various coping strategies. Therefore understanding coping strategies could help to identify the social and personal resources required by individuals to mitigate psychological stress as COVID-19 continues, and in future pandemics.
Coping is broadly defined as the conscious or unconscious cognitive and behavioural strategies an individual employs to manage stress [ 8 , 9 ]. Numerous coping strategies have been identified, including self-distraction, active coping, denial, substance use, use of emotional support, use of informational support, and behavioural changes. These different coping strategies are often categorised into different groups. For example, 'approach' strategies typically focus on the stressor and one’s actions towards it (e.g. seeking emotional support or planning to resolve and reduce stressors)[ 10 ], while by contrast, 'avoidant' strategies seek to avoid the stressor and ones reaction to it (e.g. withdrawing from others, substance use, and denying the reality of the stressor) [ 11 , 12 ]. Additional groupings of focus on whether activities are 'emotion-focused' (aiming to manage emotional distress; e.g. denial, venting, emotional support) or 'problem-focused' (efforts to modify the problem at hand; e.g. informational support, active coping) [ 13 ]. There is much debate as to whether certain strategies are more beneficial than others. For example, avoidance strategies may be helpful in reducing short term stress, but are generally considered harmful from the perspective of physical well-being as no direct actions are taken to reduce the stressor, leaving the individual to feel helpless or self-blaming [ 11 , 14 , 15 , 16 , 17 ].
Previous studies have identified a range of predictors for coping style choice. Evidence suggests lower SEP is associated with greater use of avoidant strategies. These individuals have increased likelihood of exposure to stressors across the life course and may have less efficient coping strategies as a result of the social resources needed to combat stressors as well as less access to social support [ 18 ]. Personality type may influence coping strategy choice indirectly (influencing severity of stressors and effectiveness of coping) or directly by facilitating how individuals engage or disengage with threats and stressors (e.g. threat sensitivity in neurotic individuals may result in disengagement, while highly social extraverts may seek more supportive coping) [ 19 , 20 ]. Furthermore, the way individuals react to stressors can have long term health effects [ 21 , 22 ]. Avoidance strategies are typically at the core of depression and anxiety [ 23 ], which is why the most effective therapies (i.e. cognitive-behavioural therapy) focus on cognitive reappraisal and problem solving responses [ 24 ]. For example when faced with a traumatic event, adoption of avoidant strategies are associated with later mental health problems. This is particularly pertinent when considering individuals’ psychological responses to adversities during the COVID-19 pandemic as it is possible that coping strategies may be influenced solely by existing traits. However, it is also possible that the unusual and adverse circumstances of the pandemic may affect individuals’ coping resources and alter usual psychological responses [ 25 ]. It is vital to understand these patterns and predictors of coping strategies in order to identify who is most at need of additional psychological support.
Therefore, this study examined predictors of coping strategies amongst adults during the COVID-19 pandemic. Specifically, we explored (i) whether sociodemographic predictors of coping strategies align with usual predictors not during a pandemic, (ii) whether psychosocial factors including individuals’ roles during the pandemic, their living situation and their health status affected their use of coping strategies, and (iii) whether specific adverse experiences during the pandemic predisposed individuals to using more avoidant coping strategies above and beyond trait sociodemographic and psychosocial factors.
Participants
Data were drawn from the COVID-19 Social Study; a large panel study of the psychological and social experiences of over 70,000 adults (aged 18 +) in the United Kingdom (UK) during the COVID-19 pandemic. The study commenced on 21st March 2020 and involves online weekly data collection from participants for the duration of the COVID-19 pandemic in the UK. The study is not random and therefore is not representative of the UK population. But it does contain a well-stratified sample that was recruited using three primary approaches. First, snowballing was used, including promoting the study through existing networks and mailing lists (including large databases of adults who had previously consented to be involved in health research across the UK (e.g. UCL BioResource and Health Wise Wales), print and digital media coverage, and social media. Second, more targeted recruitment was undertaken focusing on (i) individuals from a low-income background (recruitment via via Find Out Now, SEO Works, FieldworkHub, and Optimal Worskhop, (ii) individuals with no or few educational qualifications, and (iii) individuals who were unemployed. Third, the study was promoted via partnerships with third sector organisations to vulnerable groups (e.g. UKRI MARCH Mental Health Research Network), including adults with pre-existing mental health conditions, older adults, carers, and people experiencing domestic violence or abuse.
Questions on coping were asked during a week-long module that was introduced in week 8 of the study 09th to 15th May. A total of 29,882 participants completed these questions in addition to all completing a detailed questionnaire on baseline sociodemographic factors and weekly data on experiences during COVID-19 during the period from 21st March until 15th May. Those who responded 'prefer not to say' to gender (0.43%) and income (9.4%) variables were set to missing, and we excluded participants who were missing data across any of the predictor variables (n = 3,302). An additional 390 participants were excluded as they did not have a baseline wave used to derive survey weights (although took part in the demographic part of the survey at later waves), which left a total complete case analytical sample size of 26,016 (Additional file 1 : Table S1).
Coping strategies
Coping was assessed by asking ‘how have you been coping during lockdown’ and measured using the 28-item brief-COPE questionnaire; a short version of the original 60-item scale. This scale determines primary coping styles as either approach or avoidant and covers the following domains of coping: self-distraction, active coping, denial, substance use, use of emotional support, use of instrumental support, behavioural disengagement, venting, positive reframing, planning, humour, acceptance, religion, & self-blame [ 26 , 27 ]. In line with previous research, we used a previously-derived 4 factor model for our analyses: problem focused coping (active coping, planning), emotion focused coping (positive reframing, acceptance, humour, religion) avoidant coping (behavioural disengagement, denial, substance use), and socially supported coping (emotional support, instrumental support, and venting) [ 28 ].
Sociodemographic predictors
Six sociodemographic predictors were collected at baseline interview: (1) gender (male vs female), (2) age group were chosen to represent younger, middle, and older ages (18–29 vs 30–59 vs 60 +), (3) ethnicity (white vs BAME), (4) educational attainment (General Certificate of Secondary Education (GCSE) or lower (qualifications at age 16) vs A-Levels or vocational training (qualifications at age 18) vs undergraduate degree vs postgraduate degree), (5) low household income (< £30,000 per annum vs ≥ £30,000 per annum), and (6) employment status (employed vs student vs inactive vs unemployed).
Psychosocial predictors
Eight psychosocial predictors were collected at baseline interview: (1) area of dwelling (urban vs rural), (2) living status (alone vs not alone with children vs with others no children), (3) household overcrowding (alone vs with others-not overcrowded vs with others- overcrowded), (4) keyworker status was derived from responses to the question 'Are you currently fulfilling any of the government’s identified 'keyworker' roles?' (keyworker vs non-keyworker), (5) mental health condition (reports of a diagnosis vs none), (6) long term/pre-existing physical health condition or disability (reports of a diagnosis vs none), (7) number of close friends (continuous 1–10 +), (8) Social support was measured using an adapted version of the six-item short form of Perceived Social Support Questionnaire (F-SozU K-6) [ 29 , 30 ]. Each item was rated on a 5-point scale from “not true at all” to “very true”, with higher scores indicating higher levels of perceived social support. Minor adaptations were made to the language in the scale to make it relevant to experiences during COVID-19 (see Additional file 1 : Table S2 for a comparison of changes).
Two psychosocial predictors were asked as repeated questions each week and responses for this analysis were taken from week 8 of the study: [ 9 ] personality was measured using the Big Five Inventory (BFI-2), which measures five domains and 15 facets: Extraversion (sociability, assertiveness, and energy level), Agreeableness (compassion, respectfulness, and trust), Conscientiousness (organisation, productiveness, and responsibility), Nervousness (anxiety, depression, and emotional volatility), and Openness (intellectual curiosity, aesthetic sensitivity, and creative imagination) [ 31 ]. Each item uses a 5-point scale ranging from “strongly disagree” to “strongly agree”, with higher score indicating greater levels of each domain. Finally, [ 10 ] Loneliness was measured using the 3-item UCLA-3 loneliness, a short form of the Revised UCLA Loneliness Scale (UCLA-R) [ 32 ]. Each item was rated with a 4-point rating scale, ranging from “never” to “always”, with higher score indicating greater loneliness, scores were averaged across each week.
Adversity predictors
Repeated questions each week assessed participants’ experience of adversities and responses for this analysis were taken from week 8 of the study: (1) Covid-19 status (positive/suspected vs none); (2) experience of one of a number of specific adversities including financial adversities (yes to any of the following: whether participants had lost their job or been unable to work, their partner had lost their job or was unable to work, or they had experienced a major cut in household income), challenges meeting basic needs (yes to any of the following: whether participants had lost their accommodation, they had been unable to access sufficient food, or they had been unable to access required medication), and virus related adversities (yes to any of the following: whether in the past week the participant had suspected or diagnosed COVID-19, somebody close to them was hospitalised, or they had lost somebody close to them) [ 33 ]; and (3) adversity worries were captured from two questions that asked participants to select which of a list of items had caused them major stress in the past week financial stressors (yes to any of the following: losing your job/unemployment), stressors relating to meeting basic needs (yes to any of the following: your own safety/security, getting food, and getting medication), and stressors relating to the virus (catching or becoming seriously ill from COVID-19) [ 34 ].
We used fixed-effects ordinary least squares regression models to identify predictors of coping styles. 3 additive models were applied to each of the coping styles in a forward stepwise selection. Model 1 included sociodemographic variables, Model 2 additionally included psychosocial factors (Model 2), and Model 3 additionally included experience of specific adverse worries or events.
Complete model specifications are as follows:
Model 1 : [coping style ~ sociodemographic predictors]
Model 2 : [coping style ~ sociodemographic + psychosocial predictors]
Model 3 : [coping style ~ gender + sociodemographic + psychosocial + adversity predictors]
To account for the non-random nature of the sample, data were weighted to the proportions of age group, gender and educational level on the basis of Office for National Statistics (ONS) population estimates [ 35 ]. A cross-sectional weight variable was created for all participants at baseline using the Stata user-written command ‘ebalence’ [ 36 ]. All analyses were carried out in Stata version 16.0 (Statacorps, Texas).
Characteristics of the study sample (both unweighted and weighted samples) are shown in Table 1 . 51% of participants in the weighted sample were female, 91% were of white ethnicity, 45% aged 30–49, and 60% were in full time employment.
The use of problem-focused coping in the sample range from − 0.75 to 1.38 (M =: 0.01, SD = 0.50) with skewness of 0.25 and kurtosis of 2.57, Use of emotion-focused coping ranged from − 1.45 to 1.59 (M = 0.00, SD = 0.66) with skewness of 0.14 and kurtosis of 2.77. Use of avoidant coping ranged from -0.45 to 1.48 (M = 0.08, SD = 0.53) with skewness of 0.98 and kurtosis of 3.20, while use of socially supported coping ranged from -0.91 to 1.71 (M = -0.01, SD = 0.67) with skewness of 0.37 and kurtosis of 2.53.
Women were more likely to use all coping strategies than men (Table 2 [Model 1]). Older adults were less likely to use avoidant and socially supported coping strategies. There were no associations observed for coping strategy by ethnicity. Higher educational attainment was associated with more use of problem-focused, emotion focused, and socially supportive strategies. People who were ‘inactive’ in terms of employment (i.e. retired or home-makers) were less likely to use problem or emotion-focused coping. In terms of SEP, lower SEP (indicated by not owning a home and having lower household income) was associated with greater use of disengagement strategies, while low income was also associated with less use of active and supportive strategies.
Even when controlling for sociodemographic predictors, individuals living in over-crowded households were more likely to use avoidant strategies, whilst individuals living alone were more likely to use a range of coping strategies (Table 3 [Model 2]; full results available in Additional file 1 : Table S3). Individuals living in rural areas were less likely to draw on avoidant or support strategies. Individuals who were lonely were more likely to use a rage of coping strategies, as were those with social support although this was protective against avoidant coping. Keyworkers were less likely to use problem-focused or emotion-focused coping strategies. People with a diagnosed mental health condition were more likely to use avoidant coping and supportive coping, while those with a health condition used supporting strategies. All personality types were generally associated with greater use of all strategies, with the exception, and conscientiousness being associated with lower levels of support, and avoidant, strategies.
Specific events and worries
Even when controlling for the wide range of sociodemographic and psychosocial factors in models 1 and 2, specific adversities were associated with use of specific strategies (Table 4 [Model 3]; full results available in Additional file 1 : Table S4). Experience of worries about finances, basic needs, and events related to Covid-19 were associated with a range of strategies, while experience of financial adversities was associated with problem-focused, emotion-focused and avoidant coping. There were no associations between coping styles and experiencing challenges in meeting basic needs, but Covid-19 related adversities were associated with a lower use of socially-supported coping.
Unweighted analyses for all models are provided in Additional file 1 : Tables S5–S7.
This study explored predictors of coping strategies during the COVID-19 pandemic. Active coping strategies were more common amongst women, older adults, people with higher educational attainment, people who were employed, people with higher income, but was less strongly predicted by psychosocial factors.
Problem-focused and emotion-focused coping strategies were more common amongst women, people with higher educational attainment, and those in school, but less strongly predicted by psychosocial factors. Supportive coping strategies were similarly more common in women, and people with higher education but also amongst younger adults and people with higher income. People living with others were more likely to draw on support strategies, as were people who lonely, who lived in urban areas, and who had a diagnosed mental health condition. Avoidant coping strategies were used more by women, younger adults, and people of lower educational attainment and lower socio-economic position, as well as people living with others, and people with mental health conditions and people who were more lonely.
The demographic predictors of coping including gender [ 37 , 38 ] and age [ 39 , 40 ], and age align with usual predictors of coping styles not occurring during a pandemic. For example, women scored higher on a range of coping styles compared to men [ 37 ]. Older adults were less likely to use lower engagement avoidant and socially supported strategies, which may result from accumulated experience with stressors leading to the adoption of more pro-active approaches [ 39 , 40 ]. Further, there were no apparent differences in coping styles depending on ethnicity. This slightly contrasts with previous studies, which have suggested that individuals from BAME groups are more likely to use alternative coping styles such as religion [ 38 , 41 , 42 ]. But as religion was incorporated within emotion focused coping, this finding may have been obscured. Socioeconomic predictors of coping strategies echoed previous studies, with disadvantaged groups more likely to use avoidant coping strategies [ 18 , 43 ]. Therefore, this study found that the usual demographic predictors of coping strategies were preserved during the COVID-19 pandemic, suggesting that individual’s traits and socio-economic circumstances are at least partly responsible for differences in management of stressors during the pandemic.
However, over and above trait demographic factors, a number of psychosocial factors were also found to influence use of coping strategies. Diagnosed mental health conditions were associated with a heightened use of avoidant coping strategies, echoing previous studies [ 22 , 23 , 25 ]. Although, we also found evidence that people with depression and anxiety turned to supportive coping during the pandemic. This could have been as a direct result of schemes such as Mutual Aid groups, which explicitly tried to support individuals with mental health problems, and a heightened awareness of supporting mental wellbeing during the pandemic. Our findings that keyworkers made less use of problem and emotion-focused coping strategies go against previous research, which suggests that workers in areas such as nursing employ active coping to maintain psychological health and resilience [ 44 , 45 ] However, one potential explanation for this divergence is that a number of keyworkers in the current study unexpectedly found themselves in critical roles (e.g. supermarket employees, delivery and transportation drivers) and lacked previous training or experience in developing specific supportive emotion regulation responses unlike medical professionals, who have been the focus of much of the previous research on coping strategies [ 46 , 47 ]. Our research mirrors previous work showing that overcrowded living is associated with increased avoidant coping strategies [ 48 ]. Additionally, one study of living alone during the pandemic found an increase in substance use coping, although this study did not examine other methods beyond substance use [ 49 ]. With regards to loneliness, increased loneliness in our study was associated with a range of coping styles, which is also supported by previous evidence [ 50 ]. But social support as a coping predictor outside clinical populations [ 51 , 52 ] has not typically been examined. Here we found it associated with decreased avoidant coping, but further research is needed to understand whether this relationship is an artefact of the COVID-19 context or a more general indicator of social predictors of coping styles.
What is most notable, however, is that certain specific events related to the Covid-19 pandemic were also associated with the use of different coping strategies, even after adjusting for sociodemographic factors, and psychosocial characteristics. The finding that events involving Covid-19 adversities were associated with less socially supported strategies, while worries about these events were associated with a range of coping strategies. This suggests that individuals’ have a more positive outlook of how they envision handling certain situations versus the trauma of actually experiencing them. This is supported by previous research showing that people respond more positively in their coping styles to hypothetical situations than to situations for which they have prior experience (such as bullying). The decreased probability of using socially supported coping strategies could underlie the relationship being reported between worries and adversities relating to the virus during the pandemic and poorer levels of depression and anxiety shown in other research [ 34 ]. This is concerning because coping styles aimed at addressing the problems directly have been associated with positive affect and less association with negative affect, while avoidance styles display the opposite [ 53 ]. Coping styles are thought to initiate, modulate, and maintain affective responses, therefore avoidance coping is the least beneficial as it blocks attempts to address the stressors/problem and further blocks awareness that the situation may change. While this can be an effective short term strategy for distracting and resting from a stressor, prolonged reliance on avoidance coping may be harmful as the situation is not changed and individuals are engaging with the stressor for prolonged periods which in turn maintains negative affect [ 53 , 54 , 55 ].
This paper demonstrates that there are not only demographic and social predictors of coping styles during the COVID-19 pandemic, but specific adversities are related to the ways that adults cope. Whilst there are some concerning patterns suggesting that certain groups are at greater risk of using avoidant coping strategies, there is also evidence that individuals can change their coping strategies over time. So coping could be a target for interventions designed to improve mental health during the pandemic. Two approaches could be considered here. First, whilst changing demographic predictors is not a feasible intervention, it is possible that interventions targeting psychosocial factors or specific adversities could provide support. For example, supporting individuals in developing their social networks has been shown to help individuals engage with positive coping during the pandemic [ 56 ]. Second, previous studies have shown that techniques such as Cognitive Behavioural Therapy, stress management apps, and seeking social support can be used to increase adaptive coping strategies [ 23 , 57 , 58 ]. This shift has been found not just to change in-the-moment coping, but also to enhance psychosocial outcomes. For example, lonely individuals who learn more active coping strategies are able to reduce their loneliness [ 50 ]. Similarly, people with mental health problems have been found to experience a reduction in negative symptoms when shifting from avoidant to adaptive coping through the use of cognitive behavioural therapies [ 24 ]. This has been shown specifically for people in isolation too: improvements in mental health have been found for people in prison if they manage to adopt new coping strategies [ 59 , 60 ]. Given the evidence in this study of clear socio-demographic predictors of coping strategies, such interventions could be specifically targeted at individuals in more deprived areas, and those experiencing financial loss [ 61 ].
This study has a number of strengths including its large sample size, its longitudinal tracking of participants used to identify adversities and worries across the first 8 weeks of lockdown, and its rich inclusion of measures on psychological and social experiences during COVID-19. We measured coping using the brief-COPE, a large validated measure. Further, a large portion coping literature is centred around specific traumatic events (e.g. health diagnosis, war, or abuse) and therefore it’s difficult to determine general population versus specific event predictors. However, in our three models we separated out known trait predictors from COVID-19 specific predictors. However, there are several limitations. The study is not nationally representative, although it does have good stratification across all major socio-demographic groups and analyses were weighted on the basis of population estimates of core demographics. Whilst the recruitment strategy deliberately over-sampled from groups such as individuals those from a low-income background, individuals with no or few educational qualifications, and individuals who were unemployed, it is possible that more extreme experiences were not adequately captured. Coping was only measured at one timepoint and therefore, we were not able to examine changes in coping strategy across time. Furthermore, it is possible that individuals experiencing highest levels of adversities including bereavement during the pandemic may have dropped out prior to week eight when the measures on coping were asked, or the sampling may have been selective towards individuals more likely to engage with positive coping strategies as undertaking a weekly questionnaire was arguably an approach-focused strategy. Nevertheless, we had good spread across possible responses for each of the measures included in the coping questionnaire and the sample remained heterogeneous.
Overall our study shows that a combination of trait demographic factors, psychosocial factors, and factors specific to experiences during the first UK lockdown in the COVID-19 pandemic predicted coping strategies. People most at risk of using avoidant coping strategies included those of lower socioeconomic position, with mental health conditions, higher rates of loneliness, and those experiencing COVID-19 related adverse events relating to finances and basic needs. This is noteworthy as the same groups have been identified as having poorer mental health experiences across this period, suggesting that one’s coping strategies could play an important role in how effectively individuals manage to cognitively and behaviourally manage stress during pandemics. It also highlights the importance of both providing specific support that will reduce individuals’ use of avoidant coping strategies such as digital or mutual aid [ 56 , 62 ], and supporting and educating individuals (in particular those most at risk of adverse mental health outcomes) in how to use supportive coping strategies. Such work will be important as the COVID-19 pandemic continues and in the future to help mitigate the adverse psychological effects of such events.
Availability of data and materials
The data was taken from the Covid-19 Social Study ( www.covidsocialstudy.org ), which is not currently open access (May 2021) but will be made available on a third-party archive following the end of the pandemic. Analytical code is available on Github: https://github.com/UCL-BSH/coping-predictors .
Abbreviations
Coronavirus
Black Asian Minority Ethic
Socioeconomic position
United Kingdom
General Certificate of Secondary Education
Perceived Social Support Questionnaire
Big Five Inventory
Office for National Statistics
The Lancet. Redefining vulnerability in the era of COVID-19. The Lancet. 2020;395(10230):1089.
Article Google Scholar
Pierce M, Hope H, Ford T, Hatch S, Hotopf M, Kontopantelis E, et al. Mental health before and during the COVID-19 pandemic: a longitudinal probability sample survey of the UK population. Rochester, NY: Social Science Research Network; 2020 Jun [cited 2020 Jul 9]. Report No.: ID 3624264. https://papers.ssrn.com/abstract=3624264 .
Bu F, Steptoe A, Fancourt D. Who is lonely in lockdown? Cross-cohort analyses of predictors of loneliness before and during the COVID-19 pandemic|medRxiv. Public Health. 2020 [cited 2020 Jul 9]; https://doi.org/10.1101/2020.05.14.20101360v1 .
Brooks SK, Webster RK, Smith LE, Woodland L, Wessely S, Greenberg N, et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. The Lancet. 2020;395(10227):912–20.
Anderson RM, Heesterbeek H, Klinkenberg D, Hollingsworth TD. How will country-based mitigation measures influence the course of the COVID-19 epidemic? The Lancet. 2020;395(10228):931–4.
Holmes EA, O’Connor RC, Perry VH, Tracey I, Wessely S, Arseneault L, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7:547–60.
Article PubMed PubMed Central Google Scholar
Holmes EA, O’Connor RC, Perry VH, Tracey I, Wessely S, Arseneault L, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7(6):547–60.
Lazarus RS, Folkman S. The concept of coping. New York: Columbia University Press; 1991. (Stress and coping: An anthology, 3rd ed.).
Ray C, Lindop J, Gibson S. The concept of coping. Psychol Med. 1982;12(2):385–95.
Article PubMed Google Scholar
Aspinwall LG, Taylor SE. A stitch in time: self-regulation and proactive coping. Psychol Bull. 1997;121(3):417–36.
Rippetoe PA, Rogers RW. Effects of components of protection-motivation theory on adaptive and maladaptive coping with a health threat. J Pers Soc Psychol. 1987;52(3):596–604.
Skinner EA, Edge K, Altman J, Sherwood H. Searching for the structure of coping: A review and critique of category systems for classifying ways of coping. Psychol Bull. 2003;129:216–69.
Baker JP, Berenbaum H. Emotional approach and problem-focused coping: a comparison of potentially adaptive strategies. Cogn Emot. 2007;21(1):95–118.
Leventhal H. Findings and theory in the study of fear communications. In: Berkowitz L, editor. Advances in experimental social psychology. Academic Press: Cambridge; 1970. p. 119–86.
Google Scholar
Hollifield M, Hewage C, Gunawardena CN, Kodituwakku P, Bopagoda K, Weerarathnege K. Symptoms and coping in Sri Lanka 20–21 months after the 2004 tsunami. Br J Psychiatry. 2008;192(1):39–44.
Sliter M, Kale A, Yuan Z. Is humor the best medicine? The buffering effect of coping humor on traumatic stressors in firefighters. J Organ Behav. 2014;35(2):257–72.
Huang J, Liu Q, Li J, Li X, You J, Zhang L, et al. Post-traumatic stress disorder status in a rescue group after the Wenchuan earthquake relief. Neural Regen Res. 2013;8(20):1898–906.
PubMed PubMed Central Google Scholar
Palomar Lever J. Poverty, stressful life events, and coping strategies. [cited 2020 Jul 4]; https://core.ac.uk/reader/38810346 .
Bolger N, Zuckerman A. A framework for studying personality in the stress process. J Pers Soc Psychol. 1995;69(5):890–902.
Connor-Smith JK, Flachsbart C. Relations between personality and coping: a meta-analysis. J Pers Soc Psychol. 2007;93(6):1080–107.
Busch IM, Moretti F, Purgato M, Barbui C, Wu AW, Rimondini M. Dealing with adverse events: a meta-analysis on second victims’ coping strategies. J Patient Saf. 2020;16(2):e51.
Billings AG, Moos RH. The role of coping responses and social resources in attenuating the stress of life events. J Behav Med. 1981;4(2):139–57.
Beck AT. Cognitive therapy and the emotional disorders. New York: Penguin; 1979.
Aldao A, Nolen-Hoeksema S, Schweizer S. Emotion-regulation strategies across psychopathology: a meta-analytic review. Clin Psychol Rev. 2010;30(2):217–37.
Satija YK, Advani GB, Nathawat SS. Influence of stressful life events and coping strategies in depression. Indian J Psychiatry. 1998;40(2):165–71.
Carver CS. You want to measure coping but your protocol’s too long: consider the brief COPE. Int J Behav Med. 1997;4(1):92–100.
Ross CE, Mirowsky J. Explaining the social patterns of depression: control and problem solving–or support and talking? J Health Soc Behav. 1989;30(2):206–19.
Nahlen Bose C, Bjorling G, Elfstrom ML, Persson H, Saboonchi F. Assessment of coping strategies and their associations with health related quality of life in patients with chronic heart failure: the brief COPE restructured. Cardiol Res. 2015;6(2):239–48.
Kliem S, Mößle T, Rehbein F, Hellmann DF, Zenger M, Brähler E. A brief form of the Perceived Social Support Questionnaire (F-SozU) was developed, validated, and standardized. J Clin Epidemiol. 2015;68(5):551–62.
Lin M, Hirschfeld G, Margraf J. Brief form of the Perceived Social Support Questionnaire (F-SozU K-6): Validation, norms, and cross-cultural measurement invariance in the USA, Germany, Russia, and China. Psychol Assess. 2019;31(5):609–21.
Soto CJ, John OP. The next Big Five Inventory (BFI-2): Developing and assessing a hierarchical model with 15 facets to enhance bandwidth, fidelity, and predictive power. J Pers Soc Psychol. 2017;113(1):117–43.
Russell D, Peplau LA, Cutrona CE. The revised UCLA Loneliness Scale: Concurrent and discriminant validity evidence. J Pers Soc Psychol. 1980;39(3):472–80.
Wright L, Steptoe A, Fancourt D. Are we all in this together? Longitudinal assessment of cumulative adversities by socioeconomic position in the first 3 weeks of lockdown in the UK. J Epidemiol Community Health. 2020;74:683–8.
PubMed Google Scholar
Wright L, Steptoe A, Fancourt D. How are adversities during COVID-19 affecting mental health? Differential associations for worries and experiences and implications for policy. Psychiatry Clin Psychol. 2020. https://doi.org/10.1101/2020.05.14.20101717 .
Population estimates for the UK, England and Wales, Scotland and Northern Ireland—Office for National Statistics. [cited 2020 May 13]. https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/bulletins/annualmidyearpopulationestimates/mid2018 .
Hainmueller J, Xu Y. ebalance: a Stata package for entropy balancing. J Stat Softw. 2013;54(1):1–18.
Panayiotou G, Kokkinos CM, Kapsou M. Indirect and direct associations between personality and psychological distress mediated by dispositional coping. J Psychol. 2014;148(5):549–67.
Frydenberg E, Lewis R. Boys play sport and girls turn to others: age, gender and ethnicity as determinants of coping. J Adolesc. 1993;16(3):253–66.
Chen Y, Peng Y, Xu H, O’Brien WH. Age differences in stress and coping: problem-focused strategies mediate the relationship between age and positive affect. Int J Aging Hum Dev. 2018;86(4):347–63.
Hamarat E, Thompson D, Aysan F, Steele D, Matheny K, Simons C. Age differences in coping resources and satisfaction with life among middle-aged, young-old, and oldest-old adults. J Genet Psychol. 2002;163(3):360–7.
Copeland EP, Hess RS. Differences in young adolescents’ coping strategies based on gender and ethnicity. J Early Adolesc. 1995;15(2):203–19.
Bhui K, King M, Dein S, O’Connor W. Ethnicity and religious coping with mental distress. J Ment Health. 2008;17(2):141–51.
Krueger PM, Chang VW. Being poor and coping with stress: health behaviors and the risk of death. Am J Public Health. 2008;98(5):889–96.
Restubog SLD, Ocampo ACG, Wang L. Taking control amidst the chaos: emotion regulation during the COVID-19 pandemic. J Vocat Behav. 2020;119:103440.
Diefendorff JM, Richard EM, Yang J. Linking emotion regulation strategies to affective events and negative emotions at work. J Vocat Behav. 2008;73(3):498–508.
Williamson V, Murphy D, Greenberg N. COVID-19 and experiences of moral injury in front-line key workers. Occup Med Lond. 2020. https://doi.org/10.1093/occmed/kqaa052/5814939 .
Greenberg N, Docherty M, Gnanapragasam S, Wessely S. Managing mental health challenges faced by healthcare workers during covid-19 pandemic. BMJ. 2020;368:m1211.
Banyard VL, Graham-Bermann SA. Surviving poverty: stress and coping in the lives of housed and homeless mothers. Am J Orthopsychiatry. 1998;68(3):479–89.
Wardell J, Kempe T, Rapinda KK, Single AN, Bilevicius E, Frohlich JR, et al. Drinking to cope during the COVID-19 pandemic: The role of external and internal stress-related factors in coping motive pathways to alcohol use, solitary drinking, and alcohol problems. PsyArXiv; 2020 Jun [cited 2020 Aug 6]. https://osf.io/8vfp9
Deckx L, van den Akker M, Buntinx F, van Driel M. A systematic literature review on the association between loneliness and coping strategies. Psychol Health Med. 2018;23(8):899–916.
Coyne JC, Downey G. Social factors and psychopathology: stress, social support, and coping processes. Annu Rev Psychol. 1991;42(1):401–25.
Roohafza HR, Afshar H, Keshteli AH, Mohammadi N, Feizi A, Taslimi M, et al. What’s the role of perceived social support and coping styles in depression and anxiety? J Res Med Sci. 2014;19(10):944–9.
Ben-Zur H. Coping styles and affect. Int J Stress Manag. 2009;16(2):87.
Compas BE, Jaser SS, Bettis AH, Watson KH, Gruhn MA, Dunbar JP, et al. Coping, emotion regulation, and psychopathology in childhood and adolescence: A meta-analysis and narrative review. Psychol Bull. 2017;143(9):939–91.
Lazarus RS. Stress and emotion: a new synthesis. New York: Springer; 1999.
Moore KA, March E. Socially Connected during COVID-19: Online social connections mediate the relationship between loneliness and positive coping strategies. in review; 2020 [cited 2020 Jul 5]. https://www.researchsquare.com/article/rs-35835/v1 .
Christmann CA, Hoffmann A, Bleser G. Stress management apps with regard to emotion-focused coping and behavior change techniques: a content analysis. JMIR Mhealth Uhealth. 2017;5(2):e22.
Dijkstra MTM, Homan AC. Engaging in rather than disengaging from stress: effective coping and perceived control. Front Psychol. 2016;7:1415.
Porter LC, DeMarco LM. Beyond the dichotomy: incarceration dosage and mental health*. Criminology. 2019;57(1):136–56.
Fancourt D, Steptoe A, Bu F. Trajectories of depression and anxiety during enforced isolation due to COVID-19: longitudinal analyses of 59,318 adults in the UK with and without diagnosed mental illness. medRxiv. 2020;2020.06.03.20120923.
Atal S, Cheng C. Socioeconomic health disparities revisited: coping flexibility enhances health-related quality of life for individuals low in socioeconomic status. Health Qual Life Outcomes. 2016;14:7.
Tomstad S, Dale B, Sundsli K, Sævareid HI, Söderhamn U. Who often feels lonely? A cross-sectional study about loneliness and its related factors among older home-dwelling people. Int J Older People Nurs. 2017;12(4):e12162.
Download references
Acknowledgements
We are very grateful to all participants in the COVID-19 Social Study.
This Covid-19 Social Study was funded by the Nuffield Foundation [WEL/FR-000022583], but the views expressed are those of the authors and not necessarily the Foundation. The study was also supported by the MARCH Mental Health Network funded by the Cross-Disciplinary Mental Health Network Plus initiative supported by UK Research and Innovation [ES/S002588/1], and by the Wellcome Trust [221400/Z/20/Z]. DF was funded by the Wellcome Trust [205407/Z/16/Z]. The researchers are grateful for the support of a number of organisations with their recruitment efforts including: the UKRI Mental Health Networks, Find Out Now, UCL BioResource, SEO Works, FieldworkHub, and Optimal Workshop. The study was also supported by HealthWise Wales, the Health and Car Research Wales initiative, which is led by Cardiff University in collaboration with SAIL, Swansea University. The funders had no final role in the study design; in the collection, analysis and interpretation of data; in the writing of the report; or in the decision to submit the paper for publication. All researchers listed as authors are independent from the funders and all final decisions about the research were taken by the investigators and were unrestricted.
Author information
Authors and affiliations.
Department of Behavioural Science and Health, University College London, 1-19 Torrington Place, London, WC1E 7HB, UK
Meg Fluharty & Daisy Fancourt
You can also search for this author in PubMed Google Scholar
Contributions
MF and DF developed the study concept. MF performed the data analysis and drafted the manuscript. DF provided critical revisions. All authors read and approved the final manuscript.
Authors’ information
Meg Fluharty is a Research Fellow in Statistics & Epidemiology at The Department of Behavioural Science and Health, University College London.
Daisy Fancourt is an Associate Professor of Psychobiology & Epidemiology at The Department of Behavioural Science and Health, University College London.
Corresponding author
Correspondence to Meg Fluharty .
Ethics declarations
Ethical approval and consent to participate.
Ethical approval for the COVID-19 Social Study was granted by the UCL Ethics Committee. All participants provided fully informed written consent. The study is GDPR compliant.
Consent for publication
Not applicable.
Competing interests
The authors declare they have no competing interests.
Additional information
Publisher's note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Additional file 1..
Provides demographic characterics (Table S1); comparison of origional and revised F-SozU K-6 Questionnaire (Table S2); full model results (Tables S3 & S4), and unweighted models (Tabled S5–S7).
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Fluharty, M., Fancourt, D. How have people been coping during the COVID-19 pandemic? Patterns and predictors of coping strategies amongst 26,016 UK adults. BMC Psychol 9 , 107 (2021). https://doi.org/10.1186/s40359-021-00603-9
Download citation
Received : 13 November 2020
Accepted : 21 June 2021
Published : 15 July 2021
DOI : https://doi.org/10.1186/s40359-021-00603-9
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
BMC Psychology
ISSN: 2050-7283
- General enquiries: [email protected]
Click through the PLOS taxonomy to find articles in your field.
For more information about PLOS Subject Areas, click here .
Loading metrics
Open Access
Peer-reviewed
Research Article
A count of coping strategies: A longitudinal study investigating an alternative method to understanding coping and adjustment
Roles Conceptualization, Formal analysis, Methodology, Project administration, Software, Validation, Visualization, Writing – original draft, Writing – review & editing
* E-mail: [email protected]
Affiliation Department of Psychology, Brock University, St. Catharines, Ontario, Canada
Roles Conceptualization, Data curation, Formal analysis, Funding acquisition, Investigation, Methodology, Project administration, Resources, Software, Supervision, Validation, Visualization, Writing – original draft, Writing – review & editing
- Taylor Heffer,
- Teena Willoughby

- Published: October 5, 2017
- https://doi.org/10.1371/journal.pone.0186057
- Reader Comments
Researchers recently have suggested that coping flexibility (i.e., an individual’s ability to modify and change coping strategies depending on the context) may be an important way to investigate coping. The availability of numerous coping strategies may be an important precursor to coping flexibility, given that flexibility can only be obtained if an individual is able to access and use different coping strategies. Typically, studies examining the use of coping strategies compute means-based analyses, which assess not only what strategies are used but also how much they are used. Thus, there is limited ability to differentiate between individuals who use a lot of strategies infrequently, and individuals who use only one or two strategies a lot. One way to address this confound is to count the number of strategies that an individual uses without attention to how frequently they use them (i.e., a count-based approach). The present longitudinal study compares a count-based model and a means-based model of coping and adjustment among undergraduates ( N = 1132). An autoregressive cross-lagged path analysis revealed that for the count-based approach, using a greater number of positive coping strategies led to more positive adjustment and less suicide ideation over time than using a smaller number of positive coping strategies. Further, engagement in a greater number of negative coping strategies predicted more depressive symptoms and poorer emotion regulation over time. In comparison, the means-based model revealed identical results for negative coping strategies; however, engagement in more frequent positive coping strategies did not predict better positive adjustment over time. Thus, a count-based approach offers a novel way to examine how the number of coping strategies that individuals use can help promote adjustment among university students.
Citation: Heffer T, Willoughby T (2017) A count of coping strategies: A longitudinal study investigating an alternative method to understanding coping and adjustment. PLoS ONE 12(10): e0186057. https://doi.org/10.1371/journal.pone.0186057
Editor: Scott McDonald, Hunter Holmes McGuire VA Medical Center, UNITED STATES
Received: August 17, 2016; Accepted: September 25, 2017; Published: October 5, 2017
Copyright: © 2017 Heffer, Willoughby. This is an open access article distributed under the terms of the Creative Commons Attribution License , which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Data Availability: All relevant data are available at: http://hdl.handle.net/10464/11163 .
Funding: This work was supported by Social Sciences and Humanities Research Council, Grant Number: 435-2014-1929 (TW). The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Competing interests: The authors have declared that no competing interests exist.
Introduction
For many students, attending university can be stressful and challenging [ 1 , 2 ]. Students often are faced with many demands (e.g., moving away from home, struggling with financial constraints, etc.) often without the close social support of family and friends that they experienced when living at home [ 3 , 4 ]. Importantly, accumulation of these daily stressors can impact students’ adjustment [ 2 , 5 , 6 ]. Indeed, the rates of suicide ideation and depressive symptoms among university students are alarming. In a study of 16,760 American undergraduates, 36.1% reported feeling so depressed in the past year that it was difficult to function and 10.3% seriously considered suicide—yet many students may not seek out or be aware of appropriate resources that are available to them [ 7 , 8 ]. Thus, managing these challenges places a reliance on students’ own ability to cope. The current study seeks to investigate how the number of coping strategies that individuals use may be associated with adjustment over time.
The transactional theory of coping posits that coping is an evolving process that changes in response to context, in an effort to manage different internal and external demands [ 9 ]. Accordingly, the transactional theory of coping presumes that successful coping involves an ability to adjust and change coping strategies in a way that facilitates positive outcomes.
With this in mind, current models of coping have focused on the idea of coping flexibility- a way of studying coping that identifies an individual’s ability to modify their coping behavior according to the nature of each stressful situation (see [ 10 ]).
The availability of numerous coping strategies when stressed may be an important precursor to coping flexibility—in order to demonstrate flexibility among a variety of coping strategies, individuals must first possess a diverse range of coping strategies that they are able to use when stressed [ 11 ]. Studies investigating the use of coping strategies typically compute means-based analyses whereby they not only investigate what strategies are used, but also how much (i.e., a little, a medium amount, a lot) each is used—a composite score then is computed based on the average frequency of use across all the strategies [ 12 – 15 ]. As a result, this approach is unable to differentiate between individuals who use a lot of strategies infrequently and individuals who use only one or two strategies a lot. For example, an individual who uses three coping strategies “a little” (scored as a 2 on the Likert scale) would have an identical mean to someone who indicates using two strategies “not at all” (scored as a 1) and a third strategy “a lot” (scored as a 4); both means would be 2. In other words, when using a means-based analysis, distinct coping patterns can present with identical means, limiting the conclusions that can be made regarding the relationship between the number of coping strategies used and adjustment. One way to address this confound is to count the number of strategies that an individual uses when stressed without attention to how frequently they use them (i.e., a count-based approach).
Regardless of approach (count or mean), it also is important to note that some strategies may not be advantageous, regardless of how well an individual is able to use that specific strategy [ 16 ]. For instance, consider a person who copes with different situations by blaming themselves, self-medicating through alcohol use, and seeking support; this person would not be expected to have a more favourable outcome compared to if they had just used only one strategy such as seeking support, given that self-blame and alcohol use are unlikely to help. Thus, adaptive coping may require an ability to use coping strategies that are at least relatively positive in nature. The current study examines this hypothesis by separating coping strategies based on positive and negative coping. In doing so, differential associations between adjustment and the count of positive strategies versus the count of negative coping strategies used can be assessed. Of note, however, there may be some instances where certain coping strategies may not be considered to be truly negative or positive (e.g., distraction coping may not help an individual succeed on an exam). Thus, we acknowledge that these terms may be oversimplified.
Coping and negative adjustment
Despite the potential benefits of using multiple strategies to cope with stress, doing this may be difficult for individuals experiencing poor adjustment. Two indicators of poor adjustment that are examined in the current study are depressive symptoms and suicide ideation. Importantly, individuals with high levels of depressive symptoms demonstrate a more negative attribution style (i.e., a stable and internalized attitude that unpleasant circumstances will persist) compared to their non-depressed peers ([ 17 , 18 ]; see [ 19 ] for a review). Thus, believing that nothing can be done to alter an aversive situation may discourage an individual from seeking out new positive ways to cope with problems.
In line with this idea, concurrent studies using a means-based approach have found that using more frequent negative coping strategies (e.g., self-blame) are associated with higher depressive symptoms [ 20 ]. Further, in a longitudinal investigation, Lee and colleagues [ 21 ] found that more frequent engagement in avoidant coping was associated with more depressive symptoms over time, although they only tested one direction—from coping to depressive symptoms over time (see also [ 22 ]). Thus, interpretation of these findings generally is that negative coping leads to more depressive symptoms over time. However, a longitudinal study testing bidirectionality is necessary before conclusions about the direction of effects can be ascertained.
Suicide ideation also is associated with how well individuals are able to cope with stress [ 23 – 26 ]. For example, findings from concurrent studies indicate that individuals with higher levels of suicide ideation engage in more frequent (calculated by a means-based approach) maladaptive coping strategies [ 23 , 25 ] and tend to have more trouble problem solving in the face of stress [ 27 ], compared to individuals with lower levels of suicide ideation. Thus, individuals who engage in more suicide ideation may have more difficulty accessing multiple productive coping strategies when faced with stress. But it also may be that individuals who use more negative coping strategies in the face of stress have higher suicide ideation over time- a longitudinal study testing both directions of the effects is required in order to address these hypotheses.
Overall, while there is evidence of a means-based association between coping and negative adjustment, less is known about whether these results are transferable when looking solely at the number of strategies individuals have available to them. Interestingly, researchers often suggest that one way to help decrease negative adjustment (e.g., depressive symptoms and suicide ideation) may be to reduce the number of negative coping strategies that individuals use. Yet, a direct test of this hypothesis has not been conducted. Research examining a count-based approach is necessary before concluding that the number of strategies that individuals use is associated with adjustment. In addition, the current study will investigate the direction of effects of these relations over time. For example, it may be that individuals who engage in a greater number of negative coping strategies when stressed report more depressive symptoms and suicide ideation over time than their peers. On the other hand, individuals who report depressive symptoms and suicide ideation at Time 1 may engage in a greater number of negative coping strategies over time. In fact, both possibilities may be true—the effect may be bidirectional. Thus, an important goal of the present study is to investigate the direction of effects of these relations for both positive and negative coping.
Coping and positive adjustment
A second objective of the current study is to investigate the relationship between coping and positive adjustment. Coping often is investigated in terms of its ability to decrease negative outcomes. The current study, however, seeks to investigate whether coping can also play an important role in increasing positive outcomes. Indeed, having a higher number of positive coping strategies available in the face of stress may provide the individual with more resources to deal with stress. This may allow an individual to manage stress more effectively and be more confident in their ability to deal with problems. There is less research directly investigating coping and positive adjustment than coping and negative adjustment, and the research that has been done generally is concurrent rather than longitudinal.
As adjustment can be examined in a variety of ways, in the present study we will focus on three indicators: emotion regulation, self-esteem and academic achievement. All three are associated with coping [ 28 – 30 ] and represent particularly important indicators of adjustment among students. One indicator of positive adjustment that is associated with coping is emotion regulation. Individuals who are better able to regulate their emotions and engage in more positive affect may be more likely to seek out and use a number of positive coping strategies. According to the broaden-and-build theory, the experience of positive emotions (e.g., joy) broadens attention and thinking (i.e., heightens openness to new possibilities, big picture focus, etc.), in comparison to negative emotions, which tend to result in a narrowing of focus (i.e., fight or flight, etc., [ 31 ]). This broadening of attention is hypothesized to build personal resources, such as adaptive coping strategies [ 32 ]. In light of this, individuals who are better able to regulate emotions in a more positive manner may have a heightened ability to think more broadly, allowing for engagement in a variety of positive coping strategies, compared to those who have more narrow thinking. Alternatively, it may be that individuals who engage in a greater number of positive coping strategies may have a greater sense of control, and demonstrate a greater ability to adjust their coping responses and adapt to stress. As a result, these individuals may become more proficient in their ability to regulate their emotions. Fredrickson [ 33 ] posits that both interpretations warrant investigation (i.e., bidirectionality) by emphasizing that experience of positive emotion should help facilitate a broader source of coping, which could help improve later experiences of positive emotions.
Another way that coping has been implicated in promotion of positive adjustment is in its association to self–esteem [ 21 ]. For instance, individuals with high self-esteem are thought to have more effective and appropriate coping resources available to deal with stress (e.g., planning and problem solving [ 34 ]. With regards to the count of coping strategies used, it could be that individuals with high self-esteem may be more confident in their ability to cope with different stressors (and thus be more likely to engage in a variety of positive coping strategies). It also may be, however, that individuals who are able to use a greater number of positive coping strategies may develop a sense of control and feelings of confidence in their ability to handle different situations appropriately, thus leading to increased self-esteem.
In addition, academic achievement may be another important factor associated with coping. Academic achievement typically requires an ability to work well under pressure (e.g., writing exams, oral presentations) as well as an ability to collaborate on group projects. The ability to cope efficiently and employ more frequent positive orientated strategies when under stress/pressure has been found to be associated with better academic achievement, compared to those who rely on less effective coping strategies [ 35 , 36 ]. Further, Zeidner [ 37 ] emphasizes that success on exams is associated with a combined use of multiple strategies (i.e., increase study time, seek support from friends. While associations have been found between academic achievement and use of effective coping strategies, less is known about the longitudinal association between academic achievement and a count of the number of coping strategies used.
The current study seeks to investigate relationships between positive adjustment and a count of the number of strategies individuals use. A count-based analysis will help to clarify if having a number of positive coping strategies available when stressed will be associated with positive adjustment over time. It also is necessary to use a longitudinal design in order to assess bidirectionality. As an example, interpretations of concurrent studies surrounding academic achievement imply that having better coping strategies leads to better academic achievement; it also could be, however, that the ability to succeed in an academic setting may help build confidence and lead to a broadening of focus which could help increase the use of a variety of coping strategies. The same issues with interpretations can be applied to emotion regulation and self-esteem, thus further longitudinal examination is required.
Stress as a moderator
While a key goal of the present study is to investigate bidirectionality, it is quite possible that the associations among these variables may differ depending on the individuals’ level of stress. For instance, coping is generally considered in the context of stress; thus if an individual is not experiencing stress, we might not expect them to apply and use a number of coping strategies compared to individuals who are experiencing stress [ 38 , 39 ]. Indeed, it may be that individuals who have a lot of different stressors in their life may benefit more from using a variety of strategies, compared to individuals who have few stressors.
The current study
There are three main research questions associated with this longitudinal study. First, how is a count-based approach associated with adjustment over time, and are these effects bidirectional? Although research using a means-based approach has provided evidence for associations between coping and adjustment, little work has used a count-based approach or used this approach with a longitudinal design. We predict that using a greater number of positive coping strategies when stressed might be associated with better adjustment (i.e., less depressive symptoms, less suicide ideation, more self-esteem, better emotion regulation and higher academic achievement) over time than using a smaller number of positive coping strategies. We also expect that using a higher number of negative strategies will be associated with poorer adjustment (e.g., greater depressive symptoms, and higher suicide ideation) than using a smaller number of negative coping strategies. Given the lack of research, it is not clear whether using a greater number of negative coping strategies will be associated with poorer self esteem, emotion regulation and academic achievement over time. Further, the analyses examining bidirectionality in these associations over time are exploratory.
Second, the current study offers a comparison of a count-based approach and a means-based approach to studying coping and adjustment. Given that a counts-based model does not take into consideration how much individuals use each strategy and only examines the number of coping strategies individuals use, it also would be beneficial to compare this model to a means-based model that takes both of these factors into consideration. In doing so, differential associations between the two models can be compared in order to address the ways in which a count-based approach may be an alternative method to studying coping.
A third purpose of this study is to investigate whether stress is an important moderator of the association between coping (for both the count-based and the means-based methods) and adjustment. Additionally, all analyses controlled for sex and parental education given research suggesting that these variables are associated with coping and adjustment [ 40 – 42 ].
Participants
The current sample of 1,132 (70.5% female) first-year undergraduate students ( M age = 19.06, SD = .92) from a mid-sized Canadian university was drawn from a larger longitudinal study examining adjustment in university. In total, 87.5% of the participants were born in Canada. Consistent with the broader demographics for the region; the most common ethnic backgrounds endorsed other than Canadian were British (19%), Italian (16.8%), French (9.5%) and German (9%; [ 43 ]). Data on socioeconomic status indicated mean levels of parental education falling between “some college, university or apprenticeship program” and “completed a college/ apprenticeship/ technical diploma.”
Missing data occurred within each assessment time point because some students did not finish the entire questionnaire (average missing data = 1.8%) and because some students did not complete both waves of the data. Out of the original sample that completed the survey at Time 1, 73.1% completed Time 2 of the survey. The overall multivariate test for missingness was significant, Λ = .941, F (9, 1010) = 7.017, p < .001, η 2 = .059. Participants who were missing at the second time point were not significantly different from participants who were there at both time points, with two exceptions. Specifically, those who completed both waves of the study were more likely to be females and to have higher grades compared to those who only completed one wave of the study ( p s < .001). Missing values were imputed using the expectation–maximization algorithm (EM; iterations = 200) with all study measures included in the analysis, thus avoiding the biased parameter estimates that can occur with pairwise deletion, list-wise deletion or means substitution [ 44 ].
First-year university students were invited to participate in the survey examining factors related to stress and adjustment. The study was advertised by way of posters, emails, classroom announcements, website posting, and residence visits. Students could participate regardless of academic major, and were given monetary compensation or course credit for their participation. Only students who completed the first wave were invited (by email and/or phone) to participate again in the second wave. The Social Science Research Ethics Board approved the study (Ethics Approval Number: 09–118) and all participants provided informed written consent. Trained research assistants administered the survey. To ensure the safety of our participants a full debriefing was provided at the end of the survey and a list was given of both available mental health resources and researcher contact information. Participants also were given the opportunity during the survey to provide their contact information so that they could be contacted by a mental health professional if they were experiencing any distress.
Demographics.
Sex and parental education (one item per parent, scale ranged from 1 ( did not finish high school ) to 6 ( professional degree ), averaged for participants reporting on both parents; r = .40) were assessed at Time 1.
Coping was assessed using a shortened version of the Brief COPE (15 items) at Time 1 and then again one year later at Time 2 [ 45 ]. The Brief COPE includes positive and negative coping strategies. In order to differentiate between these positive and negative coping strategies, a principal components factor analysis with direct oblimin rotation was conducted using the data from Time 1. Four components emerged with eigenvalues > 1. Factor 2 was comprised of four negative coping items that hung together (i.e., self-blame, self-criticism, alcohol use, and giving up; eigenvalues = 2.73) with factor loadings ranging from 0.63 to 0.77. These items thus were included in the count of negative coping strategies. The three remaining factors reflected different subtypes of positive coping strategies such as religion (e.g., I pray or meditate), seeking support (e.g., I get emotional support from others), and reframing/humor (e.g., I look for something good in what is happening). Indeed, previous research has found that positive adjustment is associated with positive reframing and humor [ 46 ], seeking support [ 47 ] as well as religious coping strategies (see [ 48 ]). As the focus of this study was to investigate how many strategies individuals have access to using (regardless of the subtype of positive strategies), the items from the three remaining factors were grouped together in order to create the count of positive coping strategies (see S1 Table for more information on the factors).
When filling out the coping measure, participants were asked to indicate what they do when under a lot of stress on a scale ranging from 1 ( I usually don’t do this at all ) to 4 ( I usually do this a lot ). In order to create a count of how many strategies individuals use when stressed, the items were recoded such that that 0 represented not using the strategy (i.e., I usually don’t do this at all ), while 1 represented using the strategy to any degree (i.e., I usually do this a little bit , I usually do this a medium amount , I usually do this a lot ).
The count of negative coping strategies was created by counting the number of negative strategies individuals use when stressed (e.g., “I blame myself”, “I use alcohol and other drugs to make myself feel better,” etc.). An average of these strategies (based on the original items with the four-point scale) was also created and used in the means-based approach. Cronbach’s alpha was .68 at Time 1 and .72 at Time 2. The count of positive coping strategies was assessed by counting the number of positive strategies individuals use when stressed (e.g., “I get comfort and understanding from someone,” “I look for something good in what is happening” etc.). An average of these strategies (based on the original items with the four-point scale) was also created and used in the means-based approach. Cronbach’s alpha was .76 at Time 1 and .74 at Time 2. The Brief COPE has been shown to have good internal consistency and validity in previous research [ 45 ].
Depressive symptoms.
Participants completed The Center for Epidemiological Studies Depression Scale at Time 1 and Time 2 in order to assess their level of depressive symptoms (CES-D Scale; [ 49 ]; e.g., “I felt lonely” and “My sleep was restless”). Individuals indicated on a scale of 1 ( none of the time ) to 5 ( most of the time ) how often they experienced 20 symptoms associated with depression. Cronbach’s alpha in the present study was .91 at Time 1 and .92 at Time 2.
Suicide ideation.
Suicide ideation in the past year was assessed at Time 1 and Time 2 using a question from the Suicide Behaviors Questionnaire-Revised (SBQR; [ 50 ]; “How often have you thought about killing yourself in the past year?”). This item was rated using a 5-point scale that ranged from 1 ( never ) to 5 ( very often ). The SBQR has been shown to have good internal consistency and validity in previous research [ 50 ].
Self esteem.
Self-esteem was measured at Time 1 and Time 2 using the Rosenberg Self-Esteem Scale [ 51 ]. The measure included 10 items (e.g., “I take a positive attitude toward myself”) that were rated on a scale from 1 ( strongly disagree ) to 5 ( strongly agree ). Cronbach’s alpha was .904 at Time 1 and .916 at Time 2.
Academic achievement.
Academic achievement was measured at both Time 1 and Time 2 using students’ academic average for the corresponding year, recorded in percentages (e.g., 70%). Information was obtained from the University Registrar with the participants’ permission.
Emotion regulation.
Emotion regulation was assessed at both Time 1 and Time 2 using 6 items from the Difficulties in Emotion Regulation (DERS; [ 52 ]); e.g., ‘‘When I’m upset or stressed, I have difficulty concentrating”). The responses were based on a five-point Likert scale ranging from 1 ( almost never ) to 5 ( almost always ). The scale was recoded so that higher scores indicated better emotion regulation. Cronbach’s alphas at Time 1 and Time 2 were .73 and .74, respectively.
Stress was measured using The Daily Hassles Scale. Participants indicated how bothered they felt by 25 daily hassles. Hassles related to daily life stressors such as peer conflict, family, school and money (e.g., “Being lonely” and “Not having enough time”). Responses were rated on a scale from 1 ( almost never bothers me ) to 3 ( often bothers me ). Cronbach’s alpha for these 25 items was .84.
Preliminary analyses
The means and standard deviations of all study variables are outlined in Table 1 . All variables demonstrated acceptable levels of skewness and kurtosis with the exception of suicide ideation, which was transformed using the log-likelihood method to correct for non-normality. There was a significant main effect of sex on the number of positive coping strategies used, with females reporting using a greater number of positive coping strategies than males at both Time 1 and Time 2, p s < .004. Females also reported having more depressive symptoms than males at Time 1, p < .001, and higher academic achievement at Time 2, p = .006, than males. In contrast, males were significantly more likely to have better emotion regulation than females at both Time 1 and Time 2, ps < .001. At Time 2, males were more likely to engage in a greater number of negative coping strategies, p = .027, and also reported higher suicide ideation, p = .014, than females. There were no significant differences on parental education, p > .05.
- PPT PowerPoint slide
- PNG larger image
- TIFF original image
https://doi.org/10.1371/journal.pone.0186057.t001
Primary analyses
The primary statistical analyses were carried out using an auto-regressive cross-lagged path analysis in MPlus 7. Two models were run, a count-based model and a means-based model. The models were comprised of seven variables measured over 2 years: positive coping strategies, negative coping strategies, depressive symptoms, suicide ideation, academic achievement, emotion regulation, and self-esteem (see Figs 1 and 2 ). Across the two time periods, we included cross-lag paths among all seven key study variables, autoregressive paths (i.e., within each variable), and concurrent associations among all variables within each wave. Sex and parental education also were included as covariates, such that correlations were specified between each of the covariates and each variable at Time 1 and paths were estimated between the covariates and each variable at Time 2. Any significant path, therefore, accounted for covariates, previous scores on the outcome variables, correlations among variables within a wave, as well as any other predictors in the model (i.e., estimating the unique relation between study variables). Significant paths among the seven key study variables for both models (count-based and means-based) are depicted in Figs 1 and 2 (see S2 and S3 Tables for full results among key variables). Model fit was not relevant given that the models were saturated.
Numbers 1 and 2 indicate Time 1 and Time 2, respectively. Values indicate standardized beta weights (standard errors are in parenthesis). Pos = Positive, Neg = Negative.
https://doi.org/10.1371/journal.pone.0186057.g001
https://doi.org/10.1371/journal.pone.0186057.g002
The following results for the paths related to coping were consistent across both the count-based model and the means-based model (See Figs 1 and 2 as well as S2 and S3 Tables for specific path results as well as all results among adjustment indicators). There was a bidirectional association between the use of negative coping strategies and depressive symptoms, such that using more (as measured by a count and a mean) negative coping strategies at Time 1 was associated with higher depressive symptoms at Time 2, and depressive symptoms at Time 1 were positively associated with more engagement in negative coping strategies at Time 2. There also was a unidirectional association found between the use of negative coping and emotion regulation; specifically, using less negative coping strategies (as measured by a count and a mean) at Time 1 was associated with better emotion regulation at Time 2.
Critically, some results were not consistent among the two models. For the count-based model, using a greater number of positive coping strategies at Time 1 was associated with less suicide ideation, engagement in fewer negative coping strategies, higher self-esteem, as well as higher academic achievement one year later. There was also a bidirectional association between the number of positive coping strategies used and emotion regulation. Using a greater number of positive coping strategies at Time 1 was associated with better emotion regulation at Time 2, and better emotion regulation at Time 1 was associated with use of a greater number of positive coping strategies at Time 2.
For the means-based analysis, in addition to the overlapping findings among both models, there also was a unidirectional association found between positive coping and emotion regulation, such that better emotion regulation at Time 1 was associated with more positive coping (means-based) at Time 2. Further, there was a unidirectional association between academic achievement and negative coping. Specifically, higher academic achievement at Time 1 was associated with less negative coping (means-based) at Time 2.
We assessed whether stress was a significant moderator of the pattern of results in both the count-based and means-based models. Stress was categorized into two equal percentiles (50% each) encompassing higher versus lower daily stress. The Chi-Square Difference Test of Relative Fit was not significant for either the count model, χ 2 diff (42) = 45.516, p = .292, or the means-based model χ 2 diff (42) = 42.727, p = .439, indicating that the pattern of associations for both models was not different between people with lower stress compared to people with higher stress. We also assessed whether stress might be a significant moderator if we only included individuals who scored at the more extreme ends of stress (bottom 33% vs top 33%). Consistent with the previous result, the Chi-Square Difference Test of Relative Fit was not significant for either the count-based model, χ 2 diff (42) = 25.439, p = .980 or for the means-based model χ 2 diff (42) = 27.275, p = .961. Overall, these results reveal that stress does not appear to be a moderator of the pattern of results between coping and adjustment.
A large volume of research has been conducted on coping, stress, and adjustment [ 53 ]. In line with the transactional theory of coping, coping flexibility is an important way of studying coping that accounts for an individual’s ability to adjust and change coping styles in response to different internal and external demands [ 9 ]. Importantly, the availability of numerous coping strategies may be an important precursor to coping flexibility, given that flexibility may only be obtained if an individual is able to access and use different coping strategies [ 11 ]. Studies that have investigated the use of coping strategies, however, typically compute a means-based analysis—an approach that does not allow for differentiation between individuals who use a lot of strategies infrequently and individuals who use only one or two strategies a lot. In order to address this limitation, the current study created a count-based measure of coping, whereby the number of strategies that an individual uses was counted without attention to how frequently they use them.
The focus of the present study was to investigate the relationship between a count-based approach to coping and adjustment. Critically, using a greater number of positive coping strategies was associated with better adjustment (e.g., less suicide ideation, using a fewer number of negative coping strategies, higher self-esteem and better academic achievement) over time. Of note, this finding was not true for the means-based analysis. This is an important finding as it suggests that encouraging students to use a greater number of positive coping strategies can not only help to decrease negative adjustment, but also aid in promoting positive adjustment.
In terms of bidirectionality, there was a bidirectional relationship between using a greater number of negative coping strategies and more depressive symptoms. This finding is in line with the research suggesting that individuals with depression may have a more negative attribution style and thus may be more likely to use strategies such as giving up. Additionally, using these types of negative coping strategies predicted more depressive symptoms over time. In line with the broaden-and-build theory, a bidirectional association also was found between emotion regulation and the number of positive coping strategies used when stressed. Our results suggest that emotion regulation may be a distinct way to help broaden an individual’s positive coping resources when stressed, and in turn, individuals who use a greater amount of positive coping strategies when stressed may be better able to regulate their emotions in a more positive manner.
Another goal of the current study was to compare a means-based approach to a counts-based approach. Overall, it appears that the count-based approach offers similar findings to the means-based approach in terms of negative coping. The count-based approach, however, provided additional findings that suggest that using a greater number of positive coping strategies may be distinctly important for promoting positive adjustment as well as decreasing negative adjustment. Further research is needed to investigate why using a greater number of positive coping strategies may be adaptive. For instance, it could be that having more resources available or alternative ways to deal with stress allows individuals to deal with problems more effectively. It also is important for future research to identify the factors that lead some individuals to use more coping strategies than their peers (e.g., access to role models, higher executive functioning and planning skills, openness to experience, etc.). In addition, future research would benefit from identifying if there are differences between the number of strategies individuals think they might use in a situation (e.g., using hypothetical scenarios) compared to the number of strategies that they actually use when faced with stress. This would help identify whether individuals have certain strategies available but do not use them. Studies addressing these issues could help inform interventions aimed at teaching individuals how to use a variety of positive coping strategies as a way to promote adjustment.
The current study also found that stress was not a significant moderator of the relation between coping strategies and adjustment. This finding suggests that the using a greater number of positive coping strategies as well as using less negative coping strategies (lower average and a fewer number of negative strategies) may be beneficial for people with either high or low stress. Thus, even if an individual does not have a lot of stress in their life, it is still beneficial to have a greater number of positive coping strategies available to deal with problems effectively.
This study has important strengths, including a large sample, multiple indicators of adjustment, as well as being the first longitudinal study to offer a comparison between a means-based approach and a count-based approach to coping and adjustment. At the same time, the study has several limitations. First, generalizability is limited due to a predominantly Caucasian sample of university students. Second, the measure of stress comes from a self-report questionnaire of daily hassles. Thus, this measure is targeting more minor daily stressors, compared to major or severe stressors. It is worth noting, however, research findings emphasize the importance of cumulative daily stress/hassles in the role of negative adjustment [ 54 , 55 ]. Nonetheless, future research may benefit from investigating if the relationship between the number of coping strategies used and adjustment is more prominent among individuals facing major stressors. Another limitation is that coping was assessed via retrospective reports. It would be valuable for future research to assess these constructs in real time through techniques such as ecological moment sampling (e.g., daily diaries). Of note, the current study was unable to assess how coping may change depending on the situational context. Admittedly, it would be extremely difficult to evaluate and account for varying subjective stressors, as well as dispositional and environmental factors, in order to identify an objective measure of how coping may be adaptive in response to specific contexts [ 56 ]. Future research is needed to help disentangle how context may play a role in the relationship between a count of coping strategies used and adjustment.
In conclusion, the present study helps to elucidate the associations between adjustment and two methods of investigating coping over time. Understanding coping behaviours over time can help researchers and practitioners implement programs to improve coping efficiency and adjustment. Studies that investigate only a means-based approach are unable to differentiate between individuals who use one or two strategies a lot as opposed to those who use multiple strategies infrequently. Thus, a count-based method offers an innovative and practical way to implement interventions that could focus on teaching individuals to use a larger variety of coping strategies. Indeed, using a greater number of positive coping strategies is associated with less use of negative coping strategies, less suicide ideation, as well as higher self-esteem, emotion regulation, and academic achievement over time. Further, decreasing the ways in which individuals use negative coping strategies (average and count), can help to decrease depressive symptoms as well as increase emotion regulation over time. Given that university students report alarming rates of depressive symptoms and suicide ideation [ 8 ], there is a strong need for research investigating ways to decrease mental health problems as well as promote more positive adjustment.
Supporting information
S1 table. exploratory factor analysis..
https://doi.org/10.1371/journal.pone.0186057.s001
S2 Table. Autoregressive cross-lagged results for the count-based model.
https://doi.org/10.1371/journal.pone.0186057.s002
S3 Table. Autoregressive cross-lagged results for the means-based model.
https://doi.org/10.1371/journal.pone.0186057.s003
- View Article
- PubMed/NCBI
- Google Scholar
- 5. Kadison R, DiGeronimo TF. College of the overwhelmed: Campus mental health crisis and what to do about it. Vol. 46. New York: Wiley; 2004. 556–558 p.
- 8. American College Health Association. American College Health Association- National College Health Assessment II: Reference Group Executive Summary Fall 2015. Hanover, MD; 2015.
- 43. Statistics Canada. Population by selected ethnic origins [on-line]. [Internet]. http://www40.statcan.ca/l01/cst01/demo27i-eng.htm . 2006. http://www.statcan.gc.ca/tables-tableaux/sum-som/l01/cst01/demo27i-eng.htm
- 50. Osman A. Suicide Behavior Questionnaire-Revised (SBQ-R). University of Northern Iowa, Department of Psychology. 2002.
- Tools and Resources
- Customer Services
- Affective Science
- Biological Foundations of Psychology
- Clinical Psychology: Disorders and Therapies
- Cognitive Psychology/Neuroscience
- Developmental Psychology
- Educational/School Psychology
- Forensic Psychology
- Health Psychology
- History and Systems of Psychology
- Individual Differences
- Methods and Approaches in Psychology
- Neuropsychology
- Organizational and Institutional Psychology
- Personality
- Psychology and Other Disciplines
- Social Psychology
- Sports Psychology
- Share Facebook LinkedIn Twitter
Article contents
Work, stress, coping, and stress management.
- Sharon Glazer Sharon Glazer University of Baltimore
- , and Cong Liu Cong Liu Hofstra University
- https://doi.org/10.1093/acrefore/9780190236557.013.30
- Published online: 26 April 2017
Work stress refers to the process of job stressors, or stimuli in the workplace, leading to strains, or negative responses or reactions. Organizational development refers to a process in which problems or opportunities in the work environment are identified, plans are made to remediate or capitalize on the stimuli, action is taken, and subsequently the results of the plans and actions are evaluated. When organizational development strategies are used to assess work stress in the workplace, the actions employed are various stress management interventions. Two key factors tying work stress and organizational development are the role of the person and the role of the environment. In order to cope with work-related stressors and manage strains, organizations must be able to identify and differentiate between factors in the environment that are potential sources of stressors and how individuals perceive those factors. Primary stress management interventions focus on preventing stressors from even presenting, such as by clearly articulating workers’ roles and providing necessary resources for employees to perform their job. Secondary stress management interventions focus on a person’s appraisal of job stressors as a threat or challenge, and the person’s ability to cope with the stressors (presuming sufficient internal resources, such as a sense of meaningfulness in life, or external resources, such as social support from a supervisor). When coping is not successful, strains may develop. Tertiary stress management interventions attempt to remediate strains, by addressing the consequence itself (e.g., diabetes management) and/or the source of the strain (e.g., reducing workload). The person and/or the organization may be the targets of the intervention. The ultimate goal of stress management interventions is to minimize problems in the work environment, intensify aspects of the work environment that create a sense of a quality work context, enable people to cope with stressors that might arise, and provide tools for employees and organizations to manage strains that might develop despite all best efforts to create a healthy workplace.
- stress management
- organization development
- organizational interventions
- stress theories and frameworks
Introduction
Work stress is a generic term that refers to work-related stimuli (aka job stressors) that may lead to physical, behavioral, or psychological consequences (i.e., strains) that affect both the health and well-being of the employee and the organization. Not all stressors lead to strains, but all strains are a result of stressors, actual or perceived. Common terms often used interchangeably with work stress are occupational stress, job stress, and work-related stress. Terms used interchangeably with job stressors include work stressors, and as the specificity of the type of stressor might include psychosocial stressor (referring to the psychological experience of work demands that have a social component, e.g., conflict between two people; Hauke, Flintrop, Brun, & Rugulies, 2011 ), hindrance stressor (i.e., a stressor that prevents goal attainment; Cavanaugh, Boswell, Roehling, & Boudreau, 2000 ), and challenge stressor (i.e., a stressor that is difficult, but attainable and possibly rewarding to attain; Cavanaugh et al., 2000 ).
Stress in the workplace continues to be a highly pervasive problem, having both direct negative effects on individuals experiencing it and companies paying for it, and indirect costs vis à vis lost productivity (Dopkeen & DuBois, 2014 ). For example, U.K. public civil servants’ work-related stress rose from 10.8% in 2006 to 22.4% in 2013 and about one-third of the workforce has taken more than 20 days of leave due to stress-related ill-health, while well over 50% are present at work when ill (French, 2015 ). These findings are consistent with a report by the International Labor Organization (ILO, 2012 ), whereby 50% to 60% of all workdays are lost due to absence attributed to factors associated with work stress.
The prevalence of work-related stress is not diminishing despite improvements in technology and employment rates. The sources of stress, such as workload, seem to exacerbate with improvements in technology (Coovert & Thompson, 2003 ). Moreover, accessibility through mobile technology and virtual computer terminals is linking people to their work more than ever before (ILO, 2012 ; Tarafdar, Tu, Ragu-Nathan, & Ragu-Nathan, 2007 ). Evidence of this kind of mobility and flexibility is further reinforced in a June 2007 survey of 4,025 email users (over 13 years of age); AOL reported that four in ten survey respondents reported planning their vacations around email accessibility and 83% checked their emails at least once a day while away (McMahon, 2007 ). Ironically, despite these mounting work-related stressors and clear financial and performance outcomes, some individuals are reporting they are less “stressed,” but only because “stress has become the new normal” (Jayson, 2012 , para. 4).
This new normal is likely the source of psychological and physiological illness. Siegrist ( 2010 ) contends that conditions in the workplace, particularly psychosocial stressors that are perceived as unfavorable relationships with others and self, and an increasingly sedentary lifestyle (reinforced with desk jobs) are increasingly contributing to cardiovascular disease. These factors together justify a need to continue on the path of helping individuals recognize and cope with deleterious stressors in the work environment and, equally important, to find ways to help organizations prevent harmful stressors over which they have control, as well as implement policies or mechanisms to help employees deal with these stressors and subsequent strains. Along with a greater focus on mitigating environmental constraints are interventions that can be used to prevent anxiety, poor attitudes toward the workplace conditions and arrangements, and subsequent cardiovascular illness, absenteeism, and poor job performance (Siegrist, 2010 ).
Even the ILO has presented guidance on how the workplace can help prevent harmful job stressors (aka hindrance stressors) or at least help workers cope with them. Consistent with the view that well-being is not the absence of stressors or strains and with the view that positive psychology offers a lens for proactively preventing stressors, the ILO promotes increasing preventative risk assessments, interventions to prevent and control stressors, transparent organizational communication, worker involvement in decision-making, networks and mechanisms for workplace social support, awareness of how working and living conditions interact, safety, health, and well-being in the organization (ILO, n.d. ). The field of industrial and organizational (IO) psychology supports the ILO’s recommendations.
IO psychology views work stress as the process of a person’s interaction with multiple aspects of the work environment, job design, and work conditions in the organization. Interventions to manage work stress, therefore, focus on the psychosocial factors of the person and his or her relationships with others and the socio-technical factors related to the work environment and work processes. Viewing work stress from the lens of the person and the environment stems from Kurt Lewin’s ( 1936 ) work that stipulates a person’s state of mental health and behaviors are a function of the person within a specific environment or situation. Aspects of the work environment that affect individuals’ mental states and behaviors include organizational hierarchy, organizational climate (including processes, policies, practices, and reward structures), resources to support a person’s ability to fulfill job duties, and management structure (including leadership). Job design refers to each contributor’s tasks and responsibilities for fulfilling goals associated with the work role. Finally, working conditions refers not only to the physical environment, but also the interpersonal relationships with other contributors.
Each of the conditions that are identified in the work environment may be perceived as potentially harmful or a threat to the person or as an opportunity. When a stressor is perceived as a threat to attaining desired goals or outcomes, the stressor may be labeled as a hindrance stressor (e.g., LePine, Podsakoff, & Lepine, 2005 ). When the stressor is perceived as an opportunity to attain a desired goal or end state, it may be labeled as a challenge stressor. According to LePine and colleagues’ ( 2005 ), both challenge (e.g., time urgency, workload) and hindrance (e.g., hassles, role ambiguity, role conflict) stressors could lead to strains (as measured by “anxiety, depersonalization, depression, emotional exhaustion, frustration, health complaints, hostility, illness, physical symptoms, and tension” [p. 767]). However, challenge stressors positively relate with motivation and performance, whereas hindrance stressors negatively relate with motivation and performance. Moreover, motivation and strains partially mediate the relationship between hindrance and challenge stressors with performance.
Figure 1. Organizational development frameworks to guide identification of work stress and interventions.
In order to (1) minimize any potential negative effects from stressors, (2) increase coping skills to deal with stressors, or (3) manage strains, organizational practitioners or consultants will devise organizational interventions geared toward prevention, coping, and/or stress management. Ultimately, toxic factors in the work environment can have deleterious effects on a person’s physical and psychological well-being, as well as on an organization’s total health. It behooves management to take stock of the organization’s health, which includes the health and well-being of its employees, if the organization wishes to thrive and be profitable. According to Page and Vella-Brodrick’s ( 2009 ) model of employee well-being, employee well-being results from subjective well-being (i.e., life satisfaction and general positive or negative affect), workplace well-being (composed of job satisfaction and work-specific positive or negative affect), and psychological well-being (e.g., self-acceptance, positive social relations, mastery, purpose in life). Job stressors that become unbearable are likely to negatively affect workplace well-being and thus overall employee well-being. Because work stress is a major organizational pain point and organizations often employ organizational consultants to help identify and remediate pain points, the focus here is on organizational development (OD) frameworks; several work stress frameworks are presented that together signal areas where organizations might focus efforts for change in employee behaviors, attitudes, and performance, as well as the organization’s performance and climate. Work stress, interventions, and several OD and stress frameworks are depicted in Figure 1 .
The goals are: (1) to conceptually define and clarify terms associated with stress and stress management, particularly focusing on organizational factors that contribute to stress and stress management, and (2) to present research that informs current knowledge and practices on workplace stress management strategies. Stressors and strains will be defined, leading OD and work stress frameworks that are used to organize and help organizations make sense of the work environment and the organization’s responsibility in stress management will be explored, and stress management will be explained as an overarching thematic label; an area of study and practice that focuses on prevention (primary) interventions, coping (secondary) interventions, and managing strains (tertiary) interventions; as well as the label typically used to denote tertiary interventions. Suggestions for future research and implications toward becoming a healthy organization are presented.
Defining Stressors and Strains
Work-related stressors or job stressors can lead to different kinds of strains individuals and organizations might experience. Various types of stress management interventions, guided by OD and work stress frameworks, may be employed to prevent or cope with job stressors and manage strains that develop(ed).
A job stressor is a stimulus external to an employee and a result of an employee’s work conditions. Example job stressors include organizational constraints, workplace mistreatments (such as abusive supervision, workplace ostracism, incivility, bullying), role stressors, workload, work-family conflicts, errors or mistakes, examinations and evaluations, and lack of structure (Jex & Beehr, 1991 ; Liu, Spector, & Shi, 2007 ; Narayanan, Menon, & Spector, 1999 ). Although stressors may be categorized as hindrances and challenges, there is not yet sufficient information to be able to propose which stress management interventions would better serve to reduce those hindrance stressors or to reduce strain-producing challenge stressors while reinforcing engagement-producing challenge stressors.
Organizational Constraints
Organizational constraints may be hindrance stressors as they prevent employees from translating their motivation and ability into high-level job performance (Peters & O’Connor, 1980 ). Peters and O’Connor ( 1988 ) defined 11 categories of organizational constraints: (1) job-related information, (2) budgetary support, (3) required support, (4) materials and supplies, (5) required services and help from others, (6) task preparation, (7) time availability, (8) the work environment, (9) scheduling of activities, (10) transportation, and (11) job-relevant authority. The inhibiting effect of organizational constraints may be due to the lack of, inadequacy of, or poor quality of these categories.
Workplace Mistreatment
Workplace mistreatment presents a cluster of interpersonal variables, such as interpersonal conflict, bullying, incivility, and workplace ostracism (Hershcovis, 2011 ; Tepper & Henle, 2011 ). Typical workplace mistreatment behaviors include gossiping, rude comments, showing favoritism, yelling, lying, and ignoring other people at work (Tepper & Henle, 2011 ). These variables relate to employees’ psychological well-being, physical well-being, work attitudes (e.g., job satisfaction and organizational commitment), and turnover intention (e.g., Hershcovis, 2011 ; Spector & Jex, 1998 ). Some researchers differentiated the source of mistreatment, such as mistreatment from one’s supervisor versus mistreatment from one’s coworker (e.g., Bruk-Lee & Spector, 2006 ; Frone, 2000 ; Liu, Liu, Spector, & Shi, 2011 ).
Role Stressors
Role stressors are demands, constraints, or opportunities a person perceives to be associated, and thus expected, with his or her work role(s) across various situations. Three commonly studied role stressors are role ambiguity, role conflict, and role overload (Glazer & Beehr, 2005 ; Kahn, Wolfe, Quinn, Snoek, & Rosenthal, 1964 ). Role ambiguity in the workplace occurs when an employee lacks clarity regarding what performance-related behaviors are expected of him or her. Role conflict refers to situations wherein an employee receives incompatible role requests from the same or different supervisors or the employee is asked to engage in work that impedes his or her performance in other work or nonwork roles or clashes with his or her values. Role overload refers to excessive demands and insufficient time (quantitative) or knowledge (qualitative) to complete the work. The construct is often used interchangeably with workload, though role overload focuses more on perceived expectations from others about one’s workload. These role stressors significantly relate to low job satisfaction, low organizational commitment, low job performance, high tension or anxiety, and high turnover intention (Abramis, 1994 ; Glazer & Beehr, 2005 ; Jackson & Schuler, 1985 ).
Excessive workload is one of the most salient stressors at work (e.g., Liu et al., 2007 ). There are two types of workload: quantitative and qualitative workload (LaRocco, Tetrick, & Meder, 1989 ; Parasuraman & Purohit, 2000 ). Quantitative workload refers to the excessive amount of work one has. In a summary of a Chartered Institute of Personnel & Development Report from 2006 , Dewe and Kompier ( 2008 ) noted that quantitative workload was one of the top three stressors workers experienced at work. Qualitative workload refers to the difficulty of work. Workload also differs by the type of the load. There are mental workload and physical workload (Dwyer & Ganster, 1991 ). Excessive physical workload may result in physical discomfort or illness. Excessive mental workload will cause psychological distress such as anxiety or frustration (Bowling & Kirkendall, 2012 ). Another factor affecting quantitative workload is interruptions (during the workday). Lin, Kain, and Fritz ( 2013 ) found that interruptions delay completion of job tasks, thus adding to the perception of workload.
Work-Family Conflict
Work-family conflict is a form of inter-role conflict in which demands from one’s work domain and one’s family domain are incompatible to some extent (Greenhaus & Beutell, 1985 ). Work can interfere with family (WIF) and/or family can interfere with work (FIW) due to time-related commitments to participating in one domain or another, incompatible behavioral expectations, or when strains in one domain carry over to the other (Greenhaus & Beutell, 1985 ). Work-family conflict significantly relates to work-related outcomes (e.g., job satisfaction, organizational commitment, turnover intention, burnout, absenteeism, job performance, job strains, career satisfaction, and organizational citizenship behaviors), family-related outcomes (e.g., marital satisfaction, family satisfaction, family-related performance, family-related strains), and domain-unspecific outcomes (e.g., life satisfaction, psychological strain, somatic or physical symptoms, depression, substance use or abuse, and anxiety; Amstad, Meier, Fasel, Elfering, & Semmer, 2011 ).
Individuals and organizations can experience work-related strains. Sometimes organizations will experience strains through the employee’s negative attitudes or strains, such as that a worker’s absence might yield lower production rates, which would roll up into an organizational metric of organizational performance. In the industrial and organizational (IO) psychology literature, organizational strains are mostly observed as macro-level indicators, such as health insurance costs, accident-free days, and pervasive problems with company morale. In contrast, individual strains, usually referred to as job strains, are internal to an employee. They are responses to work conditions and relate to health and well-being of employees. In other words, “job strains are adverse reactions employees have to job stressors” (Spector, Chen, & O’Connell, 2000 , p. 211). Job strains tend to fall into three categories: behavioral, physical, and psychological (Jex & Beehr, 1991 ).
Behavioral strains consist of actions that employees take in response to job stressors. Examples of behavioral strains include employees drinking alcohol in the workplace or intentionally calling in sick when they are not ill (Spector et al., 2000 ). Physical strains consist of health symptoms that are physiological in nature that employees contract in response to job stressors. Headaches and ulcers are examples of physical strains. Lastly, psychological strains are emotional reactions and attitudes that employees have in response to job stressors. Examples of psychological strains are job dissatisfaction, anxiety, and frustration (Spector et al., 2000 ). Interestingly, research studies that utilize self-report measures find that most job strains experienced by employees tend to be psychological strains (Spector et al., 2000 ).
Leading Frameworks
Organizations that are keen on identifying organizational pain points and remedying them through organizational campaigns or initiatives often discover the pain points are rooted in work-related stressors and strains and the initiatives have to focus on reducing workers’ stress and increasing a company’s profitability. Through organizational climate surveys, for example, companies discover that aspects of the organization’s environment, including its policies, practices, reward structures, procedures, and processes, as well as employees at all levels of the company, are contributing to the individual and organizational stress. Recent studies have even begun to examine team climates for eustress and distress assessed in terms of team members’ homogenous psychological experience of vigor, efficacy, dedication, and cynicism (e.g., Kożusznik, Rodriguez, & Peiro, 2015 ).
Each of the frameworks presented advances different aspects that need to be identified in order to understand the source and potential remedy for stressors and strains. In some models, the focus is on resources, in others on the interaction of the person and environment, and in still others on the role of the person in the workplace. Few frameworks directly examine the role of the organization, but the organization could use these frameworks to plan interventions that would minimize stressors, cope with existing stressors, and prevent and/or manage strains. One of the leading frameworks in work stress research that is used to guide organizational interventions is the person and environment (P-E) fit (French & Caplan, 1972 ). Its precursor is the University of Michigan Institute for Social Research’s (ISR) role stress model (Kahn, Wolfe, Quinn, Snoek, & Rosenthal, 1964 ) and Lewin’s Field Theory. Several other theories have since evolved from the P-E fit framework, including Karasek and Theorell’s ( 1990 ), Karasek ( 1979 ) Job Demands-Control Model (JD-C), the transactional framework (Lazarus & Folkman, 1984 ), Conservation of Resources (COR) theory (Hobfoll, 1989 ), and Siegrist’s ( 1996 ) Effort-Reward Imbalance (ERI) Model.
Field Theory
The premise of Kahn et al.’s ( 1964 ) role stress theory is Lewin’s ( 1997 ) Field Theory. Lewin purported that behavior and mental events are a dynamic function of the whole person, including a person’s beliefs, values, abilities, needs, thoughts, and feelings, within a given situation (field or environment), as well as the way a person represents his or her understanding of the field and behaves in that space. Lewin explains that work-related strains are a result of individuals’ subjective perceptions of objective factors, such as work roles, relationships with others in the workplace, as well as personality indicators, and can be used to predict people’s reactions, including illness. Thus, to make changes to an organizational system, it is necessary to understand a field and try to move that field from the current state to the desired state. Making this move necessitates identifying mechanisms influencing individuals.
Role Stress Theory
Role stress theory mostly isolates the perspective a person has about his or her work-related responsibilities and expectations to determine how those perceptions relate with a person’s work-related strains. However, those relationships have been met with somewhat varied results, which Glazer and Beehr ( 2005 ) concluded might be a function of differences in culture, an environmental factor often neglected in research. Kahn et al.’s ( 1964 ) role stress theory, coupled with Lewin’s ( 1936 ) Field Theory, serves as the foundation for the P-E fit theory. Lewin ( 1936 ) wrote, “Every psychological event depends upon the state of the person and at the same time on the environment” (p. 12). Researchers of IO psychology have narrowed the environment to the organization or work team. This narrowed view of the organizational environment is evident in French and Caplan’s ( 1972 ) P-E fit framework.
Person-Environment Fit Theory
The P-E fit framework focuses on the extent to which there is congruence between the person and a given environment, such as the organization (Caplan, 1987 ; Edwards, 2008 ). For example, does the person have the necessary skills and abilities to fulfill an organization’s demands, or does the environment support a person’s desire for autonomy (i.e., do the values align?) or fulfill a person’s needs (i.e., a person’s needs are rewarded). Theoretically and empirically, the greater the person-organization fit, the greater a person’s job satisfaction and organizational commitment, the less a person’s turnover intention and work-related stress (see meta-analyses by Assouline & Meir, 1987 ; Kristof-Brown, Zimmerman, & Johnson, 2005 ; Verquer, Beehr, & Wagner, 2003 ).
Job Demands-Control/Support (JD-C/S) and Job Demands-Resources (JD-R) Model
Focusing more closely on concrete aspects of work demands and the extent to which a person perceives he or she has control or decision latitude over those demands, Karasek ( 1979 ) developed the JD-C model. Karasek and Theorell ( 1990 ) posited that high job demands under conditions of little decision latitude or control yield high strains, which have varied implications on the health of an organization (e.g., in terms of high turnover, employee ill-health, poor organizational performance). This theory was modified slightly to address not only control, but also other resources that could protect a person from unruly job demands, including support (aka JD-C/S, Johnson & Hall, 1988 ; and JD-R, Bakker, van Veldhoven, & Xanthopoulou, 2010 ). Whether focusing on control or resources, both they and job demands are said to reflect workplace characteristics, while control and resources also represent coping strategies or tools (Siegrist, 2010 ).
Despite the glut of research testing the JD-C and JD-R, results are somewhat mixed. Testing the interaction between job demands and control, Beehr, Glaser, Canali, and Wallwey ( 2001 ) did not find empirical support for the JD-C theory. However, Dawson, O’Brien, and Beehr ( 2016 ) found that high control and high support buffered against the independent deleterious effects of interpersonal conflict, role conflict, and organizational politics (demands that were categorized as hindrance stressors) on anxiety, as well as the effects of interpersonal conflict and organizational politics on physiological symptoms, but control and support did not moderate the effects between challenge stressors and strains. Coupled with Bakker, Demerouti, and Sanz-Vergel’s ( 2014 ) note that excessive job demands are a source of strain, but increased job resources are a source of engagement, Dawson et al.’s results suggest that when an organization identifies that demands are hindrances, it can create strategies for primary (preventative) stress management interventions and attempt to remove or reduce such work demands. If the demands are challenging, though manageable, but latitude to control the challenging stressors and support are insufficient, the organization could modify practices and train employees on adopting better strategies for meeting or coping (secondary stress management intervention) with the demands. Finally, if the organization can neither afford to modify the demands or the level of control and support, it will be necessary for the organization to develop stress management (tertiary) interventions to deal with the inevitable strains.
Conservation of Resources Theory
The idea that job resources reinforce engagement in work has been propagated in Hobfoll’s ( 1989 ) Conservation of Resources (COR) theory. COR theory also draws on the foundational premise that people’s mental health is a function of the person and the environment, forwarding that how people interpret their environment (including the societal context) affects their stress levels. Hobfoll focuses on resources such as objects, personal characteristics, conditions, or energies as particularly instrumental to minimizing strains. He asserts that people do whatever they can to protect their valued resources. Thus, strains develop when resources are threatened to be taken away, actually taken away, or when additional resources are not attainable after investing in the possibility of gaining more resources (Hobfoll, 2001 ). By extension, organizations can invest in activities that would minimize resource loss and create opportunities for resource gains and thus have direct implications for devising primary and secondary stress management interventions.
Transactional Framework
Lazarus and Folkman ( 1984 ) developed the widely studied transactional framework of stress. This framework holds as a key component the cognitive appraisal process. When individuals perceive factors in the work environment as a threat (i.e., primary appraisal), they will scan the available resources (external or internal to himself or herself) to cope with the stressors (i.e., secondary appraisal). If the coping resources provide minimal relief, strains develop. Until recently, little attention has been given to the cognitive appraisal associated with different work stressors (Dewe & Kompier, 2008 ; Liu & Li, 2017 ). In a study of Polish and Spanish social care service providers, stressors appraised as a threat related positively to burnout and less engagement, but stressors perceived as challenges yielded greater engagement and less burnout (Kożusznik, Rodriguez, & Peiro, 2012 ). Similarly, Dawson et al. ( 2016 ) found that even with support and control resources, hindrance demands were more strain-producing than challenge demands, suggesting that appraisal of the stressor is important. In fact, “many people respond well to challenging work” (Beehr et al., 2001 , p. 126). Kożusznik et al. ( 2012 ) recommend training employees to change the way they view work demands in order to increase engagement, considering that part of the problem may be about how the person appraises his or her environment and, thus, copes with the stressors.
Effort-Reward Imbalance
Siegrist’s ( 1996 ) Model of Effort-Reward Imbalance (ERI) focuses on the notion of social reciprocity, such that a person fulfills required work tasks in exchange for desired rewards (Siegrist, 2010 ). ERI sheds light on how an imbalance in a person’s expectations of an organization’s rewards (e.g., pay, bonus, sense of advancement and development, job security) in exchange for a person’s efforts, that is a break in one’s work contract, leads to negative responses, including long-term ill-health (Siegrist, 2010 ; Siegrist et al., 2014 ). In fact, prolonged perception of a work contract imbalance leads to adverse health, including immunological problems and inflammation, which contribute to cardiovascular disease (Siegrist, 2010 ). The model resembles the relational and interactional psychological contract theory in that it describes an employee’s perception of the terms of the relationship between the person and the workplace, including expectations of performance, job security, training and development opportunities, career progression, salary, and bonuses (Thomas, Au, & Ravlin, 2003 ). The psychological contract, like the ERI model, focuses on social exchange. Furthermore, the psychological contract, like stress theories, are influenced by cultural factors that shape how people interpret their environments (Glazer, 2008 ; Thomas et al., 2003 ). Violations of the psychological contract will negatively affect a person’s attitudes toward the workplace and subsequent health and well-being (Siegrist, 2010 ). To remediate strain, Siegrist ( 2010 ) focuses on both the person and the environment, recognizing that the organization is particularly responsible for changing unfavorable work conditions and the person is responsible for modifying his or her reactions to such conditions.
Stress Management Interventions: Primary, Secondary, and Tertiary
Remediation of work stress and organizational development interventions are about realigning the employee’s experiences in the workplace with factors in the environment, as well as closing the gap between the current environment and the desired environment. Work stress develops when an employee perceives the work demands to exceed the person’s resources to cope and thus threatens employee well-being (Dewe & Kompier, 2008 ). Likewise, an organization’s need to change arises when forces in the environment are creating a need to change in order to survive (see Figure 1 ). Lewin’s ( 1951 ) Force Field Analysis, the foundations of which are in Field Theory, is one of the first organizational development intervention tools presented in the social science literature. The concept behind Force Field Analysis is that in order to survive, organizations must adapt to environmental forces driving a need for organizational change and remove restraining forces that create obstacles to organizational change. In order to do this, management needs to delineate the current field in which the organization is functioning, understand the driving forces for change, identify and dampen or eliminate the restraining forces against change. Several models for analyses may be applied, but most approaches are variations of organizational climate surveys.
Through organizational surveys, workers provide management with a snapshot view of how they perceive aspects of their work environment. Thus, the view of the health of an organization is a function of several factors, chief among them employees’ views (i.e., the climate) about the workplace (Lewin, 1951 ). Indeed, French and Kahn ( 1962 ) posited that well-being depends on the extent to which properties of the person and properties of the environment align in terms of what a person requires and the resources available in a given environment. Therefore, only when properties of the person and properties of the environment are sufficiently understood can plans for change be developed and implemented targeting the environment (e.g., change reporting structures to relieve, and thus prevent future, communication stressors) and/or the person (e.g., providing more autonomy, vacation days, training on new technology). In short, climate survey findings can guide consultants about the emphasis for organizational interventions: before a problem arises aka stress prevention, e.g., carefully crafting job roles), when a problem is present, but steps are taken to mitigate their consequences (aka coping, e.g., providing social support groups), and/or once strains develop (aka. stress management, e.g., healthcare management policies).
For each of the primary (prevention), secondary (coping), and tertiary (stress management) techniques the target for intervention can be the entire workforce, a subset of the workforce, or a specific person. Interventions that target the entire workforce may be considered organizational interventions, as they have direct implications on the health of all individuals and consequently the health of the organization. Several interventions categorized as primary and secondary interventions may also be implemented after strains have developed and after it has been discerned that a person or the organization did not do enough to mitigate stressors or strains (see Figure 1 ). The designation of many of the interventions as belonging to one category or another may be viewed as merely a suggestion.
Primary Interventions (Preventative Stress Management)
Before individuals begin to perceive work-related stressors, organizations engage in stress prevention strategies, such as providing people with resources (e.g., computers, printers, desk space, information about the job role, organizational reporting structures) to do their jobs. However, sometimes the institutional structures and resources are insufficient or ambiguous. Scholars and practitioners have identified several preventative stress management strategies that may be implemented.
Planning and Time Management
When employees feel quantitatively overloaded, sometimes the remedy is improving the employees’ abilities to plan and manage their time (Quick, Quick, Nelson, & Hurrell, 2003 ). Planning is a future-oriented activity that focuses on conceptual and comprehensive work goals. Time management is a behavior that focuses on organizing, prioritizing, and scheduling work activities to achieve short-term goals. Given the purpose of time management, it is considered a primary intervention, as engaging in time management helps to prevent work tasks from mounting and becoming unmanageable, which would subsequently lead to adverse outcomes. Time management comprises three fundamental components: (1) establishing goals, (2) identifying and prioritizing tasks to fulfill the goals, and (3) scheduling and monitoring progress toward goal achievement (Peeters & Rutte, 2005 ). Workers who employ time management have less role ambiguity (Macan, Shahani, Dipboye, & Philips, 1990 ), psychological stress or strain (Adams & Jex, 1999 ; Jex & Elaqua, 1999 ; Macan et al., 1990 ), and greater job satisfaction (Macan, 1994 ). However, Macan ( 1994 ) did not find a relationship between time management and performance. Still, Claessens, van Eerde, Rutte, and Roe ( 2004 ) found that perceived control of time partially mediated the relationships between planning behavior (an indicator of time management), job autonomy, and workload on one hand, and job strains, job satisfaction, and job performance on the other hand. Moreover, Peeters and Rutte ( 2005 ) observed that teachers with high work demands and low autonomy experienced more burnout when they had poor time management skills.
Person-Organization Fit
Just as it is important for organizations to find the right person for the job and organization, so is it the responsibility of a person to choose to work at the right organization—an organization that fulfills the person’s needs and upholds the values important to the individual, as much as the person fulfills the organization’s needs and adapts to its values. When people fit their employing organizations they are setting themselves up for experiencing less strain-producing stressors (Kristof-Brown et al., 2005 ). In a meta-analysis of 62 person-job fit studies and 110 person-organization fit studies, Kristof-Brown et al. ( 2005 ) found that person-job fit had a negative correlation with indicators of job strain. In fact, a primary intervention of career counseling can help to reduce stress levels (Firth-Cozens, 2003 ).
Job Redesign
The Job Demands-Control/Support (JD-C/S), Job Demands-Resources (JD-R), and transactional models all suggest that factors in the work context require modifications in order to reduce potential ill-health and poor organizational performance. Drawing on Hackman and Oldham’s ( 1980 ) Job Characteristics Model, it is possible to assess with the Job Diagnostics Survey (JDS) the current state of work characteristics related to skill variety, task identity, task significance, autonomy, and feedback. Modifying those aspects would help create a sense of meaningfulness, sense of responsibility, and feeling of knowing how one is performing, which subsequently affects a person’s well-being as identified in assessments of motivation, satisfaction, improved performance, and reduced withdrawal intentions and behaviors. Extending this argument to the stress models, it can be deduced that reducing uncertainty or perceived unfairness that may be associated with a person’s perception of these work characteristics, as well as making changes to physical characteristics of the environment (e.g., lighting, seating, desk, air quality), nature of work (e.g., job responsibilities, roles, decision-making latitude), and organizational arrangements (e.g., reporting structure and feedback mechanisms), can help mitigate against numerous ill-health consequences and reduced organizational performance. In fact, Fried et al. ( 2013 ) showed that healthy patients of a medical clinic whose jobs were excessively low (i.e., monotonous) or excessively high (i.e., overstimulating) on job enrichment (as measured by the JDS) had greater abdominal obesity than those whose jobs were optimally enriched. By taking stock of employees’ perceptions of the current work situation, managers might think about ways to enhance employees’ coping toolkit, such as training on how to deal with difficult clients or creating stimulating opportunities when jobs have low levels of enrichment.
Participatory Action Research Interventions
Participatory action research (PAR) is an intervention wherein, through group discussions, employees help to identify and define problems in organizational structure, processes, policies, practices, and reward structures, as well as help to design, implement, and evaluate success of solutions. PAR is in itself an intervention, but its goal is to design interventions to eliminate or reduce work-related factors that are impeding performance and causing people to be unwell. An example of a successful primary intervention, utilizing principles of PAR and driven by the JD-C and JD-C/S stress frameworks is Health Circles (HCs; Aust & Ducki, 2004 ).
HCs, developed in Germany in the 1980s, were popular practices in industries, such as metal, steel, and chemical, and service. Similar to other problem-solving practices, such as quality circles, HCs were based on the assumptions that employees are the experts of their jobs. For this reason, to promote employee well-being, management and administrators solicited suggestions and ideas from the employees to improve occupational health, thereby increasing employees’ job control. HCs also promoted communication between managers and employees, which had a potential to increase social support. With more control and support, employees would experience less strains and better occupational well-being.
Employing the three-steps of (1) problem analysis (i.e., diagnosis or discovery through data generated from organizational records of absenteeism length, frequency, rate, and reason and employee survey), (2) HC meetings (6 to 10 meetings held over several months to brainstorm ideas to improve occupational safety and health concerns identified in the discovery phase), and (3) HC evaluation (to determine if desired changes were accomplished and if employees’ reports of stressors and strains changed after the course of 15 months), improvements were to be expected (Aust & Ducki, 2004 ). Aust and Ducki ( 2004 ) reviewed 11 studies presenting 81 health circles in 30 different organizations. Overall study participants had high satisfaction with the HCs practices. Most companies acted upon employees’ suggestions (e.g., improving driver’s seat and cab, reducing ticket sale during drive, team restructuring and job rotation to facilitate communication, hiring more employees during summer time, and supervisor training program to improve leadership and communication skills) to improve work conditions. Thus, HCs represent a successful theory-grounded intervention to routinely improve employees’ occupational health.
Physical Setting
The physical environment or physical workspace has an enormous impact on individuals’ well-being, attitudes, and interactions with others, as well as on the implications on innovation and well-being (Oksanen & Ståhle, 2013 ; Vischer, 2007 ). In a study of 74 new product development teams (total of 437 study respondents) in Western Europe, Chong, van Eerde, Rutte, and Chai ( 2012 ) found that when teams were faced with challenge time pressures, meaning the teams had a strong interest and desire in tackling complex, but engaging tasks, when they were working proximally close with one another, team communication improved. Chong et al. assert that their finding aligns with prior studies that have shown that physical proximity promotes increased awareness of other team members, greater tendency to initiate conversations, and greater team identification. However, they also found that when faced with hindrance time pressures, physical proximity related to low levels of team communication, but when hindrance time pressure was low, team proximity had an increasingly greater positive relationship with team communication.
In addition to considering the type of work demand teams must address, other physical workspace considerations include whether people need to work collaboratively and synchronously or independently and remotely (or a combination thereof). Consideration needs to be given to how company contributors would satisfy client needs through various modes of communication, such as email vs. telephone, and whether individuals who work by a window might need shading to block bright sunlight from glaring on their computer screens. Finally, people who have to use the telephone for extensive periods of time would benefit from earphones to prevent neck strains. Most physical stressors are rather simple to rectify. However, companies are often not aware of a problem until after a problem arises, such as when a person’s back is strained from trying to move heavy equipment. Companies then implement strategies to remediate the environmental stressor. With the help of human factors, and organizational and office design consultants, many of the physical barriers to optimal performance can be prevented (Rousseau & Aubé, 2010 ). In a study of 215 French-speaking Canadian healthcare employees, Rousseau and Aubé ( 2010 ) found that although supervisor instrumental support positively related with affective commitment to the organization, the relationship was even stronger for those who reported satisfaction with the ambient environment (i.e., temperature, lighting, sound, ventilation, and cleanliness).
Secondary Interventions (Coping)
Secondary interventions, also referred to as coping, focus on resources people can use to mitigate the risk of work-related illness or workplace injury. Resources may include properties related to social resources, behaviors, and cognitive structures. Each of these resource domains may be employed to cope with stressors. Monat and Lazarus ( 1991 ) summarize the definition of coping as “an individual’s efforts to master demands (or conditions of harm, threat, or challenge) that are appraised (or perceived) as exceeding or taxing his or her resources” (p. 5). To master demands requires use of the aforementioned resources. Secondary interventions help employees become aware of the psychological, physical, and behavioral responses that may occur from the stressors presented in their working environment. Secondary interventions help a person detect and attend to stressors and identify resources for and ways of mitigating job strains. Often, coping strategies are learned skills that have a cognitive foundation and serve important functions in improving people’s management of stressors (Lazarus & Folkman, 1991 ). Coping is effortful, but with practice it becomes easier to employ. This idea is the foundation for understanding the role of resilience in coping with stressors. However, “not all adaptive processes are coping. Coping is a subset of adaptational activities that involves effort and does not include everything that we do in relating to the environment” (Lazarus & Folkman, 1991 , p. 198). Furthermore, sometimes to cope with a stressor, a person may call upon social support sources to help with tangible materials or emotional comfort. People call upon support resources because they help to restructure how a person approaches or thinks about the stressor.
Most secondary interventions are aimed at helping the individual, though companies, as a policy, might require all employees to partake in training aimed at increasing employees’ awareness of and skills aimed at handling difficult situations vis à vis company channels (e.g., reporting on sexual harassment or discrimination). Furthermore, organizations might institute mentoring programs or work groups to address various work-related matters. These programs employ awareness-raising activities, stress-education, or skills training (cf., Bhagat, Segovis, & Nelson, 2012 ), which include development of skills in problem-solving, understanding emotion-focused coping, identifying and using social support, and enhancing capacity for resilience. The aim of these programs, therefore, is to help employees proactively review their perceptions of psychological, physical, and behavioral job-related strains, thereby extending their resilience, enabling them to form a personal plan to control stressors and practice coping skills (Cooper, Dewe, & O’Driscoll, 2011 ).
Often these stress management programs are instituted after an organization has observed excessive absenteeism and work-related performance problems and, therefore, are sometimes categorized as a tertiary stress management intervention or even a primary (prevention) intervention. However, the skills developed for coping with stressors also place the programs in secondary stress management interventions. Example programs that are categorized as tertiary or primary stress management interventions may also be secondary stress management interventions (see Figure 1 ), and these include lifestyle advice and planning, stress inoculation training, simple relaxation techniques, meditation, basic trainings in time management, anger management, problem-solving skills, and cognitive-behavioral therapy. Corporate wellness programs also fall under this category. In other words, some programs could be categorized as primary, secondary, or tertiary interventions depending upon when the employee (or organization) identifies the need to implement the program. For example, time management practices could be implemented as a means of preventing some stressors, as a way to cope with mounting stressors, or as a strategy to mitigate symptoms of excessive of stressors. Furthermore, these programs can be administered at the individual level or group level. As related to secondary interventions, these programs provide participants with opportunities to develop and practice skills to cognitively reappraise the stressor(s); to modify their perspectives about stressors; to take time out to breathe, stretch, meditate, relax, and/or exercise in an attempt to support better decision-making; to articulate concerns and call upon support resources; and to know how to say “no” to onslaughts of requests to complete tasks. Participants also learn how to proactively identify coping resources and solve problems.
According to Cooper, Dewe, and O’Driscoll ( 2001 ), secondary interventions are successful in helping employees modify or strengthen their ability to cope with the experience of stressors with the goal of mitigating the potential harm the job stressors may create. Secondary interventions focus on individuals’ transactions with the work environment and emphasize the fit between a person and his or her environment. However, researchers have pointed out that the underlying assumption of secondary interventions is that the responsibility for coping with the stressors of the environment lies within individuals (Quillian-Wolever & Wolever, 2003 ). If companies cannot prevent the stressors in the first place, then they are, in part, responsible for helping individuals develop coping strategies and informing employees about programs that would help them better cope with job stressors so that they are able to fulfill work assignments.
Stress management interventions that help people learn to cope with stressors focus mainly on the goals of enabling problem-resolution or expressing one’s emotions in a healthy manner. These goals are referred to as problem-focused coping and emotion-focused coping (Folkman & Lazarus, 1980 ; Pearlin & Schooler, 1978 ), and the person experiencing the stressors as potential threat is the agent for change and the recipient of the benefits of successful coping (Hobfoll, 1998 ). In addition to problem-focused and emotion-focused coping approaches, social support and resilience may be coping resources. There are many other sources for coping than there is room to present here (see e.g., Cartwright & Cooper, 2005 ); however, the current literature has primarily focused on these resources.
Problem-Focused Coping
Problem-focused or direct coping helps employees remove or reduce stressors in order to reduce their strain experiences (Bhagat et al., 2012 ). In problem-focused coping employees are responsible for working out a strategic plan in order to remove job stressors, such as setting up a set of goals and engaging in behaviors to meet these goals. Problem-focused coping is viewed as an adaptive response, though it can also be maladaptive if it creates more problems down the road, such as procrastinating getting work done or feigning illness to take time off from work. Adaptive problem-focused coping negatively relates to long-term job strains (Higgins & Endler, 1995 ). Discussion on problem-solving coping is framed from an adaptive perspective.
Problem-focused coping is featured as an extension of control, because engaging in problem-focused coping strategies requires a series of acts to keep job stressors under control (Bhagat et al., 2012 ). In the stress literature, there are generally two ways to categorize control: internal versus external locus of control, and primary versus secondary control. Locus of control refers to the extent to which people believe they have control over their own life (Rotter, 1966 ). People high in internal locus of control believe that they can control their own fate whereas people high in external locus of control believe that outside factors determine their life experience (Rotter, 1966 ). Generally, those with an external locus of control are less inclined to engage in problem-focused coping (Strentz & Auerbach, 1988 ). Primary control is the belief that people can directly influence their environment (Alloy & Abramson, 1979 ), and thus they are more likely to engage in problem-focused coping. However, when it is not feasible to exercise primary control, people search for secondary control, with which people try to adapt themselves into the objective environment (Rothbaum, Weisz, & Snyder, 1982 ).
Emotion-Focused Coping
Emotion-focused coping, sometimes referred to as palliative coping, helps employees reduce strains without the removal of job stressors. It involves cognitive or emotional efforts, such as talking about the stressor or distracting oneself from the stressor, in order to lessen emotional distress resulting from job stressors (Bhagat et al., 2012 ). Emotion-focused coping aims to reappraise and modify the perceptions of a situation or seek emotional support from friends or family. These methods do not include efforts to change the work situation or to remove the job stressors (Lazarus & Folkman, 1991 ). People tend to adopt emotion-focused coping strategies when they believe that little or nothing can be done to remove the threatening, harmful, and challenging stressors (Bhagat et al., 2012 ), such as when they are the only individuals to have the skills to get a project done or they are given increased responsibilities because of the unexpected departure of a colleague. Emotion-focused coping strategies include (1) reappraisal of the stressful situation, (2) talking to friends and receiving reassurance from them, (3) focusing on one’s strength rather than weakness, (4) optimistic comparison—comparing one’s situation to others’ or one’s past situation, (5) selective ignoring—paying less attention to the unpleasant aspects of one’s job and being more focused on the positive aspects of the job, (6) restrictive expectations—restricting one’s expectations on job satisfaction but paying more attention to monetary rewards, (7) avoidance coping—not thinking about the problem, leaving the situation, distracting oneself, or using alcohol or drugs (e.g., Billings & Moos, 1981 ).
Some emotion-focused coping strategies are maladaptive. For example, avoidance coping may lead to increased level of job strains in the long run (e.g., Parasuraman & Cleek, 1984 ). Furthermore, a person’s ability to cope with the imbalance of performing work to meet organizational expectations can take a toll on the person’s health, leading to physiological consequences such as cardiovascular disease, sleep disorders, gastrointestinal disorders, and diabetes (Fried et al., 2013 ; Siegrist, 2010 ; Toker, Shirom, Melamed, & Armon, 2012 ; Willert, Thulstrup, Hertz, & Bonde, 2010 ).
Comparing Coping Strategies across Cultures
Most coping research is conducted in individualistic, Western cultures wherein emotional control is emphasized and both problem-solving focused coping and primary control are preferred (Bhagat et al., 2010 ). However, in collectivistic cultures, emotion-focused coping and use of secondary control may be preferred and may not necessarily carry a negative evaluation (Bhagat et al., 2010 ). For example, African Americans are more likely to use emotion-focused coping than non–African Americans (Knight, Silverstein, McCallum, & Fox, 2000 ), and among women who experienced sexual harassment, Anglo American women were less likely to employ emotion focused coping (i.e., avoidance coping) than Turkish women and Hispanic American women, while Hispanic women used more denial than the other two groups (Wasti & Cortina, 2002 ).
Thus, whereas problem-focused coping is venerated in Western societies, emotion-focused coping may be more effective in reducing strains in collectivistic cultures, such as China, Japan, and India (Bhagat et al., 2010 ; Narayanan, Menon, & Spector, 1999 ; Selmer, 2002 ). Indeed, Swedish participants reported more problem-focused coping than did Chinese participants (Xiao, Ottosson, & Carlsson, 2013 ), American college students engaged in more problem-focused coping behaviors than did their Japanese counterparts (Ogawa, 2009 ), and Indian (vs. Canadian) students reported more emotion-focused coping, such as seeking social support and positive reappraisal (Sinha, Willson, & Watson, 2000 ). Moreover, Glazer, Stetz, and Izso ( 2004 ) found that internal locus of control was more predominant in individualistic cultures (United Kingdom and United States), whereas external locus of control was more predominant in communal cultures (Italy and Hungary). Also, internal locus of control was associated with less job stress, but more so for nurses in the United Kingdom and United States than Italy and Hungary. Taken together, adoption of coping strategies and their effectiveness differ significantly across cultures. The extent to which a coping strategy is perceived favorably and thus selected or not selected is not only a function of culture, but also a person’s sociocultural beliefs toward the coping strategy (Morimoto, Shimada, & Ozaki, 2013 ).
Social Support
Social support refers to the aid an entity gives to a person. The source of the support can be a single person, such as a supervisor, coworker, subordinate, family member, friend, or stranger, or an organization as represented by upper-level management representing organizational practices. The type of support can be instrumental or emotional. Instrumental support, including informational support, refers to that which is tangible, such as data to help someone make a decision or colleagues’ sick days so one does not lose vital pay while recovering from illness. Emotional support, including esteem support, refers to the psychological boost given to a person who needs to express emotions and feel empathy from others or to have his or her perspective validated. Beehr and Glazer ( 2001 ) present an overview of the role of social support on the stressor-strain relationship and arguments regarding the role of culture in shaping the utility of different sources and types of support.
Meaningfulness and Resilience
Meaningfulness reflects the extent to which people believe their lives are significant, purposeful, goal-directed, and fulfilling (Glazer, Kożusznik, Meyers, & Ganai, 2014 ). When faced with stressors, people who have a strong sense of meaning in life will also try to make sense of the stressors. Maintaining a positive outlook on life stressors helps to manage emotions, which is helpful in reducing strains, particularly when some stressors cannot be problem-solved (Lazarus & Folkman, 1991 ). Lazarus and Folkman ( 1991 ) emphasize that being able to reframe threatening situations can be just as important in an adaptation as efforts to control the stressors. Having a sense of meaningfulness motivates people to behave in ways that help them overcome stressors. Thus, meaningfulness is often used in the same breath as resilience, because people who are resilient are often protecting that which is meaningful.
Resilience is a personality state that can be fortified and enhanced through varied experiences. People who perceive their lives are meaningful are more likely to find ways to face adversity and are therefore more prone to intensifying their resiliency. When people demonstrate resilience to cope with noxious stressors, their ability to be resilient against other stressors strengthens because through the experience, they develop more competencies (Glazer et al., 2014 ). Thus, fitting with Hobfoll’s ( 1989 , 2001 ) COR theory, meaningfulness and resilience are psychological resources people attempt to conserve and protect, and employ when necessary for making sense of or coping with stressors.
Tertiary Interventions (Stress Management)
Stress management refers to interventions employed to treat and repair harmful repercussions of stressors that were not coped with sufficiently. As Lazarus and Folkman ( 1991 ) noted, not all stressors “are amenable to mastery” (p. 205). Stressors that are unmanageable and lead to strains require interventions to reverse or slow down those effects. Workplace interventions might focus on the person, the organization, or both. Unfortunately, instead of looking at the whole system to include the person and the workplace, most companies focus on the person. Such a focus should not be a surprise given the results of van der Klink, Blonk, Schene, and van Dijk’s ( 2001 ) meta-analysis of 48 experimental studies conducted between 1977 and 1996 . They found that of four types of tertiary interventions, the effect size for cognitive-behavioral interventions and multimodal programs (e.g., the combination of assertive training and time management) was moderate and the effect size for relaxation techniques was small in reducing psychological complaints, but not turnover intention related to work stress. However, the effects of (the five studies that used) organization-focused interventions were not significant. Similarly, Richardson and Rothstein’s ( 2008 ) meta-analytic study, including 36 experimental studies with 55 interventions, showed a larger effect size for cognitive-behavioral interventions than relaxation, organizational, multimodal, or alternative. However, like with van der Klink et al. ( 2001 ), Richardson and Rothstein ( 2008 ) cautioned that there were few organizational intervention studies included and the impact of interventions were determined on the basis of psychological outcomes and not physiological or organizational outcomes. Van der Klink et al. ( 2001 ) further expressed concern that organizational interventions target the workplace and that changes in the individual may take longer to observe than individual interventions aimed directly at the individual.
The long-term benefits of individual focused interventions are not yet clear either. Per Giga, Cooper, and Faragher ( 2003 ), the benefits of person-directed stress management programs will be short-lived if organizational factors to reduce stressors are not addressed too. Indeed, LaMontagne, Keegel, Louie, Ostry, and Landsbergis ( 2007 ), in their meta-analysis of 90 studies on stress management interventions published between 1990 and 2005 , revealed that in relation to interventions targeting organizations only, and interventions targeting individuals only, interventions targeting both organizations and individuals (i.e. the systems approach) had the most favorable positive effects on both the organizations and the individuals. Furthermore, the organization-level interventions were effective at both the individual and organization levels, but the individual-level interventions were effective only at the individual level.
Individual-Focused Stress Management
Individual-focused interventions concentrate on improving conditions for the individual, though counseling programs emphasize that the worker is in charge of reducing “stress,” whereas role-focused interventions emphasize activities that organizations can guide to actually reduce unnecessary noxious environmental factors.
Individual-Focused Stress Management: Employee Assistance Programs
When stress become sufficiently problematic (which is individually gauged or attended to by supportive others) in a worker’s life, employees may utilize the short-term counseling services or referral services Employee Assistance Programs (EAPs) provide. People who utilize the counseling services may engage in cognitive behavioral therapy aimed at changing the way people think about the stressors (e.g., as challenge opportunity over threat) and manage strains. Example topics that may be covered in these therapy sessions include time management and goal setting (prioritization), career planning and development, cognitive restructuring and mindfulness, relaxation, and anger management. In a study of healthcare workers and teachers who participated in a 2-day to 2.5-day comprehensive stress management training program (including 26 topics on identifying, coping with, and managing stressors and strains), Siu, Cooper, and Phillips ( 2013 ) found psychological and physical improvements were self-reported among the healthcare workers (for which there was no control group). However, comparing an intervention group of teachers to a control group of teachers, the extent of change was not as visible, though teachers in the intervention group engaged in more mastery recovery experiences (i.e., they purposefully chose to engage in challenging activities after work).
Individual-Focused Stress Management: Mindfulness
A popular therapy today is to train people to be more mindful, which involves helping people live in the present, reduce negative judgement of current and past experiences, and practicing patience (Birnie, Speca, & Carlson, 2010 ). Mindfulness programs usually include training on relaxation exercises, gentle yoga, and awareness of the body’s senses. In one study offered through the continuing education program at a Canadian university, 104 study participants took part in an 8-week, 90 minute per group (15–20 participants per) session mindfulness program (Birnie et al., 2010 ). In addition to body scanning, they also listened to lectures on incorporating mindfulness into one’s daily life and received a take-home booklet and compact discs that guided participants through the exercises studied in person. Two weeks after completing the program, participants’ mindfulness attendance and general positive moods increased, while physical, psychological, and behavioral strains decreased. In another study on a sample of U.K. government employees, study participants receiving three sessions of 2.5 to 3 hours each training on mindfulness, with the first two sessions occurring in consecutive weeks and the third occurring about three months later, Flaxman and Bond ( 2010 ) found that compared to the control group, the intervention group showed a decrease in distress levels from Time 1 (baseline) to Time 2 (three months after first two training sessions) and Time 1 to Time 3 (after final training session). Moreover, of the mindfulness intervention study participants who were clinically distressed, 69% experienced clinical improvement in their psychological health.
Individual-Focused Stress Management: Biofeedback/Imagery/Meditation/Deep Breathing
Biofeedback uses electronic equipment to inform users about how their body is responding to tension. With guidance from a therapist, individuals then learn to change their physiological responses so that their pulse normalizes and muscles relax (Norris, Fahrion, & Oikawa, 2007 ). The therapist’s guidance might include reminders for imagery, meditation, body scan relaxation, and deep breathing. Saunders, Driskell, Johnston, and Salas’s ( 1996 ) meta-analysis of 37 studies found that imagery helped reduce state and performance anxiety. Once people have been trained to relax, reminder triggers may be sent through smartphone push notifications (Villani et al., 2013 ).
Smartphone technology can also be used to support weight loss programs, smoking cessation programs, and medication or disease (e.g., diabetes) management compliance (Heron & Smyth, 2010 ; Kannampallil, Waicekauskas, Morrow, Kopren, & Fu, 2013 ). For example, smartphones could remind a person to take medications or test blood sugar levels or send messages about healthy behaviors and positive affirmations.
Individual-Focused Stress Management: Sleep/Rest/Respite
Workers today sleep less per night than adults did nearly 30 years ago (Luckhaupt, Tak, & Calvert, 2010 ; National Sleep Foundation, 2005 , 2013 ). In order to combat problems, such as increased anxiety and cardiovascular artery disease, associated with sleep deprivation and insufficient rest, it is imperative that people disconnect from their work at least one day per week or preferably for several weeks so that they are able to restore psychological health (Etzion, Eden, & Lapidot, 1998 ; Ragsdale, Beehr, Grebner, & Han, 2011 ). When college students engaged in relaxation-type activities, such as reading or watching television, over the weekend, they experienced less emotional exhaustion and greater general well-being than students who engaged in resources-consuming activities, such as house cleaning (Ragsdale et al., 2011 ). Additional research and future directions for research are reviewed and identified in the work of Sonnentag ( 2012 ). For example, she asks whether lack of ability to detach from work is problematic for people who find their work meaningful. In other words, are negative health consequences only among those who do not take pleasure in their work? Sonnetag also asks how teleworkers detach from their work when engaging in work from the home. Ironically, one of the ways that companies are trying to help with the challenges of high workload or increased need to be available to colleagues, clients, or vendors around the globe is by offering flexible work arrangements, whereby employees who can work from home are given the opportunity to do so. Companies that require global interactions 24-hours per day often employ this strategy, but is the solution also a source of strain (Glazer, Kożusznik, & Shargo, 2012 )?
Individual-Focused Stress Management: Role Analysis
Role analysis or role clarification aims to redefine, expressly identify, and align employees’ roles and responsibilities with their work goals. Through role negotiation, involved parties begin to develop a new formal or informal contract about expectations and define resources needed to fulfill those expectations. Glazer has used this approach in organizational consulting and, with one memorable client engagement, found that not only were the individuals whose roles required deeper re-evaluation happier at work (six months later), but so were their subordinates. Subordinates who once characterized the two partners as hostile and akin to a couple going through a bad divorce, later referred to them as a blissful pair. Schaubroeck, Ganster, Sime, and Ditman ( 1993 ) also found in a three-wave study over a two-year period that university employees’ reports of role clarity and greater satisfaction with their supervisor increased after a role clarification exercise of top managers’ roles and subordinates’ roles. However, the intervention did not have any impact on reported physical symptoms, absenteeism, or psychological well-being. Role analysis is categorized under individual-focused stress management intervention because it is usually implemented after individuals or teams begin to demonstrate poor performance and because the intervention typically focuses on a few individuals rather than an entire organization or group. In other words, the intervention treats the person’s symptoms by redefining the role so as to eliminate the stimulant causing the problem.
Organization-Focused Stress Management
At the organizational level, companies that face major declines in productivity and profitability or increased costs related to healthcare and disability might be motivated to reassess organizational factors that might be impinging on employees’ health and well-being. After all, without healthy workers, it is not possible to have a healthy organization. Companies may choose to implement practices and policies that are expected to help not only the employees, but also the organization with reduced costs associated with employee ill-health, such as medical insurance, disability payments, and unused office space. Example practices and policies that may be implemented include flexible work arrangements to ensure that employees are not on the streets in the middle of the night for work that can be done from anywhere (such as the home), diversity programs to reduce stress-induced animosity and prejudice toward others, providing only healthy food choices in cafeterias, mandating that all employees have physicals in order to receive reduced prices for insurance, company-wide closures or mandatory paid time off, and changes in organizational visioning.
Organization-Focused Stress Management: Organizational-Level Occupational Health Interventions
As with job design interventions that are implemented to remediate work characteristics that were a source of unnecessary or excessive stressors, so are organizational-level occupational health (OLOH) interventions. As with many of the interventions, its placement as a primary or tertiary stress management intervention may seem arbitrary, but when considering the goal and target of change, it is clear that the intervention is implemented in response to some ailing organizational issues that need to be reversed or stopped, and because it brings in the entire organization’s workforce to address the problems, it has been placed in this category. There are several more case studies than empirical studies on the topic of whole system organizational change efforts (see example case studies presented by the United Kingdom’s Health and Safety Executive). It is possible that lack of published empirical work is not so much due to lack of attempting to gather and evaluate the data for publication, but rather because the OLOH interventions themselves never made it to the intervention stage, the interventions failed (Biron, Gatrell, & Cooper, 2010 ), or the level of evaluation was not rigorous enough to get into empirical peer-review journals. Fortunately, case studies provide some indication of the opportunities and problems associated with OLOH interventions.
One case study regarding Cardiff and Value University Health Board revealed that through focus group meetings with members of a steering group (including high-level managers and supported by top management) and facilitated by a neutral, non-judgemental organizational health consultant, ideas for change were posted on newsprint, discussed, and areas in the organization needing change were identified. The intervention for giving voice to people who initially had little already had a positive effect on the organization, as absence decreased by 2.09% and 6.9% merely 12 and 18 months, respectively, after the intervention. Translated in financial terms, the 6.9% change was equivalent to a quarterly savings of £80,000 (Health & Safety Executive, n.d. ). Thus, focusing on the context of change and how people will be involved in the change process probably helped the organization realize improvements (Biron et al., 2010 ). In a recent and rare empirical study, employing both qualitative and quantitative data collection methods, Sørensen and Holman ( 2014 ) utilized PAR in order to plan and implement an OLOH intervention over the course of 14 months. Their study aimed to examine the effectiveness of the PAR process in reducing workers’ work-related and social or interpersonal-related stressors that derive from the workplace and improving psychological, behavioral, and physiological well-being across six Danish organizations. Based on group dialogue, 30 proposals for change were proposed, all of which could be categorized as either interventions to focus on relational factors (e.g., management feedback improvement, engagement) or work processes (e.g., reduced interruptions, workload, reinforcing creativity). Of the interventions that were implemented, results showed improvements on manager relationship quality and reduced burnout, but no changes with respect to work processes (i.e., workload and work pace) perhaps because the employees already had sufficient task control and variety. These findings support Dewe and Kompier’s ( 2008 ) position that occupational health can be reinforced through organizational policies that reinforce quality jobs and work experiences.
Organization-Focused Stress Management: Flexible Work Arrangements
Dewe and Kompier ( 2008 ), citing the work of Isles ( 2005 ), noted that concern over losing one’s job is a reason for why 40% of survey respondents indicated they work more hours than formally required. In an attempt to create balance and perceived fairness in one’s compensation for putting in extra work hours, employees will sometimes be legitimately or illegitimately absent. As companies become increasingly global, many people with desk jobs are finding themselves communicating with colleagues who are halfway around the globe and at all hours of the day or night (Glazer et al., 2012 ). To help minimize the strains associated with these stressors, companies might devise flexible work arrangements (FWA), though the type of FWA needs to be tailored to the cultural environment (Masuda et al., 2012 ). FWAs give employees some leverage to decide what would be the optimal work arrangement for them (e.g., part-time, flexible work hours, compressed work week, telecommuting). In other words, FWA provides employees with the choice of when to work, where to work (on-site or off-site), and how many hours to work in a day, week, or pay period (Kossek, Thompson, & Lautsch, 2015 ). However, not all employees of an organization have equal access to or equitable use of FWAs; workers in low-wage, hourly jobs are often beholden to being physically present during specific hours (Swanberg McKechnie, Ojha, & James, 2011 ). In a study of over 1,300 full-time hourly retail employees in the United States, Swanberg et al. ( 2011 ) showed that employees who have control over their work schedules and over their work hours were satisfied with their work schedules, perceived support from the supervisor, and work engagement.
Unfortunately, not all FWAs yield successful results for the individual or the organization. Being able to work from home or part-time can have problems too, as a person finds himself or herself working more hours from home than required. Sometimes telecommuting creates work-family conflict too as a person struggles to balance work and family obligations while working from home. Other drawbacks include reduced face-to-face contact between work colleagues and stakeholders, challenges shaping one’s career growth due to limited contact, perceived inequity if some have more flexibility than others, and ambiguity about work role processes for interacting with employees utilizing the FWA (Kossek et al., 2015 ). Organizations that institute FWAs must carefully weigh the benefits and drawbacks the flexibility may have on the employees using it or the employees affected by others using it, as well as the implications on the organization, including the vendors who are serving and clients served by the organization.
Organization-Focused Stress Management: Diversity Programs
Employees in the workplace might experience strain due to feelings of discrimination or prejudice. Organizational climates that do not promote diversity (in terms of age, religion, physical abilities, ethnicity, nationality, sex, and other characteristics) are breeding grounds for undesirable attitudes toward the workplace, lower performance, and greater turnover intention (Bergman, Palmieri, Drasgow, & Ormerod, 2012 ; Velez, Moradi, & Brewster, 2013 ). Management is thus advised to implement programs that reinforce the value and importance of diversity, as well as manage diversity to reduce conflict and feelings of prejudice. In fact, managers who attended a leadership training program reported higher multicultural competence in dealing with stressful situations (Chrobot-Mason & Leslie, 2012 ), and managers who persevered through challenges were more dedicated to coping with difficult diversity issues (Cilliers, 2011 ). Thus, diversity programs can help to reduce strains by directly reducing stressors associated with conflict linked to diversity in the workplace and by building managers’ resilience.
Organization-Focused Stress Management: Healthcare Management Policies
Over the past few years, organizations have adopted insurance plans that implement wellness programs for the sake of managing the increasing cost of healthcare that is believed to be a result of individuals’ not managing their own health, with regular check-ups and treatment. The wellness programs require all insured employees to visit a primary care provider, complete a health risk assessment, and engage in disease management activities as specified by a physician (e.g., see frequently asked questions regarding the State of Maryland’s Wellness Program). Companies believe that requiring compliance will reduce health problems, although there is no proof that such programs save money or that people would comply. One study that does, however, boast success, was a 12-week workplace health promotion program aimed at reducing Houston airport workers’ weight (Ebunlomo, Hare-Everline, Weber, & Rich, 2015 ). The program, which included 235 volunteer participants, was deemed a success, as there was a total weight loss of 345 pounds (or 1.5 lbs per person). Given such results in Houston, it is clear why some people are also skeptical over the likely success of wellness programs, particularly as there is no clear method for evaluating their efficacy (Sinnott & Vatz, 2015 ).
Moreover, for some, such a program is too paternalistic and intrusive, as well as punishes anyone who chooses not to actively participate in disease management programs (Sinnott & Vatz, 2015 ). The programs put the onus of change on the person, though it is a response to the high costs of ill-health. The programs neglect to consider the role of the organization in reducing the barriers to healthy lifestyle, such as cloaking exempt employment as simply needing to get the work done, when it usually means working significantly more hours than a standard workweek. In fact, workplace health promotion programs did not reduce presenteeism (i.e., people going to work while unwell thereby reducing their job performance) among those who suffered from physical pain (Cancelliere, Cassidy, Ammendolia, & Côte, 2011 ). However, supervisor education, worksite exercise, lifestyle intervention through email, midday respite from repetitive work, a global stress management program, changes in lighting, and telephone interventions helped to reduce presenteeism. Thus, emphasis needs to be placed on psychosocial aspects of the organization’s structure, including managers and overall organizational climate for on-site presence, that reinforces such behavior (Cancelliere et al., 2011 ). Moreover, wellness programs are only as good as the interventions to reduce work-related stressors and improve organizational resources to enable workers to improve their overall psychological and physical health.
Concluding Remarks
Future research.
One of the areas requiring more theoretical and practical attention is that of the utility of stress frameworks to guide organizational development change interventions. Although it has been proposed that the foundation for work stress management interventions is in organizational development, and even though scholars and practitioners of organization development were also founders of research programs that focused on employee health and well-being or work stress, there are few studies or other theoretical works that link the two bodies of literature.
A second area that requires additional attention is the efficacy of stress management interventions across cultures. In examining secondary stress management interventions (i.e., coping), some cross-cultural differences in findings were described; however, there is still a dearth of literature from different countries on the utility of different prevention, coping, and stress management strategies.
A third area that has been blossoming since the start of the 21st century is the topic of hindrance and challenge stressors and the implications of both on workers’ well-being and performance. More research is needed on this topic in several areas. First, there is little consistency by which researchers label a stressor as a hindrance or a challenge. Researchers sometimes take liberties with labels, but it is not the researchers who should label a stressor but the study participants themselves who should indicate if a stressor is a source of strain. Rodríguez, Kozusznik, and Peiró ( 2013 ) developed a measure in which respondents indicate whether a stressor is a challenge or a hindrance. Just as some people may perceive demands to be challenges that they savor and that result in a psychological state of eustress (Nelson & Simmons, 2003 ), others find them to be constraints that impede goal fulfillment and thus might experience distress. Likewise, some people might perceive ambiguity as a challenge that can be overcome and others as a constraint over which he or she has little control and few or no resources with which to cope. More research on validating the measurement of challenge vs. hindrance stressors, as well as eustress vs. distress, and savoring vs. coping, is warranted. Second, at what point are challenge stressors harmful? Just because people experiencing challenge stressors continue to perform well, it does not necessarily mean that they are healthy people. A great deal of stressors are intellectually stimulating, but excessive stimulation can also take a toll on one’s physiological well-being, as evident by the droves of professionals experiencing different kinds of diseases not experienced as much a few decades ago, such as obesity (Fried et al., 2013 ). Third, which stress management interventions would better serve to reduce hindrance stressors or to reduce strain that may result from challenge stressors while reinforcing engagement-producing challenge stressors?
A fourth area that requires additional attention is that of the flexible work arrangements (FWAs). One of the reasons companies have been willing to permit employees to work from home is not so much out of concern for the employee, but out of the company’s need for the focal person to be able to communicate with a colleague working from a geographic region when it is night or early morning for the focal person. Glazer, Kożusznik, and Shargo ( 2012 ) presented several areas for future research on this topic, noting that by participating on global virtual teams, workers face additional stressors, even while given flexibility of workplace and work time. As noted earlier, more research needs to be done on the extent to which people who take advantage of FWAs are advantaged in terms of detachment from work. Can people working from home detach? Are those who find their work invigorating also likely to experience ill-health by not detaching from work?
A fifth area worthy of further research attention is workplace wellness programing. According to Page and Vella-Brodrick ( 2009 ), “subjective and psychological well-being [are] key criteria for employee mental health” (p. 442), whereby mental health focuses on wellness, rather than the absence of illness. They assert that by fostering employee mental health, organizations are supporting performance and retention. Employee well-being can be supported by ensuring that jobs are interesting and meaningful, goals are achievable, employees have control over their work, and skills are used to support organizational and individual goals (Dewe & Kompier, 2008 ). However, just as mental health is not the absence of illness, work stress is not indicative of an absence of psychological well-being. Given the perspective that employee well-being is a state of mind (Page & Vella-Brodrick, 2009 ), we suggest that employee well-being can be negatively affected by noxious job stressors that cannot be remediated, but when job stressors are preventable, employee well-being can serve to protect an employee who faces job stressors. Thus, wellness programs ought to focus on providing positive experiences by enhancing and promoting health, as well as building individual resources. These programs are termed “green cape” interventions (Pawelski, 2016 ). For example, with the growing interests in positive psychology, researchers and practitioners have suggested employing several positive psychology interventions, such as expressing gratitude, savoring experiences, and identifying one’s strengths (Tetrick & Winslow, 2015 ). Another stream of positive psychology is psychological capital, which includes four malleable functions of self-efficacy, optimism, hope, and resilience (Luthans, Youssef, & Avolio, 2007 ). Workplace interventions should include both “red cape” interventions (i.e., interventions to reduce negative experiences) and “green cape” interventions (i.e., workplace wellness programs; Polly, 2014 ).
A Healthy Organization’s Pledge
A healthy workplace requires healthy workers. Period. Among all organizations’ missions should be the focus on a healthy workforce. To maintain a healthy workforce, the company must routinely examine its own contributions in terms of how it structures itself; reinforces communications among employees, vendors, and clients; how it rewards and cares for its people (e.g., ensuring they get sufficient rest and can detach from work); and the extent to which people at the upper levels are truly connected with the people at the lower levels. As a matter of practice, management must recognize when employees are overworked, unwell, and poorly engaged. Management must also take stock of when it is doing well and right by its contributors’ and maintain and reinforce the good practices, norms, and procedures. People in the workplace make the rules; people in the workplace can change the rules. How management sees its employees and values their contribution will have a huge role in how a company takes stock of its own pain points. Providing employees with tools to manage their own reactions to work-related stressors and consequent strains is fine, but wouldn’t it be grand if organizations took better notice about what they could do to mitigate the strain-producing stressors in the first place and take ownership over how employees are treated?
- Abramis, D. J. (1994). Work role ambiguity, job satisfaction, and job performance: Meta-analyses and review. Psychological Report, 75 , 1411–1433.
- Adams, G. A. , & Jex, S. M. (1999). Relationships between time management, control, work–family conflict, and strain. Journal of Occupational Health Psychology, 1 , 72–77.
- Alloy, L. B. , & Abramson, L. Y. (1979). Judgment of contingency in depressed and nondepressed students: Sadder but wiser? Journal of Experimental Psychology: General, 108 , 441–483.
- Amstad, F. T. , Meier, L. L. , Fasel, U. , Elfering, A. , & Semmer, N. K. (2011). A meta-analysis of work-family conflict and various outcomes with a special emphasis on cross-domain versus matching-domain relations. Journal of Occupational Health Psychology, 16 , 151–169.
- Assouline, M. , & Meir, E. I. (1987). Meta-analysis of the relationship between congruence and well-being measures. Journal of Vocational Behavior, 31 , 319–332.
- Aust, B. , & Ducki, A. (2004). Comprehensive health promotion interventions at the workplace: Experiences with health circles in Germany. Journal of Occupational Health Psychology, 9 , 258–270.
- Bakker, A. B. Demerouti, E. , Sanz-Vergel, A. I. (2014). Burnout and work engagement: The JD-R approach. Annual Review of Organizational Behavior, 1 , 389–411.
- Bakker, A. B. , van Veldhoven, M. J. P. M. , & Xanthopoulou, D. (2010). Beyond the demand-control model: Thriving on high job demands and resources. Journal of Personnel Psychology, 9 , 3–16.
- Beehr, T. A. , Glaser, K. M. , Canali, K. G. , & Wallwey, D. A. (2001). Back to basics: Re-examination of demand control theory of occupational stress. Work & Stress, 15 , 115–130.
- Beehr, T. A. , & Glazer, S. (2001). A cultural perspective of social support in relation to occupational stress. In P. Perrewé , D. C. Ganster , & J. Moran (Eds.), Research in occupational stress and well-being (pp. 97–142). Amsterdam: JAI Press.
- Bergman, M. E. , Palmieri, P. A. , Drasgow, F. , & Ormerod, A. J. (2012). Racial/ethnic harassment and discrimination, its antecedents, and its effect on job-related outcomes. Journal of Occupational Health Psychology, 17 , 65–78.
- Bhagat, R. S. , Krishnan, B. , Nelson, T. A. , Leonard, K. M. , Ford, D. J. , & Billing, T. K. (2010). Organizational stress, psychological strain, and work outcomes in six national contexts: A closer look at the moderating influences of coping styles and decision latitude . Cross Cultural Management, 17 , 10–29.
- Bhagat, R. S. , O’Driscoll, M. P. , Babakus, E. , Frey, L. , Chokkar, J. , Ninokumar, B. H , et al. (1994). Organizational stress and coping in seven national contexts: A cross-cultural investigation . In G. P. Keita & J. J. Hurrell (Eds.), Job stress in a changing workforce: Investigating gender, diversity, and family issues (pp. 93–105). Washington, DC: American Psychological Association.
- Bhagat, R. S. , Segovis, J. C. , & Nelson, T. A. (2012). Work stress and coping in the era of globalization . New York: Routledge.
- Billings, A. G. , & Moos, R. H. (1981). The role of coping responses and social resources in attenuating the stress of life events. Journal of Behavioral Medicine, 4 , 139–157.
- Birnie, K. , Speca, M. , & Carlson, L. E. (2010). Exploring self-compassion and empathy in the context of mindfulness-based stress reduction (MBSR). Stress & Health, 26 , 359–371.
- Biron, C. , Gatrell, C. , & Cooper, C. L. (2010). Autopsy of a failure: Evaluating process and contextual issues in an organizational-level work stress intervention. International Journal of Stress Management, 17 , 135–158.
- Bowling, N. A. , & Kirkendall, C. (2012). Workload: A review of causes, consequences, and potential interventions. In J. Houdmont , S. Leka , & R. Sinclair (Eds.), Contemporary occupational health psychology (Vol. 2) (pp. 221–238). Chichester, U.K.: Wiley.
- Breaugh, J. A. , & Colihan, J. P. (1994). Measuring facets of job ambiguity: Construct validity evidence. Journal of Applied Psychology, 79 , 191–202.
- Bruk-Lee, V. , & Spector, P. E. (2006). The social stressors-counterproductive work behaviors link: Are conflicts with supervisors and coworkers the same? . Journal of Occupational Health Psychology, 11 , 145–156.
- Cancelliere, C. , Cassidy, J. D. , Ammendolia, C. , & Côte, P. (2011). Are workplace health promotion programs effective at improving presenteeism in workers? A systematic review and best evidence synthesis of the literature. BMC Public Health, 11 , 395–406.
- Caplan, R. D. (1987). Person–environment fit in organizations: Theories, facts, and values. In A. W. Riley & S. J. Zaccaro (Eds.), Occupational stress and organizational effectiveness (pp. 103–140). New York: Praeger.
- Cartwright, S. , & Cooper, C. L. (2005). Individually targeted interventions. In J. Barling , E. K. Kelloway , & M. R. Frone (Eds.), Handbook of work stress (pp. 607–622). Thousand Oaks, CA: SAGE.
- Cavanaugh, M. A. , Boswell, W. R. , Roehling, M. V. , & Boudreau, J. W. (2000). An empirical examination of self-reported work stress among U.S. managers . Journal of Applied Psychology, 85 , 65–74.
- Chong, D. S. F. , van Eerde, W. , Rutte, C. G. , & Chai, K. H. (2012). Bringing employees closer: The effect of proximity on communication when teams function under time pressure. Journal of Product Innovation Management, 29 , 205–215.
- Chrobot-Mason, D. , & Leslie, J. B. (2012). The role of multicultural competence and emotional intelligence in managing diversity. Psychologist-Manager Journal, 15 , 219–236.
- Cilliers, F. (2011). Individual diversity management and salutogenic functioning. International Review of Psychiatry, 23 , 501–507.
- Claessens, B. C. , Van Eerde, W. , Rutte, C. G. , & Roe, R. A. (2004). Planning behavior and perceived control of time at work . Journal of Organizational Behavior, 25 , 937–950.
- Cooper, C. L. , Dewe, P. D. , & O’Driscoll, M. P. (2011). Employee assistance programs: Strengths, challenges, and future roles. In J. C. Quick , L. E. Tetrick , J. C. Quick , L. E. Tetrick (Eds.), Handbook of occupational health psychology (2d ed.) (pp. 337–356). Washington, DC: American Psychological Association.
- Cooper, C. L. , Dewe, P. J. , & O’Driscoll, M. P. (2001). Organizational stress: A review and critique of theory, research, and applications . Thousand Oaks, CA: SAGE.
- Coovert, M. D. & Thompson, L. F. (2003). Technology and workplace health. In J. C. Quick & L. E. Tetrick (Eds.), Handbook of occupational health psychology (pp. 221–241). Washington, DC: American Psychological Association.
- Dawson, K. M. , O’Brien, K. E. , & Beehr, T. A. (2016). The role of hindrance stressors in the job demand-control-support model of occupational stress: A proposed theory revision . Journal of Organizational Behavior, 37 (3), 397–415.
- Dewe, P. , & Kompier, M. (2008). Foresight mental capital and wellbeing project: Wellbeing and work: Future challenges . London: The Government Office for Science.
- Dopkeen, J. C. , & DuBois, R. (2014). Stress in the workplace: A policy synthesis on its dimensions and prevalence . White paper. University of Illinois Chicago, Center for Employee Health Studies, School of Public Health.
- Dwyer, D. J. , & Ganster, D. C. (1991). The effects of job demands and control on employee attendance and satisfaction. Journal of Organizational Behavior, 12 , 595–608.
- Ebunlomo, E. O. , Hare-Everline, N. , Weber, A. , & Rich, J. (2015). Development of a comprehensive 12-week health promotion program for Houston Airport System. Texas Public Health Journal, 67 (1), 11–13.
- Edwards, J. R. (2008). Person-environment fit in organizations: An assessment of theoretical progress. The Academy of Management Annals, 2 , 167–230.
- Etzion, D. , Eden, D. , & Lapidot, Y. (1998). Relief from job stressors and burnout: Reserve service as a respite. Journal of Applied Psychology, 83 , 577–585.
- Firth-Cozens, J. (2003). Doctors, their wellbeing, and their stress: It’s time to be proactive about stress—and prevent it. British Medical Journal, 326 , 670–671.
- Flaxman, P. E. , & Bond, F. W. (2010). Worksite stress management training: Moderated effects and clinical significance. Journal of Occupational Health Psychology, 15 , 347–358.
- Folkman, S. , & Lazarus, R. S. (1980). An analysis of coping in a middle-aged community sample . Journal of Health and Social Behavior, 21 , 219–239.
- French, J. R. P., Jr. , & Caplan, R. D. (1972). Organizational stress and individual strain. In A. Marrow (Ed.), The failure of success . New York: AMACOM.
- French, J. R. P., Jr. , & Kahn, R. L. (1962). A programmatic approach to studying the industrial environment and mental health. Journal of Social Issues, 18 , 1–48.
- French, S. (2015, May 27). PCS workload and work-life balance survey 2013 . London: Public and Commercial Services Union.
- Fried, Y. , Laurence, G. A. , Shirom, A. , Melamed, S. , Toker, S. , Berliner, S. , & Shapira, I. (2013). The relationship between job enrichment and abdominal obesity: A longitudinal field study of apparently healthy individuals. Journal of Occupational Health Psychology, 18 , 458–468.
- Frone, M. R. (2000). Interpersonal conflict at work and psychological outcomes: Testing a model among young workers. Journal of Occupational Health Psychology, 5 , 246–255.
- Giga, S. I. , Cooper, C. L. , & Faragher, B. (2003). The development of a framework for a comprehensive approach to stress management interventions at work. International Journal of Stress Management, 10 , 280–296.
- Glazer, S. (2008). Cross-cultural issues in stress and burnout. In J. R. B. Halbesleben (Ed.), Handbook of Stress and Burnout in Health Care (pp. 79–93). Huntington, NY: Nova Science Publishers.
- Glazer, S. , & Beehr, T. A. (2005). Consistency of the implications of three role stressors across four countries. Journal of Organizational Behavior , 26 , 467–487.
- Glazer, S. , Kożusznik, M. W. , Meyers, J. H. , & Ganai, O. (2014). Cultural implications of meaningfulness as a resource to mitigate work stress. In S. Leka & R. Sinclair (Eds.), Contemporary occupational health psychology: Global perspectives on research and practice (Vol. 3) (pp. 114–130). Hoboken, NJ: Wiley.
- Glazer, S. , Kożusznik, M. W. , & Shargo, I. A. (2012). Global virtual teams: A cure for- or a cause of- stress. In P. L. Perrewé , J. Halbesleben , & C. Rosen (Eds.), Research in occupational stress and well being: The role of the economic context on occupational stress and well being (Vol. 10, pp. 213–266). Bingley, U.K.: Emerald.
- Glazer, S. , Stetz, T. A. , & Izso, L. (2004). Effects of personality on subjective job stress: A cultural analysis. Personality and Individual Differences, 37 , 645–658.
- Greenhaus, J. H. , & Beutell, N. J. (1985). Sources of conflict between work and family roles. Academy of Management Review, 10 , 76–88.
- Hackman, J. R. , & Oldham, G. R. (1980). Work Redesign . Reading, MA: Addison-Wesley.
- Hauke, A. , Flintrop, J. , Brun, E. , & Rugulies, R. (2011). The impact of work-related psychosocial stressors on the onset of musculoskeletal disorders in specific body regions: A review and meta-analysis of 54 longitudinal studies . Work & Stress, 25 , 243–256.
- Health & Safety Executive (n.d.). Cardiff and Value University Health Board—A stress case study .
- Heron, K. E. , & Smyth, J. M. (2010). Ecological momentary interventions: Incorporating mobile technology into psychosocial and health behaviour treatments. British Journal of Health Psychology, 15 , 1–39.
- Hershcovis, M. (2011). “Incivility, social undermining, bullying … oh my!”: A call to reconcile constructs within workplace aggression research . Journal of Organizational Behavior, 32 , 499–519.
- Higgins, J. E. , & Endler, N. S. (1995). Coping, life stress, and psychological and somatic distress . European Journal of Personality, 9 , 253–270.
- Hobfoll, S. E. (1989). Conservation of resources: A new attempt at conceptualizing stress. American Psychologist, 44 , 513–524.
- Hobfoll, S. E. (1998). Stress, culture, and community: The psychology and philosophy of stress . New York: Plenum Press.
- Hobfoll, S. E. (2001). The influence of culture, community, and the nested-self in the stress process: Advancing Conservation of Resources Theory. Applied Psychology: An International Review, 50 , 337–421.
- International Labor Organization (2012, July 5). Why stress at work matters . International Labor Organization.
- International Labor Organization (n.d.). Psychosocial risks and work-related stress . International Labor Organization.
- Jackson, S. E. , & Schuler, R. S. (1985). A meta-analysis and conceptual critique of research on role ambiguity and role conflict in work settings. Organizational Behavior and Human Decision Processes, 36 , 16–78.
- Jayson, S. (2012, January 11). Yeah, we’re stressed but dealing with it; Americans report a decrease in stress for the first time in five years, maybe because it’s just the new normal . USA Today .
- Jex, S. M. , & Beehr, T. A. (1991). Emerging theoretical and methodological issues in the study of work-related stress. Research in Personnel and Human Resources Management, 9 , 311–365.
- Jex, S. M. , & Elaqua, T. C. (1999). Time management as a moderator of relations between stressors and employee strain. Work & Stress, 13 , 182–191.
- Johnson, J. V. , & Hall, E. M. (1988). Job strain, workplace social support, and cardiovascular disease: A cross-sectional study of a random sample of the Swedish working population. American Journal of Public Health, 78 , 1336–1342.
- Kahn, R. L. , Wolfe, D. M. , Quinn, R. P. , Snoek, J. D. , & Rosenthal, R. A. (1964). Organizational stress: Studies in role conflict and ambiguity . New York: Wiley.
- Kannampallil, T. G. , Waicekauskas, K. , Morrow, D. G. , Kopren, K. M. , & Fu, W. (2013). External tools for collaborative medication scheduling. Cognition, Technology & Work, 15 , 121–131.
- Karasek, R. A. (1979). Job demands, job decision latitude, and mental strain: Implications for job redesign. Administrative Science Quarterly , 24 , 285–308.
- Karasek, R. A. , & Theorell, T. (1990). Healthy work: Stress, productivity, and the reconstruction of working life . New York: Basic Books.
- van der Klink, J. J. L. , Blonk, R. W. B. , Schene, A. H. , & van Dijk, F. J. H. (2001). The benefits of interventions for work-related stress. American Journal of Public Health, 91 , 270–276.
- Knight, B. G. , Silverstein, M. , McCallum, T. J. , & Fox, L. S. (2000). A sociocultural stress and coping model for mental health outcomes among African American caregivers in southern California . The Journals of Gerontology: Series B: Psychological Sciences and Social Sciences, 55B , 142–150.
- Kossek, E. E. , Thompson, R. J. , Lautsch, B. A. (2015). Balanced workplace flexibility: Avoiding the traps. California Management Review, 57 , 5–25.
- Kożusznik, M. , Rodriguez, I. , & Peiró, J. M. (2012). Cross-national outcomes of stress appraisal. Cross Cultural Management, 19 , 507–525.
- Kożusznik, M. , Rodriguez, I. , & Peiró, J. M. (2015). Eustress and distress climates in teams: Patterns and outcomes. International Journal of Stress Management, 22 , 1–23.
- Kristof-Brown, A. L. , Zimmerman, R. D. , & Johnson, E. C. (2005). Consequences of individuals’ fit at work: A meta-analysis of person-job, person-organization, person-group, and person-supervisor fit. Personnel Psychology, 58 , 281–342.
- LaMontagne, A. D. , Keegel, T. , Louie, A. M. , Ostry, A. , & Landsbergis, P. A. (2007). A systematic review of the job-stress intervention evaluation literature, 1990–2005. International Journal of Occupational and Environmental Health, 13 , 268–280.
- LaRocco, J. M. , Tetrick, L. E. , & Meder, D. (1989). Differences in perceptions of work environment conditions, job attitudes, and health beliefs among military physicians, dentists, and nurses. Military Psychology, 1 , 135–151.
- Lazarus, R. S. , & Folkman, S. (1984). Stress, appraisal, and coping . New York: Springer.
- Lazarus, R. S. , & Folkman, S. (1991). The concept of coping. In A. Monat & R. S. Lazarus (Eds.), Stress and coping: An anthology (3d ed.) (pp. 189–206). New York: Columbia University Press.
- LePine, J. A. , Podsakoff, N. P. , & LePine, M. A. (2005). A meta-analytic test of the challenge stressor-hindrance stressor framework: An explanation for inconsistent relationships among stressors and performance. Academy of Management Journal, 48 , 764–775.
- Lewin, K. (1936). Principles of topological psychology . New York: McGraw-Hill.
- Lewin K. (1951). Field theory in social science . New York: Harper and Row.
- Lewin, K. (1997). Resolving social conflicts & Field theory in social science . Washington, DC: American Psychological Association. Previously published in 1948 and 1951.
- Lin, B. C. , Kain, J. M. , & Fritz, C. (2013). Don’t interrupt me! An examination of the relationship between intrusions at work and employee strain. International Journal of Stress Management, 20 , 77–94.
- Liu, C. , & Li, H. (2017) Stressor and stressor appraisals: The moderating effect of task efficacy . Journal of Business and Psychology , 1–14.
- Liu, C. , Liu, Y. , Spector, P. E. , Shi, L. (2011). The interaction of job autonomy and conflict with supervisor in China and the United States: A qualitative and quantitative comparison. International Journal of Stress Management, 18 , 222–245.
- Liu, C. , Spector, P. E. , & Shi, L. (2007). Cross-national job stress: A quantitative and qualitative study. Journal of Organizational Behavior, 28 , 209–239.
- Luckhaupt, S. E. , Tak, S. , Calvert, G. M. (2010). The prevalence of short sleep duration by industry and occupational in the National Health Interview Survey. Sleep, 33 , 149–159.
- Luthans, F. , Youssef, C. M. , & Avolio, B. J. (2007). Psychological capital: Developing the human competitive edge . New York: Oxford University Press.
- Macan, T. H. (1994). Time management: Test of a process model. Journal of Applied Psychology, 79 , 381–391.
- Macan, T. H. , Shahani, C. , Dipboye, R. L. , & Philips, A. P. (1990). College students’ time management: Correlations with academic performance and stress. Journal of Educational Psychology, 82 , 760–768.
- Masuda, A. D. , Poelmans, S. A. Y. , Allen, T. D. , Spector, P. E. , Lapierre, L. M. , Cooper, C. L. , et al. (2012). Flexible work arrangements availability and their relationship with work-to-family conflict, job satisfaction, and turnover intentions: A comparison of three country clusters. Applied Psychology: An International Review, 61 , 1–29.
- McMahon, M. (2007). Think you might be addicted to email? You’re not alone . AOL.
- Monat, A. , & Lazarus, R. S. (Eds.). (1991). Stress and coping: An anthology (3d ed.). New York: Columbia University Press.
- Morimoto, H. , Shimada, H. , & Ozaki, K. (2013). Does stressor evaluation mediate sociocultural influence on coping selection? An investigation using Japanese employees. International Journal of Stress Management, 20 , 1–19.
- Narayanan, L. , Menon, S. , & Spector, P. E. (1999). A cross-cultural comparison of job stressors and reactions among employees holding comparable jobs in two countries. International Journal of Stress Management, 6 , 197–212.
- National Sleep Foundation (2005). Segment profiles . National Sleep Foundation.
- National Sleep Foundation (2013). How much sleep do adults need? . National Sleep Foundation.
- Nelson, D. L. , & Simmons, B. L. (2003). Health psychology and work stress: A more positive approach. In J. C. Quick & L. E. Tetrick (Eds.), Handbook of Occupational Health Psychology (pp. 97–119). Washington, DC: American Psychological Association.
- Norris, P. A. , Fahrion, S. L. , & Oikawa, L. O. (2007). Autogenic biofeedback training in psychophysiological therapy and stress management. In P. M. Lehrer , R. L. Woolfolk , & W. E. Sime (Eds.), Principles and practices of stress management (3d ed., pp. 175–205). New York: Guilford.
- Ogawa, N. (2009). Stress, coping behavior, and social support in Japan and the United States. Dissertation Abstracts International Section A , 69 , 3802.
- Oksanen, K. , & Ståhle, P. (2013). Physical environment as a source for innovation: Investigating the attributes of innovative space. Journal of Knowledge Management, 17 , 815–827.
- Page, K. M. , & Vella-Brodrick, D. A. (2009). The “what,” “why” and “how” of employee well-being: A new model. Social Indicators Research, 90 , 441–458.
- Parasuraman, S. , & Cleek, M. A. (1984). Coping behaviors and managers’ affective reactions to role stressors . Journal of Vocational Behavior, 24 , 179–193.
- Parasuraman, S. , & Purohit, Y. S. (2000). Distress and boredom among orchestra musicians: The two faces of stress. Journal of Occupational Health Psychology, 5 , 74–83.
- Pawelski, J. O. (2016). Defining the “positive” in positive psychology: Part II. A normative analysis . Journal of Positive Psychology, 11 , 357–365.
- Pearlin, L. I. , & Schooler, C. (1978). The structure of coping . Journal of Health and Social Behavior, 19 , 2–21.
- Peeters, M. A. G. , & Rutte, C. G. (2005). Time management behavior as a moderator for the job demand-control interaction. Journal of Occupational Health Psychology , 1 , 64–75.
- Peters, L. H. , & O’Connor, E. J. (1980). Situational constraints and work outcomes: The influence of a frequently overlooked construct. Academy of Management Review , 5, 391–397.
- Peters, L. H. , & O’Connor, E. J. (1988). Measuring work obstacles: Procedures, issues, and implications. In F. D. Schoorman & B. Schneider (Eds.), Facilitating work effectiveness (pp. 105–123). Lexington, MA: Lexington Books.
- Polly, S. (2014, July 2). Workplace well-being is not an oxymoron . Positive Psychology News Daily .
- Quick, C. J. , Quick, J. D. , Nelson, D. L. , & Hurrell, J. J. (2003). Preventive stress management in organizations . Washington, DC: APA.
- Quillian-Wolever, R. E. , & Wolever, M. E. (2003). Stress management at work . In J. C. Quick & L. E. Tetrick (Eds.), Handbook of occupational health psychology (pp. 355–375). Washington, DC: American Psychological Association.
- Ragsdale, J. M. , Beehr, T. A. , Grebner, S. , & Han, K. (2011). An integrated model of weekday stress and weekend recovery of students. International Journal of Stress Management, 18 , 153–180.
- Richardson, K. M. , & Rothstein, H. R. (2008). Effects of occupational stress management intervention programs: A meta-analysis. Journal of Occupational Health Psychology, 13 , 69–93.
- Rodríguez, I. , Kozusznik, M. W. , & Peiró, J. M. (2013). Development and validation of the Valencia Eustress-Distress Appraisal Scale. International Journal of Stress Management, 20 , 279–308.
- Rothbaum, F. , Weisz, J. R. , & Snyder, S. S. (1982). Changing the world and changing the self: A two-process model of perceived control. Journal of Personality and Social Psychology, 42 , 5–37.
- Rotter, J. B. (1966). Generalized expectancies for internal versus external control of reinforcement. Psychological Monographs, 80 , 609.
- Rousseau, V. , & Aubé, C. (2010). Social support at work and affective commitment to the organization: The moderating effect of job resource adequacy and ambient conditions. Journal of Social Psychology, 150 , 321–340.
- Saunders, T. , Driskell, J. E. , Johnston, J. , & Salas, E. (1996). The effect of stress inoculation training on anxiety and performance. Journal of Occupational Health Psychology, 1 , 170–186.
- Schaubroeck, J. , Ganster, D. C. , Sime, W. E. , & Ditman, D. (1993). A field experiment testing supervisory role clarification. Personnel Psychology, 46 , 1–25.
- Selmer, J. (2002). Coping strategies applied by Western vs overseas Chinese business expatriates in China. International Journal of Human Resource Management, 13 , 19–34.
- Siegrist, J. (1996). Adverse health effects of high effort/low reward conditions. Journal of Occupational Health Psychology, 1 , 27–41.
- Siegrist, J. (2010). Effort-reward imbalance at work and cardiovascular diseases. International Journal of Occupational Medicine and Environmental Health, 23 , 279–285.
- Siegrist, J. , Dragano, N. , Nyberg, S. T. , Lunau, T. , Alfredsson, L. , Erbel, R. , et al. (2014). Validating abbreviated measures of effort-reward imbalance at work in European cohort studies: The IPD-Work consortium. International Archives of Occupational and Environmental Health, 87 , 249–256.
- Sinha, B. K. , Willson, L. R. , & Watson, D. C. (2000). Stress and coping among students in India and Canada . Canadian Journal of Behavioural Science/Revue Canadienne Des Sciences Du Comportement , 32 (4), 218–225.
- Sinnott, J. , & Vatz, R. E. (2015, March 13). Maryland doesn’t trust state employees to manage their health . Baltimore Sun .
- Siu, O. L. , Cooper, C. L. , & Phillips, D. R. (2013, July 1). Intervention studies on enhancing work well-being, reducing burnout, and improving recovery experiences among Hong Kong health care workers and teachers . International Journal of Stress Management, 21 , 69–84.
- Sonnentag, S. (2012). Psychological detachment from work during leisure time: The benefits of mentally disengaging from work. Current Directions in Psychological Science, 21 , 114–118.
- Sørensen, O. H. , & Holman, D. (2014). A participative intervention to improve employee well-being in knowledge work jobs: A mixed-methods evaluation study. Work & Stress, 28 , 67–86.
- Spector, P. E. , Chen, P. Y. , & O’Connell, B. J. (2000). A longitudinal study of relations between job stressors and job strains while controlling for prior negative affectivity and strains. Journal of Applied Psychology, 85 , 211–218.
- Spector, P. E. , & Jex, S. M. (1998). Development of four self-report measures of job stressors and strains: Interpersonal Conflict at Work Scale, Organizational Constraints Scale, Quantitative Workload Inventory, and Physical Symptoms Inventory. Journal of Occupational Health Psychology, 3 , 356–367.
- State of Maryland . (n.d.). Wellness program frequently asked questions . Maryland.gov.
- Strentz, T. , & Auerbach, S. M. (1988). Adjustment to the stress of simulated captivity: Effects of emotion-focused versus problem-focused preparation on hostages differing in locus of control . Journal of Personality and Social Psychology, 55 , 652–660.
- Swanberg, J. E. , McKechnie, S. P. , Ojha, M. U. , & James, J. B. (2011). Schedule control, supervisor support and work engagement: A winning combination for workers in hourly jobs? Journal of Vocational Behavior, 79 , 613–624.
- Tarafdar, M. , Tu, Q. , Ragu-Nathan, B. S. , & Ragu-Nathan, T. , (2007). The impact of technostress on role stress and productivity. Journal of Management Information Systems, 24 , 301–328.
- Tepper, B. J. , & Henle, C. A. (2011). A case for recognizing distinctions among constructs that capture interpersonal mistreatment in work organizations . Journal of Organizational Behavior, 32 , 487–498.
- Tetrick, L. E. , & Winslow, C. J. (2015). Workplace stress management interventions and health promotion. Annual Review of Organizational Psychology and Organizational Behavior, 2 , 583–603.
- Thomas, D. C. , Au, K. , & Ravlin, E. C. (2003). Cultural variation and the psychological contract. Journal of Organizational Behavior, 24 , 451–471.
- Toker, S. , Shirom, A. , Melamed, S. , & Armon, G. (2012). Work characteristics as predictors of diabetes incidence among apparently healthy employees. Journal of Occupational Health Psychology, 17 , 259–267.
- Velez, B. L. , Moradi, B. , & Brewster, M. E. (2013). Testing the tenets of minority stres theory in workplace contexts. Journal of Counseling Psychology, 60 , 532–542.
- Verquer, M. L. , Beehr, T. A. , & Wagner, S. H. (2003). A meta-analysis of relations between person–organization fit and work attitudes. Journal of Vocational Behavior, 63 , 473–489.
- Villani, D. , Grassi, A. , Cognetta, C. , Toniolo, D. , Cipresso, P. , & Riva, G. (2013). Self-help stress management training through mobile phones: An experience with oncology nurses. Psychological Services , 10 , 315–322.
- Vischer, J. C. (2007). The effects of the physical environment on job performance: Towards a theoretical model of workspace stress. Stress & Health, 23 , 175–184.
- Wasti, S. A. , & Cortina, L. M. (2002). Coping in context: Sociocultural determinants of responses to sexual harassment . Journal of Personality and Social Psychology , 83, 394–405.
- Willert, M. V. , Thulstrup, A. M. , Hertz, J. , & Bonde, J. P. (2010). Sleep and cognitive failures improved by a three-month stress management intervention . International Journal of Stress Management, 17 , 193–213.
- Xiao Q. , Ottosson I. , & Carlsson I. (2013). Stressors and coping strategies in Chinese and Swedish students at a Swedish university. Chinese Journal of Clinical Psychology, 21 , 309–312.
Related Articles
- Work and Family
- Organizational Climate and Culture
- Physical Activity and Stress Reactivity
- The Roles of Psychological Stress, Physical Activity, and Dietary Modifications on Cardiovascular Health Implications
- Inflammation as a Biomarker Method in Lifespan Developmental Methodology
- Stress and Coping Theory Across the Adult Lifespan
- Occupational Health Psychology
Printed from Oxford Research Encyclopedias, Psychology. Under the terms of the licence agreement, an individual user may print out a single article for personal use (for details see Privacy Policy and Legal Notice).
date: 14 September 2024
- Cookie Policy
- Privacy Policy
- Legal Notice
- Accessibility
- [81.177.182.159]
- 81.177.182.159
Character limit 500 /500
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Coping strategies: a prospective study of patterns, stability, and relationships with psychological distress
- PMID: 24697686
- DOI: 10.1111/sjop.12103
The aims of this article are: (1) to explore patterns (clusters) of coping strategies; (2) to examine the stability of individual coping strategies and patterns of coping over time; and (3) to establish long term associations between coping and psychological distress. Coping strategies were assessed with the Brief Cope questionnaire, whereas psychological distress was measured with the ten-item version of the Hopkins Symptom Checklist, in a two-year prospective sample comprising 3,738 employees. Based on TwoStep cluster analysis of the Brief Cope, three different coping patterns were identified: low coping, engagement coping, and disengagement coping. Analyses of long-term stability indicated malleable properties for the individual coping strategies as well as the three clusters. Disengagement coping strategies in the form of self-blame and self-distraction were most strongly associated with distress at follow-up, whereas baseline distress was related to increased use of these strategies two years later. Coping patterns at baseline had no main effects on later levels of distress, but levels of distress at baseline predicted subsequent use of engagement and disengagement coping patterns. The finding that specific coping strategies are malleable suggests that it is possible to modify and develop dysfunctional strategies. The associations between disengagement coping strategies and distress indicate that this kind of coping is especially problematic with regard to mental health problems. A main contribution of this study is that it establishes cluster analytic techniques as beneficial in the assessment of coping.
PubMed Disclaimer
Similar articles
- [Multidimensional assessment of coping: validation of the Brief COPE among French population]. Muller L, Spitz E. Muller L, et al. Encephale. 2003 Nov-Dec;29(6):507-18. Encephale. 2003. PMID: 15029085 French.
- Farmers' stress and coping in a time of drought. Gunn KM, Kettler LJ, Skaczkowski GL, Turnbull DA. Gunn KM, et al. Rural Remote Health. 2012;12:2071. Epub 2012 Oct 9. Rural Remote Health. 2012. PMID: 23067269
- Acute stress reactions and associated factors in the help-seekers after the L'Aquila earthquake. Casacchia M, Bianchini V, Mazza M, Pollice R, Roncone R. Casacchia M, et al. Psychopathology. 2013;46(2):120-30. doi: 10.1159/000339459. Epub 2012 Aug 21. Psychopathology. 2013. PMID: 22922557
- Longitudinal association between coping and psychological distress in rheumatoid arthritis: a systematic review. Vriezekolk JE, van Lankveld WG, Geenen R, van den Ende CH. Vriezekolk JE, et al. Ann Rheum Dis. 2011 Jul;70(7):1243-50. doi: 10.1136/ard.2010.143271. Epub 2011 Apr 7. Ann Rheum Dis. 2011. PMID: 21474486 Review.
- An integrative review of coping related to problematic computer use in adolescence. Trnka R, Martínková Z, Tavel P. Trnka R, et al. Int J Public Health. 2016 Apr;61(3):317-27. doi: 10.1007/s00038-015-0693-8. Epub 2015 May 27. Int J Public Health. 2016. PMID: 26012847 Review.
- Predictors of poor psychological functioning of healthcare workers based in Greece during the COVID-19 pandemic. Puri BK, Miari A, Theodoratou M. Puri BK, et al. Health Psychol Res. 2023 Dec 28;11:91274. doi: 10.52965/001c.91274. eCollection 2023. Health Psychol Res. 2023. PMID: 38162540 Free PMC article.
- A longitudinal study of loneliness in autism and other neurodevelopmental disabilities: Coping with loneliness from childhood through adulthood. Schiltz H, Gohari D, Park J, Lord C. Schiltz H, et al. Autism. 2024 Jun;28(6):1471-1486. doi: 10.1177/13623613231217337. Epub 2023 Dec 28. Autism. 2024. PMID: 38153097 Free PMC article.
- Veterans and Nonveterans Coping With Stress During 4 Months of COVID-19. Butler JM, Wang X, Riddoch M, Thorpe A, Stevens V, Scherer LD, Drews FA, Shoemaker H, Fagerlin A. Butler JM, et al. Ann Fam Med. 2023 Nov-Dec;21(6):508-516. doi: 10.1370/afm.3046. Ann Fam Med. 2023. PMID: 38012035 Free PMC article.
- Living by the sea: place attachment, coastal risk perception, and eco-anxiety when coping with climate change. Parreira N, Mouro C. Parreira N, et al. Front Psychol. 2023 Jun 22;14:1155635. doi: 10.3389/fpsyg.2023.1155635. eCollection 2023. Front Psychol. 2023. PMID: 37425177 Free PMC article.
- Satisfaction with Life and Coping Strategies among Patients with Hidradenitis Suppurativa: A Cross-Sectional Study. Rymaszewska JE, Krajewski PK, Matusiak Ł, Maj J, Szepietowski JC. Rymaszewska JE, et al. J Clin Med. 2023 Apr 7;12(8):2755. doi: 10.3390/jcm12082755. J Clin Med. 2023. PMID: 37109092 Free PMC article.
- Search in MeSH
LinkOut - more resources
Full text sources, other literature sources.
- scite Smart Citations
- MedlinePlus Health Information
Research Materials
- NCI CPTC Antibody Characterization Program

- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
ORIGINAL RESEARCH article
Coping strategies and self-efficacy in university students: a person-centered approach.

- 1 Department of Psychology, University of A Coruña, A Coruña, Spain
- 2 Department of Pedagogy and Didactics, University of Santiago de Compostela, Santiago de Compostela, Spain
- 3 Faculty of Psychology, University of Oviedo, Oviedo, Spain
In daily academic life, students are exposed to a wide range of potentially stressful situations which could negatively affect their academic achievement and their health. Among the factors that could be weakened by academic stress, attention has been paid to expectations of self-efficacy, which are considered one of the most important determinants for student engagement, persistence, and academic success. From a proactive perspective, research on academic stress has emphasized the importance of coping strategies in preventing harmful consequences. In recent years, there has been a growing interest in discovering the extent to which individuals are able to combine different coping strategies and the adaptive consequences this flexibility entails. However, studies using this person-centered approach are still scarce in the academic context. On that basis, this current study had two objectives: (a) to examine the existence of different profiles of university students based on how they combined different approach coping strategies (positive reappraisal, support seeking, and planning) and (b) to determine the existence of differences in general expectations of self-efficacy between those coping profiles. A total of 1,072 university students participated in the study. The coping profiles were determined by latent profile analysis (LPA). The differences in the self-efficacy variable were determined using ANCOVA, with gender, university year, and degree type as covariates. Four approach coping profiles were identified: (a) low generalized use of approach coping strategies; (b) predominance of social approach coping approaches; (c) predominance of cognitive approach coping approaches; and (d) high generalized use of approach coping strategies. The profile showed that a greater combination of the three strategies was related to higher general self-efficacy expectations and vice versa. These results suggest that encouraging flexibility in coping strategies would help to improve university students’ self-efficacy.
Introduction
The mental health of university students has been a growing concern in recent years ( Milojevich and Lukowski, 2016 ). Various studies have demonstrated the high frequency of psychological symptoms associated with this stage of education ( Blanco et al., 2008 ; Kim et al., 2015 ), with stress being one of the psychosocial problems that have become prevalent ( Deasy et al., 2014 ; American College Health Association, 2018 ; Gustems-Carnicer et al., 2019 ). In their daily lives, university students have to face a wide variety of demands, both academic and non-academic, that could affect their well-being. Academic demands include adaptation to a new context, overwork, insufficient time to do their academic tasks, preparation for and doing of exams, and the pressure to perform ( Beiter et al., 2015 ; Vizoso and Arias, 2016 ; Erschens et al., 2018 ; Webber et al., 2019 ). Non-academic demands include change of where they live; the need to create new social relationships; conflicts with partners, family, or friends; money worries; and concerns about future work ( Howard et al., 2006 ; Galatzer-Levy et al., 2012 ; DeRosier et al., 2013 ; Beiter et al., 2015 ). Stress can bring with it significant harm to the student’s academic performance (e.g., reduced ability to pay attention or to memorize, less dedication to study, and more absences from class) ( Chou et al., 2011 ; Turner et al., 2015 ), as well as to the student’s physical and psychological health (e.g., substance abuse, insomnia, anxiety, and physical and emotional exhaustion) ( Waqas et al., 2015 ; Schönfeld et al., 2016 ). These harmful effects have triggered interest in the identification of individual psychological resources that could be protective factors against the inherent stressors of the university context ( Tavolacci et al., 2013 ). These resources would modulate the relationship between the potential threats and the stress response, encouraging better psychological adjustment ( Leiva-Bianchi et al., 2012 ). Two of the most widely studied resources are coping strategies and self-efficacy.
Coping Strategies
Lazarus and Folkman (1984) thought of stress as an interactive process between the person and their surroundings, in which the influence of stressful events on physical and psychological well-being is determined by coping. From this widely accepted transactional approach, coping would come to be defined by cognitive and behavioral efforts employed in response to external or internal demands that the individual deems to be threats to their well-being.
Despite the documentation of more than 400 coping strategies ( Skinner et al., 2003 ), they are generally categorized into two broad types (for a complete categorization, see Zimmer-Gembeck and Skinner, 2016 ): approach (also called active) strategies and evasive (or disengagement) strategies. Approach strategies involve cognitive and behavioral mechanisms aimed at making an active response to the stressor, directly changing the problem (primary control) or the negative emotions associated with it (secondary control). This category includes strategies such as planning, taking specific action, seeking support (instrumental and emotional), positive reappraisal of the situation, or acceptance. Evasive strategies are those which involve cognitive and behavioral mechanisms used to evade the stressful situation, such as distraction, denial, and wishful thinking. Based on this classification, there is a broad consensus that approach strategies are related to good academic, physical, and psychological adjustment ( Clarke, 2006 ; Syed and Seiffge-Krenke, 2015 ; Gustems-Carnicer et al., 2019 ), whereas evasive strategies usually mean maladaptive consequences for the students ( Tavolacci et al., 2013 ; Deasy et al., 2014 ; Skinner et al., 2016 ; Tran and Lumley, 2019 ).
Self-Efficacy
Expectations of self-efficacy are a central element of the social cognitive theory proposed by Bandura (1997) . This construct is about a person’s beliefs about their ability to mobilize courses of action needed to achieve desired personal goals. It is, therefore, a fundamental psychological resource for exercising control over events in one’s life ( Wood and Bandura, 1989 ). In fact, self-efficacy is considered a powerful motivational, cognitive, and affective determinant of student behavior, with significant influence on their involvement, effort, persistence, self-regulation, and achievement ( Schunk and Pajares, 2010 ; Honicke and Broadbent, 2016 ; Ritchie, 2016 ; Zumbrunn et al., 2019 ). These characteristics make self-efficacy an important variable in controlling stress ( Bandura et al., 2003 ; Sahin and Çetin, 2017 ; Lanin et al., 2019 ), and it is a protection factor against the impact of day-to-day stressors at university ( Freire et al., 2019 ; Schönfeld et al., 2019 ).
Although self-efficacy has commonly been characterized as an expectation that is strongly linked to a specific task or situation, various studies have demonstrated the existence of a more generalized belief—that is, general self-efficacy—around perceived competence in the face of a broad range of demands ( Scholz et al., 2002 ; Feldman et al., 2015 ; Volz et al., 2019 ).
Current Study
The literature reviewed reiterated the importance of considering both coping strategies and expectations of self-efficacy in protection against stress. However, far from being independent resources, some studies have suggested that coping strategies and self-efficacy are related. They postulate that coping behaviors would influence an individual’s expectations of control ( Lazarus and Folkman, 1984 ), such that self-efficacy would be a mediator between coping strategies and the stress response ( Zimmer-Gembeck and Skinner, 2016 ).
Given that, our study aimed to examine the possible influence of coping strategies on the expectations of self-efficacy in a population that is particularly vulnerable to stress, university students. Some studies have shown a positive, significant influence of approach coping strategies on self-efficacy in infant samples ( Sandler et al., 2000 ) and in adults with rheumatoid arthritis ( Keefe et al., 1997 ). However, as far as we are aware, there have been none in the university context.
The main contribution of this study lies in the analysis of student coping strategies using a person-centered focus. Traditionally, research on coping strategies has attempted to determine the suitability of a given strategy, evaluating the benefit or harm that it produces for the individual. This variable-centered approach assumes that certain coping mechanisms are universally adaptive or maladaptive, an argument that has been called the “fallacy of uniform efficacy” ( Bonanno and Burton, 2013 ).
The very characterization of coping strategies as responses to a specific challenge demonstrates their situational specificity. This has led in recent years to the adoption of an approach based on the flexibility of coping, under the supposition that a single individual can combine different strategies, using one or the other depending on the specific situation they are facing ( Eisenbarth, 2012 ; Kobylińska and Kusev, 2019 ). In this vein, the benefits provided by approach coping strategies are maximized if the individual employs problem-focused coping strategies (e.g., planning and seeking instrumental support) or emotion-centered strategies (e.g., positive reappraisal and seeking emotional support) based on the perceived controllability of the stressor facing them ( Cheng, 2001 ; Siltanen et al., 2019 ). In contrast, people who are less flexible in their coping have a smaller repertoire of strategies, which are less effective adjusting to the specific demands of the situation ( Cheng and Cheung, 2005 ).
Studying individuals’ profiles in light of the flexibility of their coping is therefore adopting a person-centered focus ( Laursen and Hoff, 2006 ), making it possible to identify subgroups of students characterized by high internal similarity in their repertoire of coping strategies, who differ from the way that other students combine their strategies. An additional advantage over the traditional, variable-focused approaches is that studying profiles of flexibility of coping makes it possible to identify specific groups of individuals who can be prioritized in the design of interventions ( Kaluza, 2000 ).
Considering a perspective based on coping flexibility, the research question we posed in this study was whether the different student profiles—in the way they combine their coping strategies—would be related to significantly different levels of general self-efficacy. In the university context, various studies have demonstrated that, in comparison to those with less flexible profiles, students who are more flexible in their coping demonstrate lower vulnerability to stress ( Cheng, 2001 ; Kato, 2012 ; Doron et al., 2014 ; González Cabanach et al., 2018 ) and to depressive symptomatology ( Gabrys et al., 2018 ; Hasselle et al., 2019 ), as well as greater psychological well-being ( Freire et al., 2018 ). Based on that research, our hypothesis is that students who exhibit a more flexible profile of strategies will demonstrate significantly higher levels of self-efficacy than less flexible students.
Assuming that in the young population the use of approach coping strategies is more typical ( Cheng et al., 2014 ), in our study, we examined coping profiles based on the combination of three approach strategies that are very common in educational contexts ( Skinner et al., 2016 ): a primary control (planning), a secondary control (positive reappraisal), and a mixed type (seeking instrumental and emotional support). Similarly, given the extensive and varied range of demands faced by students in their daily lives (both academic and non-academic), we examined their level of general self-efficacy. Finally, in this study, we also tried to control for the effects of the variables gender, university year, and degree type. It would seem that men report higher levels of self-efficacy than women, with this difference emerging at the end of adolescence ( Huang, 2013 ). It may also be the case that students in their first year of university, because of their inexperience, may have lower levels of self-efficacy than students with more academic experience ( Honicke and Broadbent, 2016 ). As for the type of course, scientific disciplines have been related to lower levels of self-efficacy ( Findley-Van Nostrand and Pollenz, 2017 ).

Materials and Methods
Participants.
The study used a sample of 1,085 undergraduate students from the University of A Coruña (Spain). The inclusion criteria were for subjects to be undergraduate students at the time of the study. Exclusion criteria included failing to respond to more than 20% of the items. We excluded 13 cases because they failed to respond to enough items. There were a smaller number of missing values in 28 other cases, which were dealt with using full information maximum likelihood (FIML) via Mplus 7.11 ( Muthén and Muthén, 1998–2012 ). This means that the definitive sample was made up of 1,072 students aged between 18 and 48 years ( M = 21.09; SD = 3.16). Just over two thirds ( n = 729; 68%) were women, and 343 (32%) were men. The distribution by degree course was as follows: 383 (37.5%) were studying educational sciences (infant education, primary education, social education, physical education, language and hearing, speech therapy, and educational psychology); 203 (19%) were studying health sciences (physiotherapy, nursing, and sports science); 207 (19.3%) were studying legal and social sciences (law and sociology); and 279 (26%) were studying technical sciences (architecture, technical architecture, and civil engineering). The distribution of students in terms of their university year was 304 (28.4%) in their first year, 307 (28.6%) in their second year, 302 (28.2%) in their third year, 91 (8.5%) in their fourth year, and 68 (6.3%) in their fifth year.
Instruments
We used the coping scale from the Academic Stress Questionnaire to measure coping strategies ( Cabanach et al., 2010 ). This instrument has 23 items evaluating three approach strategies for coping: positive reappraisal, support seeking, and planning. Positive reappraisal is a secondary control strategy in which the student seeks to reassign the stressful event, highlighting the positive (e.g., “When I am faced with a problematic situation, I forget unpleasant aspects and highlight the positive ones”). The psychometric properties were acceptable, in terms of both reliability (α = 0.860; ω = 0.864; construct reliability = 0.857; composite reliability = 0.857) and validity (convergent validity = 0.483; construct validity: χ 2 = 119.87; df = 30; p > 0.05; GFI = 0.98; AGFI = 0.96; TLI = 0.96; CFI = 0.98; RMR = 0.03; RMSEA = 0.05). Support seeking is a mixed coping strategy, as the student can do that with the aim of seeking information and advice from others to resolve the issue at hand (e.g., “When I am faced with a problematic situation, I ask for advice from a family member or a close friend”) or they can seek consolation and emotional relief (e.g., “When I am faced with a problematic situation, I manifest my feelings and opinions to others”). The psychometric properties of this subscale were good, in reliability (α = 0.902; ω = 0.903; construct reliability = 0.900; composite reliability = 0.900) and validity (convergent validity = 0.566; construct validity: χ 2 = 35.43; df = 12; p > 0.05; GFI = 0.99; AGFI = 0.98; TLI = 0.99; CFI = 0.99; RMR = 0.02; RMSEA = 0.04). Planning is a primary control strategy, characterized by analysis and the design of a plan of action aimed at resolving the problematic situation (“When I am faced with a problematic situation, I draw up an action plan and follow it”). The psychometric properties were acceptable, in terms of both reliability (α = 0.81; ω = 0.81; construct reliability = 0.85; composite reliability = 0.82) and validity (convergent validity = 0.504; construct validity: χ 2 = 33.52; df = 8; p > 0.05; GFI = 0.99; AGFI = 0.97; TLI = 0.97; CFI = 0.98; RMR = 0.03; RMSEA = 0.05). The participants’ responses are recorded on a five-point Likert scale (1 = never to 5 = always).
We used the Spanish validation of the General Self-efficacy Scale from Baessler and Schwarzer (1996) . The scale has 10 items (e.g., “I can solve difficult problems if I try hard enough”) that the participants respond to on a Likert scale from 1 (never) to 5 (always). In this study, the psychometric properties were good, in reliability (α = 0.91; ω = 0.91; construct reliability = 0.909; composite reliability = 0.909) and validity (convergent validity = 0.514; construct validity: χ 2 = 121.36; df = 30; p > 0.05; GFI = 0.98; AGFI = 0.96; TLI = 0.98; CFI = 0.98; RMR = 0.02; RMSEA = 0.05).
The study protocol was designed and executed in compliance with the code of ethics set out by the university in which the research was done, with the informed consent of all participants, as required by the Helsinki Declaration. Data collection was carried out at the beginning of the academic year in order to avoid periods of high academic demands (e.g., work overload and preparation for exams) that could favor greater emotional activation in students and, therefore, influence their responses to the questionnaires. Before beginning the study, the participants were informed of the objectives and were asked to participate; they were assured of anonymity and the confidentiality of their responses. Likewise, the instructor explained that students who did not wish to participate in the study could leave the classroom until the end of the tests, without any repercussions or negative consequences. The questionnaires were administered in the classrooms where the students had their usual classes, during normal class hours, and in a single session without a time limit.
Data Analysis
To identify the student profiles according to the flexibility of their coping, we performed a latent profile analysis (LPA) ( Lanza et al., 2003 ) using the statistical program Mplus 7.11 ( Muthén and Muthén, 1998–2012 ). LPA allows the identification of latent categorical variables to group the subjects into classes (profiles), establishing what fits best from a finite set of models. The following were used as reference parameters to determine the optimum model: the Akaike Information Criterion (AIC), the Schwarz Bayesian information criterion (BIC), the BIC adjusted for sample size (SSA-BIC), the formal adjusted maximum likelihood ratio test from Lo et al. (2001) (LMRT), the parametric bootstrap likelihood ratio test (PBLRT), and the sample size for each subgroup. The AIC, BIC, and SSA-BIC indices are descriptive, the lowest values indicating the best fit of the model, whereas LMRT and PBLRT are the indices that allow the final decision to be made. The values of p associated with LMRT and PBLRT indicate whether the solution with more ( p < 0.05) or fewer classes ( p > 0.05) is the one with the best fit to the data. Another of the exclusion criteria was the existence of spurious classes ( n ≤ 5% of the sample), which would indicate excessive extraction of profiles ( Hipp and Bauer, 2006 ).
Once the optimal model was selected based on the above criteria, we moved on to determining its classifying accuracy using the entropy statistic and calculation of a posteriori probabilities as references. Another criterion for evaluating the validity of the model was a MANOVA analyzing the differences between classes in the three criterion variables (positive reappraisal, support seeking, and planning). Statistically significant differences between the three variables would indicate that the latent classes suggested by the model were distinct. Finally, the differences in self-efficacy between the different coping profiles were established using an ANCOVA, with gender, year, and degree type as covariables. The effect size of the differences between the groups was determined using partial eta squared and Cohen’s (1988) d : null, η p 2 < 0.01 ( d < 0.09); small, η p 2 = 0.01 to η p 2 = 0.058 ( d = 0.10 to d = 0.49); medium, η p 2 = 0.059 to η p 2 = 0.137 ( d = 0.50 to d = 0.79); and large, η p 2 ≥ 0.138 ( d ≥ 0.80). These analyses were performed using SPSS 26.0 ( IBM Corp, 2019 ).
Preliminary Analysis
Descriptive statistics and the values of (Pearson) correlations between the variables are given in Table 1 . The asymmetry and kurtosis data indicate that the variables followed a normal distribution (all values between −1 and 1). Similarly, all of the correlations were statistically significant ( p < 0.001). Statistically speaking, the results of the Bartlett sphericity test indicate that the variables were sufficiently intercorrelated [χ 2 (6) = 1,066.75; p < 0.001)], an important requirement for subsequent multivariate analysis.
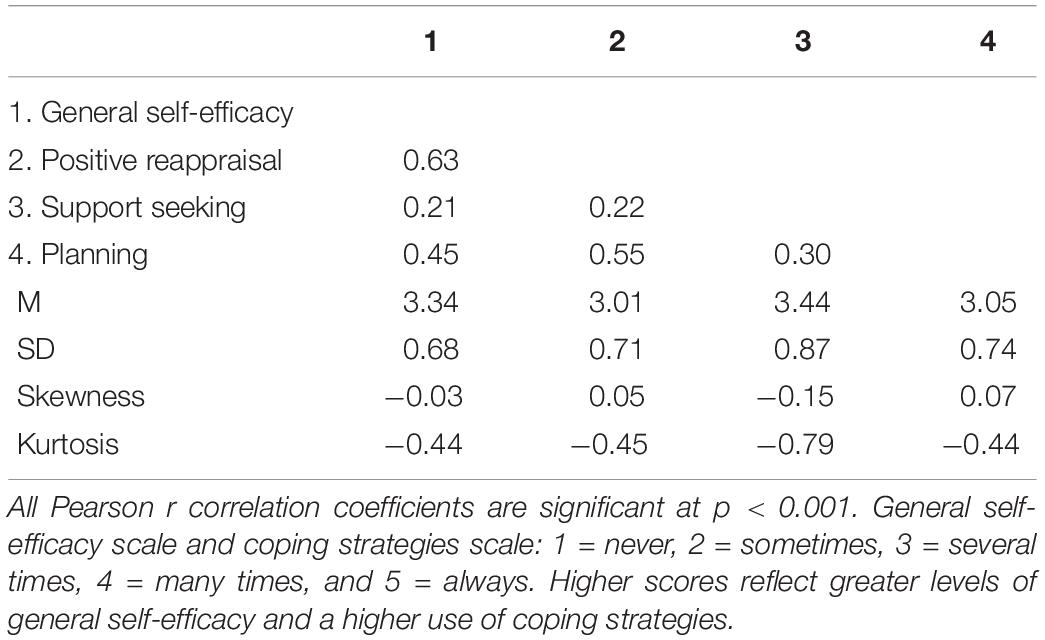
Table 1. Means, standard deviations, and correlations for the three strategies for coping with stress and general self-efficacy ( N = 1072).
Identification of Coping Profiles
The fit of various latent profile models was examined (models from two to five classes). In the model fit, it was assumed that variances could differ between indicators within each group, with the restriction specifying that they be equal between the groups. Similarly, a restriction was set on the independence between indicators, both within and between groups.
Table 2 gives the results of the model fit. The analysis of fit was stopped at the five-class model for various reasons: (a) the values of BIC and SSA-BIC were higher in the five-class model than in the four-class model, and the AIC was almost the same in the two models; (b) the values of LMRT and PBLRT for the five-class model were not statistically significant ( p > 0.05, in both cases), which indicated that the fit of this model was not better than that of the four-class model; (c) the five-class model included a group made up of fewer than 5% of the total sample, which indicated excessive extraction of profiles. In contrast, in the four-class model, all of the groups made up more than 5% of the total sample. Similarly, all of the data summarized in Table 2 indicated that the four-class model demonstrated better fit than the two- and three-class models, leading to the selection of the four-class model as the optimum.
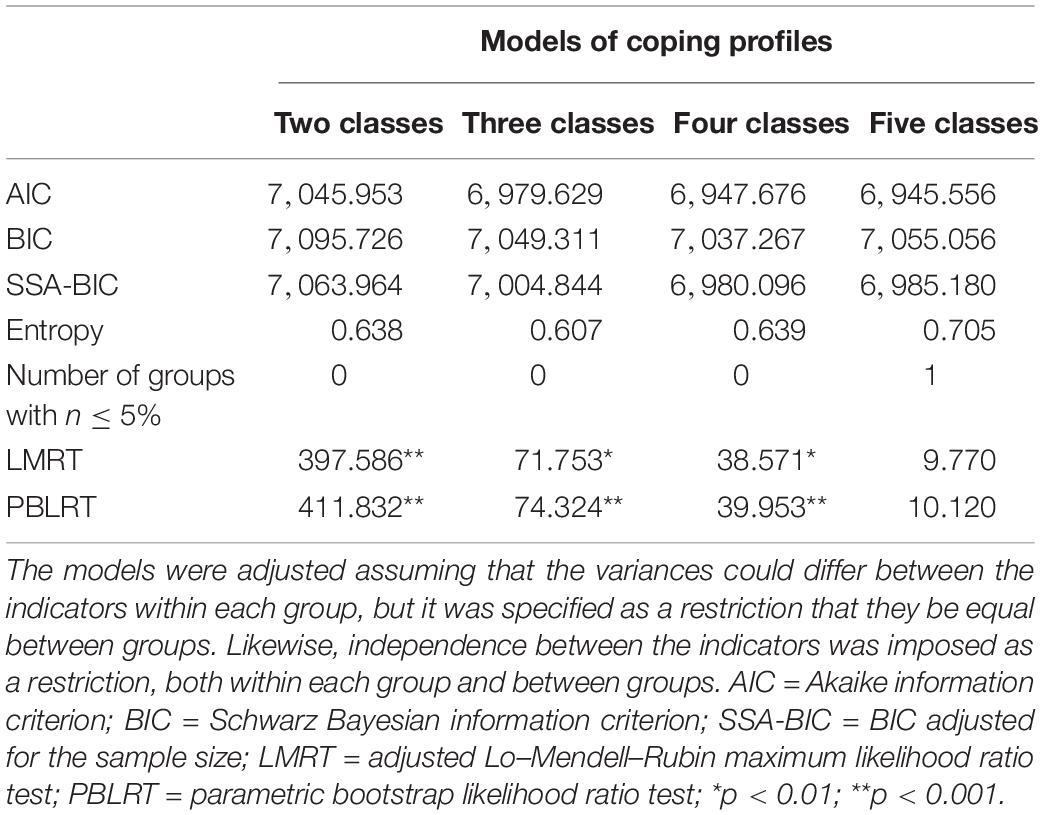
Table 2. Statistics for the identification of fit of latent class models and classifying accuracy.
Table 3 gives the classifying accuracy of the four-class model, as well as the number of participants (overall sample and by gender) making up each class in that model, both in absolute terms ( n ) and as a percentage (%). The means associated with the groups the participants were assigned to are given in the main diagonal in the table in bold. The first group demonstrated a classification coefficient of 85%, whereas the other three groups had coefficients a little below 80%. Overall, these data indicate that the four-class model demonstrates adequate classification accuracy. Similarly, the value of the entropy statistic of this model (0.639) ( Table 2 ), although modest, is acceptable ( Nylund et al., 2007 ).
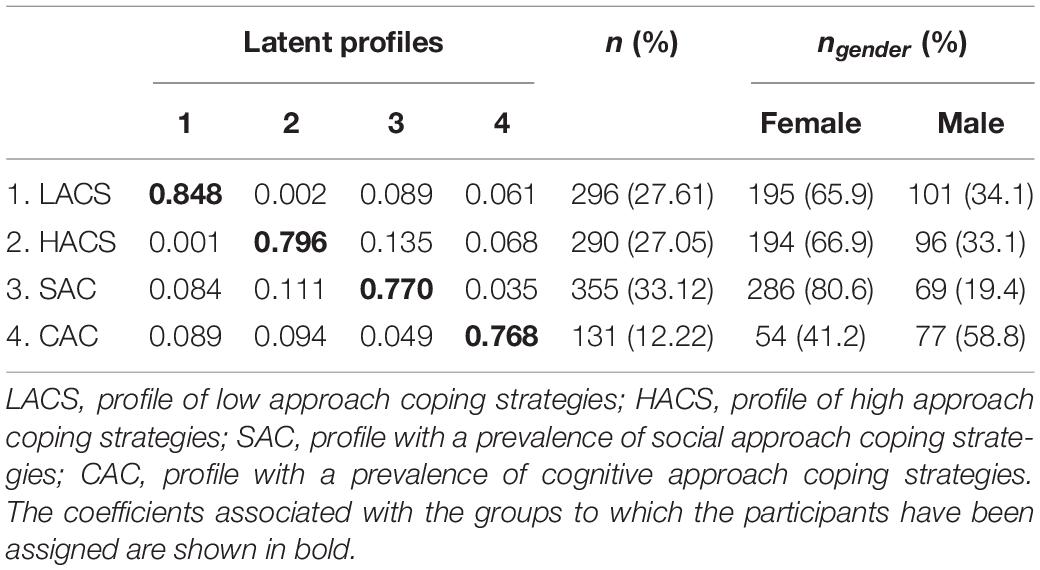
Table 3. Characterization of the latent profiles and classifying accuracy of the individuals in each profile.
As an additional criterion for assessing the suitability of the four-class model, the results of the MANOVA showed statistically significant differences between the four classes in the three criterion variables: positive reappraisal [ F (3, 1068) = 391.49; p < 0.001; η p 2 = 0.524], support seeking [ F (3, 1068) = 770.37; p < 0.001; η p 2 = 0.684], and planning [ F (3, 1068) = 463.61; p < 0.001; η p 2 = 0.566]. The effect size was large in all cases.
Description of Coping Profiles
The mean scores (direct and standardized) of the members of each of the latent classes (coping profiles) in the selected model are given in Table 4 . The same profiles are shown graphically in Figure 1 .
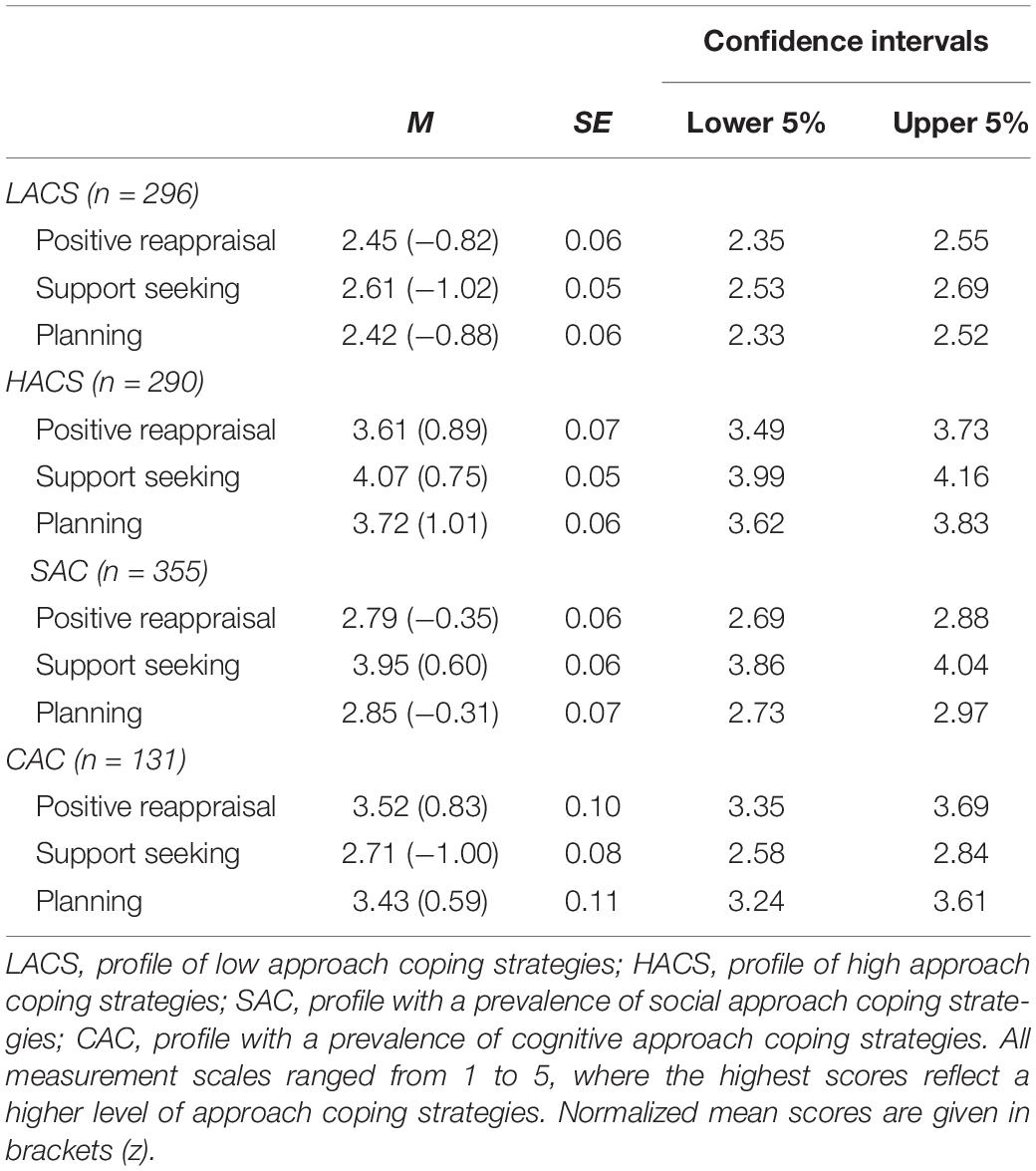
Table 4. Description of latent profiles (means, standard errors, and confidence intervals).
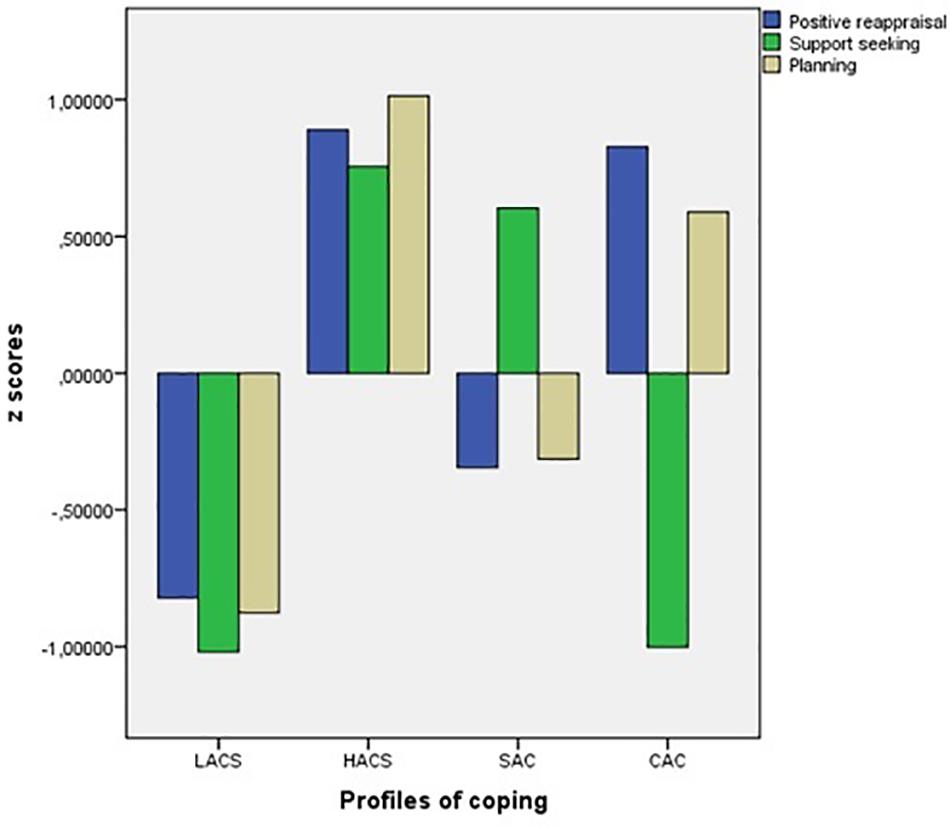
Figure 1. Graphical representation of coping profiles (standardized scores). LACS: profile of low approach coping strategies; HACS: profile of high approach coping strategies; SAC: profile with a prevalence of social approach coping strategies; CAC: profile with a prevalence of cognitive approach coping strategies.
The first group ( n = 296; 27.61%) was made up of students with low scores in the three approach coping strategies (profile of low approach coping strategies, LACS), who demonstrated low flexibility in the use of these strategies. The second group ( n = 290; 27.05%) demonstrated the opposite, scoring highly in the three coping strategies (profile of high approach coping strategies, HACS). Compared to the other profiles, these were the students who demonstrated the most flexibility in deploying approach coping strategies. The third group was the largest ( n = 355; 33.12%) and was made up of students with high scores in support seeking and low scores in positive reappraisal and planning. Given the overwhelmingly social nature of support seeking, we called this the social approach coping (SAC) profile. Finally, the smallest group in quantitative terms ( n = 131; 12.22%) was made up of students demonstrating the opposite pattern to SAC, high scores in positive reappraisal and planning and low scores in support seeking. We called this the cognitive approach coping (CAC) profile as these students seemed to prefer more cognitive approach strategies, rather than social strategies.
Relationship Between Coping Profiles and Self-Efficacy
Once the effects of gender, year, and degree course had been controlled for, the results of the ANCOVA demonstrated statistically significant differences between the coping profiles in the variable self-efficacy [ F (3, 1065) = 140.638, p < 0.001, η p 2 = 0.284), with a large effect size. The a posteriori tests (Scheffé) showed that the HACS profile scored highest in self efficacy, with statistically significant differences between it and the SAC and LACS profiles, the effect size being large in both cases ( d = 0.98 and d = 1.55, respectively). The CAC profile also had significantly higher scores in self-efficacy than the SAC and LACS profiles, with large effect sizes ( d = 0.88 and d = 1.46, respectively). The self-efficacy scores from the SAC profile were significantly higher than those from the LACS profile, with a medium effect size ( d = 0.58). These data indicate that the LACS profile scored significantly lower in self-efficacy than the other coping profiles identified in this study. Table 5 gives the descriptive statistics for the four coping profiles with respect to the self-efficacy variable. When we looked at the covariables, there was no statistically significant effect found with the year variable, but there was with the degree type [ F (1065) = 5.163, p < 0.05, η p 2 = 0.005] and gender [ F (1065) = 50.405, p < 0.001, η p 2 = 0.045], although the effect size was null for the degree type and small for gender. Having noted the small effect of gender on self-efficacy, we looked more deeply at this interaction in each of the coping profiles. In the LACS [ t (294) = 6.56, p < 0.001, d = 0.45], HACS [ t (288) = 4.17, p < 0.001, d = 0.27], and SAC profiles [ t (353) = 3.43, p < 0.01, d = 0.26], men scored significantly higher in self-efficacy than women, whereas the effect of gender on self-efficacy was not significant in the CAC profile.
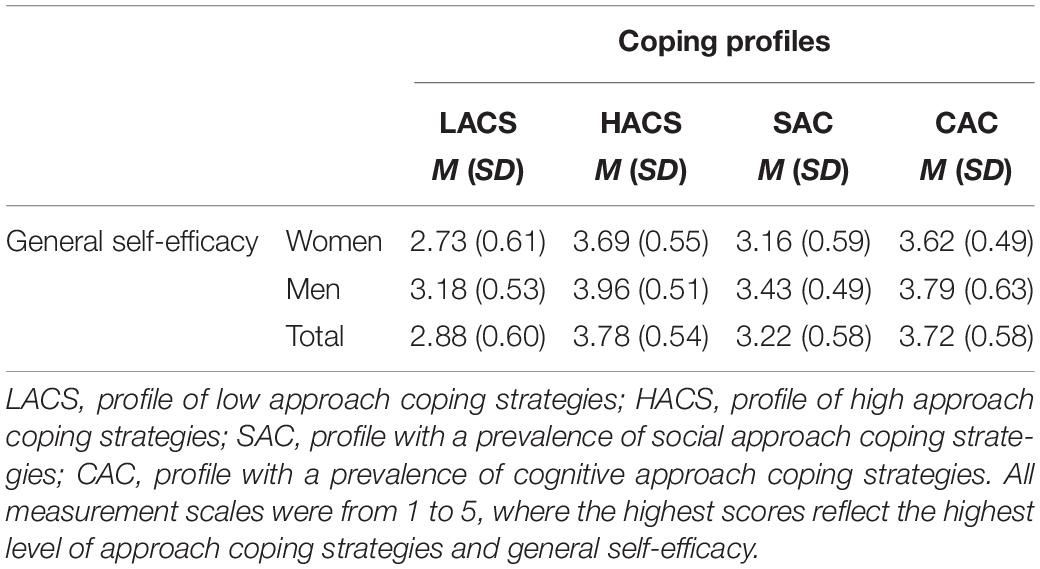
Table 5. Descriptive statistics (means and standard deviations) corresponding to coping profiles in general self-efficacy.
Although previous research has demonstrated the importance of coping strategies and self-efficacy in the prevention of stress, the relationship between these two psychological resources has not been the focus of attention previously in the university context. The main contribution of this study is in the analysis of the relationship between coping strategies and general self-efficacy in university students in light of coping flexibility.
From this person-centered focus, it is assumed that coping strategies are not mutually exclusive categories but instead operate together ( Eisenbarth, 2012 ; Kobylińska and Kusev, 2019 ), such that their functionality depends on the individuals having a repertoire of strategies available that would allow them to respond specifically to the challenge they have to deal with ( Cheng et al., 2014 ; Siltanen et al., 2019 ). The results of our study are consistent with this approach, we have identified four profiles of university students which differ in the extent of their flexibility in approach coping with stress. One of the profiles we identified (HACS) has a coping repertoire which combines high levels of positive reappraisal, support seeking, and planning. This is a group of highly flexible students when it comes to coping with problems, bringing together strategies for primary control of stressors (planning and instrumental support seeking) with others aimed at secondary control (positive reappraisal and emotional support seeking). In general, research suggests that when facing problems, the most effective method is to use primary control strategies when the situation is deemed controllable, whereas relying on secondary control strategies is more beneficial when the challenge is perceived as uncontrollable ( Zimmer-Gembeck and Skinner, 2016 ). From this perspective, the HACS profile would be highly adaptive, as the students in this group would have both types of strategy available. Our findings also demonstrated the existence of two profiles of students who displayed lower levels of coping flexibility than the HACS profiles, as their repertoires included high levels of some but not all of the three approach coping strategies we examined. One group was characterized by the combination of high levels of positive reappraisal and planning, with low levels of support seeking (the CAC profile). The other, in contrast, combined high levels of support seeking with low levels of the other two strategies (the SAC profile).
These two profiles are, to a certain extent, opposites, as students in the SAC group exhibited predominantly social coping, prioritizing their sources of support as the routes to find advice and/or emotional consolation about their problematic situations, whereas students in the CAC group preferred to opt for a more cognitive coping (i.e., focus on the positives of the situation and plan how to deal with it) rather than sharing their problems socially. According to this characterization, the students with a SAC profile would have a much smaller repertoire of approach coping strategies, which could indicate excessive instrumental and emotional dependence on their significant social circle when they have to deal with academic and non-academic stressors. Students with a CAC profile would choose to respond to stressors more autonomously, either because of a lack of interpersonal skills to ask for help or because they feel they do not have this social support or because they feel the advantages of seeking help are outweighed by the disadvantages ( Scharp and Dorrance Hall, 2019 ), such as being considered incompetent or weak. Finally, in this study, we identified the existence of a group of students characterized by a low use of positive reappraisal, support seeking, and planning (the LACS profile). Assuming that these three strategies are highly functional in academic contexts ( Skinner et al., 2016 ), the reduced availability of them in this profile would seem to indicate the students’ lack of flexibility to respond adaptively to the various demands of day-to-day university life.
The identification of these four profiles adds to the growing line of work which supports the benefits of analyzing coping with stress in the university context with a person-centered approach (e.g., Cheng, 2001 ; Kato, 2012 ; Doron et al., 2014 ; Freire et al., 2018 ; Gabrys et al., 2018 ; González Cabanach et al., 2018 ; Hasselle et al., 2019 ). To be specific, the four-profile solution in our study coincides with results from González Cabanach et al. (2018) , in a study which also examined flexibility of coping based on the combination of positive reappraisal, support seeking, and planning strategies. This may point to a potential generalization of the profiles identified when the flexibility of approach coping with stress is examined in a university context.
Beyond affirming the existence of student profiles characterized by differences in the flexibility of coping, the objective of our study was to determine whether these groups diverged in their expectations of self-efficacy. In accordance with our hypothesis, the greater the flexibility in approach coping with stress, the higher the students’ levels of general self-efficacy and vice versa. The student profiles that had most flexibility in their coping (HACS and CAC) exhibited notable differences (i.e., large effect sizes) in self-efficacy compared to less flexible profiles (SAC and LACS). Additionally, the SAC profile exhibited moderately higher self-efficacy (i.e., medium effect size) than the LACS profile.
These results could indicate, in line with other studies from the healthcare context (e.g., Haythornthwaite et al., 1998 ), that flexibility in coping enhances university students’ perception of control over their day-to-day challenges, making them feel better able to handle them. This explanation may be connected with what Hobfoll’s conservation of resources theory ( Hobfoll et al., 2018 ) postulates. According to this theory, individuals who have high levels of personal resources (e.g., a variety of approach coping strategies) participate in an upward spiral of acquisition, development, and preservation of new resources (e.g., self-efficacy). In contrast, scarce resources in the face of a given challenge (e.g., low flexibility in coping) would put the individual into a downward spiral of losing resources (e.g., low self-efficacy) which would make them more vulnerable to stress. In this way, personal resources would act in “convoy” ( Holmgreen et al., 2017 ), one after the other, whether upward or downward. In addition, the fact that we did not find significant differences between the HACS and CAC profiles with regard to general self-efficacy suggests that, in terms of developing generalized self-referential beliefs about personal competency in response to the demands of university life, the combination of cognitive strategies (positive reappraisal and planning) is more important than social strategies (support seeking). This idea is in line with the lower potency that Bandura’s (1997) social cognitive theory ascribes to social sources in making up expectations of self-efficacy. Thus, it is possible that the low availability of cognitive coping resources exhibited by students with the SAC profile would negatively affect their beliefs of competency for dealing with stressors, which would lead them to seek feedback from their sources of support that would give them some degree of self-efficacy, albeit significantly less than students with HACS and CAC profiles, but still somewhat higher than students with the LACS profile.
Implications of the Results of the Study
University stress is a growing psychosocial concern, both because of its prevalence and because of the negative consequences it can have for the student. Although this scenario highlights the need to implement effective coping interventions in the entire university population, this need is even more pronounced in students who are studying healthcare-related degrees ( Saeed et al., 2016 ), in which stress levels are significantly higher ( Heinen et al., 2017 ; Zeng et al., 2019 ). In line with that, the results of our study may represent a significant contribution, in that they help increase our understanding of how two important psychological resources, flexibility of approach coping strategies and general self-efficacy, function in the prevention of stress.
To be more specific, our findings allow the identification of those students who, depending on the level of their flexibility in the use of approach coping strategies, are more (LACS and SAC profiles) or less (HACS and CAC profiles) vulnerable with respect to developing their expectations of generalized self-efficacy.
Not only does self-efficacy play an important role in the prevention of university stress ( Freire et al., 2019 ; Schönfeld et al., 2019 ), it is also one of the most influential factors in the motivational, cognitive, and behavioral responses of the student to the teaching–learning process ( Schunk and Pajares, 2010 ). Consequently, in light of our results, students in the SAC and particularly in the LACS profiles should be the focus of priority intervention in order to enhance flexibility in their repertoire of approach coping strategies as a way of improving their generalized expectations of self-efficacy. In recent years, interventions aimed at improving the coping skills of university students have proliferated. Most of these initiatives have adopted an approach based on cognitive behavioral therapy ( Houston et al., 2017 ), mindfulness ( Kang et al., 2009 ), or a combination of the two ( Recabarren et al., 2019 ). In these programs, students learn to identify the main symptoms associated with stress, as well as the external (environmental demands) and internal (thoughts and emotions) factors that contribute to its appearance. Furthermore, students acquire various primary control (e.g., planning and problem solving) and secondary control (e.g., positive reappraisal and meditation) adaptive coping strategies.
Although these types of interventions have shown their effectiveness both in reducing stress ( Regehr et al., 2013 ; Yusufov et al., 2019 ) and in increasing self-efficacy ( Molla Jafar et al., 2015 ; Phang et al., 2015 ), they have limited influence by themselves on the students’ abilities to be flexible in their coping strategies ( Cheng and Cheung, 2005 ). Prior research offers us evidence of the efficacy of focused training to enhance both individuals’ repertoires of strategies and their metacognitive abilities to evaluate and select the best coping strategies in each situation ( Cheng et al., 2012 ).
From this, it would seem that metacognitive self-regulation and executive functioning skills (e.g., planning, organization, emotional management) constitute an important resource for improving students’ abilities to make their repertoires of strategies more flexible, in addition to specific training aimed at increasing their coping strategies ( Bettis et al., 2017 ; de la Fuente et al., 2018a ). Some online tools in this area, such as e-Coping with Academic Stress TM , have demonstrated good results in the improvement of self-regulating skills (e.g., self-evaluation and decision making) in students when facing potentially stressful situations in the university context ( de la Fuente et al., 2018b ). These results also have important implications at the classroom level, given that if teachers encourage the development of self-regulation skills in university students, they increase the tendency for students to autonomously use approach coping strategies, such as establishing a plan of action, assessing the positive aspects of the situation, or seeking advice and emotional support from other people ( de la Fuente et al., 2020 ). These self-regulatory skills have also been shown to be effective in increasing students’ self-efficacy beliefs ( Cerezo et al., 2019 ).
Limitations of the Study and Lines for Future Research
The contributions of this study should be assessed, taking into account the limitations inherent in its design. First, the transversal nature of the study does not allow causal relationships to be established between the variables studied. Therefore, although our results suggest that flexibility in coping with stress influences the generalized expectations of self-efficacy, the causal order between these variables must be examined in the light of more rigorous study designs (e.g., longitudinal studies). A second limitation lies in the composition of the sample, which was dissimilar in terms of gender representation, university year, and degree type. In this study, those three variables were considered as covariates to statistically control their effect, with degree type and gender exhibiting a null effect and a small effect, respectively. However, new studies are needed that would be able to corroborate the extent to which these variables are important, or not, in the configuration of the profiles of coping flexibility and in the relationship between these profiles and self-efficacy. In fact, based on our findings, the levels of general self-efficacy were significantly higher in men (albeit with a small effect size) in all of the coping profiles except the group which had similar levels of representation of both sexes (the CAC profile), where there were no differences. Therefore, in order to make the results more generalizable to the university student population, future studies should use more thorough recruitment procedures that would give more balanced samples in terms of gender, university year, and degree type. In the same vein, future work should consider the extent to which variables not addressed in this study, such as students’ previous academic performance, their socioeconomic status, or their intellectual abilities (e.g., cognitive and attention level), may be relevant in the relationship between stress coping profiles and general self-efficacy in the university context. The fact that all of the participants were recruited from the same university constitutes a third limitation of our study. In order to facilitate generalization of the results, new studies are needed which involve students from other geographical and cultural contexts.
Fourth, the use of self-reports as a data collection method may limit the veracity of the results, since participants may have response biases, ranging from a misunderstanding of the items to social desirability bias (i.e., the tendency of survey respondents to answer questions in a manner that will be viewed favorably by others, even if the survey is anonymous) ( Rosenman et al., 2011 ). These biases may have been increased by the effect of the data collection method used (collective and pencil-and-paper condition). In fact, this type of method can increase the perception of a lack of privacy and confidentiality when other participants are present ( van de Looij-Jansen and de Wilde, 2008 ), encouraging the social desirability response effect and a higher rate of questions not answered, especially with sensitive questions such as those related to mental health ( Raat et al., 2007 ). These and other limitations—for example, data collection costs and data entry errors ( Colasante et al., 2019 ), physical and emotional fatigue of the participants at the time data collection, and absence of a rigorous control over the time taken to complete the questionnaires ( Díaz de Rada, 2018 )—could be minimized by using computerized administration of questionnaires. Likewise, future studies should corroborate our findings using a combination of methods that include not only questionnaires but also classroom observations and in-depth interviews with the students.
There is another limitation with respect to the questionnaires used, specifically the questionnaire we used to evaluate coping strategies. Although the three strategies evaluated by this instrument (positive reappraisal, support seeking, and planning) are widely used in academic contexts, that does not preclude the possibility of students using other types of strategies. Future research should examine the possible makeup of flexible coping profiles considering other strategies that were not assessed in this study.
Finally, another limitation lies in the operationalization of the concept of coping flexibility. Our results seem to be consistent with the conceptualization of coping flexibility in terms of balanced profiles, according to which the student deploys various strategies at similar levels ( Kaluza, 2000 ). Despite this idea of coping flexibility being widely adopted in the educational field, there are other ways to operationalize this construct (e.g., a broad repertoire or cross-situational variability; for a more precise characterization, see Cheng et al., 2014 ), which might impede comparison between studies and the generalization of the results.
Data Availability Statement
The datasets generated for this study are available on request to the corresponding author.
Ethics Statement
The studies involving human participants were reviewed and approved by the Ethics Committee at the University of A Coruña. The patients/participants provided their written informed consent to participate in this study.
Author Contributions
CF and MF contributed to the conceptualization, investigation, methodology, writing, and supervision of this study. BR and SR contributed to the investigation, writing, and supervision of this study. AV and JN contributed to the methodology, writing, and supervision of this study.
This work was financed by the research projects EDU2013-44062-P (MINECO), EDU2017-82984-P (MEIC), and the Consejería de Empleo, Industria y Turismo del Principado de Asturias (Department of Employment, Industry and Tourism of the Principality of Asturias, Spain) (ref. FC-GRUPIN-IDI/2018/000199).
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
The authors would like to thank the students who participated in the study.
American College Health Association (2018). National College Health Assessment II: Reference Group Executive Summary Fall 2018. Hanover, MD: American College Health Association.
Google Scholar
Baessler, J., and Schwarzer, R. (1996). Evaluación de la autoeficacia: adaptación española de la escala de autoeficacia general [Evaluation of self-efficacy: spanish adaptation of the General Self-efficacy Scale]. Ans. Estrés 2, 1–8.
Bandura, A. (1997). Self-Efficacy: The exercise of Control. New York, NY: Freeman.
Bandura, A., Caprara, G. V., Barbaranelli, C., Gerbino, M., and Pastorelli, C. (2003). Role of affective self-regulatory efficacy in diverse spheres of psychosocial functioning. Child Dev. 74, 769–782. doi: 10.1111/1467-8624.00567
PubMed Abstract | CrossRef Full Text | Google Scholar
Beiter, R., Nash, R., McCrady, M., Rhoades, D., Linscomb, M., Clarahan, M., et al. (2015). The prevalence and correlates of depression, anxiety, and stress in a sample of college students. J. Affect. Disord. 173, 90–96. doi: 10.1016/j.jad.2014.10.054
Bettis, A. H., Coiro, M. J., England, J., Murphy, L. K., Zelkowitz, R. L., Dejardins, L., et al. (2017). Comparison of two approaches to prevention of mental health problems in college students: enhancing coping and executive function skills. J. Am. Coll. Health 65, 313–322. doi: 10.1080/07448481.2017
CrossRef Full Text | Google Scholar
Blanco, C., Okuda, M., Wright, C., Hasin, D. S., Grant, B. F., Liu, S.-M., et al. (2008). Mental health of college students and their non-college-attending peers: results from the national epidemiologic study on alcohol and related conditions. Arch. Gen. Psychiatry 65, 1429–1437. doi: 10.1001/archpsyc.65.12.1429
Bonanno, G. A., and Burton, C. L. (2013). Regulatory flexibility: an individual differences perspective on coping and emotion regulation. Perspect. Psychol. Sci. 8, 591–612. doi: 10.1177/1745691613504116
Cabanach, R. G., Valle, A., Rodríguez, S., Piñeiro, I., and Freire, C. (2010). Escala de Afrontamiento del Estrés Académico (A-CEA) [The coping scale of academic stress questionnaire (A-CEA)]. Rev. Iberoam. Psicol. Salud. 1, 51–64.
Cerezo, R., Fernández, E., Amieiro, N., Valle, A., Rosário, P., and Núñez, J. C. (2019). Mediating role of self-efficacy and usefulness between self-regulated learning strategy knowledge and its use. Rev. Psicodidact. 24, 1–8. doi: 10.1016/j.psicoe.2018.09.001
Cheng, C. (2001). Assessing coping flexibility in real-life and laboratory settings: a multimethod approach. J. Pers. Soc. Psychol. 80, 814–833. doi: 10.1037//0022-3514.80.5.814
Cheng, C., and Cheung, M. W. L. (2005). Cognitive processes underlying coping flexibility: differentiation and integration. J. Pers. 73, 859–886. doi: 10.1111/j.1467-6494.2005.00331.x
Cheng, C., Kogan, A., and Chio, J. H. (2012). The effectiveness of a new, coping flexibility intervention as compared with a cognitive-behavioural intervention in managing work stress. Work Stress 26, 272–288. doi: 10.1080/02678373.2012.710369
Cheng, C., Lau, H.-P. B., and Chan, M. P. S. (2014). Coping flexibility and psychological adjustment to stressful life changes: a meta-analytic review. Psychol. Bull. 140, 1582–1607. doi: 10.1037/a0037913
Chou, P.-C., Chao, Y.-M. Y., Yang, H.-J., Yeh, G.-L., and Lee, T. S.-H. (2011). Relationships between stress, coping and depressive symptoms among overseas university preparatory Chinese students: a cross-sectional study. BMC Public Health 11:352. doi: 10.1186/1471-2458-11-352
Clarke, A. T. (2006). Coping with interpersonal stress and psychosocial health among children and adolescents: a meta-analysis. J. Youth Adolesc. 35, 10–23. doi: 10.1007/s10964-005-9001-x
Cohen, J. (1988). Statistical Power Analysis for the Behavioral Sciences. Hillsdale, MI: Erlbaum.
Colasante, E., Benedetti, E., Fortunato, L., Scalese, M., Potente, R., Cutilli, A., et al. (2019). Paper-and-pencil versus computerized administration mode: comparison of data quality and risk behavior prevalence estimates in the European school survey project on alcohol and other drugs (ESPAD). PLoS One 14:e0225140. doi: 10.1371/journal.pone.0225140
de la Fuente, J., Amate, J., González-Torres, M. C., Artuch, R., García-Torrecillas, J. M., and Fadda, S. (2020). Effects of levels of self-regulation and regulatory teaching on strategies for coping with academic stress in undergraduate students. Front. Psychol. 11:22. doi: 10.3389/fpsyg.2020.00022
de la Fuente, J., Mañas, I., Franco, C., Cangas, A. J., and Soriano, E. (2018a). Differential effect of level of self-regulation and mindfulness training on coping strategies used by university students. Int. J. Environ. Res. Public Health 15:E2230. doi: 10.3390/ijerph15102230
de la Fuente, J., Martínez-Vicente, J. M., Peralta-Sánchez, F. J., González-Torres, M. C., Artuch, R., and Garzón-Umerenkova, A. (2018b). Satisfaction with the self-assessment of university students through e-Coping with academic stress UtilityTM. Front. Psychol. 9:1932. doi: 10.3389/fpsyg.2018.01932
Deasy, C., Coughlan, B., Pironom, J., Jourdan, D., and Mannix-McNamara, P. (2014). Psychological distress and coping amongst higher education students: a mixed method enquiry. PLoS One 9:e115193. doi: 10.1371/journal.pone.0115193
DeRosier, M. E., Frank, E., Schwartz, V., and Leary, K. A. (2013). The potential role of resilience education for preventing mental health problems for college students. Psychiatr. Ann. 43, 538–544. doi: 10.3928/00485713-20131206-05
Díaz de Rada, V. (2018). Face-to-face surveys using paper or a computer: difference in attitudes. Papers 103, 199–227. doi: 10.5565/rev/papers.2301
Doron, J., Trouillet, R., Maneveau, A., Neveu, D., and Ninot, G. (2014). Coping profiles, perceived stress and health-related behaviors: a cluster analysis approach. Health Promot. Int. 30, 88–100. doi: 10.1093/heapro/dau090
Eisenbarth, C. (2012). Coping profiles and psychological distress: a cluster analysis. N. Am. J. Psychol. 14, 485–496.
Erschens, R., Herrmann-Werner, A., Keifenheim, K. E., Loda, T., Bugaj, T. J., Nikendei, C., et al. (2018). Differential determination of perceived stress in medical students and high-school graduates due to private and training-related stressors. PLoS One 13:e0191831. doi: 10.1371/journal.pone.0191831
Feldman, D. B., and Kubota, M. (2015). Hope, self-efficacy, optimism, and academic achievement: distinguishing constructs and levels of specificity in predicting college grade-point average. Learn Indiv. Differ. 37, 210–216. doi: 10.1016/j.lindif.2014.11.022
Findley-Van Nostrand, D., and Pollenz, R. S. (2017). Evaluating psychosocial mechanisms underlying STEM persistence in undergraduates: evidence of impact from a six-day pre–college engagement STEM Academy Program. CBE Life Sci. Educ. 16, 1–15. doi: 10.1187/cbe.16-10-0294
Freire, C., Ferradás, M. M., Núñez, J. C., and Valle, A. (2018). Coping flexibility and eudaimonic well-being in university students. Scand. J. Psychol. 59, 433–442. doi: 10.1111/sjop.12458
Freire, C., Ferradás, M. M., Núñez, J. C., Valle, A., and Vallejo, G. (2019). Eudaimonic well-being and coping with stress in university students: the mediating/moderating role of self-efficacy. Int. J. Environ. Res. Public Health 16:48. doi: 10.3390/ijerph16010048
Gabrys, R. L., Tabri, H., Anisman, N., and Matheson, K. (2018). Cognitive control and flexibility in the context of stress and depressive symptoms: the cognitive control and flexibility questionnaire. Front. Psychol. 9:2219. doi: 10.3389/fpsyg.2018.02219
Galatzer-Levy, I. R., Burton, C. L., and Bonanno, G. A. (2012). Coping flexibility, potentially traumatic life events, and resilience: a prospective study of college student adjustment. J. Soc. Clin. Psychol. 31, 542–567. doi: 10.1521/jscp.2012.31.6.542
González Cabanach, R., Souto-Gestal, A., González-Doniz, L., and Franco, V. (2018). Perfiles de afrontamiento y estrés académico en estudiantes universitarios [Profiles of coping and academic stress among university students]. Rev. Invest. Educ. 36, 421–433. doi: 10.6018/rie.36.2.290901
Gustems-Carnicer, J., Calderón, C., and Calderón-Garrido, D. (2019). Stress, coping strategies and academic achievement in teacher education students. Eur. J. Teach. Educ. 42, 375–390. doi: 10.1080/02619768.2019.1576629
Hasselle, A. J., Schwartz, L. E., Berlin, K. S., and Howell, K. H. (2019). A latent profile analysis of coping responses to individuals’ most traumatic event: associations with adaptive and maladaptive mental health outcomes. Anxiety Stress Copin 32, 626–640. doi: 10.1080/10615806.2019.1638733
Haythornthwaite, J. A., Menefee, L. A., Heinberg, L. J., and Clark, M. R. (1998). Pain coping strategies predict perceived control over pain. Pain 77, 33–39. doi: 10.1016/s0304-3959(98)00078-5
Heinen, I., Bullinger, M., and Kocalevent, R. D. (2017). Perceived stress in first year medical students - associations with personal resources and emotional distress. BMC Med. Educ. 17:4. doi: 10.1186/s12909-016-0841-8
Hipp, J. R., and Bauer, D. J. (2006). Local solutions in the estimation of growth mixture models. Psychol. Methods 11, 36–53. doi: 10.1037/1082-989X.11.1.36
Hobfoll, S. E., Halbesleben, J., Neveu, J. P., and Westman, M. (2018). Conservation of resources in the organizational context: the reality of resources and their consequences. Ann. Rev. Organ. Psychol. Organ. Behav. 5, 103–128. doi: 10.1146/annurev-orgpsych-032117-104640
Holmgreen, L., Tirone, V., Gerhart, J., and Hobfoll, S. E. (2017). “Conservation of resources theory. Resource caravans and passageways in health contexts,” in The Handbook of Stress and Health: A Guide to Research and Practice , eds C. L. Cooper and J. C. Quick (Oxford: Wiley), 443–458.
Honicke, T., and Broadbent, J. (2016). The relation of academic self-efficacy to university student academic performance: a systematic review. Educ. Res. Rev. 17, 63–84. doi: 10.1016/j.edurev.2015.11.002
Houston, J. B., First, J., Spialek, M. L., Sorenson, M. E., Mills-Sandoval, T., Lockett, M., et al. (2017). Randomized controlled trial of the resilience and coping intervention (RCI) with undergraduate university students. J. Am. Coll. Health 65, 1–9. doi: 10.1080/07448481.2016.1227826
Howard, D. E., Schiraldi, G., Pineda, A., and Campanella, R. (2006). “Stress and mental health among college students: overview and promising prevention interventions,” in Stress and Mental Health of College Students , ed. M. V. Landow (New York, NY: Nova Science Publishers), 91–124.
Huang, C. (2013). Gender differences in academic self-efficacy: a meta-analysis. Eur. J. Psychol. Educ. 28, 1–35. doi: 10.1007/s10212-011-0097-y
IBM Corp. (2019). SPSS STATISTICS for Windows, Version 26.0. Armonk, NY: IBM Corp.
Kaluza, G. (2000). Changing unbalanced coping profiles-A prospective controlled intervention trial in worksite health promotion. Psychol. Health 15, 423–433. doi: 10.1080/08870440008402003
Kang, Y. S., Choi, S. Y., and Ryu, E. (2009). The effectiveness of a stress coping program based on mindfulness meditation on the stress, anxiety, and depression experienced by nursing students in Korea. Nurse Educ. Today 29, 538–543. doi: 10.1016/j.nedt.2008.12.003
Kato, T. (2012). Development of the coping flexibility scale: evidence for the coping flexibility hypothesis. J. Couns. Psychol. 59, 262–273. doi: 10.1037/a0027770
Keefe, F. J., Kashikar-Zuck, S., Robinson, E., Salley, A., Beaupre, P., Caldwell, D., et al. (1997). Pain coping strategies that predict patient’s and spouses’ rating of patients’ self-efficacy. Pain 73, 191–199. doi: 10.1016/S0304-3959(97)00109-7
Kim, J. E., Saw, A., and Zane, N. (2015). The influence of psychological symptoms on mental health literacy of college students. Am. J. Orthopsychiatry 85, 620–630. doi: 10.1037/ort0000074
Kobylińska, D., and Kusev, P. (2019). Flexible emotion regulation: how situational demands and individual differences influence the effectiveness of regulatory strategies. Front. Psychol. 10:72. doi: 10.3389/fpsyg.2019.00072
Lanin, D. G., Guyll, M., Cornish, M. A., Vogel, D. L., and Madon, S. (2019). The importance of counseling self-efficacy: physiologic stress in student helpers. J. College Stud. Psychother. 33, 14–24. doi: 10.1080/87568225.2018.1424598
Lanza, S. T., Flaherty, B. P., and Collins, L. M. (2003). “Latent class and latent transition analysis,” in Handbook of Psychology: Research Methods in Psychology , eds J. A. Schinka and W. F. Velicer (Hobobken, NJ: Wiley), 663–685.
Laursen, B., and Hoff, E. (2006). Person-centered and variable-centered approaches to longitudinal data. Merrill-Palmer Q. 52, 377–389. doi: 10.1353/mpq.2006.0029
Lazarus, R. S., and Folkman, S. (1984). Stress, Appraisal, and Coping. New York, NY: Springer.
Leiva-Bianchi, M., Baher, G., and Poblete, C. (2012). The effects of stress coping strategies in post-traumatic stress symptoms among earthquake survivors. An explanatory model of post-traumatic stress. Terapia Psicol. 30, 51–59. doi: 10.4067/s0718-48082012000200005
Lo, Y., Mendell, N. R., and Rubin, D. B. (2001). Testing the number of components in a normal mixture. Biometrika 88, 767–778. doi: 10.1093/biomet/88.3.767
Milojevich, H. M., and Lukowski, A. F. (2016). Sleep and mental health in undergraduate students with generally healthy sleep habits. PLoS One 11:e0156372. doi: 10.1371/journal.pone.0156372
Molla Jafar, H., Salabifard, S., Mousavi, S. M., and Sobhani, Z. (2015). The effectiveness of group training of CBT-based stress management on anxiety, psychological hardiness and general self-efficacy among university students. Glob. J. Health Sci. 8, 47–54. doi: 10.5539/gjhs.v8n6p47
Muth, L. K., and Muthén, B. O. (1998–2012). Mplus User’s Guide , 6th Edn. Los Angeles, CA: Muthén & Muthén.
Nylund, K. L., Asparouhov, T., and Muthén, B. (2007). Deciding on the number of classes in latent class analysis and growth mixture modeling: a monte carlo simulation study. Struct. Equ. Modeling 14, 535–569. doi: 10.1080/10705510701575396
Phang, C. K., Mukhtar, F., Ibrahim, N., Keng, S. L., and Mohd Sidik, S. (2015). Effects of a brief mindfulness-based intervention program for stress management among medical students: the Mindful-Gym randomized controlled study. Adv. Health Sci. Educ. Theory Pract. 20, 1115–1134. doi: 10.1007/s10459-015-9591-3
Raat, H., Mangunkusumo, R. T., Landgraf, J. M., Kloek, G., and Brug, J. (2007). Feasibility, reliability, and validity of adolescent health status measurement by the child health questionnaire child form (CHQ-CF): internet administration compared with the standard paper version. Qual. Life Res. 16, 675–685. doi: 10.1007/s11136-006-9157-1
Recabarren, R. E., Gaillard, C., Guillod, M., and Martin-Soelch, C. (2019). Short-term effects of a multidimensional stress prevention program on quality of life, well-being and psychological resources. A randomized controlled trial. Front. Psychiatry 10:88. doi: 10.3389/fpsyt.2019.00088
Regehr, C., Glancy, D., and Pitts, A. (2013). Interventions to reduce stress in university students: a review and meta-analysis. J. Affect. Disord. 148, 1–11. doi: 10.1016/j.jad.2012.11.026
Ritchie, L. (2016). Fostering self-Efficacy in Higher Education Students. London: Palgrave MacMillan.
Rosenman, R., Tennekoon, V., and Hill, L. G. (2011). Measuring bias in self-reported data. Int. J. Behav. Healthc. Res. 2, 320–332. doi: 10.1504/IJBHR.2011.043414
Saeed, A. A., Bahnassy, A. A., Al-Hamdan, N. A., Almudhaibery, F. S., and Alyahya, A. Z. (2016). Perceived stress and associated factors among medical students. J. Family Community Med. 23, 166–171. doi: 10.4103/2230-8229.189132
Sahin, F., and Çetin, F. (2017). The mediating role of general self-efficacy in the relationship between the big five personality traits and perceived stress: A weekly assessment study. Psychol. Stud. 62, 35–46. doi: 10.1007/s12646-016-0382-6
Sandler, I. N., Tein, J.-Y., Mehta, P., Wolchik, S., and Ayers, T. (2000). Coping efficacy and psychological problems of children of divorce. Child Dev. 71, 1099–1118. doi: 10.1111/1467-8624.00212
Scharp, K. M., and Dorrance Hall, E. (2019). Examining the relationship between undergraduate student parent social support-seeking factors, stress, and somatic symptoms: a two-model comparison of direct and indirect effects. Health Commun. 34, 54–64. doi: 10.1080/10410236.2017.1384427
Scholz, U., Doña, B. G., Sud, S., and Schwarzer, R. (2002). Is general self-efficacy a universal construct? Psychometric findings from 25 countries. Eur. J. Psychol. Assess. 18, 242–251. doi: 10.1027//1015-5759.18.3.242
Schönfeld, P., Brailovskaia, J., Bieda, A., Zhang, X. C., and Margraf, A. (2016). The effects of daily stress on positive and negative mental health: mediation through self-efficacy. Int. J. Clin. Health Psychol. 16, 1–10. doi: 10.1016/j.ijchp.2015.08.005
Schönfeld, P., Brailovskaia, J., Zhang, X. C., and Margraf, A. (2019). Self-efficacy as a mechanism linking daily stress to mental health in students: a three-wave cross-lagged study. Psychol. Rep. 122, 2074–2095. doi: 10.1177/0033294118787496
Schunk, D., and Pajares, F. (2010). “Self-efficacy beliefs,” in International Encyclopedia of Education , 3rd Edn, eds P. Peterson, E. Baker, and B. McGaw (New York, NY: Elsevier), 668–672.
Siltanen, S., Rantanen, T., Portegijs, E., Tourunen, A., Poranen-Clark, T., Eronen, J., et al. (2019). Association of tenacious goal pursuit and flexible goal adjustment with out-of-home mobility among community-dwelling older people. Aging Clin. Exp. Res. 31, 1249–1256. doi: 10.1007/s40520-018-1074-y
Skinner, E. A., Edge, K., Altman, J., and Sherwood, H. (2003). Searching for the structure of coping: A review and critique of category systems for classifying ways of coping. Psychol. Bull. 129, 216–269. doi: 10.1037/0033-2909.129.2.216
Skinner, E. A., Pitzer, J. R., and Steele, J. S. (2016). Can student engagement serve as a motivational resource for academic coping, persistence, and learning during late elementary and early middle school? Dev. Psychol. 52, 2099–2117. doi: 10.1037/dev0000232
Syed, M., and Seiffge-Krenke, I. (2015). Change in ego development, coping, and symptomatology from adolescence to emerging adulthood. J. Appl. Dev. Psychol. 41, 110–119. doi: 10.1016/j.appdev.2015.09.003
Tavolacci, M. P., Ladner, J., Grigioni, S., Richard, L., Villet, H., and Dechelotte, P. (2013). Prevalence and association of perceived stress, substance use and behavioral addictions: a cross-sectional study among university students in France, 2009-2011. BMC Public Health 13:724. doi: 10.1186/1471-2458-13-724
Tran, A. W. Y., and Lumley, M. N. (2019). Internalized stigma and student well-being: the role of adaptive and maladaptive coping. Soc. Work Ment. Health 17, 408–425. doi: 10.1080/15332985.2018.1563023
Turner, J., Bartlett, D., Andiappan, M., and Cabot, L. (2015). Students’ perceived stress and perception of barriers to effective study: impact on academic performance in examinations. Br. Dent. J. 219, 453–458. doi: 10.1038/sj.bdj.2015.850
van de Looij-Jansen, P. M., and de Wilde, E. J. (2008). Comparison of web-based versus paper-and-pencil self-administered questionnaire: effects on health indicators in Dutch adolescents. Health Serv. Res. 43, 1708–1721. doi: 10.1111/j.1475-6773.2008.00860.x
Vizoso, C. M., and Arias, O. (2016). Estresores académicos percibidos por estudiantes universitarios y su relación con el burnout y el rendimiento académicos [Academic stressors perceived by university students and their relationship with academic burnout, efficacy and performance]. Anu. Psicol. 46, 90–97. doi: 10.1016/j.anpsic.2016.07.006
Volz, M., Voelkle, M. C., and Werheid, K. (2019). General self-efficacy as a driving factor of post-stroke depression: a longitudinal study. Neuropsychol. Rehabil. 29, 1426–1438. doi: 10.1080/09602011.2017.1418392
Waqas, A., Khan, S., Sharif, W., Khalid, U., and Ali, A. (2015). Association of academic stress with sleeping difficulties in medical students of a Pakistani medical school: a cross sectional survey. PeerJ 3:e840. doi: 10.7717/peerj.840
Webber, J., Skodda, S., Muth, T., Angerer, P., and Loerbroks, A. (2019). Stressors and resources related to academic studies and improvements suggested by medical students: a qualitative study. BMC Med. Educ. 19:312. doi: 10.1186/s12909-019-1747-z
Wood, R. E., and Bandura, A. (1989). Impact of conceptions of ability on self-regulatory mechanisms and complex decision making. J. Pers. Soc. Psychol. 56, 407–415. doi: 10.1037/0022-3514.56.3.407
Yusufov, M., Nicoloro-SantaBarbara, J., Grey, N. E., Moyer, A., and Lobel, M. (2019). Meta-analytic evaluation of stress reduction interventions for undergraduate and graduate students. Int. J. Stress Manag. 26, 132–145. doi: 10.1037/str0000099
Zeng, Y., Wang, G., Xie, C., Hu, X., and Reinhardt, J. D. (2019). Prevalence and correlates of depression, anxiety and symptoms of stress in vocational college nursing students from Sichuan. China: a cross-sectional study. Psychol. Health Med. 24, 798–811. doi: 10.1080/13548506.2019.1574358
Zimmer-Gembeck, M. J., and Skinner, E. A. (2016). “The development of coping: Implications for psychopathology and resilience,” in Developmental Psychology: Risk, Resilience, and Intervention , ed. D. Cicchetti (New York, NY: John Wiley & Sons), 485–545.
Zumbrunn, S., Broda, M., Varier, S., and Conklin, S. (2019). Examining the multidimensional role of self-efficacy for writing on student writing self-regulation and grades in elementary and high school. Br. J. Educ. Psychol. doi: 10.1111/bjep.12315 [Epub ahead of print].
CrossRef Full Text | PubMed Abstract | Google Scholar
Keywords : coping strategies, coping flexibility, stress, self-efficacy, university students
Citation: Freire C, Ferradás MdM, Regueiro B, Rodríguez S, Valle A and Núñez JC (2020) Coping Strategies and Self-Efficacy in University Students: A Person-Centered Approach. Front. Psychol. 11:841. doi: 10.3389/fpsyg.2020.00841
Received: 29 January 2020; Accepted: 06 April 2020; Published: 19 May 2020.
Reviewed by:
Copyright © 2020 Freire, Ferradás, Regueiro, Rodríguez, Valle and Núñez. This is an open-access article distributed under the terms of the Creative Commons Attribution License (CC BY) . The use, distribution or reproduction in other forums is permitted, provided the original author(s) and the copyright owner(s) are credited and that the original publication in this journal is cited, in accordance with accepted academic practice. No use, distribution or reproduction is permitted which does not comply with these terms.
*Correspondence: María del Mar Ferradás, [email protected]
Disclaimer: All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
- Open access
- Published: 26 June 2020
“I need to take care of myself”: a qualitative study on coping strategies, support and health promotion for social workers serving refugees and homeless individuals
- Janika Mette 1 ,
- Tanja Wirth 2 ,
- Albert Nienhaus 2 , 3 ,
- Volker Harth 1 &
- Stefanie Mache 1
Journal of Occupational Medicine and Toxicology volume 15 , Article number: 19 ( 2020 ) Cite this article
13k Accesses
10 Citations
1 Altmetric
Metrics details
Social workers provide support for various groups of clients, such as refugees and homeless people. Refugees and homeless individuals represent particularly vulnerable groups in precarious living conditions. Therefore, social workers serving these clients are likely to be confronted with extensive job demands. The aim of this study was to investigate the coping strategies of social workers serving refugees and homeless individuals and to explore their support sources and health promotion offers at work as well as their respective needs.
26 semi-structured qualitative interviews were carried out with social workers in Berlin and Hamburg and analysed according to Mayring’s qualitative content analysis.
The respondents reported various coping strategies to deal with their job demands which involved both problem-oriented (e.g. time management, setting boundaries, seeking support in conflict situations) and emotion-focused approaches (e.g. self-care, distance from work, leisure activities). In addition, they emphasised various sources of workplace (social) support, e.g. provided by team members, supervisors, and other institutions. However, unmet needs for support were also formulated by the workers, e.g. in terms of individual supervision and regular exchange. Furthermore, several employees did not know about any health promotion offers at their workplace and expressed a desire for structural and behavioural health promotion measures.
Conclusions
In view of the diverse needs of the workers, the results can provide a basis to design needs-based health promotion interventions for staff in social work.
Social work in the refugee and homeless aid
In recent years, a persistent upward trend in the number of refugees and homeless individuals has been observed worldwide [ 1 , 2 ]. The global refugee population is constantly increasing, reaching 25.9 million by the end of 2018 [ 1 ]. In the context of the rapidly increasing migration in Europe in 2015 and 2016, a total of 745,545 people submitted asylum applications in Germany in 2016 [ 3 ]. Since then, the number of asylum applications in Germany has declined again (2019: 165,938), which was partly due to the refugee agreement between the European Union and Turkey [ 3 ].
Homelessness has also increased substantially in most countries [ 2 ]. In 2017, there were around 650,000 homeless individuals in Germany, from which the number of homeless recognised refugees was estimated at about 375,000. In fact, there is a notable overlap between the groups of refugees and homeless people; from 2007 to 2017, an increase in the number of non-German EU citizens and non-EU citizens in homeless assistance was observed [ 2 ]. The main reasons cited for the rising number of homeless people in Germany are the insufficient supply of affordable housing, the shrinking social housing stock and the consolidation of poverty [ 2 ].
Refugees and homeless individuals represent particularly vulnerable groups. They find themselves in precarious life circumstances, are often marginalised and frequently suffer from severe traumatic experiences [ 4 , 5 , 6 ]. Prejudices were revealed in recent surveys. For example, in 2017, 80% of German survey respondents feared a burden on the welfare state and 72% feared an increase in social conflicts due to refugee immigration [ 7 ]. Regarding homelessness, in a representative long-term study of the German population, homeless people were perceived as unpleasant (38%) and work-shy (30%) [ 8 ]. Both groups share certain similarities in terms of their precariousness (e.g., their material situation, income, social integration) and regarding their health impairment and strain (e.g. high rates of traumatisation, comorbidities between mental health disorders and substance misuse) [ 4 , 9 ]. In terms of traumatic experiences, the prevalence of traumatisation among refugee clients was found to be around 40–60%, corresponding to a significantly increased risk in these clients [ 4 ]. Overall, both refugees and homeless individuals represent important clients for today’s and future social work [ 1 , 2 ].
Previous research has examined the working conditions and health of various subgroups of social workers, e.g. mental health workers [ 10 ] or child welfare workers [ 11 , 12 ]. However, less attention has been paid to the situation of social workers in refugee and homeless aid. Social workers who provide counselling and care services for refugees and homeless individuals are likely to face similar demands in their daily work [ 13 ], which makes it plausible to conduct research studies that address workers for both client groups simultaneously. For example, particular stress factors for social workers serving refugees and homeless persons consist of cultural and language problems, negative attitudes from public towards their work and their clients as well as high caseloads due to the increasing number of clients [ 13 ]. Moreover, a relatively high prevalence of secondary or post-traumatic stress has been revealed in social workers serving refugees (52% [ 14 ]) and homeless clients (36% [ 15 ]).
In a recent scoping review of 25 studies, evidence on the working conditions, health and coping strategies of social workers serving refugees and homeless individuals was systematically mapped for the first time [ 9 ]. The review revealed common job demands for this staff, including high workloads, the bureaucratic system, clients’ suffering, difficulties in maintaining boundaries with clients, as well as limited success concerning the clients’ progress. Job resources of value to workers were also identified, e.g. a high personal meaning of work and social support from colleagues. Overall, there was a high prevalence of mental health problems (e.g. burnout) among social workers in these areas. At the same time, they were found to show high levels of job satisfaction. The review also demonstrated methodological issues in relation to available studies and claimed for more research to examine the effectiveness of coping strategies and workplace health promotion offers for staff in social work with refugees and homeless clients [ 9 ].
Similar results regarding these topics were obtained in our interview study in which social workers in refugee and homeless aid described high emotional demands, high word loads, a lack of personnel, and overtime work as critical job demands [ 13 ]. In contrast, the joy of working with their clients and appreciation from clients, colleagues and superiors were underlined as job resources. Strain reactions in relation to their work involved perceptions of fatigue and stress (as short-term reactions) as well as sleeping problems, depression and burnout symptoms (as long-term consequences). Moreover, some respondents stated that they felt ill more frequently and reported high levels of sickness absences within their institutions [ 13 ].
Given the recent findings on the job demands and strains experienced by social workers in the refugee and homeless aid as well as the limited evidence, it is important to address the question of how these workers deal with their job demands. Precisely, what coping strategies do they use and what sources of support and health promotion offers at work help them to maintain their health and well-being?
Coping strategies of social workers
In previous studies, social workers in refugee and homeless aid were found to use various coping strategies to deal with their job demands [ 5 , 6 , 16 , 17 , 18 ]. They consisted of accepting the boundaries of one’s sphere of influence [ 18 ] and maintaining professional boundaries with clients [ 5 , 16 , 17 ] and between work and private life [ 5 , 16 , 17 ]. Further coping strategies were to engage in hobbies (e.g. physical activity, reading, listening to music) and to have an active social life and exchange with friends, family members, and colleagues [ 5 , 6 , 16 , 17 ]. Moreover, coping behaviours employed by staff in the homeless sector included the acknowledgement of small successes [ 5 ] and the acceptance of clients’ undesirable behaviour without taking it personally [ 19 ]. In addition, in a study with social workers serving unaccompanied asylum-seeking refugee children, the workers used both emotion-focused (e.g. positive reappraisal, distancing) and problem-focused strategies (planful problem solving) [ 20 ].
In general, evidence from coping research suggests that coping may have an impact on the link between employees’ working conditions and health [ 21 ]. This buffering effect has also been proven in the area of social work [ 12 , 22 ]. For example, using active control-oriented coping behaviours which implied personal engagement (e.g. problem solving, cognitive restructuring, expressing emotions) buffered the impact of work stress on the emotional exhaustion and job satisfaction of social workers [ 12 , 23 ]. Similarly, in a study with child protection workers, the use of active and engaged coping strategies (rather than avoidant coping strategies) led to a decline in depersonalisation levels and increased employees’ sense of personal accomplishment [ 22 ].
Sources of support for social workers
Research suggests that further sources of support at work may help social workers to deal with their job demands [ 16 , 17 , 24 , 25 ]. In general, team support has been described as a relevant job resource for social workers [ 16 , 17 ]. Furthermore, several forms of supervision and training have been highlighted in their importance [ 16 , 24 ]. In a study with case managers serving homeless clients, managers were offered an occupational therapy consultant who provided client assessments and treatment recommendations [ 25 ]. The results showed that case managers who used the consultations more actively showed higher levels of job satisfaction and self-efficacy.
However, disparity was found in previous studies with regard to whether staff felt adequately supported or wished for more support at work [ 16 ]. Indeed, social workers in refugee and homeless aid expressed the need for external counselling, supervision and training (e.g. on self-protection or to better understand new policies) [ 5 , 16 , 17 , 24 , 26 ]. In a study with German refugee aid workers, the workers particularly wished for training to better recognise the mental health problems of their clients and learn about suitable intervention strategies [ 27 ]. In addition, frontline homeless workers expressed a desire for more support (e.g. in the form of manuals, additional personnel and supervision), team development activities and greater recognition of their needs [ 15 ].
Workplace health promotion for social workers
Studies in the area of social work, in particular refugee and homeless aid, have not yet focused on the topic of workplace health promotion. Therefore, it is still unclear to what extent social workers may benefit from health promotion offers. In general, meta-analyses indicate that workplace health promotion can contribute to maintaining employees’ health and well-being, e.g. with regard to their physical activity [ 28 , 29 ], dietary habits [ 30 , 31 ], and mental well-being [ 32 ]. Health promotion offers were also found to be associated with reduced job stress [ 28 ] and sickness absence [ 28 , 32 , 33 ] as well as increased work ability [ 32 ]. Moreover, they were related to economic benefits for companies in the form of a high return on investment [ 34 , 35 ]. In view of the possible positive effects of workplace health promotion, it seems worthwhile to explore the availability of such offers for the target group more closely.
Theoretical framework
To investigate the coping strategies of social workers, the concept of coping by Lazarus and Folkman was used as a theoretical framework [ 36 , 37 ]. According to this model, coping is defined as cognitive and behavioural efforts made to master, tolerate or reduce external and internal demands, as well as conflicts among them [ 36 , 37 ]. Coping is seen as a buffer between stressors and health outcomes [ 38 , 39 ]. Before coping behaviour is initiated, a cognitive-transactional process takes place which encompasses a primary cognitive appraisal (evaluation of the situation as potentially stressful) and a secondary cognitive appraisal (assessment of available coping resources) [ 36 , 37 ]. Coping strategies either aim at managing the stress-inducing problem (problem-focused) or at regulating emotions or distress caused by the problem (emotion-focused).
To examine the sources of support for the workers, we primarily referred to the concept of workplace social support [ 40 ]. Workplace social support emanates from multiple sources, such as supervisors, colleagues and the institution. A meta-analysis concluded that workplace social support includes both an individual’s belief that one is valued, appreciated and cared for, as well as the perception that one has access to helping relationships of varying quality and strength [ 40 ].
To assess the availability of health promotion offers and social workers’ respective needs, the Luxembourg Declaration on Workplace Health Promotion provided a useful framework [ 41 ]. The declaration defines workplace health promotion as “the combined efforts of employees, employers and society to improve the health and well-being of people at work”. Health promotion offers can include behavioural and structural interventions; the former aim at changing behavioural patterns of individuals or groups, while the latter refer to environmental and political interventions to influence health-related ecological, social, cultural and technical-material environments [ 42 ].
Study aims and research questions
The aim of the study was to investigate the coping strategies of social workers in homeless and refugee aid to deal with their job demands. In addition, we aimed to explore the sources of support and health promotion offers for these workers, as well as their respective needs. To address our study objectives, we proposed the following research questions:
What coping strategies do social workers in refugee and homeless aid use to deal with their job demands?
What sources of support are available to social workers in refugee and homeless aid at their workplace?
What health promotion offers are available to social workers in refugee and homeless aid, and what are their respective needs that are currently not addressed?
Materials and methods
Study design.
We conducted 26 semi-structured qualitative interviews with staff in social work in Berlin and Hamburg. Interviews were carried out from October to December 2017. The qualitative approach was chosen as it allowed us to gain first explorative insights into little researched topics. Since little was known about the topics for the specific target group, a qualitative investigation was most suitable to get a comprehensive and detailed understanding. A central advantage of the qualitative method is that it allows to describe complex social phenomena from the perspective of the people affected. Semi-structured interviews were especially suitable in order to approach the target group and study the topics within their natural environment [ 43 ]. The results of the qualitative study were subsequently used as a basis to design a quantitative online survey.
Recruitment of participants
Participants were recruited from institutions in the refugee and homeless aid sector. Purposeful sampling was applied to the selection of institutions by contacting walk-in and residential facilities from various supporting organisations. Institutions were informed about the study by telephone and sent invitation emails and leaflets which were distributed within the organisations. In total, 19 institutions were contacted from which 10 agreed to participate. Employees who were interested in participation could contact the researchers confidentially and directly to make interview appointments (convenience sample). Eligibility criteria for study participation were as follows: participants had to have direct contact with refugees and/or homeless individuals at work and at least 6 months of work experience in social work. Moreover, they had to be of full age and fluent in the German language. Volunteers and employees working in administrative services without direct contact to clients were excluded from the study.
Data collection
A semi-structured interview guideline was developed based on the empirical evidence and theoretical background. The questions of the interview guideline regarding the coping strategies, sources of support and health promotion are provided in Additional file 1 . The guideline consisted of further questions, e.g. regarding social workers’ working conditions and strains, which are presented elsewhere [ 13 ]. A pretest interview was carried out with a former social worker from refugee aid. The guideline was slightly revised based on the workers’ recommendations. The interviews were conducted by two female researchers, a health scientist and a psychologist who were experienced with qualitative research and worked as researchers in occupational health psychology during the study period. Prior to data collection, participants were informed about the study aims and data confidentiality and signed a declaration of informed consent. All interviews were carried out face-to-face and took place in the workers’ institutions during their work time. The interviews were conducted in German and recorded with an audio device. They lasted from 27 to 86 min (51 min on average). The participants were able to terminate the interviews at any time. Interviews were conducted until no new topics were identified, i.e. data saturation was reached. Field notes were made immediately after each interview. No repeat interviews were carried out.
Data analysis
The audio recordings were transcribed verbatim and subsequently anonymised. The data analysis was carried out in a deductive-inductive process according to Mayring’s qualitative content analysis [ 44 ]. Important features of this analysis include the systematic and rule-based approach and the development of a profound category system [ 44 ]. The well-validated, rule guided process applied in Mayring’s content analysis strengthens the reliability of the qualitative results. Qualitative content analysis was chosen, since this method focuses on the content (rather than on the latent meaning) of what is said [ 45 ]. Thus, we adopted a realistic position in the theory of science by focusing on the semantic content of the data [ 45 ]. The main categories were retrieved deductively on the basis of the interview guideline. Moreover, sub-categories were developed inductively in an iterative process. First, one interview was test-coded by both interviewers and compared in terms of consensus. Disagreements were thoroughly discussed until consensus was reached and the coding system was slightly revised. The other interviews were then each coded by one interviewer. Unclear coding was regularly discussed during team meetings. The software MAXQDA Analytics Pro (version 11) was used for the analysis [ 46 ]. The final coding system was summarised in a separate document in which the material was further compacted (paraphrased, generalised and reduced) in accordance with Mayring’s specifications [ 44 ]. During the analysis, the researchers’ personal involvement, preconceptions and influence on the results and interpretations were thoroughly reflected upon. In order to minimize such personal influences, special emphasis was placed on discussing results in the team and weighing up alternative paths of interpretation together to increase validity of the findings. Results were not made available to the participants before completion of the data analysis. Direct quotes from the interviewees were translated into English by a native speaker. The COREQ-Checklist was used to describe the study [ 47 ].
Participant characteristics
In total, 17 interviewees were female and 9 were male (Table 1 ). They were aged between 26 and 64 years with a mean age of 42 years. The majority had a degree in social work ( n = 16). 14 interviewees worked in homeless aid and 12 in refugee aid. Most of the participants worked full-time ( n = 20) and had three or less years of experience in social work ( n = 15).
Coping strategies
The coping strategies presented in the following were named by the participants as strategies they actually applied and perceived as helpful. The strategies were classified into problem-oriented and emotion-oriented strategies.
Problem-oriented strategies
Problem-oriented strategies referred to employees’ work tasks and content, to the work organisation, social relations and personal strategies (Table 2 ).
Work tasks and content
Some employees reported that they had actively reduced their work tasks and only accepted tasks they were responsible for and able to finish on time. Moreover, acquiring knowledge in dealing with stress was described as a coping strategy and associated with an increased sense of security and the development of a professional identity. Knowledge was, for example, acquired through training and education, reading books and having discussions with experts in the field. Moreover, independent problem-solving and solution-oriented thinking were reported as a further coping strategy at work:
“There is a lot of collaborative thinking involved, and a lot of ‘Yes, okay, how can we solve this now? It’s hard, of course, but we’ll try to find a solution for this now too.’ And, yes, there is a lot of willingness too.” [#21, female, homeless aid].
Work organisation
With respect to work organisation, having good time management was an important strategy. This included scheduling enough breaks between appointments and avoiding appointments at the beginning of a working day to be able to prepare for the day. Furthermore, compliance with regular working hours, breaks and counselling times and the avoidance of overtime work were highlighted in order to recover briefly during breaks and between consultations:
“Yes, so at the beginning I did a lot more overtime. And, well, now I’m trying to curb that a bit. (…) Including when it comes to consulting time. “[#9, female, homeless aid].
Two interviewees mentioned that they had deliberately reduced their work time in order to decrease their workloads, which was perceived as a relief. In situations of high workload and time pressure, another strategy named by the interviewees was to prioritise tasks that needed to be done:
“Setting priorities. You learn that with time. What can I move, what can I let go? (…) But that simply comes with experience, which comes with time.” [#23, male, homeless aid].
Many interviewees described that setting clear boundaries between work and private life was an essential strategy to be able to switch off from work. These people explained, for example, that they did not share their private telephone numbers with clients, did not meet clients in their spare time and did not discuss work-related problems at home with their family and friends:
“Sometimes we even make it clear, and say that today we aren’t going to talk about work, or about clients, or about anything remotely to do with social work. Simply so that you can switch off for once.” [#22, female, homeless aid].
Two interviewees also described their efforts to create change at higher levels of the system, e.g. through discourse with responsible staff, committee work or work situation analyses at their workplaces in order to identify critical job demands.
Social relations
Several workers reported setting limits towards clients at work as a fundamental coping strategy. This involved showing clients the limits for aid and support, pointing out clients’ personal responsibilities and encouraging them to reflect on their (sometimes unrealistic) expectations:
“Sometimes there are these expectations: ‘You’re my support worker, you have to solve this for me or do that for me.’ And we have to tell people again and again, I can help you with this and that issue, I’m here to help you with this, but this and that you have to do yourself.” [#24, female, refugee aid].
Employees stated that it was particularly important to set clear boundaries in cases where clients showed demanding and aggressive behaviour or disrespectful conduct towards women:
“And I set really clear boundaries. If they come in acting in an aggressive manner and insult me, then I say: ‘You have to leave now and when you’ve calmed down, then you can come back and we can talk to each other calmly.” And then they might come back a couple of days later and have calmed down.” [#25, male, refugee aid].
A general coping strategy in conflict situations consisted of acting self-confidently, calmly and in a self-determined manner, while showing understanding and empathy for the clients’ needs at the same time. Moreover, actively searching for support in challenging situations was another strategy stated by many interviewees; for example, asking colleagues for help, requesting additional supervision or calling the police as a last resort in cases where clients acted in an extremely violent or aggressive manner:
“And when it’s totally unacceptable and residents won’t calm down at all, then I just call the police.” [#22, female, homeless aid].
In addition, overcoming language barriers with clients by communicating through gestures and mimicry was reported as a strategy by one worker. Another respondent described that it was important to discuss conflicts with colleagues and superiors (e.g. bullying, gossip) directly and openly with the involved team members.
Personal strategies
With respect to coping strategies at a personal level, one worker mentioned receiving medical treatment for insomnia and sleep disorders. Furthermore, three interviewees stated that they had started psychotherapy to be able to talk about their job strain and learn about mechanisms to better deal with their demands at work:
“A year ago I started psychotherapy because I was just going straight to sleep when I got home from work. And I simply wasn’t doing anything else (…). It was just work and sleep, work and sleep. So that’s why I started therapy and have learned how to deal with this strain.” [#4, female, refugee aid].
In this regard, psychotherapy sessions were described as a substitute for a lack of collegial counselling and individual supervision that was not provided by the employer:
“In the end I sorted out psychotherapy for myself (…). I just simply got to the point where I said, ‘Okay, I have to look after myself, because what I need isn’t happening here.’” [#6, female, refugee aid].
Emotion-oriented strategies
The emotion-oriented coping strategies named by the interviewees are depicted in Table 3 .
Seeking emotional support and exchange with partners, parents and friends represented an important emotion-oriented coping strategy for many participants, especially when there were acute problems at work. In addition, a lot of the interviewees highlighted the relevance of regular exchange with their colleagues, and sometimes also with executives:
“There you can also (…) talk about things that are bothering you at the moment or just vent. That really helps a lot.” [#2, female, homeless aid].
Engagement in leisure activities
Further emotion-oriented coping strategies were related to the engagement in leisure activities to seek distraction, detachment and a balance with work. Many respondents emphasised that they preferred active activities in their spare time, such as sports or physical activity (e.g. sports courses, cycling, swimming, dancing and horse riding). Spending time and pursuing activities with friends and family was often deemed helpful. Other workers reported that they preferred calm activities as a contrast to their busy working lives, e. g. yoga, qi gong, or going to the sauna:
“Well, I can already see that I really need to relax and recover a lot in my private life, so there you really have to find an absolute counterbalance, otherwise it gets really difficult.” [#11, female, refugee aid].
Spending time in nature and outdoors, for example going for walks with the dog or gardening, was described as a compensation for stressful and mainly sedentary work. According to several workers, it represented a good way to switch off from work:
“I surround myself in nature a lot. I go out with my dog and even sometimes make my journey to or from work longer and use the time to go for a walk or bike ride (…). And by doing that I definitely unwind.” [#3, female, homeless aid].
Creative hobbies were also mentioned by some respondents, e.g. making music, singing, writing, sewing or photography. Others indicated reading or using media, such as TV or the computer, to detach from work.
Acceptance and focus
Another coping strategy mentioned by many respondents consisted of withstanding negative feelings at work (e.g. caused by criticism regarding one’s way of working). As described by the interviewees, such feelings could be reduced by cognitively distancing oneself from criticism and confidently following one’s own work tasks. Moreover, accepting situations that could not be changed was described as important, for example, with regard to the fates of clients, when clients maintained their unrealistic expectations or did not accept help:
“Well, just by simply saying: ‘I accept the situation as it is.’ Being able to do that is also pretty difficult, as you actually have your own ideas of how things might go for people, but it often just doesn’t work out.” [#9, female, homeless aid].
In addition, one interviewee underlined that it was helpful to concentrate on the positive sides of work and to remind oneself and one’s clients of previous positive achievements:
“(…) that again and again you try to concentrate on the positive things and remind yourself: What went well and what have you already achieved?” [#2, female, homeless aid].
Self-care and mindfulness
Further coping strategies were related to the workers’ self-care. Some interviewees stressed the importance of reporting sick in the event of illness and of taking short breaks at work despite potentially negative comments from colleagues or postponed work. Various workers talked about not being put under stress, being mindful, knowing one’s limits and not working beyond them. Increasing awareness of one’s own needs was described as essential, as well as taking concrete actions for recovery at work, e.g. using relaxation techniques, having active breaks or following healthy eating:
“You have to watch out for that, and when you realise, you have to say: ‘Okay, good, I have to look after myself a bit too.’ So simply that you keep an eye on yourself.” [#7, female, homeless aid].
Distance to work
Creating distance from work, especially from clients’ problems and concerns, was described as a useful coping strategy to better deal with challenges and perceived failures in the work context. This meant taking a step back from clients’ problems and “getting a big tank”:
“I try maybe to not let everything get to me. So (…) that they are their problems, not my problems, basically.” [#1, female, homeless aid].
It also meant not taking failures, aggression or appointment cancellations by clients personally. Helpful mechanisms were to consciously reflect and understand that failures had nothing to do with one’s professional skills, and to recall the clients’ responsibilities:
“It’s really a question of attitude (…), that people are always independent and act independently. And, yes, that I offer support and provide guidance, but that I can’t do things for them (…).” [#21, female, homeless aid].
Sources of support
There were various sources of support mentioned by the interviewees, many of them relating to workplace social support, i.e. interpersonal relationships in the work context (Table 4 ).
Support from colleagues and supervisors
Social workers repeatedly stated that support was provided by their colleagues in the form of collegial advice in difficult situations, which was especially helpful for finding quick solutions. Good team spirit and sense of community were also underlined by most of the workers. It was stated that colleagues cared for each other and that an open question culture was promoted:
“Well, advice from colleagues, that goes really fast. We simply go from door to door or we arrange to meet, that goes pretty well and works out pretty well.” [#8, male, homeless aid].
Moreover, supervisors’ support was mentioned. For example, it was specified that they were approachable for work-related questions and particularly supportive in difficult situations at work:
“And that we also have a boss who is receptive to us and takes us seriously. That’s also worth a lot and I have had completely different experiences with that.” [#2, female, homeless aid].
Team meetings
Team meetings were also pointed out as an important source of support by several workers. In many cases, meetings in small teams were held once a week. Meetings in larger teams, e.g. cross-departmental or cross-location meetings, took place every 2 weeks, once a month or every 3 months. Team meetings were predominantly regarded as helpful for regular exchange and, in some cases, for collegial case consulting. However, some participants perceived the meetings as too superficial or too short to provide enough time for detailed discussion:
“Case assessments are sometimes too short because in team meetings we have to talk about organisational issues and things like that, and in the end case discussions are neglected a bit.” [#20, female, homeless aid].
Team meetings were sporadically used to develop concrete measures for improving the work conditions. Examples for such measures were the provision of number assignments for clients for open consultation hours, the use of stop signs indicating that there was no consultation hour, and the provision of mobile phones for communication with clients. Three workers also explained that conceptual and strategic planning took place on so-called “concept days” in the institutions:
“Well, we do concept days here where we get together and talk and think about next steps. And actually I find that pretty ideal here.” [#10, male, homeless aid].
Supervision
Supervision was another important source of support for many interviewees. It was typically provided once a month and in the form of group supervision. Some participants described larger time periods for supervision, e.g. once every 6 or 8 weeks. Two workers indicated that group supervision was not available to them. For the majority of the workers, supervision was perceived as helpful for self-reflection, knowledge exchange and for learning new tools and work methods:
“I find supervision helpful because then somebody external comes along and sometimes you’re sort of a bit out on ledge when you’re just doing things yourself. And that just gives another perspective, which is often simply a relief.” [#3, female, homeless aid].
However, dissatisfaction with supervision was also occasionally expressed, e.g. that it had to be postponed or cancelled due to understaffing, or that group supervision was not welcomed by all team members. The availability of individual supervision varied: for most of the interviewees, this form of supervision was not available. One worker stated that individual supervision was generally available, another said that it was only available for managers, and two interviewees declared that it was only available in extremely worrying situations (e.g. stalking, sexual abuse).
Training courses
The provision of training courses was another frequently mentioned source of support. Courses covered a range of topics, e.g. legal aspects, de-escalation techniques, counselling know-how and management skills. In some cases, there was a training budget available for each employee, and employees could select and request training themselves:
“I am offered [training], internally or sometimes I can even make suggestions and organise things myself. And taking part in training with other providers is also approved and financed. That’s important.” [#12, male, refugee aid].
Support from other institutions
Single interviewees described further sources of support within their institutions, e.g. support provided by experts from the human resources department or the sponsoring association. With respect to support from external sources, three workers stated that there were no other institutions to which they could turn for advice. The other workers described several sources of support in the form of network centres and counselling services (e.g. for issues like violence, drugs, debt and flight). Furthermore, sources of support also included federal associations, lawyers, doctors, psychologists, training providers, former professors and colleagues, volunteers or professionals with similar tasks who could be asked for advice. Cooperation with other institutions was generally perceived as supportive, as it allowed the interviewees to pass clients on to other parties if they were not able to provide support in all necessary aspects:
“A large part of the work is actually that we look to see where there are places where we can send our people if they need special or concrete help.” [#15, male, refugee aid].
Support in private life
Employees also described sources of support in their private lives provided by partners, families, friends and roommates. Support was particularly noticed when people in the family or circle of friends had a refugee background themselves and could assist with translation or interpreting tasks. Conversations with family members were also generally perceived as supportive:
“Well, in my family we talk about the topic of homelessness a lot (…). My partner is also very interested in what I do and asks about it, so does my family.” [#8, male, homeless aid].
- Workplace health promotion
Comments on workplace health promotion concerned the availability of health promotion offers as well as the further needs and wishes of employees.
Available health promotion offers
Overall, six respondents declared that no health promotion offers were available at their workplace, although some of them indicated the possibility of available health promotion offers that were unknown to them, e.g. due to the size of their organisations:
“Maybe it does exist. But I think I just don’t know anything about it. Around Germany, they [the institutions] have up to 14,000 workers, and (…) a lot of roles and facilities and it is sometimes not really clear and you don’t always find out about everything.” [#14, female, refugee aid].
Other workers reported several health promotion activities which consisted of individual offers rather than systematic workplace health management. With regard to behavioural measures, eleven interviewees stated that health days were organised every year or every 2 years. Two workers stated that there were massage services offered. These were either cross-departmental health days for all employees or organised individually by smaller teams. Moreover, respondents mentioned that courses and workshops were offered on different topics, ranging from stress management, mindfulness, yoga and relaxation to back training, healthy cooking and acupuncture. Quick relaxation and sports exercises were also occasionally organised, e.g. in the form of active lunch breaks. Furthermore, one respondent said that there was a volleyball group and another stated that there was an intern who had given the team Kung Fu lessons.
With respect to structural measures, four interviewees reported that companies offered medical examinations, vaccinations and funding for glasses at work. In addition, five workers reported funding for the use of gyms and two for fruit purchases at work. The implementation of a risk assessment on mental stress, regular health and safety information, funding for participation in company runs, and a service bike offer were described by one worker each.
In terms of workers’ experiences with health promotion offers, some employees stated that they had already used the offers or planned on doing so in due course. Six workers who had not used any offer so far indicated various reasons for not having done so, e.g. a lack of interest in existing offers and lacking motivation after work. In addition, the preference to take part in sport offers privately rather than in the work context was expressed by seven employees:
“I mean, doing exercise activities with my colleagues isn’t really my thing. Doing Thai Chi on the roof with people, I would find that a bit weird. Because I do my own exercise.” [#5, female, refugee aid].
Two respondents cited shift work as a major obstacle to participation in health promotion activities. Moreover, excessive workload and a resulting lack of time were described. One worker said that courses took place at unfavourable times and two commented that they took place in unfavourable locations (e.g. offers held in headquarters, but not in branch offices). Furthermore, the unclear and time-consuming registration process was noticed. Three respondents said that they would have to initiate and organise health promotion activities themselves, since this was not organised by the institutions.
Needs and wishes for health promotion offers
In terms of behavioural measures, several respondents stated their general interest in sports offers and in the organisation of company sports groups (e.g. a running group after work):
“Doing some sort of exercise activities with colleagues, some communal activities. Just that we do something to release a bit of energy and have a laugh, laughing is important.” [#7, female, homeless aid].
Requests for regular, company-wide training courses were also made. Such courses should consist of a mixture of theory and practice and deal with various topics, e.g. back therapy training, stress management, relaxation techniques, qigong, yoga, body awareness, de-escalation and self-care. Three respondents particularly wanted activities to be offered during their work hours. Moreover, easily accessible activities at different times of the day were preferred and considered necessary for coordination with shift work:
“You would really have to be able to choose when you go. (…) That you really can go in the mornings, maybe in the evenings, because, you know, we do a lot of shift work.” [#23, male, homeless aid].
Four workers reported their desire for massages at work and two wished for a massage chair. Regarding structural measures, financial support for private hobbies and discounts for nearby gyms were desired. Moreover, further supervision, contact to lawyers for legal questions and regular medical examinations were stated. In addition, one respondent introduced the idea of a social worker counsellor working in the organisation’s facilities (instead of hard-to-reach external supervision):
“If someone were to come into the facility and simply offer an open space to talk, somewhere you can simply drop in. Someone that doesn’t work here themselves, but who you could go to and simply talk about things, especially during working hours. A social worker for social workers.” [#6, female, refugee aid].
With regard to the work environment, separate rooms for exercise and relaxation activities as well as rest rooms for breaks were requested. Two workers indicated their satisfaction with the available health promotion offers and stated that they had no need for further offers.
To our knowledge, this is the first study to empirically explore the coping strategies, support sources and health promotion offers available to German social workers in the growing work areas of refugee and homeless aid. By conducting qualitative interviews with 26 social workers in these fields, we were able to gain important new insights into these topics and extend current evidence.
Some of the problem-focused coping strategies identified in this study have previously been reported for social workers, such as the strategies of setting limits and boundaries in contact with clients or with regard to work and private life [ 5 , 16 , 17 ]. Moreover, acquiring knowledge (e.g. through training activities) in order to manage work-related stress has also been stated before by German refugee aid workers [ 27 ]. In addition to this, our study uncovered further problem-oriented strategies that have received little attention so far, such as strategies related to employees’ work organisation and time management. Time management coping strategies were described as helping workers prioritise and make the best use of their time, which was particularly important in view of their multiple work tasks and restricted time resources.
Another important coping strategy revealed in our study was the search for social support. This strategy emerged both in the context of problem-oriented coping strategies (seeking instrumental support from colleagues and superiors to deal with stressful situations and concrete problems at work) and emotion-oriented coping strategies (seeking informal social support from family and friends to alleviate negative emotions). In general, the search for social support is a frequently used coping strategy, and protective links between social support and health are well documented [ 48 , 49 ]. The finding is consistent with previous research in which social support represented an essential job resource for staff in refugee and homeless aid [ 6 , 50 ].
In addition, a notable finding of our study is that some interviewees had started psychotherapy to better cope with their job demands and associated strains. The fact that psychotherapy was initiated by the interviewees themselves points to a high level of suffering among these workers, which was emphasized by the workers themselves. In accordance with this, previous studies have shown a high prevalence of long-term psychological strain reactions among social workers, including depressive moods and burnout [ 9 , 13 , 51 , 52 ]. The result is somewhat alarming, as it suggests a perceived lack of possibilities for the workers to address their problems in the workplace and receive adequate help, e.g. through individual supervision. In fact, individual supervision was unavailable to most workers in our study. Earlier research suggests that the availability of individual supervision may vary across different settings and countries. For example, in a recent study on homeless aid in the UK, 83% of the frontline workers had access to individual supervision [ 26 ].
With respect to the reported emotion-oriented coping strategies, being active (e.g. exercising, taking walks outdoors) and pursuing leisure activities were underlined by many workers as central coping behaviours. The importance of these strategies has been outlined before [ 5 , 6 , 16 , 17 ]. Moreover, actively organising their leisure time helped the workers to get away from work. Evidence suggests that social workers often find it difficult to switch off from work [ 13 , 17 ], which further explains their use of coping strategies that enable them to detach and recover from job stress.
Further emotion-focused coping strategies employed by the interviewees were the strategy of avoiding presenteeism and consciously taking self-care actions. Similarly, the use of self-care strategies (e.g. diet changes, improvement in sleep hygiene, relaxation) was found to be a functional coping strategy [ 21 ] which was also used by employees in homeless aid [ 6 ].
Notably, several emotion-oriented coping strategies used by the workers in our study involved cognitive components, e.g. gaining mental distance from work, accepting unchangeable situations and focusing on positive experiences. In earlier studies with social workers, similar cognitive coping efforts were described, e.g. with regard to the acceptance of clients’ undesirable behaviour without taking it personally [ 19 ] and of their boundaries of influence [ 18 ]. The use of cognitive coping strategies may be particularly efficacious for social workers when they encounter problems that cannot be changed directly (e.g. political laws). However, making use of such strategies is also demanding, as it firstly requires the workers’ ability to reflect problems on a meta level.
In earlier research, most of the coping strategies employed by social workers were classified as emotion-focused [ 9 ]. In comparison, employees in our study used both problem-oriented and emotion-oriented strategies, although a slight tendency towards the use of more emotion-oriented strategies was observable. Referring back to the theoretical definition of coping provided by Lazarus and Folkman [ 36 , 37 ], the variety of identified coping strategies underpins the notion that most individuals use both problem-oriented and emotion-oriented coping strategies to deal with stressful events [ 36 ].
Regarding the identified sources of support for social workers, most of them were linked to workplace social support [ 40 ], e.g. provided by team members, supervisors, external persons and institutions. This result underlines the importance of social interaction for the working group. It also suggests that the workers may already have some sources of support available in the work setting. At the same time, however, our study sheds light on potential for improvement, e.g. with regard to team meetings and supervision being postponed, too short or too superficial to provide help for complex problems. Our results are consistent with earlier research indicating that social workers (especially those with severe strain reactions) did not feel sufficiently supported by supervisors [ 13 ]. External supervision and consulting are important tools for reflecting on one’s work methods and stressors, and have shown protective effects on the health [ 53 ] and job satisfaction [ 25 ] of social workers. Conversely, a recent qualitative study suggested that inadequate supervision and a lack of supervisor support may play a critical role in the development of long-term strain among social workers [ 13 ]. Summarising the above, the need for adequate supervision for social workers in homeless and refugee aid has been raised before [ 9 , 13 ] and is strongly reinforced by our results.
With regard to workplace health promotion, a relevant finding of our study is that several employees were unaware of health promotion offers at their workplaces, although some of them indicated that such offers could possibly exist. Furthermore, several workers named individual health promotion offers, but none of them described a systematic workplace health management. On the one hand, this suggests that there may be little systematic approaches to workplace health management within the organisations so far. On the other hand, the findings may also point to a lack of information on the part of the interviewees, suggesting that health promotion offers may not be advertised properly and that communication flows within the organisations need to be improved. Many of the cited needs for behavioural and structural health promotion measures are consistent with the results from earlier research. For example, in terms of behavioural measures, the respondents wished for regular and company-wide training courses on a range of topics, which has been similarly revealed in previous studies [ 16 , 50 ]. A recent study showed that over one fifth of frontline workers in homeless services never had access to relevant training, e.g. relating to suicide, self-harm and mental health [ 26 ]. Some training options were especially scarce, e.g. training on trauma and domestic violence, which one third of the workers had never received. Needs in terms of structural measures concerned offers for supervision and counselling as well as changes in the work environment. Likewise, in a recent study, it was demanded that employees should be provided with adequate facilities to enable relaxation during their breaks [ 13 ].
Implications
From the results of our study, some implications for research can be drawn. In terms of research-related implications, quantitative studies with higher sample sizes should be carried out to generalise and quantify our findings, e.g. regarding the potentially positive effects of coping and the status quo of workplace health promotion for social workers in refugee and homeless aid. In future studies, it would be interesting to compare the support sources and health promotion offers for social workers in different work settings (e.g. organisations of different types and sizes, with independent and public sponsors, and in rural and urban structures). This could help to gain a deeper understanding of the beneficial and impeding factors for implementing health promotion offers.
Practical implications can also be derived (Table 5 ). Our findings indicate that workplace interventions should be carried out aiming at empowering social workers to further expand upon their coping strategies. In organised courses and workshops, employees could acquire relevant skills and learn about further ways of coping with job stress in a resilient manner. With respect to the development of support sources, demands for greater support and expanded supervision for social workers have previously been made [ 53 ] and are strongly reinforced by our findings. Supervision is highly valuable, as it promotes reflection, support and evidence-based expertise [ 53 ]. To support employees in dealing with their emotional demands, easy and low-threshold access to qualified supervision must be provided for all workers in the form of individual and/or group supervision. This seems particularly relevant in view of the stress factors and secondary/post-traumatic stress in social workers serving refugees and homeless clients [ 14 , 15 ]. In the same vein, it is important to inform the workers well about the usefulness of supervision, especially those who are still inexperienced and unsure about using this offer. Moreover, team support within the institutions should be nurtured and upheld. For this purpose, the provision of regular meetings with sufficient time for case consulting and enough room to spend breaks together with colleagues would be useful. Emphasis should also be placed on networking, regular exchange and cooperation with other counselling services which can provide support as neutral entities.
In view of the diverse needs for health promotion stated by the workers, our findings provide a useful starting point for planning needs-based health promotion offers. Suitable structural measures may address the work organisation (e.g. in terms of ensuring reliable work hours and a manageable workload). They should also aim at improving the work environment, e.g. by providing more rooms for rest and recovery. With respect to behavioural measures, training courses on work- and health-related topics (exercise, relaxation, de-escalation, violence, etc.) are recommended. For example, since workers in our study mentioned aggressive behaviour of clients, the availability of training courses on de-escalation and non-violent communication may be particularly helpful for those who encounter such problems at work. Our results indicate that initial health promotion offers are already available at many organisations, meaning that future interventions can be based on existing offers and can expand upon them, taking the workers’ needs into account. Employees should be given opportunities to make flexible use of health promotion offers, e.g. during work hours and at different locations in order to improve coordination with shift work, which is often a major obstacle in participation. Since health promotion offers may not always be well-promoted, this highlights the importance of systematic and target-oriented advertisement within the organisations. After all, politicians at a higher level also have a responsibility for creating a framework and providing sufficient resources to promote these crucial fields of social work, so that adequate programs can be implemented at company level.
Strengths and limitations
A particular strength of this study is that the views of social workers were assessed in a heterogeneous sample (e.g. in terms of age, work experience, etc.). Thereby, we were able to capture different perspectives and broadly map the topics of interest. Considering the explorative character of the study, a sufficient number of workers was included in order to attain data saturation [ 54 ]. Further strengths of this study are the consistent orientation towards and application of recognized field practices, e.g. the data analysis according to Mayring’s qualitative content analysis [ 44 ]. To improve the internal quality of the study, we used rich descriptions as well as numerous direct quotes to describe our results [ 55 ], and applied the international checklist “COREQ” [ 47 ]. Moreover, all results were compared to empirical references and to the theoretical framework [ 56 ].
Some limitations of the study should also be noted. As in any qualitative study, the interviewees’ responses may have been influenced by the lack of anonymity between the workers and the interviewer as well as by social desirability tendencies. Selection effects cannot be ruled out either. For example, all respondents spoke fluent German and were rather young; results could be different for older employees or employees of other nationalities. Qualitative research captures the subjective perspectives and truths of the respondents. The interview sample is not representative of the general population of social workers, and the results are not generalisable to other settings or time periods. The temporal context of the study period should also be noted: the interviews were conducted in autumn 2017, when immigration in Germany slowly subsided, leading to restructuring measures and closures of institutions. In homeless aid, employees experienced a steady increase in homelessness and changes in the clientele in terms of, for example, gender and origin [ 57 ]. Such recent developments should generally be kept in mind with regard to their potential impact on our results.
The results of the study provide novel insights into the coping strategies employed by social workers in refugee and homeless aid and into the available support sources and workplace health promotion. On the one hand, the findings show that social workers use multiple coping strategies and have access to different support sources in the workplace, helping them to deal with their job demands and regulate their emotional responses. On the other hand, the results suggest that certain needs for support among employees are not yet covered, and that systematic workplace health promotion appears to be scarce within the organisations. The identified wishes of the workers for behavioural and structural measures are particularly relevant for health promotion, as they indicate diverse areas and starting points for policy makers and organisations to design needs-based health promotion interventions for social workers in refugee and homeles aid.
Availability of data and materials
The datasets are not publicly available due to German national data protection regulations. They are available from the corresponding author upon reasonable request.
United Nations High Comissioner for Refugees. Global trends: Forced displacement in 2018. Geneva: UNHCR: The UN Refugee Agency; 2019.
Google Scholar
BAG Wohnungslosenhilfe e.V. Zahl der Wohnungslosen. Available online: http://www.bagw.de/de/themen/zahl_der_wohnungslosen/index.html (Accessed on 11.09.2019).
Bundesamt für Migration und Flüchtlinge (BAMF). Das Bundesamt in Zahlen 2019. Nürnberg: Bundesamt für Migration und Flüchtlinge; 2020.
Pell M. Sekundärtraumatisierung bei Helferinnen im Umgang mit traumatisierten Flüchtlingen. Vienna: University Vienna; 2013.
Lakeman R. How homeless sector workers Deal with the death of service users: a grounded theory study. Death Stud. 2011;35(10):925–48.
PubMed Google Scholar
Lusk M, Terrazas S. Secondary trauma among caregivers who work with Mexican and central American refugees. Hisp J Behav Sci. 2015;37(2):257–73.
Stiftung B. Willkommenskultur im “Stresstest”. Einstellungen in der Bevölkerung 2017 und Entwicklungen und Trends seit 2011/12. Gütersloh: Bertelsmann Stiftung; 2017.
Gerull S. “UNANGENEHM”, “ARBEITSSCHEU”, “ASOZIAL”. Zur Ausgrenzung von wohnungslosen Menschen. Aus Politik und Zeitgeschichte(APuZ). 2018;25-26(18):30–36.
Wirth T, Mette J, Prill J, Harth V, Nienhaus A. Working conditions, mental health and coping of staff in social work with refugees and homeless individuals: a scoping review. Health Social Care Community. 2019;27(4):e257–e69.
Coyle D, Edwards D, Hannigan B, Fothergill A, Burnard P. A systematic review of stress among mental health social workers. Int Soc Work. 2005;48(2):201–11.
McFadden P, Campbell A, Taylor B. Resilience and burnout in child protection social work: individual and organisational themes from a systematic literature review. Brit J Soc Work. 2014;45(5):1546–63.
Stalker CA, Mandell D, Frensch KM, Harvey C, Wright M. Child welfare workers who are exhausted yet satisfied with their jobs: how do they do it? Child Fam Soc Work. 2007;12(2):182–91.
Wirth T, Mette J, Nienhaus A, Schillmöller Z, Harth V, Mache S. “This Isn’t Just about Things, It’s about People and Their Future”: A qualitative analysis of the Working Conditions and Strains of Social Workers in Refugee and Homeless Aid. Int J Environ Res Public Health. 2019;16(20):3858.
PubMed Central Google Scholar
Kim YJ. Secondary traumatic stress and burnout of north Korean refugees service providers. Psych Investigation. 2017;14(2):118.
Waegemakers Schiff J, Lane A. BURNOUT AND PTSD IN WORKERS IN THE HOMELESS SECTOR IN CALGARY. 2016. Available online: http://calgaryhomeless.com/content/uploads/Calgary-Psychosocial-Stressors-Report.pdf (Accessed on 03.11.2019).
Guhan R, Liebling-Kalifani H. The experiences of staff working with refugees and asylum seekers in the United Kingdom: a grounded theory exploration. J Immigr Refug Stud. 2011;9(3):205–28.
Kidd SA, Miner S, Walker D, Davidson L. Stories of working with homeless youth: on being “mind-boggling”. Child Youth Serv Rev. 2007;29(1):16–34.
Ferris LJ, Jetten J, Johnstone M, Girdham E, Parsell C, Walter ZC. The Florence nightingale effect: organizational identification explains the peculiar link between Others’ suffering and workplace functioning in the homelessness sector. Front Psychol. 2016;7:16.
PubMed PubMed Central Google Scholar
Kosny AA, Eakin JM. The hazards of helping: work, mission and risk in non-profit social service organizations. Health Risk Soc. 2008;10(2):149–66.
Sundqvist J, Ghazinour M, Padyab M. Coping with stress in the forced repatriation of unaccompanied asylum-seeking refugee children among Swedish police officers and social workers. Psychology. 2017;08(01):97–118.
Lian Y, Gu Y, Han R, Jiang Y, Guan S, Xiao J, et al. Effect of changing work stressors and coping resources on psychological distress. J Occup Environ Med. 2016;58(7):e256–e63.
Anderson DG. Coping strategies and burnout among veteran child protection workers. Child Abuse Negl. 2000;24(6):839–48.
CAS PubMed Google Scholar
Koeske GF, Kirk SA, Koeske RD. Coping with job stress: which strategies work best? J Occup Organ Psychol. 1993;66(4):319–35.
Robinson K. Voices from the front line: social work with refugees and asylum seekers in Australia and the UK. Brit J Soc Work. 2013;44(6):1602–20.
Chapleau A, Seroczynski AD, Meyers S, Lamb K, Haynes S. Occupational therapy consultation for case managers in community mental health. Prof Case Manag. 2011;16(2):71–9.
Lemieux-Cumberlege A, Taylor EP. An exploratory study on the factors affecting the mental health and well-being of frontline workers in homeless services. Health Soc Care Community. 2019;27(4):e367–e78.
Grimm T, Georgiadou E, Silbermann A, Junker K, Nisslbeck W, Erim Y. Psychische und kontextuelle Belastungen, Motivationsfaktoren und Bedürfnisse von haupt- und ehrenamtlichen Flüchtlingshelfern. Psychother Psych Med. 2017;67(08):345–51.
Conn VS, Hafdahl AR, Cooper PS, Brown LM, Lusk SL. Meta-analysis of workplace physical activity interventions. Am J Prev Med. 2009;37(4):330–9.
Proper KI, Koning M, Van der Beek AJ, Hildebrandt VH, Bosscher RJ, van Mechelen W. The effectiveness of worksite physical activity programs on physical activity, physical fitness, and health. Clin J Sport Med. 2003;13(2):106–17.
Maes L, Van Cauwenberghe E, Van Lippevelde W, Spittaels H, De Pauw E, Oppert JM, et al. Effectiveness of workplace interventions in Europe promoting healthy eating: a systematic review. Eur J Pub Health. 2012;22(5):677–82.
Ni Mhurchu C, Aston LM, Jebb SA. Effects of worksite health promotion interventions on employee diets: a systematic review. BMC Public Health. 2010;10:62.
Kuoppala J, Lamminpää A, Husman P. Work health promotion, job well-being, and sickness absences—a systematic review and Meta-analysis. J Occup Environ Med. 2008;50(11):1216–27.
Odeen M, Magnussen LH, Mæland S, Larun L, Eriksen HR, Tveito TH. Systematic review of active workplace interventions to reduce sickness absence. Occup Med. 2013;63(1):7–16.
CAS Google Scholar
Chapman LS. Meta-evaluation of worksite health promotion economic return studies: 2012 update. Am J Health Promot. 2012;26(4):1–12.
Bräunig D, Haupt J, Kohstall T, Kramer I, Pieper C, Schröer S. iga. Report 28: Wirksamkeit und Nutzen betrieblicher Prävention. Berlin: Initiative Gesundheit und Arbeit (iga); 2015.
Folkman S, Lazarus RS. An analysis of coping in a middle-aged community sample. J Health Soc Behav. 1980;21(3):219–39.
Folkman S. Personal control and stress and coping processes: a theoretical analysis. J Pers Soc Psychol. 1984;46(4):839–52.
Pinquart M, Silbereisen RK. Coping with increased uncertainty in the field of work and family life. Int J Stress Manag. 2008;15(3):209–21.
Richter A, Näswall K, De Cuyper N, Sverke M, De Witte H, Hellgren J. Coping with job insecurity: exploring effects on perceived health and organizational attitudes. Career Dev Int. 2013;18(5):484–502.
Kossek EE, Pichler S, Bodner T, Hammer LB. Workplace social support and work-family conflict: a meta-analysis clarifying the influence of general and work-family-specific supervisor and organizational support. Pers Psychol. 2011;64(2):289–313.
Burton J. WHO healthy workplace framework and model: background and supporting literature and practices. Geneva: World Health Organization; 2010.
Franzkowiak P. Prävention und Krankheitsprävention. In: Bundeszentale für gesundheitliche Aufklärung (BZgA), editor. Leitbegriffe der Prävention und Gesundheitsförderung. Köln: Bundeszentale für gesundheitliche Aufklärung (BZgA); 2011. p. 437–47.
Creswell JW, Poth CN. Qualitative inquiry and research design: choosing among five approaches: sage publications; 2016.
Mayring P. Qualitative Inhaltsanalyse [Qualitative Content Analysis]. Forum Qual Soc Res. 2000;1(2) Available online: http://nbn-resolving.de/urn:nbn:de:0114-fqs0002204 (Accessed on 25.11.2019).
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101.
VERBI Software Consult Sozialforschung GmbH. MAXQDA 12: Reference Manual: VERBI Software. Consult. Sozialforschung. GmbH; 2014. Available online: http://www.maxqda.com/download/manuals/MAX12_manual_eng.pdf (Accessed on 10.09.2019).
Tong A, Sainsbury P, Craig J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007;19(6):349–57.
Penley JA, Tomaka J, Wiebe JS. The Association of Coping to physical and psychological health outcomes: a Meta-analytic review. J Behav Med. 2002;25(6):551–603.
Stansfeld S, Candy B. Psychosocial work environment and mental health – a meta-analytic review. Scand J Work Environ Health. 2006;32:443–62.
Mowbray CT, Thrasher SP, Cohen E, Bybee D. Improving Social Work Practice with Persons Who are Homeless and Mentally Ill. J Sociol Soc Welf. 1996;23(4):3–24.
Waegemakers Schiff J, Lane AM. PTSD symptoms, vicarious traumatization, and burnout in front line Workers in the Homeless Sector. Commun Mental Health J. 2019;55(3):454–62.
Sundqvist J, Hansson J, Ghazinour M, Ogren K, Padyab M. Unaccompanied asylum-seeking refugee Children's forced repatriation: social Workers’ and police Officers’ health and job characteristics. Glob J Health Sci. 2015;7(6):215–25.
Robinson K. Supervision found wanting: experiences of health and social Workers in non-Government Organisations Working with refugees and asylum seekers. Practice. 2013;25(2):87–103.
Guest G, Bunce A, Johnson L. How many interviews are enough? An experiment with data saturation and variability. Field Methods. 2006;18(1):59–82.
van Nes F, Abma T, Jonsson H, Deeg D. Language differences in qualitative research: is meaning lost in translation? Eur J Ageing. 2010;7(4):313–6.
Malterud K. Qualitative research: standards, challenges, and guidelines. Lancet. 2001;358(9280):483–8.
Neupert P. Wohnungsnot im Wandel? Aktuelle Daten und Entwicklungen aus dem Dokumentationssystem zur Wohnungslosigkeit. wohnungslos. 2018;4:122–8.
Download references
Acknowledgements
We’d like to thank all institutions and employees who participated in the interviews. Moreover, we thank the students Gabriel David Westermann, Friederike Seemann, Jerrit Prill, and Lara Steinke for their support in the recruitment of interview participants and data transcription.
This research was funded by the Institution for Statutory Accident Insurance and Prevention in the Health and Welfare Services (BGW; non-profit organisation which is part of the German social security system), Hamburg, Germany. The funder had no role in the study design, data collection, data analysis and interpretation, preparation of the manuscript and decision to submit the paper for publication.
Author information
Authors and affiliations.
Institute for Occupational and Maritime Medicine, University Medical Centre Hamburg-Eppendorf, Seewartenstr. 10, 20459, Hamburg, Germany
Janika Mette, Volker Harth & Stefanie Mache
Competence Centre for Epidemiology and Health Services Research for Healthcare Professionals (CVcare), University Medical Centre Hamburg-Eppendorf, Martinistr. 42, 20246, Hamburg, Germany
Tanja Wirth & Albert Nienhaus
Department of Occupational Medicine, Hazardous Substances and Public Health, Institution for Statutory Accident Insurance and Prevention in the Health and Welfare Services (BGW), Pappelallee 33/35/37, 22089, Hamburg, Germany
Albert Nienhaus
You can also search for this author in PubMed Google Scholar
Contributions
JM, TW, AN, VH, and SM planned the study and study design. JM and TW carried out the qualitative study and analysed the data. JM, TW, and SM interpreted the data. JM drafted the manuscript. TW, AN, VH, and SM reviewed the manuscript and contributed substantially to its revision. All authors read and approved the final version of the manuscript.
Corresponding author
Correspondence to Stefanie Mache .
Ethics declarations
Ethics approval and consent to participate.
The study was approved by the Medical Ethics Committee of the Hamburg Medical Association, Germany (PV5652). Prior to data collection, participants were informed about the study aims and data confidentiality and signed a declaration of informed consent.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Additional file 1..
Relevant interview guideline questions.
Additional file 2.
COREQ-checklist.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/ . The Creative Commons Public Domain Dedication waiver ( http://creativecommons.org/publicdomain/zero/1.0/ ) applies to the data made available in this article, unless otherwise stated in a credit line to the data.
Reprints and permissions
About this article
Cite this article.
Mette, J., Wirth, T., Nienhaus, A. et al. “I need to take care of myself”: a qualitative study on coping strategies, support and health promotion for social workers serving refugees and homeless individuals. J Occup Med Toxicol 15 , 19 (2020). https://doi.org/10.1186/s12995-020-00270-3
Download citation
Received : 26 November 2019
Accepted : 18 June 2020
Published : 26 June 2020
DOI : https://doi.org/10.1186/s12995-020-00270-3
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Social work
Journal of Occupational Medicine and Toxicology
ISSN: 1745-6673
- General enquiries: [email protected]
The Science of Coping: 10+ Strategies & Skills (Incl. Wheel)

We all have trouble coping at some points in life. We don’t get the promotion we hoped for; our relationship breaks down; a presentation is overdue.
Whether you cope or not depends on how you think. Stress is a feeling of emotional or physical tension, and it arises from how you interpret life’s events as they unfold.
Our coping skills have evolved to help us survive in environments very different from those in which most of us now live, work, and play (Cosmides & Tooby, 2013). While we have a body and mind well adapted to overcome the challenges faced by hunters running down a kudu in the African savannah, we are a poor match for the difficulties found in modern life (Li, Vugt, & Colarelli, 2017).
Psychological research in the fields of sports, business, and beyond has identified approaches, skills, and tools that can help us cope, overcome, and even flourish.
The strategies that follow take us beyond a focus on repairing weaknesses and attending only to what is wrong, and instead view growth as default, mental wellbeing as expected, personal strengths to be built up, and an authentic existence to be lived.
Before you continue, we thought you might like to download our three Resilience Exercises for free . These engaging, science-based exercises will help you to effectively cope with difficult circumstances and give you the tools to improve the resilience of your clients, students, or employees.
This Article Contains:
A look at the coping wheel, 5 strategies for coping with stress, a real-life example, teaching coping to children: 3 ideas, 2 ways to cope with anxiety, how to cope with anger, 7 books on the topic, realizing resilience masterclass tools, a take-home message.
Coping strategies are processes used to manage stress. They help to control your thoughts, feelings, and actions before, during, and after challenging situations.
And there are plenty of them.
Research into coping has identified over 400 strategies and multiple classifications (Machado et al., 2020), including:
- Problem focused (proactively dealing with the source of the stress) versus emotion focused (reducing stress by regulating emotion)
- Approach (alleviating the problem directly) versus avoidance (distancing oneself from the stressor)
In an analysis of 44 studies, researchers found that coping strategies fit under 12 mutually exclusive coping families , represented in the diagram below (Skinner & Zimmer-Gembeck, 2007).
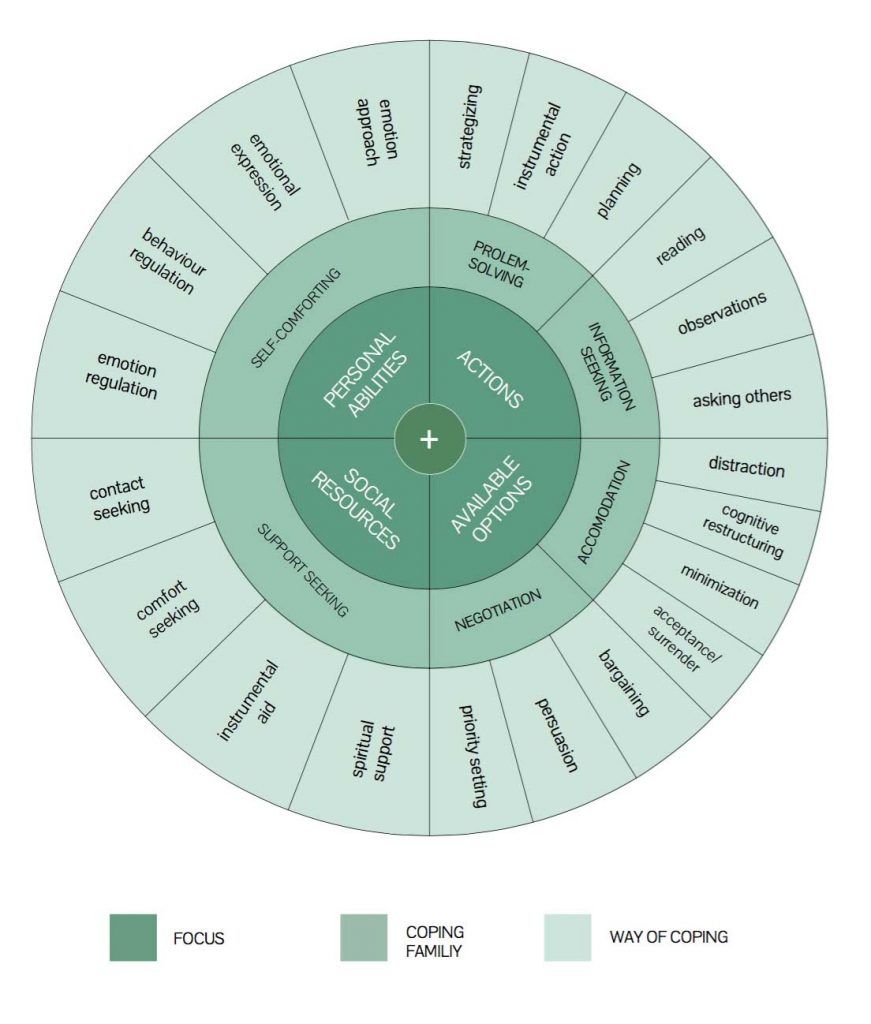
Source: The Positive Psychology Toolkit© (The Coping Strategy Wheels)
Techniques and strategies have a focus (e.g., actions, social resources), a coping family that shares the same action tendency (e.g., problem solving, negotiation), and a way of coping (e.g., surrender, emotion regulation).
Psychological stress arises in response to social and physical environments (Monroe & Slavich, 2016).
The stressor can be mild or intense: walking to the office on a hot day or traveling through the Kalahari Desert on foot, a pre-lunch rumbling stomach or failure of a vital food crop, an awkward conversation with a coworker or a hostage negotiation.
Such events cause a state of strain; impact our psychological and physical wellbeing; and vary in magnitude, timescale, and use of coping mechanisms.
The tools that follow can be adopted and adapted as needed to assist coping in difficult times, promoting growth, and supporting mental toughness and resilience .
They reframe a present or future situation, reduce or remove negative thoughts, or foster learning how to think positively.
1. ABCDE model
The ABCDE model, developed by Albert Ellis in the 1950s, provides a reflective framework. It supports us in changing our emotions and behaviors by identifying irrational beliefs and swapping them with rational ones.
Recognize, write down, and then challenge beliefs that are irrational or unhelpful.
| ABCDE model | |
|---|---|
| A – Adversity or Activating event | I didn’t do well in my math test today. |
| B – Recognize the irrational Belief | I’m useless. I can’t do anything right. |
| C – Recognize the Consequence | I give up and stop studying for the exam next week. |
| D – Dispute the irrational belief and turn it into a rational belief | I did well in the test last week. I’ve been studying well, but I hadn’t covered this topic yet. The results show me where I need to focus my attention. |
| E – Effect of the new rational belief | I sit down with my teacher to understand where I went wrong. We work on parts of the test I didn’t understand, and I include what I have learned in my future studying. |
The process of disputing irrational beliefs can lead to a more authentic, beneficial belief system. You may not have control over your environment, but you do have control over your reactions.
2. Positive thinking
Everything we know, believe, and feel is based on our internal thoughts. Positive thinking gives us extraordinary power over our thinking and ourselves (Strycharczyk & Clough, 2015).
Affirmations are used widely within sports. The repetition of short statements provides a way for the athlete to mirror the uplifting effects of hearing positive messages from a friend or coach.
Spend some time thinking about situations that you have faced or expect to encounter in the future. For each, write down a few short, supportive statements that provide strength during a challenge.
| Situation | Short, supportive statements |
|---|---|
| Interview | I have prepared well. I am looking forward to sharing my past successes. |
| Presenting | I’m confident and comfortable. I enjoy presenting and sharing my ideas. |
There is also growing evidence that the use of positive internal conversations, known as self-talk, can significantly improve how we tackle a challenge or approach a situation.
Talk to yourself as though a friend, coach, or supportive colleague is offering you positive advice.
| Situation | Suggested narrative |
|---|---|
| Difficult feedback at work | I will approach the meeting calmly and confidently, taking all the facts with me. |
| Running a marathon | I have trained for the last six months, and I am prepared for the distance. I am rested, and I have been eating well. I can do this. |
A good practice at the end of each day for positively reinforcing successful performance is to write down and review three achievements, small or large, from the last 24 hours.
This daily closure activity helps you focus on what went well, rather than dwelling on disappointments or perceived failures.
Use the achievements to take that positivity through to the next day.
| Name the achievement | Review the successes |
|---|---|
| Presentation | I nailed the presentation. I was ‘in the moment.’ The audience was engaged, and I received great feedback. |
| Time with family | I finished work early. My family and I went to the park and played. |
| Starting to write a book | I began writing a book today. It’s been on my mind for years. |
3. Visualization
It is common practice for athletes to use imagery while they prepare for an event, practice a movement, or train while injured. Swimmers mentally rehearse a perfect dolphin kick, and endurance runners imagine pulling extra miles from the depths of their mental and physical resources (Meijen, 2019; McCormick, Meijen, & Marcora, 2015).
Focusing on positive mental images can favorably impact both our mind and body and increase self-belief in our ability to cope with change.
The mind offers a safe and flexible environment for practicing a stressful task. Mentally rehearsing a daunting performance prepares the individual by asserting control over a (sometimes harmful) inner voice (Strycharczyk & Clough, 2015).
4. Control the controllable
Athletes often talk about controlling the controllable.
Adequate preparation will increase the perception of control, which is crucial to our mental toughness and motivation, and improve performance.
Write down a list of outcomes, real or imagined, to an important situation on sticky notes.
For example, when reviewing a challenging meeting:
- Did attendees arrive prepared?
- Were accurate notes and actions taken?
- Was the agenda followed and all points covered?
- Was everyone heard?
- Was agreement reached over the critical decisions?
Place each note on a large copy of the following graph:
- What went well goes at the bottom and less well, at the top.
- What can be controlled goes in the left-hand column and what cannot be controlled, in the right-hand column
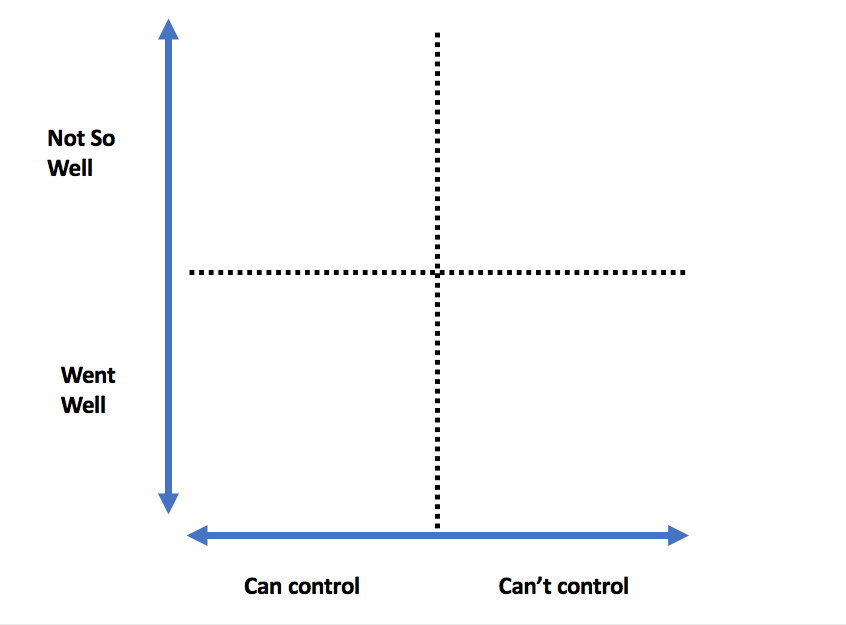
Review the completed graph.
Outcomes in the bottom-left quadrant – went well and can be controlled – require no action. Though it can be useful and increase self-belief to regularly review successes.
Outcomes in the top-left quadrant were within our control but unsuccessful. Ask yourself how you could have handled the situation better or differently. Once reviewed, consider how best to approach it next time, then let go of it. Do not dwell.
Anything on the right-hand side of the table is outside of our control. Revisit to confirm that it is still the case. Focus on what can be controlled and accept what cannot.
5. Three steps to handle stress
People who adopt the mindset that “stress is enhancing” experience more exceptional performance and less negative health symptoms (Crum & Crum, 2018).
If view positively, physical and mental stress are essential to moving from a fixed to a growth mindset.
Having worked with athletes and Navy SEALS, Crum and Crum (2018) propose a three-step approach to harnessing the positive aspects of stress while minimizing any negative health impacts.
Step one – “See your stress”
Don’t attempt to ignore stress. Label it.
Seeing it as something positive, rather than to be avoided, can change our physical, cognitive, and behavioral response to it.
See it, and label it: “ I am stressed because I haven’t completed the report yet.”
Step two – “Own it”
When you are at risk of being overwhelmed by stress, own it.
Own it: “ I recently got the promotion I wanted; this is part of my new role.”
Step three – “Use it”
Your body and mind have evolved to respond to stress; use that energy, alertness, and heightened concentration to boost your mind.
Use it: Be open to the opportunity. Use the stress to energize and motivate yourself.
Reframing stress to something positive can enable you to overcome existing and future obstacles (Crum & Crum, 2018).

Download 3 Free Resilience Exercises (PDF)
These detailed, science-based exercises will equip you or your clients to recover from personal challenges and turn setbacks into opportunities for growth.
Download 3 Free Resilience Tools Pack (PDF)
By filling out your name and email address below.
The following real-life example exemplifies the human capacity to cope. Csikszentmihalyi (2009) describes this ability as follows:
“the same stressful event might make one person utterly miserable, while another will bite the bullet and make the best of it.”
Against all odds
When Carmen’s estranged husband broke into her home, he beat her so severely that the police said it was more brutal than anything they had ever seen. Following the horrific injuries to her head, she remained in a coma for three months (Hooper, 2019).
When she regained consciousness and was finally able to get out of bed, she was in terrible pain, blind, and required multiple skin grafts. Surprisingly, rather than feeling sorry for herself, she realized she had been given a gift: the opportunity to help people.
Despite, as she describes it, “looking shocking,” she became a speaker and an inspiration to many.
And the story doesn’t end there. The tight skin grafts on Carmen’s face continued to cause her immense pain, and she became only the seventh person to have a face transplant. To give further insight into her character, she connected and struck up a close friendship with the daughter of the donor. They now see each other regularly.
Carmen’s story of resilience is incredible. Not only did she survive injuries she could have died from, but she overcame the challenges to flourish in her new life.

He has worked closely with British Olympic athletes and supported British Cycling in their considerable successes.
His bestseller, The Chimp Paradox , explains the inner workings of the brain using what he describes as the “Chimp Model.” It consists of three elements: the human, the chimp, and the computer.
The human – you – uses a logical and rational approach to solving problems. The chimp represents the fast-reacting, instinctual parts of the brain. It interprets information emotionally and often responds impulsively, frequently causing us problems.
The final element, the computer , stores previous experiences and uses them to advise the human and the chimp. It represents your memory and a set of learned, automatic responses.
In My Hidden Chimp: Helping Children to Understand and Manage Their Emotions, Thinking, and Behaviour With Ten Helpful Habits , Peters and Battista (2018) use the same model to help children develop healthy habits for life.
Understanding when the chimp tries to take over
| Situation: | Not eating healthily |
|---|---|
| Your ‘human’ thoughts: | The chimp’s thoughts: |
| I want to eat good food to make me strong and healthy. | I don’t care; I like cake and candy. |
| Situation: | I don’t want to do homework |
|---|---|
| Your ‘human’ thoughts: | The chimp’s thoughts: |
| I like school, and I am good at my lessons. | I’m watching TV; I don’t want to read. |
Identify words that describe you and your chimp
| Words to choose from | Words that describe you when the chimp doesn’t take over | Words that describe the chimp (some will match words that describe you) |
|---|---|---|
| Worried, playful, calm sad, busy, confident, funny, happy, grumpy, mean, bossy | Happy, confident, sensible, loving, helpful, funny | Grumpy, happy, naughty, sad, funny, mean, bossy |
Trying new things
Sometimes we get scared to try new things.
Can you think of three things you would say to your friend’s chimp to help it try something new?
Encourage the chimp to try something new:
- If you try something new, you might enjoy it.
- Something new could be fun, and you could share it with friends.
- You could become more confident if you try new things.
Working through each of the above examples, with or without an adult, can help the child understand their feelings better and identify when the chimp tries to take over.

World’s Largest Positive Psychology Resource
The Positive Psychology Toolkit© is a groundbreaking practitioner resource containing over 500 science-based exercises , activities, interventions, questionnaires, and assessments created by experts using the latest positive psychology research.
Updated monthly. 100% Science-based.
“The best positive psychology resource out there!” — Emiliya Zhivotovskaya , Flourishing Center CEO
Psychological research has proven the importance of relaxation as an effective technique for managing anxiety. As psychology has confirmed, we can influence our minds by taking control of our bodies (Strycharczyk & Clough, 2015).
Exercises for managing anxiety include the following.
1. Controlled distraction
Similar to self-talk, controlled distraction reduces anxiety by redirecting attention away from a negative situation.
When a quick fix is required, take your mind off your anxiety by focusing on something that doesn’t cause you upset.
For example, before giving a presentation, count lights or ceiling tiles, listen to music, or imagine a past or future vacation.
2. The Laura Mitchell Relaxation Method
The Mitchell Relaxation Method (Mitchell, 1990) has been around for decades but remains a successful and widely used treatment for patients with anxiety.
The client is asked to ‘pull’ each muscle group in turn, stopping in between; for example, ‘pull your shoulders toward your feet,’ ‘stretch out your fingers and thumbs.’ They must remain mindful of their body position, breathing, muscles, joints, and skin.

The initial rush of adrenaline leads to physical indicators that you may become aware of before you spot emotional changes: increased heart rate, faster breathing, tension, and a clenched jaw and fists.
Simple techniques can quickly be adopted and buy extra thinking time: a short walk, counting to 10, or talking to a friend for independent advice.
Breathing techniques can also help you to find calm and reduce escalating feelings.
Box breathing is practical and easy to learn. Imagining each side of a box, breathe in (side 1), hold (side 2), breathe out (side 3), and hold (side 4). Each side should last approximately four seconds.
Exercise, distraction, and mindfulness are other positive ways to handle tension or release anger.
To learn more about coping, mental toughness, resilience, and our evolutionary background, check out these 7 books available on Amazon:
- On Mental Toughness by Harvard Business Review ( Amazon )
- Mindset: Changing the Way You Think to Fulfill Your Potential by Carol Dweck ( Amazon )
- Positivity: Groundbreaking Research to Release Your Inner Optimist and Thrive by Barbara Fredrickson ( Amazon )
- Evolutionary Psychology: The New Science of the Mind by David Buss ( Amazon )
- The Chimp Paradox: The Mind Management Program to Help You Achieve Success, Confidence, and Happiness by Dr. Steve Peters ( Amazon )
- Self-Determination Theory: Basic psychological needs in motivation, development, and wellness by Richard Ryan and Edward Deci ( Amazon )
- Developing Mental Toughness: Coaching Strategies to Improve Performance, Resilience, and Wellbeing by Doug Strycharczyk and Peter Clough ( Amazon )

17 Tools To Build Resilience and Coping Skills
Empower others with the skills to manage and learn from inevitable life challenges using these 17 Resilience & Coping Exercises [PDF] , so you can increase their ability to thrive.
Created by Experts. 100% Science-based.
The Realizing Resilience – Coaching Masterclass is an excellent resource for practitioners. Teach your clients how to become more resilient and mentally tough with the science-based techniques and tools in this online masterclass.
If you’re looking for more science-based ways to help others overcome adversity, this collection contains 17 validated resilience tools for practitioners . Use them to help others recover from personal challenges and turn setbacks into opportunities for growth.
The human mind is impressive. It has evolved the potential to solve complex problems and successfully manage unexpected and novel situations.
And yet, coping is less about what is happening in the world, and more about how our minds interpret the situation. Perception is everything. This is why coping mechanisms focus on managing, reframing, or avoiding how we perceive the stressors.
If we can see stress not as something to be shied away from, but rather an opportunity to embrace, we can live a more complete, authentic life. After all, although evolution has shaped our minds and bodies, we are free to choose how we react and behave.
While we often lack control of our environment, we decide what affects us and how we respond.
It is not possible and would not be enjoyable to live a life without stress. Overcoming the challenges, pitfalls, and failures in life are just as crucial as celebrating the wins and enjoying happy outcomes. Stress is a valuable force for growth.
However, if our inability to cope is getting in the way of living a full life, achieving what we want, or causing damage to others, then we must adopt and adapt the tools that work best to overcome the situation and flourish.
Thank you for reading.
We hope you enjoyed reading this article. Don’t forget to download our three Resilience Exercises for free .
- Buss, D. (2014). Evolutionary psychology: The new science of the mind (5th ed.). Psychology Press.
- Cosmides, L., & Tooby, J. (2013). Evolutionary psychology: New perspectives on cognition and motivation. Annual Review of Psychology , 64 (1), 201–229.
- Crum, A., & Crum, T. (2018). Stress can be a good thing if you know how to use it. In Harvard Business Review, HBR’s 10 must-reads: On mental toughness . Harvard Business Review Press.
- Csikszentmihalyi, M. (2009). Flow: The psychology of optimal experience. Harper Row.
- Dweck, C. S. (2017). Mindset : Changing the way you think to fulfill your potential (6th ed.). Robinson.
- Fredrickson, B. (2010). Positivity: Groundbreaking research to release your inner optimist and thrive . Oneworld Publications.
- Hooper, R. (2019). Superhuman: Life at the extremes of mental and physical ability. Abacus.
- Li, N. P., Vugt, M. V., & Colarelli, S. M. (2017). The evolutionary mismatch hypothesis: Implications for psychological science. Current Directions in Psychological Science , 27 (1), 38–44.
- Machado, A. V., Volchan, E., Figueira, I., Aguiar, C., Xavier, M., Souza, G. G., … Mocaiber, I. (2020). Association between habitual use of coping strategies and posttraumatic stress symptoms in a non-clinical sample of college students: A Bayesian approach. PloS One, 15 (2).
- McCormick, A., Meijen, C., & Marcora, S. (2018). Effects of a motivational self-talk intervention for endurance athletes completing an ultramarathon. The Sport Psychologist , 32 (1), 42–50.
- Meijen, C. (2019). Endurance performance in sport: psychological theory and interventions. Routledge.
- Mitchell, L. (1990). Simple relaxation: The Mitchell method of physiological relaxation for easing tension. Murray.
- Monroe, S. M., & Slavich, G. M. (2016). Psychological stressors: Overview. In G. Fink (Ed.), Stress: Concepts, cognition, emotion, and behavior: Handbook in stress series (vol. 1) (pp. 109–115). Academic Press.
- Peters, S. (2016). The chimp paradox: The mind management program to help you achieve success, confidence, and happiness . Vermilion.
- Peters, S., (Author) & Battista, J. (Illustrator) (2018). My hidden chimp: Helping children to understand and manage their emotions, thinking, and behaviour with ten helpful habits. Studio Press Books.
- Ryan, R. M., & Deci, E. L. (2018). Self-determination theory: Basic psychological needs in motivation, development, and wellness. Guilford Press.
- Skinner, E. A., & Zimmer-Gembeck, M. J. (2007). The development of coping. Annual Review of Psychology , 58 , 119–144.
- Strycharczyk, D., & Clough, P. (2015). Developing mental toughness: Coaching strategies to improve performance, resilience, and wellbeing. Kogan Page.
Share this article:
Article feedback
What our readers think.
Hello, Are there teaching materials available in other languages? I have a few Spanish speakers that would benefit greatly from having the literature written in Spanish.
Hi there Carole,
Thanks for your question! As of now, we only offer our Masterclasses and manuals in English. However, many past customers have translated our teaching materials into multiple different languages so they can use it in their practices in their home countries 🙂
I hope this helps!
Kind regards, -Caroline | Community Manager
Dear Jeremy,
Thoroughly enjoyed reading the above with regards to coping methods. I am very sorry if this is irrelevant, however, which human suject Phd is related to this as I am really interested in taking on my studying further but failing in finding a good subject . Thank you and best regards
Let us know your thoughts Cancel reply
Your email address will not be published.
Save my name, email, and website in this browser for the next time I comment.
Related articles

Overcoming Trauma Bonding: 8 Strategies & Exercises
A young woman tries to save her father from a monster in a castle by sacrificing herself as a captive instead. She becomes his prisoner. [...]

Breaking Generational Trauma With Positive Psychology
Generational trauma, the enduring legacy of past adversities that reverberates through familial lines, presents profound challenges to mental and emotional wellbeing. Within the realm of [...]

Vicarious Trauma: The Silent Impact on Therapists
Vicarious trauma refers to the impact of repetitive encounters with indirect trauma while working as a helping professional. Most clients who attend psychotherapy will share [...]
Read other articles by their category
- Body & Brain (52)
- Coaching & Application (39)
- Compassion (23)
- Counseling (40)
- Emotional Intelligence (22)
- Gratitude (18)
- Grief & Bereavement (18)
- Happiness & SWB (40)
- Meaning & Values (26)
- Meditation (16)
- Mindfulness (40)
- Motivation & Goals (41)
- Optimism & Mindset (29)
- Positive CBT (28)
- Positive Communication (23)
- Positive Education (37)
- Positive Emotions (32)
- Positive Leadership (16)
- Positive Parenting (14)
- Positive Psychology (21)
- Positive Workplace (35)
- Productivity (16)
- Relationships (46)
- Resilience & Coping (39)
- Self Awareness (20)
- Self Esteem (37)
- Strengths & Virtues (29)
- Stress & Burnout Prevention (33)
- Theory & Books (42)
- Therapy Exercises (37)
- Types of Therapy (54)
3 Resilience Exercises Pack
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- Medicina (Kaunas)

Coping Strategies of Healthcare Professionals with Burnout Syndrome: A Systematic Review
Background and Objectives: To evaluate the efficacy of coping strategies used to reduce burnout syndrome in healthcare workers teams. Materials and Methods: We used PubMed and Web of Science, including scientific articles and other studies for additional citations. Only 7 of 906 publications have the appropriate inclusion criteria and were selected. A PRISMA 2020 flow diagram was used. Results: The most common coping strategies that the literature studies showed were efficient, in particular social and emotional support, physical activity, physical self-care, emotional and physical distancing from work. Coping mechanisms associated with less burnout were also physical well-being, clinical variety, setting boundaries, transcendental, passion for one’s work, realistic expectations, remembering patients and organizational activities. Furthermore, it was helpful to listen to the team’s needs and preferences about some types of training. Conclusion: We suppose that the appropriate coping strategies employed in the team could be useful also in the prevention of psychological suffering, especially in contexts where working conditions are stressful. Studies about coping strategies to face burnout syndrome in healthcare workers should be increased.
1. Introduction
Burnout syndrome has been defined as a chronic response to stress in the workplace [ 1 ] characterized by a physical, mental and emotional state of exhaustion [ 2 ] that reduces the sense of personal and professional fulfillment [ 3 ]. Risk factors could be conflicts and financial problems at work, work overload, communication or organization problems [ 4 ]. Some professions are more susceptible than others, and in particular, we focused on studies about healthcare workers that are in daily contact with the seriously ill, such as doctors, nurses and social workers [ 5 ]. Howlett et al., [ 6 ] highlighted high levels of burnout among the emergency department staff (32.1% suffered from emotional exhaustion), in particular among doctors (46%) which had a high-medium score in burnout scales, and nurses that reported unpleasant contacts with supervisors (they had a high score in burnout scales). Concerns relating to burnout, especially in recent years, have developed a growing interest among mental health scholars. In fact, an important study was recently conducted in Italy that aimed to examine personal resources and psychological symptoms associated with burnout in 933 healthcare workers during the COVID-19 epidemic period. Sociodemographic and occupational data were investigated; depression, anxiety, burnout, and posttraumatic symptoms, as well as psychological well-being, were cross-sectionally assessed using a questionnaire. Results showed a particular incidence of depression (57.9%), anxiety (65.2%), post-traumatic symptoms (55%), and burnout (25.61%) [ 7 ]. This syndrome is considered as a multidimensional problem because of a series of symptoms such as depersonalization, anxiety, lack of motivation, mental fatigue, lack of personal and professional achievement, that influence worker and patient’s wellness [ 5 ], but it is important to highlight that each person could face problems in different ways. Ding et al., [ 3 ] studied the relation between subjective coping and burnout syndrome. Imported findings found significant correlations between emotional exhaustion and emotional and dysfunctional coping, as well as depersonalization and dysfunctional coping Dix, D.M. [ 8 ]. The relationship between coping strategies and burnout for caregivers of judged youth. Dysfunctional coping was a significant predictor of burnout [ 8 ]. Coping mechanisms are a necessity when dealing with stress and its accompanying stressors. Lazarus and Folkman (1987) classified coping modes as problem-based and emotion-based [ 9 ]. Some studies showed the problem-solving approach as the most common coping behavior for health students while the avoidance approach was the least used for coping behaviors in nursing students [ 10 , 11 , 12 , 13 , 14 , 15 , 16 ]. Problem-based coping modes are known to be beneficial to students’ learning, clinical performance, and well-being, whereas emotion-based coping modes were found to be detrimental to their health [ 17 , 18 ]. Coping mechanisms and job satisfaction were shown to be associated with the incidence of burnout symptoms in a work setting, according to available literature [ 19 ]. There are many differences in job satisfaction between different types of ICUs that are related to patient diagnosis and nursing management [ 19 ]. Often the duties and responsibilities of health care workers are not harmonized with the possibilities of the workplace, and training for new tasks is often insufficient [ 20 ]. Coping is defined as cognitive and behavioral efforts to manage specific internal and/or external demands that are assessed as taxing or exceeding the person’s resources [ 21 ]. A person will be psychologically vulnerable to a particular situation if he or she does not have sufficient coping resources to manage it adequately and places great importance on the threat implicit in the consequences of this inadequate management. Several ways in stress management can be considered, such as cognitive or behavioral coping, cognitive or behavioral avoidance, emotion-focused coping, or substance use [ 22 , 23 ]. From this perspective, burnout can be observed as a progressively developed condition that results from the use of ineffective coping strategies by which professionals attempt to protect themselves from work-related stressful situations [ 24 ]. In recent years, the psychological distress and stress of health workers have been studied with interest and attention, with the intent of defining the causes, as well as the causes of stress, have been studied with interest and attention, with the aim of defining the causes, as well as the consequences on a care, organizational and individual level [ 25 ]. If, as previously reported, being close to patients is gratifying because it offers the possibility to express different feelings, it is also true that working in hospital wards is extremely demanding and tiring [ 26 ]. The quality of the life of healthcare workers is particularly affected by the evident relational asymmetry that is established between the doctor and the patient [ 27 ]. Taking care of the suffering of others in increasingly complex organizational contexts, which imply ever-increasing demands for assistance, can induce health workers to raise real defensive barriers against the patient, which leads to extinguishing the flame of passion that animates the doctor and ignites the risk of stress and related pathologies, such as burnout [ 28 ]. The aim of this review is to investigate the personal coping strategies of healthcare workers that may have consequent mental health conditions such as burnout syndrome.
We follow the guidelines for the selection of the studies that we identified from each database or register searched (rather than the total number across all databases/registers).
2. Materials and Methods
We conducted a narrative review to investigate the efficacy of coping strategies used by healthcare workers to reduce burnout symptoms. Literature studies were performed in accordance to the PRISMA (Preferred Reporting Items for Systematic Reviews and Meta-Analyses) guidelines by searching on PubMed and Web of Science and registered to PROSPERO (ID 312225). We considered the articles from 2008 to 2021. The search combined the following terms: “burnout healthcare professional hospital coping” (all field). There was a total of 844 articles identified via PubMed ( Figure 1 ) and 22 articles from Web of Science. All articles were evaluated by title, abstract, full-text and specificity of the topic ( Figure 1 ). The duplicates were removed, we considered articles that focused on coping strategies of healthcare workers in hospital context.

PRISMA 2020 flow diagram of evaluated studies.
We identified 906 studies and seven were selected ( Figure 1 ). All articles conducted research on 1006 healthcare workers with a diagnosis of Burnout Syndrome and investigated the efficacy of coping strategies ( Table 1 ). In particular, the first article highlighted those medical residents who reported low depersonalization, high personal accomplishment, high satisfaction with medicine and high emotional exhaustion after coping strategies, especially social support and entertainment. Koh et al. [ 29 ], in their second article, identified coping mechanisms associated with less burnout: physical well-being, clinical variety, setting boundaries, transcendental (meditation and quiet reflection), passion for one’s work, realistic expectations, remembering patients and organizational activities. In their study, Whitebird et al., [ 30 ] noted that staff, to manage stress, use physical activity and social support so they could reduce burnout. Mehta et al., [ 31 ] evaluated the efficacy of the Relaxation Response Resiliency Program for Palliative Care Clinicians, with positive results (reductions in perceived stress and improvements in perspective-taking). The last article investigated common stressors, coping strategies, and training needs among Palliative Care Clinicians to develop a targeted Resiliency Program. Perez et al., [ 32 ] identified three main areas of stressors and coping strategies such as physical self-care, emotional and physical distancing, social and emotional support. Furthermore, the team expressed some needs and preferences: mind–body skills training, cognitive skills, stress education, brief strategies to implement in real-time, enhancing resilience. Two different measures of burnout were identified ( Table 2 ).
Studies assessing Burnout Syndrome and coping strategies.
| References | Aim of the Study | Measures | Socio-Demographic Characteristics | Outcomes |
|---|---|---|---|---|
| [ ] | To show the experiences of stress and burnout and sociodemographic factors associated with dimensions of stress among medical residents | Demographic questions, abbreviated Maslach Inventory, 4 open-ended questions on experiences with stress | 136 medical residents (92 man, 44 women) | They responded to the survey, listing an average of 2.2 types of stressors (workload and workplace relationships were the most frequent). They listed an average of 3.1 coping strategies, especially social support and entertainment. Responses indicated low depersonalization, high personal accomplishment, high satisfaction with medicine and high emotional exhaustion |
| [ ] | To estimate the prevalence of burnout and psychological morbidity among palliative care practitioners and its associations with demographic/workplace factors, and with the use of coping mechanisms | Maslach Burnout Inventory –Human Services Survey (MBI-HSS), 12-items General Health Questionnaire (GHQ12) | 293 participants (45 Male, 226 women). Age: 20–29 years = 59; 30–39 years= 99; 40–49 years = 67; 50+ years = 44. Profession: 74 Doctors, 156 Nurses, 37 Social worker | The prevalence of burnout among respondents was 91 of 273 (33.3%); psychological morbidity was 77 (28.2%); Home hospice care practitioners (41.5%) were more at risk of developing psychological morbidity. Coping mechanisms associated with less burnout were: physical well-being, clinical variety, setting boundaries, transcendental (meditation and quiet reflection), passion for one’s work, realistic expectations, remembering patients and organizational activities |
| [ ] | To understand how stress affected mental health (in terms of burnout and compassion fatigue) in hospice workers and how they faced these problems | ShortForm12 Health Survey Version 2 (SF-12), Short-form version of the Short-Form 36 Health Survey (SF-36), Generalized Anxiety Disorder (GAD-7) Scale, Patient Health Questionnaire 8 (PHQ8), Professional Quality of Life Assessment R-III Scale (ProQOL-RIII), Short-form version of the Medical Outcomes Social Support Survey (MOS) | 547 participants (8% Male, 92% women); Professions: Registered nurses or nurses Practitioners, licensed practical nurses, social workers, home health aides, management/administrative, chaplains/bereavements, volunteer coordinators/others | Hospice staff showed high levels of stress and a small but significant proportion reported moderate to severe symptoms of depression, anxiety, compassion fatigue, and burnout. Staff managed stress through physical activity and social support. These strategies could help decrease staff burnout. |
| [ ] | To evaluate the feasibility of the Relaxation Response Resiliency Program for Palliative Care Clinicians (with the aim of decreasing stress and increasing resiliency) | Perceived Stress Scale, Positive and Negative Affect Schedule, Interpersonal Reactivity Index (IRI), Life Orientation TesteRevised, Satisfaction with Life Scale, General Self-Efficacy Scale | 15 participants (3 male, 12 women); Professions: 6 Physicians, 6 Nurses Practitioner Clinical, 2 Social workers, 1 Registered nurse | The intervention was functional. Participants reported reductions in perceived stress and improvements in perspective-taking |
| [ ] | To investigate common stressors, coping strategies, and training needs among Palliative Care Clinicians with the aim of developing a targeted Resiliency Program | Semi-structured interview guide with open-ended questions | 15 participants (3 male, 12 women); Professions: 6 Physicians, 6 Nurses Practitioner Clinical, 2 Social workers, 1 Registered nurse | Three main areas of stressors highlighted: challenges related to managing large emotionally demanding caseloads within time constraints; patient factors; personal challenges of delineating emotional and professional boundaries. Coping strategies: physical self-care (i.e., diet, physical activity, sleep, hobbies), emotional and physical distancing, social and emotional support. Training needs and preferences: mind-body skills training, cognitive skills, stress education, brief strategies to implement in real-time, enhancing resilience |
| [ ] | To investigate the effects of coping strategies on the relationship between work stress and job performance for health workers in China | Chinese Nurse Job Stressors Questionnaire | A cross-sectional survey of 852 nurses from four tertiary hospitals in Heilongjiang Province | Positive coping strategies reduce or buffer the negative effects of work stress on job performance and negative coping strategies increased the negative effects. |
| [ ] | To examine correlation between the intensity of Burnout Syndrome and physicians’ personality traits as well as between the level of Burnout Syndrome and stress coping strategies. | Maslach Burnout Inventory, The Temperament and Character Inventory and Manual for the Ways of Coping Questionnaire. | The sample consisted of 160 physicians (70 general practitioners, 50 psychiatrists, 40 surgeons) | Burnout Syndrome affects personal well-being and professional performance. |
Burnout measures.
| Burnout Scale | Domains | Items | Scales | Focus |
|---|---|---|---|---|
| Abbreviated Maslach Burnout Inventory (Maslach C., Jackson S.E. 1981) | Emotional exhaustion; Depersonalization; Personal accomplishment. | 9 items | 7-point scale | |
| Maslach Burnout Inventory—Human Services Survey (MBI-HSS) (Maslach C., Jackson S.E. 1981) | Emotional exhaustion; Depersonalization; Personal accomplishment | 22 items | 7-point scale | To assess an individual’s experience of burnout |
Recent studies found a significant correlation between burnout and other variables such as task-focused coping and job satisfaction. Research conducted by Li et al. found that age was positively associated with task-focused coping, job satisfaction, and personal accomplishment, and negatively with secondary traumatic stress, emotional exhaustion, and depersonalization. A very interesting study was conducted with 1027 participants in China, exploring the relationship between coping strategies and job stress [ 33 ]. The authors used the Job Performance Scale, the Work Stress Scale, and the Coping Strategies Scale. They determined that the investigated population of healthcare workers employed more positive coping strategies than negative coping strategies and that positive coping strategies mediated the relationship between patient care and job satisfaction, whereas negative strategies moderated the relationship between workload and job performance. Pejuskovic et al. [ 34 ] used the Maslach Burnout Inventory and the Ways of Coping scale to assess physicians in Serbia; physicians were also found to be exposed to burnout. These results showed that coping strategies are very important in the development of burnout.
4. Discussion
The results of this review, although limited to a few articles in the scientific literature, unlike other studies on this topic, have shown that in work contexts where roles, functions and boundaries are well defined, the mental health of workers is less at risk of developing burnout. It is also important to emphasize that coping strategies, in addition to being influenced by purely personal factors, may also be favored by the work context. Future research should further focus attention on the work climate by promoting individual coping as a resource of the workgroup. Welbourne et al. [ 35 ] examined the contribution of occupational attribution style to the use of various coping strategies. Results indicated that the relationship between occupational attribution style and satisfaction was mediated by the use of problem-solving/cognitive restructuring and avoidance strategies to cope with workplace stress. Gracia-Gracia et al. [ 36 ] presented results of a correlation between burnout and mindfulness self-compassion in intensive care units. The results of this study showed that the level of burnout is inversely related to their level of self-compassion [ 36 ]. A great part of the literature studies focused on the study of burnout and coping strategies in specific healthcare professions (nurses or doctors or social workers).
Healthcare workers often have to face a stressful working environment, especially when they are dealing with the seriously ill and have more responsibilities [ 4 ], so this category is particularly at risk of burnout syndrome. However, burnout symptoms seem to be generated principally from systematic and dysfunctional habits and from individual psychological reactions that damage personal wellness, especially emotional exhaustion, depersonalization and reduced personal accomplishment [ 37 ]. Instead of implementing his resources to face stressful situations, a worker could react in an “explosive” way (aggressiveness, irritability, attitudes of hostility and resentment), or “implosively” (consequent frustration, chronic anxiety or severe depression). These symptoms could worsen relationships with colleagues and even patients.
In this review, we focused on coping strategies most commonly used to face burnout symptoms in a group context. Although many studies showed personalized multidimensional interventions, the basis of a collaborative climate seems to be a good organization. Sometimes the difficulty could be the lack of habit in teamwork. It might be useful to establish a clear definition of workers’ roles and responsibilities [ 38 ], enhancing individual technical competencies. However, only the organization of work is not sufficient. According to Lee et al., [ 37 ] a better emotional awareness helped people to feel, understand and express their feelings, thus improving communication. We think that a greater emotional intelligence (the ability to understand the causes of emotions) could help to distinguish subjective and objective problems. Shah et al., [ 39 ] highlighted the positive impact of support groups where all staff could meet and discuss the emotional aspects of work, cultivating a sense of “shared understanding”, because a common problem was often the lack or poor communication between colleagues and superiors. Healthcare workers, engaging in self-awareness, regulating emotions, recognizing mistakes and expressing their doubts, could improve empathy and help others. In this way, each worker also could realize that he is not “alone” in the management of stressful situations.
It might be useful to acquire knowledge of appropriate management strategies [ 39 ]. For this purpose, in their study, Perez et al., [ 32 ] showed that workers spontaneously proposed different solutions, for example, training in mind–body skills, including relaxation exercises such as meditation, breathing, mindfulness group mantra, or yoga; cognitive skills, for example, understanding how to utilize cognitive reframing and strategies to help reduce ruminative thoughts and negative self-talk; a program about stress education that offered information about the physiology of stress and the long-term impact on the body and mind (in this way it was possible to provide a link between physiological signals and distressing thoughts); brief strategies to implement in real-time, such as techniques that helped to organize the day even when the time was limited; learning skills to enhance resilience that would allow them to effectively manage their chronic exposure to stress, improving the care and the relations with patients. This training could be a functional intervention where practice and feedback are essential to produce positive behavioral effects. Furthermore, Perez et al., [ 32 ] suggested extending these strategies outside the work environment, and also creating personal spaces for physical self-care, useful for emotional and physical distancing. During challenging periods, some workers expressed the need to briefly disengage from their work to regain composure and preserve psychological equilibrium. For example, they opted to gain physical distancing or simply seek a “time-out” asking for rest periods. In this way, they could spend time on their hobbies, practicing physical activity and taking care of their body, for example, with an adequate nutritional education.
5. Conclusions
Considering the findings in all these studies, coping mechanisms have a great influence on the occurrence of burnout, and burnout is highly associated as a significant problem in healthcare institutions. Furthermore, we suggest deepening studies where the healthcare worker’s team is the beneficiary of the appropriate coping strategies, considering that the group could be an important resource to promote collective wellness. Future research should focus further attention on the work climate by making individual coping a resource of the work group.
Author Contributions
Conceptualization, V.L.B. and G.M.; methodology, F.C.; data curation, G.C.; writing—original draft preparation, C.F.; writing—review and editing, V.L.B.; supervision, F.C. All authors have read and agreed to the published version of the manuscript.
This research received no external funding.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Conflicts of interest.
The authors declare no conflict of interest.
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
- Bipolar Disorder
- Therapy Center
- When To See a Therapist
- Types of Therapy
- Best Online Therapy
- Best Couples Therapy
- Managing Stress
- Sleep and Dreaming
- Understanding Emotions
- Self-Improvement
- Healthy Relationships
- Student Resources
- Personality Types
- Sweepstakes
- Guided Meditations
- Verywell Mind Insights
- 2024 Verywell Mind 25
- Mental Health in the Classroom
- Editorial Process
- Meet Our Review Board
- Crisis Support
Coping Strategies for Stress
From Meditation to Journaling, Try These Effective Ways to Manage Stress
Siri Berting / Blend Images / Getty Images
- Calming Strategies
- Emotional Strategies
- Solution-Oriented Strategies
- When to Seek Help
The American Psychological Association's 2022 "Stress in America" report reveals that, on a scale of one to 10, the average American has a stress level around a five. However, more than one in four survey respondents also indicated that on most days, their stress was so high that they were unable to function.
Although survey results tend to fluctuate a little each year, the findings generally show the same pattern. People face a variety of stressors , which also means that they need to find effective ways to relieve stress in their lives. With that in mind, here are a few proven coping strategies for stress.
Get Help Now
We've tried, tested, and written unbiased reviews of the best online therapy programs including Talkspace, BetterHelp, and ReGain. Find out which option is the best for you.
Calming Coping Strategies for Stress
Calming our physiology can help reverse the stress response . When our stress response is triggered, we process information differently and can feel physically and emotionally taxed. If this state is prolonged, it can escalate to chronic stress.
One way to calm our bodies, therefore also calming our minds, is to go to a quiet place and take deep, long breaths. Breathe in, hold for five seconds, then exhale slowly. Repeat several times. This breathing exercise can help soothe our nerves and slow a racing heart.
Other calming strategies include:
- Engaging in aromatherapy
- Listening to soothing music
- Practicing mindfulness meditation
- Progressive muscle relaxation
Emotion-Focused Coping Strategies for Stress
With emotion-focused coping strategies, the situation doesn’t change but our perception of it does. These strategies are great to use when we have little ability to control what happens. They help us see stressors as a challenge instead of a threat.
Research has found that maintaining a sense of humor can help people better cope with stress. Another helpful strategy is to stay optimistic. Cultivating optimism works by reducing our rates of perceived stress while also increasing our resilience.
Other emotion-focused techniques for coping with stress include:
- Journaling our emotions
- Practicing loving-kindness meditation to increase self-compassion
- Using visualization strategies to increase positive feelings
While these techniques can be time-consuming, reducing stress is necessary to improve our well-being and mental and physical health.
Solution-Focused Coping Strategies for Stress
Sometimes there’s nothing we can do to change a situation, but often we can find an opportunity to take action and change the circumstances we face. Solution-focused coping strategies can be very effective for stress relief.
Often a small change is all that’s required to make a huge shift in how we feel. One change can lead to other changes, creating a chain reaction of positive change in which opportunities open up and life changes significantly. Also, once an action is taken, the sense of being trapped with no options —a recipe for stress—can dissipate quickly.
It’s important to be thoughtful about which actions to take, as each situation may call for a unique solution. A less-stressed mind can more easily choose the most beneficial course of action.
Solution-focused techniques good for reducing workplace stress but that can also be beneficial in other situations include:
- Implementing time-management strategies when feeling overwhelmed by a busy schedule
- Reaching out to others for help, such as contacting human resources (HR) if work demands feel overwhelming or if being harassed
- Using conflict-resolution strategies to mitigate the stress, whether with co-workers or in a relationship
When to Seek Help for Stress
Through coping strategies and good self-care , we can manage our stress healthfully and avoid long-term issues. However, if stress levels do not decrease, it may be a good idea to talk to a therapist or primary healthcare provider.
This type of professional can help identify ways to minimize stress. They can also assist by developing healthy eating plans and exercise programs to help us maintain our health while handling all our other obligations.
Get Advice From The Verywell Mind Podcast
Hosted by therapist Amy Morin, LCSW, this episode of The Verywell Mind Podcast shares how you can change your mindset to cope with stress in a healthy way.
Follow Now : Apple Podcasts / Spotify / Google Podcasts
Everyone has stress in their lives, and stress levels vary depending on the day. Having healthy coping strategies in place can help us keep stress at a manageable level . If, however, we are struggling to manage our stress, it's important to seek professional help. A mental health provider can help us learn how to manage stress in a healthy way.
American Psychological Association. Stress in America 2022 .
Harvard Health Publishing. Take steps to prevent or reverse stress-related health problems .
Perciavalle V, Blandini M, Fecarotta P, et al. The role of deep breathing on stress . Neurol Sci . 2017;38(3):451-458. doi:10.1007/s10072-016-2790-8
Cann A, Collette C. Sense of humor, stable affect, and psychological well-being . Eur J Psychol . 2014;10(3):464-479. doi:10.5964/ejop.v10i3.746
Pathak R, Lata S. Optimism in relation to resilience and perceived stress . J Psychosoc Res . 2018;13(2):359-367. doi:10.32381/JPR.2018.13.02.10
Dimitroff LJ, Sliwoski L, O’Brien S, Nichols LW. Change your life through journaling--The benefits of journaling for registered nurses . JNEP . 2016;7(2):p90. doi:10.5430/jnep.v7n2p90
American Psychological Association. Stress effects on the body .
Grant AM. Solution-focused cognitive-behavioral coaching for sustainable high performance and circumventing stress, fatigue, and burnout . Consult Psychol J Pract Res . 2017;69(2):98-111. doi:10.1037/cpb0000086
Lukić J, Lazarević S. A holistic approach to workplace stress management . Škola biznisa . 2019;(1):130-141. doi:10.5937/skolbiz1-21872
By Elizabeth Scott, PhD Elizabeth Scott, PhD is an author, workshop leader, educator, and award-winning blogger on stress management, positive psychology, relationships, and emotional wellbeing.
Information
- Author Services
Initiatives
You are accessing a machine-readable page. In order to be human-readable, please install an RSS reader.
All articles published by MDPI are made immediately available worldwide under an open access license. No special permission is required to reuse all or part of the article published by MDPI, including figures and tables. For articles published under an open access Creative Common CC BY license, any part of the article may be reused without permission provided that the original article is clearly cited. For more information, please refer to https://www.mdpi.com/openaccess .
Feature papers represent the most advanced research with significant potential for high impact in the field. A Feature Paper should be a substantial original Article that involves several techniques or approaches, provides an outlook for future research directions and describes possible research applications.
Feature papers are submitted upon individual invitation or recommendation by the scientific editors and must receive positive feedback from the reviewers.
Editor’s Choice articles are based on recommendations by the scientific editors of MDPI journals from around the world. Editors select a small number of articles recently published in the journal that they believe will be particularly interesting to readers, or important in the respective research area. The aim is to provide a snapshot of some of the most exciting work published in the various research areas of the journal.
Original Submission Date Received: .
- Active Journals
- Find a Journal
- Proceedings Series
- For Authors
- For Reviewers
- For Editors
- For Librarians
- For Publishers
- For Societies
- For Conference Organizers
- Open Access Policy
- Institutional Open Access Program
- Special Issues Guidelines
- Editorial Process
- Research and Publication Ethics
- Article Processing Charges
- Testimonials
- Preprints.org
- SciProfiles
- Encyclopedia

Article Menu

- Subscribe SciFeed
- Recommended Articles
- Google Scholar
- on Google Scholar
- Table of Contents
Find support for a specific problem in the support section of our website.
Please let us know what you think of our products and services.
Visit our dedicated information section to learn more about MDPI.
JSmol Viewer
How important are optimism and coping strategies for mental health effect in reducing depression in young people.

1. Introduction
2. materials and methods, 2.1. study design and participants, 2.2. measures, 2.3. ethical considerations, 2.4. statistical analysis, 3.1. demographic data, 3.2. descriptive statistics and correlations between the study variables, 3.3. moderating effects analysis, 3.4. direct effects of optimism and coping on depression, 3.5. indirect effects of optimism and coping on depression, 3.6. total indirect effects, 4. discussion, 4.1. limitations, 4.2. clinical implications, 5. conclusions, author contributions, institutional review board statement, informed consent statement, data availability statement, acknowledgments, conflicts of interest.
- Organización Mundial de la Salud. Informe Mundial Sobre Salud Mental: Transformar la Salud Mental para Todos: Panorama General. Available online: https://iris.who.int/handle/10665/356118 (accessed on 10 March 2024).
- Organización Mundial de la Salud. Depression. Available online: https://www.who.int/es/news-room/fact-sheets/detail/depression (accessed on 13 March 2024).
- Secretaría de Salud. 2° Diagnóstico Operativo de Salud Mental y Adicciones. Secretaría de Salud. Available online: https://www.gob.mx/cms/uploads/attachment/file/730678/SAP-DxSMA-Informe-2022-rev07jun2022.pdf (accessed on 13 March 2024).
- Instituto Nacional de Estadística y Geografía. Dia Mundial para la Prevención del Suicidio. Available online: https://www.inegi.org.mx/contenidos/saladeprensa/aproposito/2023/EAP_Suicidio23 (accessed on 25 March 2024).
- Luo, J.; Cao, W.; Zhao, J.; Zeng, X.; Pan, Y. The moderating role of optimism between social trauma and depression among Chinese college students: A cross-sectional study. BMC Psychol. 2023 , 11 , 270. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Asociación Americana de Psiquiatría. Guía de Consulta de los Criterios Diagnósticos del DSM 5 ; Asociación Americana de Psiquiatría: Arlington, VA, USA, 2013; ISBN 978-0-89042-551-0. [ Google Scholar ]
- Clark, L.A.; Watson, D. Tripartite Model of Anxiety and Depression: Psychometric Evidence and Taxonomic Implications. J. Abnorm. Psychol. 1991 , 100 , 316–336. [ Google Scholar ] [ CrossRef ]
- Nima, A.A.; Rosenberg, P.; Archer, T.; Garcia, D. Anxiety, Affect, Self-Esteem, and Stress: Mediation and Moderation Effects on Depression. PLoS ONE 2013 , 8 , e73265. [ Google Scholar ] [ CrossRef ]
- Lazarus, R.S.; Folkman, S. Stress, Appraisal, and Coping ; Springer Publishing Company: New York, NY, USA, 1984; ISBN 0-8261-4191-9. [ Google Scholar ]
- Mahmoud, J.S.R.; Staten, R.T.; Hall, L.A.; Lennie, T.A. The Relationship among Young Adult College Students’ Depression, Anxiety, Stress, Demographics, Life Satisfaction, and Coping Styles. Issues Ment. Health Nurs. 2012 , 33 , 149–156. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Gustems-Carnicer, J.; Calderón, C. Coping strategies and psychological well-being among teacher education students. Eur. J. Psychol. Educ. 2013 , 28 , 1127–1140. [ Google Scholar ] [ CrossRef ]
- Taylor, S.E.; Stanton, A.L. Coping Resources, Coping Processes, and Mental Health. Annu. Rev. Clin. Psychol. 2007 , 3 , 377–401. [ Google Scholar ] [ CrossRef ]
- Romswinkel, E.V.; König, H.H.; Hajek, A. The role of optimism in the relationship between job stress and depressive symptoms. Longitudinal findings from the German Ageing Survey. J. Affect. Disord. 2018 , 241 , 249–255. [ Google Scholar ] [ CrossRef ]
- Chen, Y.; Su, J.; Zhang, Y.; Yan, W. Optimism, Social Identity, Mental Health: Findings Form Tibetan College Students in China. Front. Psychol. 2021 , 12 , 747515. [ Google Scholar ] [ CrossRef ]
- Carver, C.S.; Scheier, M.F.; Segerstrom, S.C. Optimism. Clin. Psychol. Rev. 2010 , 30 , 879–889. [ Google Scholar ] [ CrossRef ]
- Arslan, G.; Yıldırım, M. Coronavirus stress, meaningful living, optimism, and depressive symptoms: A study of moderated mediation model. Aust. J. Psychol. 2021 , 73 , 113–124. [ Google Scholar ] [ CrossRef ]
- Banerjee, P. Relationship between perceived psychological stress and depression: Testing moderating effect of dispositional optimism. J. Workplace Behav. Health 2012 , 27 , 32–46. [ Google Scholar ] [ CrossRef ]
- Zou, R.; Xu, X.; Hong, X.; Yuan, J. Higher socioeconomic status predicts less risk of depression in adolescence: Serial mediating roles of social support and optimism. Front. Psychol. 2020 , 11 , 1955. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Greenglass, R.E.; Fiksenbaum, L. Proactive coping, positive affect, and well-being: Testing for mediation using path analysis considerations. Eur. Psychol. 2009 , 14 , 29–39. [ Google Scholar ] [ CrossRef ]
- Greenglass, E.; Fiksenbaum, l.; Eaton, J. The relationship between coping social support, functional disability and depression in the elderly. Anxiety Stress Coping 2006 , 19 , 15–31. [ Google Scholar ] [ CrossRef ]
- Lun, K.W.C.; Chan, C.K.; Ip, P.K.Y.; Ma, S.Y.K.; Tsai, W.W.; Wong, C.S.; Wong, C.H.T.; Wong, T.W.; Yan, D. Depression and anxiety among university students in Hong Kong. HKMJ 2018 , 24 , 466–472. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Shi, M.; Liu, L.; Wang, Z.Y.; Wang, L. Prevalence of depressive symptoms and its correlations with positive psychological variables among Chinese medical students: An exploratory cross-sectional study. BMC Psychiatry 2016 , 16 , 3. [ Google Scholar ] [ CrossRef ]
- Palacios-Delgado, J.; Acevedo-Ibarra, J.N. Psychometric Properties of a New Mexican Optimism Scale: Ethnopsychological Approach. Eur. J. Investig. Health Psychol. Educ. 2023 , 13 , 2747–2764. [ Google Scholar ] [ CrossRef ]
- Brissette, I.; Scheier, M.F.; Carver, C.S. The role of optimism in social network development, coping, and psychological adjustment during a life transition. J. Pers. Soc. Psychol. 2002 , 82 , 102–111. [ Google Scholar ] [ CrossRef ]
- Nes, L.S.; Segerstrom, S.C. Dispositional Optimism and Coping: A Meta-Analytic Review. Pers. Soc. Psychol. Rev. 2006 , 10 , 235–251. [ Google Scholar ] [ CrossRef ]
- Achat, H.; Kawachi, I.; Spiro, A.; DeMolles, D.A.; Sparrow, D. Optimism and depression as predictors of physical and mental health functioning: The Normative Aging Study. Ann. Behav. Med. 2000 , 22 , 127–130. [ Google Scholar ] [ CrossRef ]
- Cobb, C.L.; Schwartz, S.J.; Salas-Wright, C.P.; Pinedo, M.; Martinez, P.; Meca, A.; Isaza, A.G.; Lorenzo-Blanco, E.I.; McClure, H.; Marsiglia, F.F.; et al. Alcohol use severity, depressive symptoms, and optimism among Hispanics: Examining the immigrant paradox in a serial mediation model. J. Clin. Psychol. 2020 , 76 , 2329–2344. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Hamilton, J.L.; Connolly, S.L.; Liu, R.T.; Stange, J.P.; Abramson, L.Y.; Alloy, L.B. It gets better: Future orientation buffers the development of hopelessness and depressive symptoms following emotional victimization during early adolescence. J. Abnorm. Child. Psychol. 2015 , 43 , 465–474. [ Google Scholar ] [ CrossRef ] [ PubMed ]
- Rincón, U.A.; Botelho, S.; Gouveia, J.; da Silva, J. Association between the dispositional optimism and depression in young people: A systematic review and meta-analysis. Psicol. Reflex. Crit. 2021 , 34 , 1–14. [ Google Scholar ] [ CrossRef ]
- Vickers, K.S.; Vogeltanz, N.D. Dispositional optimism as a predictor of depressive symptoms over time. Pers. Individ. Dif. 2000 , 28 , 259–272. [ Google Scholar ] [ CrossRef ]
- Agudelo, D.; Carretero-Dios, H.; Blanco Picabia, A.; Pitti, C.; Spielberger, C.; Buela-Casal, G. Evaluación del componente afectivo de la depresión: Análisis factorial del ST/DEP revisado. Salud Ment. 2005 , 28 , 32–41. [ Google Scholar ]
- Tous-Pallarés, J.; Espinoza-Díaz, I.M.; Lucas-Mangas, S.; Valdivieso-León, L.; Gómez-Romero, M.D.R. CSI-SF: Propiedades psicométricas de la versión española del inventario breve de estrategias de afrontamiento. An. Psicol. 2022 , 38 , 85–92. [ Google Scholar ] [ CrossRef ]
- Secretaría de Salud. Reglamento de la Ley General de Salud en Materia de Investigación para la Salud. 2011. Available online: http://www.salud.gob.mx/unidades/cdi/nom/compi/rlgsmis.html (accessed on 16 February 2024).
- Belsley, D.A. Assessing the presence of harmful collinearity and other forms of weak data through a test for signal-to-noise. J. Econom. 1982 , 20 , 211–253. [ Google Scholar ] [ CrossRef ]
- Hayes, A.F. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach , 2nd ed.; The Guilford Press: New York, NY, USA, 2018; ISBN 978-1-60918-230-4. [ Google Scholar ]
- Lacobucci, D.; Saldanha, N.; Deng, X. A meditation on mediation: Evidence that structural equations models perform better than regressions. J. Consum. Psychol. 2007 , 17 , 139–153. [ Google Scholar ] [ CrossRef ]
- Hayes, A.F.; Rockwood, N.J. Conditional Process Analysis: Concepts, computation, and advances in the Modeling of the Contingencies of Mechanisms. Am. Behav. Sci. 2020 , 64 , 19–54. [ Google Scholar ] [ CrossRef ]
- Fritz, C.O.; Morris, P.E.; Richler, J.J. Effect size estimates: Current use, calculations, and interpretation. J. Exp. Psychol. Gen. 2012 , 141 , 2–18. [ Google Scholar ] [ CrossRef ]
- Dafogianni, C.; Pappa, D.; Mangoulia, P.; Kourti, F.E.; Koutelekos, I.; Dousis, E.; Margari, N.; Ferentinou, E.; Stavropoulou, A.; Gerogianni, G.; et al. Anxiety, Stress and the Resilience of University Students during the First Wave of the COVID-19 Pandemic. Healthcare 2022 , 10 , 2573–2584. [ Google Scholar ] [ CrossRef ]
- Özkul, B.; Günüşen, N.P. Stressors and Coping Methods of Turkish Adolescents With High and Low Risk of Depression: A Qualitative Study. J. Am. Psychiatr. Nurses Assoc. 2020 , 27 , 458–470. [ Google Scholar ] [ CrossRef ]
- Wanjie, T.; Qian, D. Depressive symptoms among first-year Chinese undergraduates: The roles of socio-demographics, coping style, and social support. Psychiatry Res. 2018 , 270 , 89–96. [ Google Scholar ] [ CrossRef ]
- Zong, J.G.; Cao, X.Y.; Cao, Y.; Shi, Y.F.; Wang, Y.N.; Yan, C.; Abela, J.R.Z.; Gan, Y.Q.; Gong, Q.Y.; Chan, R.C.K. Coping flexibility in college students with depressive symptoms. Health Qual. Life Outcomes 2010 , 8 , 66. [ Google Scholar ] [ CrossRef ]
- Sawyer, M.G.; Pfeiffer, S.; Spence, S.H. Life events, coping and depressive symptoms among young adolescents: A one-year prospective study. J. Affect. Disord. 2009 , 117 , 48–54. [ Google Scholar ] [ CrossRef ]
- Hussong, A.M.; Miggette, A.J.; Thomas, T.E.; Coffman, J.L.; Cho, S. Coping and Mental Health in Early Adolescence during COVID-19. Res. Child Adolesc. Psychopathol. 2021 , 49 , 1113–1123. [ Google Scholar ] [ CrossRef ]
- Tobin, D.L.; Holroyd, K.A.; Reynolds, R.V.; Wigal, J.K. The Hierarchical Factor Structure of the Coping Strategies Inventory. Cogn. Ther. Res. 1989 , 13 , 343–361. [ Google Scholar ] [ CrossRef ]
- Karing, C. Prevalence and predictors of anxiety, depression and stress among university students during the period of the first lockdown in Germany. J. Affect. Disord. Rep. 2021 , 5 , 100174. [ Google Scholar ] [ CrossRef ]
- Scheier, M.F.; Carver, C.S.; Bridges, M.W. Optimism, pessimism, and psychological well-being. In Optimism & Pessimism: Implications for Theory, Research, and Practice ; Chang, E.C., Ed.; American Psychological Association: Washington, DC, USA, 2001; pp. 189–216. ISBN 1-55798-691-6. [ Google Scholar ]
Click here to enlarge figure
| Demographic Variables | Frequency | Percentage |
|---|---|---|
| Sex—gender | ||
| Men | 410 | 48.3 |
| Women | 438 | 51.7 |
| Marital status | ||
| Single | 783 | 92.3 |
| Married | 32 | 3.8 |
| Free union | 33 | 3.9 |
| Profession | ||
| Health sciences | 394 | 46.5 |
| Social sciences | 67 | 7.9 |
| Arts and humanities | 101 | 11.9 |
| Business | 110 | 13.0 |
| Tourism and gastronomy | 15 | 1.8 |
| Engineering | 125 | 14.7 |
| No profession | 36 | 4.2 |
| Occupation | ||
| Student | 508 | 59.9 |
| Worker | 85 | 10 |
| Student and worker | 255 | 30.1 |
| Region of residence | ||
| North | 602 | 71 |
| South | 215 | 24.5 |
| Center | 31 | 3.7 |
| PV | AR | H | PFE | EFD | PFD | EFE | M | SD | |
|---|---|---|---|---|---|---|---|---|---|
| Depression | −0.537 *** | −0.559 *** | −0.503 *** | −0.478 *** | 0.433 *** | 0.232 *** | −0.297 *** | 31.42 | 8.2 |
| Positive Vision | _ | 0.712 *** | 0.608 ** | 0.566 ** | −0.244 ** | −0.074 * | 0.295 ** | 21.09 | 4.6 |
| Affective Resources | — | 0.594 ** | 0.524 *** | −0.277 *** | −0.112 ** | 0.212 *** | 16.47 | 3.77 | |
| Hope | — | 0.535 *** | −0.162 *** | −0.119 ** | 0.273 *** | 22.84 | 4.5 | ||
| Problem Focused Engagement | — | −0.145 ** | −0.041 | 0.396 *** | 13.51 | 2.5 | |||
| Emotional Focused Disengagement | 0.339 *** | −0.222 *** | 12.61 | 3.0 | |||||
| Problem Focused Disengagement | 0.076 * | 10.52 | 3.0 | ||||||
| Emotion Focused Engagement | 12.43 | 3.7 |
| Confidence Intervals 95% | |||||||
|---|---|---|---|---|---|---|---|
| Study Variables | β | SE | Z | Lower | Upper | ||
| PV | → | Depression | −0.121 | 0.039 | −3.13 ** | −0.197 | −0.045 |
| AR | → | Depression | −0.207 | 0.038 | −5.94 *** | −0.281 | −0.133 |
| Hope | → | Depression | −0.155 | 0.034 | −4.59 *** | −0.222 | −0.089 |
| PFE | → | Depression | −0.059 | 0.013 | −4.60 *** | −0.084 | −0.034 |
| EFD | → | Depression | −0.082 | −0.009 | 8.98 *** | 0.064 | 0.100 |
| PFD | → | Depression | 0.031 | 0.009 | 3.52 *** | 0.014 | 0.048 |
| EFE | → | Depression | −0.018 | 0.008 | −2.34 *** | −0.032 | −0.003 |
| PFE | → | Affective resources | 0.196 | 0.012 | 16.31 *** | 0.173 | 0.220 |
| EFD | → | Affective resources | −0.066 | 0.010 | −6.50 *** | −0.086 | −0.046 |
| PFD | → | Affective resources | −0.007 | 0.010 | −0.64 | −0.026 | 0.013 |
| EFE | → | Affective resources | −0.008 | 0.009 | −0.98 | −0.025 | 0.008 |
| PFE | → | Positive vision | 0.202 | 0.012 | 17.28 *** | 0.179 | 0.225 |
| EFD | → | Positive vision | −0.051 | 0.010 | −5.07 *** | −0.070 | −0.031 |
| PFD | → | Positive vision | −0.001 | 0.010 | −0.128 | −0.021 | −0.018 |
| EFE | → | Positive vision | −0.015 | 0.008 | 1.75 | −0.002 | 0.031 |
| PFE | → | Hope | 0.192 | 0.012 | 15.82 *** | 0.169 | 0.216 |
| EFD | → | Hope | −0.014 | 0.010 | −1.39 | −0.035 | 0.006 |
| PFD | → | Hope | −0.029 | 0.010 | −2.86 ** | −0.049 | −0.009 |
| EFE | → | Hope | 0.015 | 0.008 | 1.75 | −0.002 | 0.031 |
| Confidence Intervals 95% | |||||||||
|---|---|---|---|---|---|---|---|---|---|
| Study Variables | β | SE | Z | Lower | Upper | ||||
| PFE | → | PV | → | Depression | −0.002 | 0.008 | −3.08 * | −0.040 | −0.009 |
| PFE | → | AR | → | Depression | −0.410 | 0.008 | 5.20 *** | −0.056 | −0.025 |
| PFE | → | Ho | → | Depression | −0.030 | 0.007 | −4.41 ** | −0.043 | −0.017 |
| EFD | → | PV | → | Depression | 0.006 | 0.002 | 2.65 ** | 0.002 | 0.011 |
| EFD | → | AR | → | Depression | 0.014 | 0.003 | 4.19 *** | 0.007 | 0.020 |
| EFD | → | Ho | → | Depression | 0.002 | 0.002 | 1.33 | −0.001 | 0.006 |
| PFD | → | PV | → | Depression | 0.006 | 0.002 | 2.66 ** | 0.002 | 0.011 |
| PFD | → | AR | → | Depression | 0.001 | 0.002 | 0.55 | −0.003 | 0.005 |
| PFD | → | Ho | → | Depression | 0.005 | 0.002 | 2.43 | 0.000 | 0.008 |
| EFE | → | PV | → | Depression | −0.002 | 0.002 | 0.92 | −0.002 | 0.005 |
| EFE | → | AR | → | Depression | 0.002 | 0.002 | 0.97 | −0.002 | −1.21 |
| EFE | → | Ho | → | Depression | −0.003 | 0.001 | −2.04 * | −0.006 | −2.21 |
| Confidence Intervals 95% | |||||||
|---|---|---|---|---|---|---|---|
| Study Variables | β | SE | Z | Lower | Upper | ||
| PFE | → | Depression | −0.245 | 0.023 | −10.63 *** | −0.290 | −0.200 |
| EFD | → | Depression | 0.068 | 0.016 | 4.25 *** | 0.037 | 0.99 |
| PFD | → | Depression | 0.018 | 0.013 | 1.37 | −0.008 | 0.044 |
| EFE | → | Depression | −0.011 | 0.014 | −0.89 | −0.039 | −0.015 |
| The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
Share and Cite
Palacios-Delgado, J.; Acosta-Beltrán, D.B.; Acevedo-Ibarra, J.N. How Important Are Optimism and Coping Strategies for Mental Health? Effect in Reducing Depression in Young People. Psychiatry Int. 2024 , 5 , 532-543. https://doi.org/10.3390/psychiatryint5030038
Palacios-Delgado J, Acosta-Beltrán DB, Acevedo-Ibarra JN. How Important Are Optimism and Coping Strategies for Mental Health? Effect in Reducing Depression in Young People. Psychiatry International . 2024; 5(3):532-543. https://doi.org/10.3390/psychiatryint5030038
Palacios-Delgado, Jorge, Delia Brenda Acosta-Beltrán, and Jessica Noemí Acevedo-Ibarra. 2024. "How Important Are Optimism and Coping Strategies for Mental Health? Effect in Reducing Depression in Young People" Psychiatry International 5, no. 3: 532-543. https://doi.org/10.3390/psychiatryint5030038
Article Metrics
Article access statistics, further information, mdpi initiatives, follow mdpi.

Subscribe to receive issue release notifications and newsletters from MDPI journals
- Open access
- Published: 12 September 2024
Accepting and committing to caregiving for schizophrenia—a mixed method pilot study
- Aishwarjya Chakraborty 1 ,
- Somdeb Mitra 1 &
- Deepshikha Ray 1
BMC Psychiatry volume 24 , Article number: 613 ( 2024 ) Cite this article
Metrics details
End of traditional institutionalized psychiatric care, diagnostic complexities, and associated stigma often negatively impact the social networks of caregivers, making them experience social isolation. Not the “identified patients”, caregiver perspectives are typically overlooked further adding to anticipatory stigma resulting in social death among them. Caregiving experience results in developing coping skills, preventing carers from responding to the nuances of the context, and identifying the useful rules— “Experiential Avoidance”. Psycho-education is typically combined with other formal treatment programs for case conceptualization, and to provide a clear rationale for the treatment approach but less as a distinct psychotherapy. Borrowing the philosophy of Functional Contextualism, the present study developed a “Present-Moment Awareness” guided psychoeducational intervention. The aim was to reduce schizophrenia caregiver burden and anticipatory stigma and promote the value of caregiver participation as ‘experts by experience’.
Five family caregivers of remitted schizophrenia patients were recruited using purposive sampling. Pre-post measure was taken on caregiver burden, caregiving experience, sense of personal mastery, and caregiving competence. Results were analysed quantitatively and qualitatively.
A significant decrease in caregiver burden, stigma, and negative effects on the family in post-intervention was observed. Self-compassion led to a rise in a sense of empowerment.
A caregiver-centred “Present-Moment Awareness” guided psycho-education for schizophrenia caregivers can be considered a possible means to address perceived stigma in caregivers and to reduce associated distress of carers.
Peer Review reports
Introduction
Schizophrenia is one of the most severe and debilitating forms of mental illness which mostly follows a chronic course and impairment in social and occupational functioning [ 6 ]. The family is often the major source of care and protection for a person affected by schizophrenia [ 3 , 7 , 30 ] and caring for an ill relative profoundly affects the roles and interactions within the family [ 50 ]. On one hand, the responsibility of having to take care of a relative suffering for a prolonged period along with the stress of dealing with the ill relative’s bizarre behaviour leads to despair, guilt [ 6 ], and helplessness [ 1 , 7 , 50 ]. On the other hand, there is stress associated with social stigma [ 3 , 15 , 59 ], discrimination [ 3 , 35 , 59 ] and lack of social support [ 1 , 3 , 40 ] which, in turn, may lead to social isolation for the caregivers [ 14 ] and reflects how the stigma of schizophrenia results in a series of losses in caregivers’ social identity, relationships, and growth opportunities [ 37 ]. According to Von Kardoff et al. (2016) [ 64 ], caregiving of a relative with schizophrenia may deplete the emotional resources of the primary caregiver, more specifically the parents, offsprings or spouses and make them susceptible to mental illness. It has been reported that caregivers of schizophrenia patients face significantly more challenges in comparison to caregivers of people living with other forms of mental diseases or chronic physical illness [ 31 , 42 ]. In spite of compelling evidence that caregivers of schizophrenia suffer from stress [ 4 ], relatively less emphasis is given to the amelioration of caregiver burden [ 29 ]. It is also important to note that caregiver burden is an important predictor of recovery and quality of life in schizophrenia patients [ 49 ].
The present study thus attempts to offer an intervention programme with present-moment awareness-guided psycho-education within the Indian context and to investigate its efficacy in relation to the subjective perception of caregiver burden. It was hypothesized that the positive change in the carers’ attitudes would be mainly mediated due to psychological flexibility through the awareness of their “creative hopelessness” and promote voluntary active help-seeking.
Study design
The study incorporated a mixed method design, specifically a convergent-parallel design [ 20 ] where quantitative and qualitative data were collected simultaneously and independently from the same participants.
For the quantitative part of the study, a one-group pretest–posttest design was used.
For the qualitative part of the study, thematic analysis [ 10 ].
Purposive sampling.
Recruitment
Five informal primary caregivers of patients with an ICD-10 DCR /DSM-V criteria for Schizophrenia Spectrum Disorder [ 5 , 67 ] (in recovery or partial remission) participated and completed the study. The diagnosis of Schizophrenia Spectrum Disorder was made by a licensed psychiatrist from tertiary referral hospitals in and around Kolkata. The concerned patients were referred for psychological assessment /psychotherapy to the Clinical Psychology Centre of University of Calcutta.
Participants
The group consisted of four elderly parents (three fathers, one mother) of sons and a spouse of a female patient. All participants were within the age range of 18—65 years, belonging to the middle-income group as measured by Kuppuswami’s Socio-economic status scale [ 39 ] with a minimum educational level of class 8. They were either a parent or a sibling or a child or a spouse to the patient of either sex and were providing care for a minimum of 1 year. The mean age of study participants was 56.8 years and the standard deviation (SD) was 11.05 (refer to Table 1 in the Results section).
Operational definition of key terms
The primary caregiver was operationalized as the person in the family most involved in the caregiving, providing time, support, monitoring medicines, and other aspects of the patient’s everyday life viz. spouse, parent, offspring, and sibling.
Ethical approval
Ethical approval for the work was obtained from the Institutional Ethical Committee, University of Calcutta & Secretary, UCSTA, CU (Ref No: 015/17–18/1688). Prior information regarding the purpose of the study and confidentiality issues were communicated individually to all participants. The consent form was personally read out to them by the researcher in the language they understood and they were allowed to ask questions about it. As all participants hailed from a Bengali background, Bengali written consent was provided to them individually. Written consent was obtained from all the participants before the study commenced.
Assessment tools
Burden Assessment Schedule of SCARF (BAS) [ 60 ] measures the subjective and objective components of the burden across 9 different areas. Developed at SCARF with the support of the WHO SEARO & the technical support from Dr. Helmut Sell, WHO SEARO, this 40-item scale is rated on a 3-point scale. The responses are ‘not at all’ to ‘very much’. Some of the items are reverse coded. Scores range from 40 to 120 with higher scores indicating greater burden. Inter-rater reliability (Kappa value of 0.8) [ 60 ] shows good reliability. The scale has an established criterion validity.
Experience of Caregiving Inventory (ECI) [ 57 ] is a 66-itemed questionnaire that captures the experience of caregiving across ten subscales- eight negative subscales and two positive subscales Items are responded on a five-point Likert scale from “never” to “nearly always”. The maximum score for the combined negative subscales is 208 and 56 for the positive subscales. Higher scores on the negative scales indicate greater negative perceptions of caregiving whereas higher scores on the positive scales indicate greater positive perceptions of caregiving. Each subscale has been reported to have satisfactory reliability (Cronbach alpha coefficient between 0.74 and 0.91) and the total scale (all 66 items) has also shown good reliability (Cronbach alpha = 0.93) [ 57 ].
Measure of Personal Mastery (MoPM) [ 51 ] was used to measure caregivers’ personal feelings of control over aspects of their lives. The scale consists of seven items that relate to carers’ overall control of their life. Responses are coded on a four-point scale from strongly disagree to strongly agree. Five out of a total of seven items are negatively worded and two are positively worded. The negatively worded items are reverse coded prior to scoring, resulting in a score range of 7 to 28, with higher scores indicating greater levels of mastery. Total scores range from 7 (low sense of mastery) to 28 (high sense of mastery). The scale has shown satisfactory internal consistency (Cronbach alpha = 0.78) [ 51 ].
Measure of Caregiver Competence (MoCC) [ 52 ] is a four-item questionnaire that assesses caregivers’ self-competence in providing care. The four items are measured on a four-point Likert scale (total scores range from 0 to 12). A higher score indicates a higher sense of self-competence. Although more comprehensive measures are available, it was decided that a simple measure would be satisfactory for this aspect of the study as the use of more complex tools could overburden participants. A Cronbach’s alpha of 0.74 [ 52 ] was reported indicating satisfactory, and statistically acceptable, internal consistency.
Intervention Module
Details of the assessment tools and intervention module are given below in a tabular format.
A pre-and post-assessment was conducted separately immediately before and after the intervention. After pre-assessment, participants were individually given the 11-h intervention. Each session lasted for 90 min. Participants were then interviewed after 2.5 weeks to qualitatively explore their understanding of the intervention, caregiving experience, and associated problems. Each discussion continued for 30 min. A sample size of five was chosen to determine if the study could be administered as intended. The intervention was divided into six sessions spreading over 6–7 weeks | ||
| Purpose | Points Covered |
| Psychoeducation | Disorder, symptoms as experienced by the patient, medication and relapse prevention |
| Psychoeducation | Clarification, aetiology (neuroanatomical and expressed emotion); Formulating ‘Suffering Inventory’ |
| Psychoeducation; Experience of Caregiver Burden | Clarification, free talk on feelings of meaninglessness, personal sacrifices, negativities of caregiving—forming; understanding the ‘Creative Hopelessness’ stance by means of ‘Suffering Inventory’ and ‘Magic Wand’ |
| Management of caregiver burden; sense of moving forward rather than backward, growing rather than shrinking | Unworkability of ‘Experiential Avoidance’- and ‘Ball in the pool’ and ‘Quick sand’; Present-Moment Awareness exercise “Going Along with the Process” for “Creative Hopelessness” stance; Homework |
| Management of caregiver burden; sense of moving forward rather than backward, growing rather than shrinking | Unworkability of ‘Experiential Avoidance’- and ‘Ball in the pool’ and ‘Quick sand’; Present-Moment Awareness exercise “Going Along with the Process” for “Creative Hopelessness” stance; Homework |
| Increasing Present-Moment Awareness—Acceptance of the whole process | Same as previous session; feedback and homework |
Psycho-education interventions targeted to the reduction of caregiver distress generally trys to provide information about the nature and progress of illness and about management skills. Such interventions, though effective in their own right, seldom address the emotional burden and / or burnout of the caregivers. Hence, if knowledge about the disorder is incorporated with skills related to the management of personal distress, it can be expected to be more effective in reducing caregiver burden [ ]. Recent studies have provided evidence in favour of the efficacy of interventions including an education component [ , ] and mindfulness skills in mental disorders [ , ]. As psychological distress is a critical component of caregiving experience, induction of psychological flexibility [ ] inherent in Acceptance Commitment Therapy may help caregivers detach themselves from negative experiences of caregiving [ ], reappraisal of their efficacy of caregiving, de-stigmatization, and learn to live in the present. Rigidity of cognitive fusion is problematic as it results from and leads to thought patterns characterising an absolute truth [ ]. Similar psycho-education modules combining ACT have been thus successfully used in schizophrenia [ ]. | ||
All the scales were translated and checked by three experts to obtain translations meaningful in the local context. The current intervention was planned and conducted by a clinical psychology trainee at the Clinical Psychology Centre of University of Calcutta (CPCUC), Kolkata, India and the intervention was supervised by two academic faculty members specialising in Clinical Psychology.
Assessment details conducted at pre-intervention and post-intervention of the study.
|
|
|
| Informed consent, Rapport establishment through free talk, pre-intervention measures | Checking history of caregiving and burden as experienced, Intervention program and Mental Status Examination |
| Post-intervention measures Discussion | Post-intervention assessment, Sharing personal experience and feedback |
Quantitative analysis
Descriptive statistics such as means and standard deviations were computed. The Wilcoxon signed-rank test was used to analyse the quantitative data as the sample size was small and the same group of participants was assessed at two different points of time [ 28 ].
Qualitative analysis
Post-assessment interviews were analysed using Thematic Analysis [ 10 ]. Investigator triangulation [ 24 ] involves the participation of three researchers; the author and her supervisors to arrive at a mutually agreed upon interpretation was done as a means of ensuring the trustworthiness of the data.
Quantitative results
The significant findings on the quantitative measures are as follows-.
Table 2 a shows a significant change in ‘ Burden Assessment Schedule’ scores from the pretest to the post-test ( p = 0.042) among caregivers indicating less burden in the post-intervention phase.
No significant change was observed in the ‘experience of caregiving total negative’ scores across treatment conditions ( p > 0.05). Similarly, no significant change in ‘experience of caregiving total positive’ scores across treatment ( p > 0.05) was observed. However, the domain-specific significant reduction in the domains of ‘Stigma’ and ‘Effects on Family’ in post-intervention was observed. Table 2 b shows a significant change only in ‘stigma’ ( p < 0.05) and ‘effect on family’( p < 0.05) scores across treatment conditions indicating less stigma and effect on family in post-intervention. Table 2 c. shows no statistically significant change in ‘Measure of Personal Mastery’ (MoPM) ( p > 0.05) across treatment conditions among participants while Table 2 d shows no statistically significant change in ‘Measure of Caregiving Competence’ (MoCC) ( p > 0.05) across treatment conditions among participants.
Qualitative results
Showing Focus Codes and the corresponding Open Codes for Individual Participant.
Shows Focus codes and the corresponding common components across all participant.
Tables 3 and 4 show a clear positive impact of the current intervention module on knowledge and attitude towards the illness. All participants report positive changes in the relational dynamics with the patient, a reduction in anticipatory stigma, comfortable discussing the ill-relative with others, an overall sense of empowerment, and a lookout for a better future together.
The current study utilized a six-session intervention program on caregivers of people suffering from schizophrenia spectrum disorder combining psychoeducation with ‘Present Moment Awareness’ component of Acceptance Commitment Therapy.
A statistically significant reduction in perception of “caregiver burden”, “perception of stigma”, and “effect of the disease on the family” were obtained post-intervention. While knowledge about schizophrenia and alternative coping reduced caregiver burden, ‘Present-Moment Awareness’ helped these carers shift their focus on the overall process of caregiving, no statistically significant change in the “perception of personal mastery” and “perception of caregiver competence” was found after the intervention.
To the best of our knowledge, the current study, when conducted, was one of the few studies undertaken in India, determining the effect of Acceptance and Commitment Therapy (ACT) based psycho-educational intervention on schizophrenia carers.
Discussion on the effect of intervention on caregiver burden
The current psycho-education particularly aimed at the participant’s lack of knowledge about the nature of the disorder. The illness and treatment-focused psychoeducation provided these carers with the required knowledge for problem-focused coping. Understanding patients' unpredictable behaviour and disturbances helped them to re-appraise the situation and not to interpret such behavioural abnormalities in terms of deficits in caregiving or intentional behaviour from the patient. Similar findings have been reported, where structured psycho-educational intervention is found to be more effective [ 56 ] with caregiver burden in schizophrenia [ 12 , 46 ] and has significantly increased the perception of social support and satisfaction with treatment than routine out-patient care among Indian schizophrenia caregivers [ 3 , 12 , 38 ]. Knowledge about schizophrenia and alternative coping [ 17 ] was also found to reduce perceived caregiver burden [ 8 ]. Additionally in line with previous studies, the ‘Present-Moment Exercise’, which is an Acceptance and Commitment Therapy approach, helped carer’s shift their focus from the burden aspect of care to the overall process of caregiving and notice when they are repetitively being self critical [ 63 ]. It was also found out that such intervention helped caregivers to deal with experiential avoidance of their caregiving related thoughts which, in turn, moderated their wellbeing and sense of burden [ 16 , 33 ]. Lowered levels of experiential avoidance successfully brought down the negative effect of perceived burden, also found among family carers of people with dementia [ 23 , 33 ].
Discussion on the effect of intervention on stigma
Providing care to patients with mental health problems puts a burden on families, often due to stigma [ 25 ], and moderates the use of support resources at times of need as evidenced by the qualitative data of the present study substantiated by previously established findings [ 55 ]. In line with previous studies [ 2 ], the current participants perceived societal stigma of living with a person suffering from schizophrenia led to the internalization of stigma, a condition of “affiliate stigma” [ 62 ]. It can be said that under the condition of affiliate stigma, these carers developed negative feelings toward themselves, as they identified with the stigma that prevails in society related to schizophrenia; manifested behaviourally in terms of generally engaging in less social contact, concealing the association with the patient from the public etc. According to Mak & Cheung (2008) [ 43 ], affiliate stigma may distort a caregiver’s perception of the illness and the ill relative, thereby generating greater emotional strain in the process of caregiving. Thus, internalization of stigma can be said to intensify the perception of burden in caregivers; which is also evident from the fact that “perception of stigma” is a subdomain in the scale of measurement of “experience of caregiver burden” by Szmukler et al. (1996) [ 57 ]. Werner et al. (2012) [ 65 ] had also found out that caregiver stigma increased caregiver burden in Israeli caregivers of Alzheimer's patients. Hence, it can be proposed that psycho-education incorporating information about the nature of illness (schizophrenia) helps caregivers to develop and overcome the negative attitude towards the illness stemming from lack of knowledge related to the stigma; which in turn might have reduced their perceived sense of burden in caring for the ill relative. The efficacy of psychoeducation in reducing stigma [ 8 , 35 ] and the subjective burden of caregiving [ 54 , 61 ] has been established by previous research.
From a different perspective, psychological inflexibility is associated with self-stigma [ 13 ]. Hence, the incorporation of ACT may help the participants (caregivers of persons suffering from schizophrenia) develop the ability to “engage in valued behavior by remaining open to internal experiences” [ 36 ], which, in turn, may serve to lower levels of stigma. Mak et al. (2021) [ 44 ] also reported that ACT helped caregivers to accept the inevitability of the difficulties associated with caregiving of a relative suffering from a psychiatric disorder, reduced their (caregivers) reliance on experiential avoidance, and repression of negative feelings which probably acted as resistance to stigma, and promoted their recovery.
Discussion on the effect of intervention on the effect on family
The relationship between perceived stigma and the severity of caregiver burden of schizophrenia is observed to be mediated by the caregivers’ experience of the effects schizophrenia has on the family, and other social functioning. Experiential avoidance of such unpleasant emotions might lead to a vicious circle of intensifying the negative emotions. The present-moment awareness used in this study allowed the caregivers to relate to their thoughts differently [ 58 ]. Post-intervention, the perspective of the caregivers on the negative effects of schizophrenia on the family changed. Their awareness of the moment at present opened them to commit to behaviours deeply rooted in caregiving values that ultimately reduced the impact of schizophrenia on the family and provided an integral approach to schizophrenia, as evidenced by both previous literature [ 26 ] and the current findings of the study.
Discussion of findings from qualitative study
It is evident from the findings of the qualitative part of this research that the caregivers experienced self-blame and lack of self-compassion prior to the intervention and reported improvements in these domains after the intervention [ 21 , 22 ]. Previous studies have also been able to find quantitatively measurable associations between self-compassion, psychological flexibility and mindfulness [ 18 , 19 ] which were components of the ACT incorporated within the psychoeducation program. According to their narrations, the caregivers, after receiving the intervention could consciously (mindfully) acknowledge their stigma and reappraise their role as a caregiver, accepting their experiences of distress as a natural consequence of caregiving. Similar efficacy of integrating mindfulness with traditional psychoeducation in the reduction of caregiver burden was obtained by Neff & Germer (2013) [ 47 ] and Zhang et al., (2023) [ 68 ].
The qualitative data also reveals a marked change in the nature of expressed emotion of the caregivers. The intervention program used in this study included “mindfulness” which helps clients (caregivers) to directly address their painful emotions and thoughts and thereby develop a positive self-appraisal [ 48 ]. Such a practice could have helped the participants (caregivers) to grow more understanding and compassionate towards themselves as they encountered the challenges of caring for their relatives with schizophrenia. Again, such acts of kindness towards self are also empowering in the sense they may act as a buffer against the emotional toll of caregiving, foster positive self-appraisal and a non-critical attitude towards oneself [ 66 ], leading to reduced feelings of caregiver burden. A study by Goodridge et al. (2012) [ 27 ] had also been able to show the effectiveness of “mindfulness-based self-compassion program” to enhance the emotional well-being of the participants who happened to be.
To the best of our knowledge, our study when conducted was one of the few studies undertaken in India, determining the effect of Acceptance and Commitment Therapy (ACT) based psycho-educational intervention on schizophrenia carers.
Helping the caregivers view themselves, the patient, and the future compassionately helps caregivers endure the burden of the present situation, and strengthen their value-directed behaviour. Fostering future hope is particularistic as well as general. Hope and family involvement are related to socio-cultural, age, economic, and geographical contexts. This might prompt in the future for the provision of family-focused brief ACT-based therapy and the role of social prescribing as a mandatory treatment module. However, such aims can only be achieved by systematically including informal caregivers as active partners, in treatment and research. Carers are ‘experts by experience’ just as patients are. Without their voices, the picture remains incomplete. Involving informal carers is an important means to address social expectations; to rethink the existing hierarchies of the current Indian health-related science and thus change the treatment culture as a whole.
Limitations
One major limitation of this study was the small sample size with primarily elderly caregivers. No matched control group was included. A randomized waitlist control group, dynamic waitlist design (DWLD), and regression point displacement (RPDD) as alternatives could have increased the efficiency and generalization power of the study findings. Availability of caregivers was a major restriction due to the lack of an in-patient facility at the study centre coupled with stigma toward family intervention. Also, attending a family program conveyed a series of monetary and logistical difficulties including time, motivation, and energy.
Future implications
A major observation and an impediment faced while carrying out the study was the lack of willingness for families to be active participants in treatment due to the existing social stigma related to mental health. The exact interconnection and frequency of real and anticipated stigma in India needs clarification [ 26 ]. Further studies similar to the current study should specifically focus on developing self-compassion-based psycho-educational intervention using cognitive defusion and present-moment awareness skills. It will be worth observing how the current intervention may promote psychological resilience and mindful self-compassion [ 32 , 41 ] along with reducing caregiver burden [ 53 ] and affiliate stigma [ 62 ].
The general understanding of the need for collaborative family-based intervention to mainstream patients was poor. Families often approach therapy as an individual endeavour and not as a collective phenomenon. While the attitude towards the development of any mental illness is a failure on the part of the affected individual, similarly cure is often perceived as the patient’s responsibility. Thus, it is essential to deeply explore the role of Indian collectivism in promoting social security and how the prevailing paternalism outweighs quality healthcare. From a treatment perspective, more than reducing actual stigma, the focus should be on how to normalize perceived discrimination and thus reduce the social death of these families. Further qualitative research is required to study these overlapping pathways between the mental bias of experiential avoidance and decision-making to curate human-centric interventions.
Availability of data and materials
The data that support the findings of this study are available from the 1st author (corresponding author), but restrictions apply to the availability of these data and are not publicly available. The data are, however, available from the author upon reasonable request and with the permission of the university's ethical committee.
Aggarwal M, Avasthi A, Kumar S, Grover S. Experience of caregiving in schizophrenia: a study from India. Int J Soc Psychiatry. 2009,2011;57(3);224–36. https://doi.org/10.1177/0020764009352822 .
Ahmedani BK. Mental health stigma: society, individuals, and the profession. J Soc Work Values Ethics. 2011;8(2):4–1.
PubMed Central Google Scholar
Akbari M, Alavi M, Irajpour A, Maghsoudi J. Challenges of family caregivers of patients with mental disorders in Iran: a narrative review. Iran J Nurs Midwifery Res. 2018;23(5):329–37.
Article PubMed PubMed Central Google Scholar
Alzahrani SH, Fallata EO, Alabdulwahab MA, Alsafi WA, Bashawri J. Assessment of the burden on caregivers of patients with mental disorders in Jeddah. Saudi Arabia BMC psychiatry. 2017;17:1–8.
Google Scholar
American Psychiatric Association DS, American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. Washington: American psychiatric association; 2013.
Book Google Scholar
Awad AG, Voruganti LNP. The Burden of schizophrenia on caregivers. Pharmacoeconomics. 2008;26(2):149–62. https://doi.org/10.2165/00019053-200826020-00005 .
Article PubMed Google Scholar
Azarudeen MJ, Ramamurthy S, Chandrasekar S, Gopal BS. Depression and the caregiver burden for schizophrenia patients. IAR J Med Surg Res. 2023;4(4):1–6.
Article Google Scholar
Bahrami R, Khalifi T. The effect of psycho-education on the affiliate stigma in family caregivers of people with bipolar disorder. SAGE Open Nurs. 2022;8:23779608221132170.
Bilgin A, Ozdemir L. Interventions to improve the preparedness to care for family caregivers of cancer patients: a systematic review and meta-analysis. Cancer Nurs. 2022;45(3):E689-705.
Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3(2):77–101.
Çetin N, Aylaz R. The effect of mindfulness-based psychoeducation on insight and medication adherence of schizophrenia patients. Arch Psychiatr Nurs. 2018;32(5):737–44.
Chakraborty S, Bhatia T, Anderson C, Nimgaonkar VL, Deshpande SN. Caregiver’s burden, coping and psycho-education in Indian households with single-and multiple-affected members with schizophrenia. Int J Ment Health Promot. 2013;15(5):288–98.
Chan KK, Mak WW. The cognitive content and habitual process of self-stigma: effects on self-esteem and recovery. Eur Psychiatry. 2015;30:734.
Chien WT, Thompson DR. Effects of a mindfulness-based psychoeducation programme for Chinese patients with schizophrenia: 2-year follow-up. Br J Psychiatry. 2014;205(1):52–9. https://doi.org/10.1192/bjp.bp.113.134635 .
Cleary M, West S, Hunt GE, McLean L, Kornhaber R. A qualitative systematic review of caregivers’ experiences of caring for family diagnosed with schizophrenia. Issues Ment Health Nurs. 2020;41(8):667–83. https://doi.org/10.1080/01612840.2019.1710012 . PMID: 32255401.
Cookson C, Luzon O, Newland J, Kingston J. Examining the role of cognitive fusion and experiential avoidance in predicting anxiety and depression. Psychol Psychother Theory Res Pract. 2020;93(3):456–73.
Creado DA, Parkar SR, Kamath RM. A comparison of the level of functioning in chronic schizophrenia with coping and burden in caregivers. Indian J Psychiatry. 2006;48(1):27–33. https://doi.org/10.4103/0019-5545.31615 . PMID: 20703411; PMCID: PMC2913639.
Dahm KA, Meyer EC, Neff KD, Kimbrel NA, Gulliver SB, Morissette SB. Mindfulness, self-compassion, posttraumatic stress disorder symptoms, and functional disability in US Iraq and Afghanistan war veterans. J Trauma Stress. 2015;28(5):460–4.
Davey A, Chilcot J, Driscoll E, McCracken LM. Psychological flexibility, self-compassion and daily functioning in chronic pain. J Contextual Behav Sci. 2020;17:79–85.
Demir SB, Pismek N. A convergent parallel mixed-methods study of controversial issues in social studies classes: a clash of ideologies. Educ Sci Theory Pract. 2018;18(1):119–49.
Dudley J, Eames C, Mulligan J, Fisher N. Mindfulness of voices, self-compassion, and secure attachment in relation to the experience of hearing voices. Br J Clin Psychol. 2018;57(1):1–7.
Eicher AC, Davis LW, Lysaker PH. Self-compassion: a novel link with symptoms in schizophrenia? J Nerv Ment Dis. 2013;201(5):389–93.
Fauth EB, Novak JR, Levin ME. Outcomes from a pilot online Acceptance and Commitment Therapy program for dementia family caregivers. Aging Ment Health. 2022;26(8):1620–9.
Flick U. Triangulation in qualitative research. In: A companion to qualitative research, vol. 3. 2004. p. 178–83.
Girma E, Möller-Leimkühler AM, Dehning S, Mueller N, Tesfaye M, Froeschl G. Self-stigma among caregivers of people with mental illness: toward caregivers’ empowerment. J Multidiscip Healthc. 2014:37–43.
González-Menéndez A, ArboleyaFaedo T, González-Pando D, Ordoñez-Camblor N, García-Vega E, Paino M. Psychological inflexibility in people with chronic psychosis: the mediating role of self-stigma and social functioning. Int J Environ Res Public Health. 2021;18(23):12376.
Goodridge D, Reis N, Neiser J, Haubrich T, Westberg B, Erickson-Lumb L, Storozinski J, Gonzales C, Michael J, Cammer A, Osgood N. An app-based mindfulness-based self-compassion program to support caregivers of people with dementia: participatory feasibility study. JMIR Aging. 2021;4(4):e28652.
Guilford JP. Fundamental statistics in psychology and education. 1950.
Hamann J, Heres S. Why and how family caregivers should participate in shared decision making in mental health. Psychiatr Serv. 2019;70(5):418–21.
Hou SY, Ke CL, Su YC, Lung FW, Huang CJ. Exploring the burden of the primary family caregivers of schizophrenia patients in Taiwan. Psychiatry Clin Neurosci. 2008;62(5):508–14. https://doi.org/10.1111/j.1440-1819.2008.01843.x . PMID: 18950369.
Kamil SH, Velligan DI. Caregivers of individuals with schizophrenia: who are they and what are their challenges? Curr Opin Psychiatry. 2019;32(3):157–63.
Khoury B, Lecomte T, Fortin G, Masse M, Therien P, Bouchard V, Chapleau MA, Paquin K, Hofmann SG. Mindfulness-based therapy: a comprehensive meta-analysis. Clin Psychol Rev. 2013;33(6):763–71.
Kishita N, Contreras ML, West J, Mioshi E. Exploring the impact of carer stressors and psychological inflexibility on depression and anxiety in family carers of people with dementia. J Contextual Behav Sci. 2020;17:119–25.
Kor PP, Chien WT, Liu JY, Lai CK. Mindfulness-based intervention for stress reduction of family caregivers of people with dementia: a systematic review and meta-analysis. Mindfulness. 2018;9:7–22.
Koschorke M, Padmavati R, Kumar S, Cohen A, Weiss HA, Chatterjee S, Pereira J, Naik S, John S, Dabholkar H, Balaji M. Experiences of stigma and discrimination of people with schizophrenia in India. Soc Sci Med. 2014;123:149–59.
Krafft J, Klimczak KS, Levin ME. Effects of cognitive restructuring and defusion for coping with difficult thoughts in a predominantly white female college student sample. Cogn Ther Res. 2022;46(1):86–94.
Králová J. What is social death?. InSocial Death 2018 Apr 19 (pp. 13-26). Routledge.
Kulhara P, Chakrabarti S, Avasthi A, Sharma A, Sharma S. Psychoeducational intervention for caregivers of Indian patients with schizophrenia: a randomised-controlled trial. Acta Psychiatr Scand. 2009;119(6):472–83.
Article CAS PubMed Google Scholar
Kuppuswamy B. Manual of socio-economic status scale (urban). Manasyan: Delhi; 1981.
Leng A, Xu C, Nicholas S, Nicholas J, Wang J. Quality of life in caregivers of a family member with serious mental illness: evidence from China. Arch Psychiatr Nurs. 2019;33(1):23–9.
Lök N, Bademli K. The effect of a mindful self-compassion intervention on burden, express emotion and mental well-being in family caregivers of patients with Schizophrenia: a randomized controlled trial. Comm Mental Health J. 2024:1–9.
Magliano L, Fiorillo A, De Rosa C, Malangone C, Maj M, National Mental Health Project Working Group. Family burden in long-term diseases: a comparative study in schizophrenia vs. physical disorders. Soc Sci Med. 2005;61(2):313–22.
Mak WW, Cheung RY, Law RW, Woo J, Li PC, Chung RW. Examining attribution model of self-stigma on social support and psychological well-being among people with HIV+/AIDS. Soc Sci Med. 2007;64(8):1549–59.
Mak WW, Chio FH, Chong KS, Law RW. From mindfulness to personal recovery: the mediating roles of self-warmth, psychological flexibility, and valued living. Mindfulness. 2021;12:994–1001.
Muntean LM, Popa CO, Nireștean A, Cojocaru C, Schenk A, Bologh FI. The relationship between unconditional self-acceptance and cognitive fusion in psychosis. Psihiatru. ro. 2020;62(3).
Nasr T, Kausar R. Psychoeducation and the family burden in schizophrenia: a randomized controlled trial. Ann Gen Psychiatry. 2009;8:1–6.
Neff KD, Germer CK. A pilot study and randomized controlled trial of the mindful self-compassion program. J Clin Psychol. 2013;69(1):28–44.
Neff KD. Does self-compassion entail reduced self-judgment, isolation, and over-identification? A response to Muris, Otgaar, and Petrocchi (2016). Mindfulness. 2016;7(3):791–7.
Nuttall AK, Thakkar KN, Luo X, Mueser KT, Glynn SM, Achtyes ED, Kane JM. Longitudinal associations of family burden and patient quality of life in the context of first-episode schizophrenia in the RAISE-ETP study. Psychiatry Res. 2019;276:60–8.
Pan Z, Li T, Jin G, Lu X. Caregiving experiences of family caregivers of patients with schizophrenia in a community: a qualitative study in Beijing. BMJ Open. 2024;14(4):e081364.
Pearlin LI, Mullan JT, Semple SJ, Skaff MM. Caregiving and the stress process: an overview of concepts and their measures. Gerontologist. 1990;30(5):583–94.
Pearlin LI, Schooler C. The structure of coping. J Health Soc Behav. 1978:2–1.
Poulin PA, Mackenzie CS, Soloway G, Karayolas E. Mindfulness training as an evidenced-based approach to reducing stress and promoting well-being among human services professionals. Int J Health Promot Educ. 2008;46(2):72–80.
Shamsaei F, Cheraghi F, Esmaeilli R. The family challenge of caring for the chronically mentally ill: a phenomenological study. Iran J Psychiatry Behav Sci. 2015;9(3).
Shamsaei F, Nazari F, Sadeghian E. The effect of training interventions of stigma associated with mental illness on family caregivers: a quasi-experimental study. Ann Gen Psychiatry. 2018;17:1–5.
Shihabuddeen TM, Gopinath PS. Effectiveness of Brief Psycho Education [BPE] in Schizophrenia and Bipolar Mood Disorder. Indian J Psychol Med. 2005;27(1):113–9. https://doi.org/10.1177/0975156420050112 .
Szmukler GI, Burgess P, Herrman H, Bloch S, Benson A, Colusa S. Caring for relatives with serious mental illness: the development of the Experience of Caregiving Inventory. Soc Psychiatry Psychiatr Epidemiol. 1996;31:137–48.
Tai S, Turkington D. The evolution of cognitive behavior therapy for schizophrenia: current practice and recent developments. Schizophr Bull. 2009;35(5):865–73.
Tawiah PE, Adongo PB, Aikins M. Mental health-related stigma and discrimination in ghana: experience of patients and their caregivers. Ghana Med J. 2015;49(1):30–9.
Article CAS PubMed PubMed Central Google Scholar
Thara R, Padmavati R, Kumar S, Srinivasan L. Instrument to assess burden on caregivers of chronic mentally ill. Indian J Psychiatry. 1998;40(1):21–9.
CAS PubMed PubMed Central Google Scholar
Vaghee S, Salarhaji A, Asgharipour N, Chamanzari H. Effects of psychoeducation on stigma in family caregivers of patients with schizophrenia: a clinical trial. Evid Based Care. 2015;5(3):63–76.
Van den Bossche P, Schoenmakers B. The impact of Dementia’s affiliate stigma on the mental health of relatives: a cross section survey. Front Psychol. 2022;12:789105.
Van Hout E, Contreras ML, Mioshi E, Kishita N. Does avoiding distressing thoughts and feelings influence the relationship between carer subjective burden and anxiety symptoms in family carers of people with dementia? J Appl Gerontol. 2023;42(8):1760–9.
Von Kardorff E, Soltaninejad A, Kamali M, Eslami SM. Family caregiver burden in mental illnesses: the case of affective disorders and schizophrenia–a qualitative exploratory study. Nord J Psychiatry. 2016;70(4):248–54.
Werner P, Mittelman MS, Goldstein D, Heinik J. Family stigma and caregiver burden in Alzheimer’s disease. Gerontologist. 2012;52(1):89–97.
Whitebird RR, Kreitzer M, Crain AL, Lewis BA, Hanson LR, Enstad CJ. Mindfulness-based stress reduction for family caregivers: a randomized controlled trial. Gerontologist. 2013;53(4):676–86.
World Health Organization, editor. International Statistical Classification of Diseases and related health problems: Alphabetical index. World Health Organization; 2004.
Zhang ZJ, Lo HH, Ng SM, Mak WW, Wong SY, Hung KS, Lo CS, Wong JO, Lui SS, Lin E, Siu CM. The effects of a mindfulness-based family psychoeducation intervention for the caregivers of young adults with first-episode psychosis: a randomized controlled trial. Int J Environ Res Public Health. 2023;20(2):1018.
Download references
Acknowledgements
We acknowledge the voluntary participation of the participants and patients and thank them profusely. We also thank the respective psychotherapists at the study centre who referred their patients to participate in this study. We declare no financial assistance was taken or given to conduct the study.
No fund was involved in carrying out the study.
Author information
Authors and affiliations.
Department of Psychology, University of Calcutta, Rashbehari Siksha Prangan (Commonly Known As Rajabazar Science College Campus), 92, Acharya Prafulla Chandra Road, Kolkata, West Bengal, 700009, India
Aishwarjya Chakraborty, Somdeb Mitra & Deepshikha Ray
You can also search for this author in PubMed Google Scholar
Contributions
The study was designed by A.C and supervised by S.M and D.R. A.C conducted the study, collected and analysed the data, and prepared the first draft of the manuscript. S.M and D.R supervised the data analysis and writing of the final draft of the manuscript. All the authors read the manuscript and approved it.
Corresponding author
Correspondence to Aishwarjya Chakraborty .
Ethics declarations
Ethics approval and consent to participate, consent for publication.
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note.
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License, which permits any non-commercial use, sharing, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if you modified the licensed material. You do not have permission under this licence to share adapted material derived from this article or parts of it. The images or other third party material in this article are included in the article’s Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc-nd/4.0/ .
Reprints and permissions
About this article
Cite this article.
Chakraborty, A., Mitra, S. & Ray, D. Accepting and committing to caregiving for schizophrenia—a mixed method pilot study. BMC Psychiatry 24 , 613 (2024). https://doi.org/10.1186/s12888-024-05993-9
Download citation
Received : 24 December 2023
Accepted : 29 July 2024
Published : 12 September 2024
DOI : https://doi.org/10.1186/s12888-024-05993-9
Share this article
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Schizophrenia
- Caregiver burden
- Psychoeducation
- Acceptance and commitment theraphy
BMC Psychiatry
ISSN: 1471-244X
- General enquiries: [email protected]

IMAGES
VIDEO
COMMENTS
From a proactive perspective, research on academic stress has emphasized the importance of coping strategies in preventing harmful consequences. In recent years, there has been a growing interest in discovering the extent to which individuals are able to combine different coping strategies and the adaptive consequences this flexibility entails.
Background In the case of people who carry an increased number of anxiety traits and maladaptive coping strategies, psychosocial stressors may further increase the level of perceived stress they experience. In our research study, we aimed to examine the levels of perceived stress and health anxiety as well as coping styles among university students amid the COVID-19 pandemic. Methods A cross ...
Coping is an assessment process designed to respond to external and internal challenges. Coping strategies are defined as efforts to regulate emotions, behaviors, cognitions and environmental aspects in response to the stress of everyday events. Each situation requires the use of a specific coping strategy.
It also explored their coping strategies (i.e., job resources) that helped them adjust to the demands of using a different arrangement for teaching and learning in the new normal.
reductions in life satisfaction, feelings of control, a sense of belonging, mental and physical health, and greater stress. Three coping strategies resonated with at least 45% of the students in Study 2: maintaining. social connections, developing a satisfying routine, and trying new activities.
This study emphasizes the importance of the social aspect of coping in adolescents and is essential to understanding PE as a social context. Communal coping within the social context of PE is a field that needs to be explored to a greater extent. Social isolation was a contrasting theme.
Stress is viewed as an important part of life towards self-improvement. In any case, not all learners can adapt sufficiently. This study, therefore, seeks to explore stressors and coping approaches adopted by undergraduate students pursuing teacher education programmes in the school of education and leadership of the University of Ghana.
Abstract Coping involves any effort to deal with difficult or challenging situations, and coping strategies vary, often depending on individual differences and situational circumstances. Research has typically characterized coping as either involving problem-focused or emotion-focused strategies, or sometimes approach or avoidance strategies.
Our study illuminates the different coping strategies and sources of support that adolescents experiencing varying levels of adversity in life view as protective (or less so) in relation to handling difficult situations and feelings over a three-year period - and why.
This paper demonstrates that there are not only demographic and social predictors of coping styles during the COVID-19 pandemic, but specific adversities are related to the ways that adults cope. Furthermore, this study identifies groups at risk of more avoidant coping mechanisms which may be targeted for supportive interventions.
Thus, this study aims to understand the differences in coping in young people when dealing with their own versus a friend's symptoms of poor mental health. We utilized the Transactional Theory of Coping (Lazarus & Folkman, 1984) as a framework to understand how the coping process develops.
Researchers recently have suggested that coping flexibility (i.e., an individual's ability to modify and change coping strategies depending on the context) may be an important way to investigate coping. The availability of numerous coping strategies may be an important precursor to coping flexibility, given that flexibility can only be obtained if an individual is able to access and use ...
In order to (1) minimize any potential negative effects from stressors, (2) increase coping skills to deal with stressors, or (3) manage strains, organizational practitioners or consultants will devise organizational interventions geared toward prevention, coping, and/or stress management.
Based on TwoStep cluster analysis of the Brief Cope, three different coping patterns were identified: low coping, engagement coping, and disengagement coping. Analyses of long-term stability indicated malleable properties for the individual coping strategies as well as the three clusters.
potential job loss. A multiple case study approach was used to understand what coping strategies employees use to reduce the negative effects of toxic leadership on themselves, other employees, and the overall workplace; and to understand the behaviors that result from these strategies. The purposeful and snowball sample consisted of 29 ...
Based on this assessment, our coping mechanisms and psychological responses to stress are triggered. The model suggests that coping strategies can be either problem focused or emotion focused. Problem-focused coping involves actively addressing the stressor, while emotion-focused coping involves managing the emotions associated with the stressor.
Coping Strategies A large number of community studies has examined the role of coping strategies in stress resistance. Coping encompasses cognitive and behavioral efforts to reduce or adapt to stressful conditions and associated emotional distress. Most conceptualizations distinguish between coping strategies that are oriented toward approaching and confronting the problem and strategies that ...
The profile showed that a greater combination of the three strategies was related to higher general self-efficacy expectations and vice versa. These results suggest that encouraging flexibility in coping strategies would help to improve university students' self-efficacy.
Similarly, in a study with child protection workers, the use of active and engaged coping strategies (rather than avoidant coping strategies) led to a decline in depersonalisation levels and increased employees' sense of personal accomplishment [22].
We must use coping strategies & skills to help us overcome and flourish.
Background and Objectives: To evaluate the efficacy of coping strategies used to reduce burnout syndrome in healthcare workers teams. Materials and Methods: We used PubMed and Web of Science, including scientific articles and other studies for additional ...
Stress can impact a person physically and mentally, also affecting their relationships. Learn a few effective coping strategies for stress and how to use them.
Depression is one of the most common disorders worldwide, including in Mexico. Engagement coping and optimism promote mental health, so understanding the mediation of optimism between coping strategies with depression helps to identify the psychological resources that young people can use to mitigate depression. This study aims to test the direct and indirect effects of four coping strategies ...
Caregiving experience results in developing coping skills, preventing carers from responding to the nuances of the context, and identifying the useful rules— "Experiential Avoidance". Psycho-education is typically combined with other formal treatment programs for case conceptualization, and to provide a clear rationale for the treatment ...