Communication in Nursing Practice: Gibbs’ Reflective Cycle Essay
- To find inspiration for your paper and overcome writer’s block
- As a source of information (ensure proper referencing)
- As a template for you assignment

Introduction
Description, action plan, reflective conclusion.
Communication is a fundamental element in nursing practice. This element can possibly determine patients’ satisfaction and even the outcomes of their treatment (Lotfi et al., 2019). The situation described in the paper will exemplify the potential role of communication, which is why it will serve as a Gibbs Reflective Cycle nursing example. The cycle will help to assess the situation and extract lessons from it.
The model is a widely-recognized and crucial learning instrument, allowing individuals to extract lessons from life experiences. The pattern helps one to consider previous experiences, reevaluate them in the light of new knowledge, and implement the freshly obtained insight to improve future practice (Markkanen et al., 2020). The cycle is composed of six stages (description, feelings, evaluation, analysis, conclusion, and action plan), on which the reflection regarding the personal experience will be based (Markkanen et al., 2020). The paper’s principal objective is to outline a challenging situation from personal practice using Gibbs’ Reflective Cycle. The problematic situation is an encounter with a patient suffering from an infected diabetic foot ulcer and in need of amputation. Overall, the paper aims to critically analyze the situation and transform it into a learning opportunity useful in improving my future practice as a wound care specialist.
The situation concerns a 40-year-old patient with diabetes and an infected foot ulcer who was admitted to the hospital where I was working at the moment. The patient had a long history of diabetes, from which he suffered since he was ten years old. A multidisciplinary team examined the patient and established that he needed an amputation. As I approached the patient to get a consent form, I noticed that he looked upset. Given the described situation, it might be suggested that a communication dilemma here is of ethical character, in particular – it is the delivery of the bad news. By applying the model, the provided Gibbs Reflective Cycle example communication will demonstrate what actions were undertaken to resolve the mentioned dilemma.
The incident that will be analyzed is an outstanding Gibbs Reflective Cycle nursing example, which happened several years ago when I began working as a wound care nurse. A 40-year-old diabetic patient with an infected diabetic foot ulcer was admitted to the hospital. He had a long history of diabetes, suffering from the condition for three decades. A multidisciplinary team examined and communicated with the patient; it was established that he needed a below-knee amputation. The group stated their decision and left, and I had to retrieve the consent form. While retrieving the record, I perceived that the patient looked exceedingly sorrowful and depressed. Nevertheless, I did not know whether I needed to intervene in the situation and left.
Although I worked for many years in nursing before the incident, I became a certified wound care nurse relatively recently before it took place. At the moment, I saw the situation as irreparable, so I was not sure whether I should have tried to console the patient. I felt anxious and, to an extent, powerless when faced with the man’s grief. I thought that words or an empathic response would not be able to mitigate his sadness. Additionally, I was also somewhat startled that the multidisciplinary team did not handle the conversation more delicately and left rather abruptly. Overall, I did not feel confident enough to handle the situation and was unsure whether my intervention would be appropriate.
I frequently returned to the incident, trying to understand what should have been done instead. Retrospectively, I believe that it helped me to reevaluate the role of therapeutic communication in my profession. Prior to the incident, I did not perceive preoccupation with patients’ emotional well-being as my duty as a nurse. I believed that administering medications and treatment, performing tests, recording medical history, educating patients, et cetera, was all that was required of me. Nevertheless, I did not fulfill another vital function in the described situation. To understand that a holistic approach to care presupposes therapeutic communication, I had to experience the case (2). As a nurse, showing empathy and consoling patients is a critical function that is sometimes overlooked. Furthermore, the incident demonstrates a lack of cooperation between the nursing staff and the team since communication was needed to ensure that the emotional impact of amputation on the patient was alleviated.
Some medical professionals find the process of delivering bad news challenging and feel psychologically unprepared (Van Keer et al., 2019). A lack of skills in this aspect can negatively affect patients: they might undergo extra stress, have lower psychological adjustment, and have worse health outcomes (Biazar et al., 2019; Matthews et al., 2019). Furthermore, the way the news is handled can impact patients’ understanding of the situation and adherence to treatment (Galehdar et al., 2020). Given the adverse effects, multiple protocols and approaches to communicating bad news and dealing with its consequences were developed. This situation is analyzed in detail in a ‘Gibbs Reflective Cycle example essay pdf’ that focuses on these communication challenges in healthcare.
In the patient- and family-centered approach, the process occurs based on the patient’s needs as well as their cultural and religious beliefs (Hagqvist et al., 2020). Upon communicating the information, a medical professional is supposed to assess their understanding and show empathy (Hagqvist et al., 2020). In an emotion-centered approach, a medical professional is supposed to embrace the sadness of the situation and build the patient-medical professional interaction on empathy and sympathy (Hagqvist et al., 2020). Yet, the patient- and family-centered approach seems more effective since excessive empathy can be counter-productive and impede information exchange.
Managing patients’ reactions is the final and particularly vital step in communicating bad news. Nurses are commonly involved in handling emotional responses, which entails several responsibilities:
- Additional emotional support should be given to those who cannot accept the information (Galehdar et al., 2020).
- Nurses can find more related information and share it with patients (Rathnayake et al., 2021).
- Nurses are supposed to improve the situation if bad news has been delivered poorly (Dehghani et al., 2020).
In the case of amputation, heightened emotional attention should be given to the patient, as limb loss is a life-altering procedure. Such patients commonly undergo the five stages of grief (denial, anger, bargaining, depression, and acceptance) and are prone to developing anxiety, depression, and body image issues (Madsen et al., 2023). Hence, upon delivering the news regarding amputation, it is vital to provide a patient with community resources for dealing with emotional and psychological implications.
Currently, I understand more in-depth that delivering and handling the consequences of bad news is an inescapable reality of the nursing profession. The incident allowed me to notice the aspects of my professional development that necessitate more attention and improvement. Hence, I strive to be more empathetic in my clinical practice and not undervalue the role of patient-nurse communication. I attempt to provide psychological and emotional support to patients and console them to the best of my ability and knowledge, especially if a patient has just received traumatic news. Due to the incident, I comprehended better that a patient’s emotional well-being can be dependent on my actions. I also stopped presuming that other medical professionals provide the necessary emotional support. Moreover, I understand that I am not powerless when faced with a patient’s sorrow.
Consequently, I will not neglect the importance of patient-nurse communication for patients’ health outcomes and mental well-being. I will offer hope where it is appropriate and encourage and validate patients’ emotions to help them deal with traumatic information (Font-Jimenez et al., 2019). In the future, I will use verbal and non-verbal communication clues to show that I care and, generally, be more empathetic (Font-Jimenez et al., 2019). I will not prevent my insecurities from fulfilling my nursing duties, nor will I allow the feeling of hopelessness to affect my clinical practice. Furthermore, I will rely on evidence-based approaches to handle bad news effectively and facilitate its delivery to patients.
Additionally, I will be more mindful in my nursing practice. Gibb’s reflective cycle will assist me in attaining this objective. I will continue to apply it to the situations occurring at work in order to think systematically as well as analyze and evaluate them. Furthermore, Gibb’s reflective cycle will enhance my ability to learn from my experience. The model will help me to refine my communication skills and make patient-nurse interactions more intuitive and productive (Markkanen et al., 2020).
The situation allowed me to understand the actual value of therapeutic communication in nursing. Now, I understand the need to exercise it in my clinical practice, which is a realization that I further explored in a ‘Gibbs Reflective Cycle example essay pdf.’ Learning to provide emotional support and manage the consequences of bad news is an essential quality for nurses, influencing health outcomes and satisfaction from a visit. Additionally, I become more conscious of my own emotions and the way they can prevent me from acting in a patient’s best interests. Overall, the proper tactics of delivering bad news and assisting patients in handling them became a higher priority in my clinical practice.
To conclude, this reflection featured an episode from my practice in which I analyzed a communication situation using Gibbs’ Reflective Cycle. It showed that I need to concentrate on my abilities to resolve the communication dilemma of the delivery of bad news. The above discussion also demonstrated how the implementation of an appropriate and significant evidence-based model – Gibbs’ Reflective Cycle – may result in better patient outcomes.
Biazar, G., Delpasand, K., Farzi, F., Sedighinejad, A., Mirmansouri, A., & Atrkarroushan, Z. (2019). Breaking bad news: A valid concern among clinicians . Iranian Journal of Psychiatry, 14 (3), 198–202. Web.
Dehghani, F., Barkhordari-Sharifabad, M., Sedaghati-kasbakhi, M., & Fallahzadeh, H. (2020). Effect of palliative care training on perceived self-efficacy of the nurses . BMC Palliative Care, 19 , 63. Web.
Font-Jimenez, I., Ortega-Sanz, L., Acebedo-Uridales, M. S., Aguaron-Garcia, M. J., & de Molina-Fernández, I. (2019). Nurses’ emotions on care relationship: A qualitative study . Journal of Nursing Management, 28 (8), 2247-2256. Web.
Galehdar, N., Kamran, A., Toulabi, T., & Heydari, H. (2020). Exploring nurses’ experiences of psychological distress during care of patients with COVID-19: A qualitative study . BMC Psychiatry, 20 , 489. Web.
Hagqvist, P., Oikarainen, A., Tuomikoski, A.-M., Juntunen, J., & Mikkonen, K. (2020). Clinical mentors’ experiences of their intercultural communication competence in mentoring culturally and linguistically diverse nursing students: A qualitative study . Nurse Education Today, 87 , 104348. Web.
Lotfi, M., Zamanzadeh, V., Valizadeh, L., & Khajehgoodari, M. (2019). Assessment of nurse–patient communication and patient satisfaction from nursing care . Nursing Open, 6 (3), 1189-1196. Web.
Madsen, R., Larsen, P., Carlsen, A. M. F., & Marcussen, J. (2023). Nursing care and nurses’ understandings of grief and bereavement among patients and families during cancer illness and death – A scoping review . European Journal of Oncology Nursing, 62 , 102260. Web.
Markkanen, P., Välimäki, M., Anttila, M., & Kuuskorpi, M. (2020). A reflective cycle: Understanding challenging situations in a school setting . Educational Research, 62 (1), 46-62. Web.
Matthews, T., Baken, D., Ross, K., Ogilvie, E., & Kent, L. (2019). The experiences of patients and their family members when receiving bad news about cancer: A qualitative meta-synthesis . Psycho-Oncology, 28 (12), 2286-2294. Web.
Rathnayake, S., Dasanayake, D., Maithreepala, S. D., Ekanayake, R., & Basnayake, P. L. (2021). Nurses’ perspectives of taking care of patients with Coronavirus disease 2019: A phenomenological study. PLoS ONE, 16 (9), e0257064
Van Keer, R. L., Deschepper, R., Huyghens, L., & Bilsen, J. (2019). Challenges in delivering bad news in a multi-ethnic intensive care unit: An ethnographic study . Patient Education and Counseling, 102 (12), 2199-2207. Web.
- Root Cause Analysis of Decubitus Ulcers
- Nurse Practitioner Cost Effectiveness
- Gibbs’s Reflective Cycle and Borton’s Model of Reflection
- "The Epic of Gilgamesh" by Ryan Gibbs
- The Topic of Diagnostic Measures
- Modern Nurse’s Role: Leadership
- Nurse Leader and Abbott Northwestern Hospital
- Mindfulness Meditation Program and Nursing Outcomes
- Catheter-Associated Urinary Tract Infection: Nurse-Sensitive Indicators
- Healthcare Quality and Safety in Practice
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2022, June 17). Communication in Nursing Practice: Gibbs' Reflective Cycle. https://ivypanda.com/essays/gibbs-reflective-cycle-essay-essay-examples/
"Communication in Nursing Practice: Gibbs' Reflective Cycle." IvyPanda , 17 June 2022, ivypanda.com/essays/gibbs-reflective-cycle-essay-essay-examples/.
IvyPanda . (2022) 'Communication in Nursing Practice: Gibbs' Reflective Cycle'. 17 June.
IvyPanda . 2022. "Communication in Nursing Practice: Gibbs' Reflective Cycle." June 17, 2022. https://ivypanda.com/essays/gibbs-reflective-cycle-essay-essay-examples/.
1. IvyPanda . "Communication in Nursing Practice: Gibbs' Reflective Cycle." June 17, 2022. https://ivypanda.com/essays/gibbs-reflective-cycle-essay-essay-examples/.
Bibliography
IvyPanda . "Communication in Nursing Practice: Gibbs' Reflective Cycle." June 17, 2022. https://ivypanda.com/essays/gibbs-reflective-cycle-essay-essay-examples/.
IvyPanda uses cookies and similar technologies to enhance your experience, enabling functionalities such as:
- Basic site functions
- Ensuring secure, safe transactions
- Secure account login
- Remembering account, browser, and regional preferences
- Remembering privacy and security settings
- Analyzing site traffic and usage
- Personalized search, content, and recommendations
- Displaying relevant, targeted ads on and off IvyPanda
Please refer to IvyPanda's Cookies Policy and Privacy Policy for detailed information.
Certain technologies we use are essential for critical functions such as security and site integrity, account authentication, security and privacy preferences, internal site usage and maintenance data, and ensuring the site operates correctly for browsing and transactions.
Cookies and similar technologies are used to enhance your experience by:
- Remembering general and regional preferences
- Personalizing content, search, recommendations, and offers
Some functions, such as personalized recommendations, account preferences, or localization, may not work correctly without these technologies. For more details, please refer to IvyPanda's Cookies Policy .
To enable personalized advertising (such as interest-based ads), we may share your data with our marketing and advertising partners using cookies and other technologies. These partners may have their own information collected about you. Turning off the personalized advertising setting won't stop you from seeing IvyPanda ads, but it may make the ads you see less relevant or more repetitive.
Personalized advertising may be considered a "sale" or "sharing" of the information under California and other state privacy laws, and you may have the right to opt out. Turning off personalized advertising allows you to exercise your right to opt out. Learn more in IvyPanda's Cookies Policy and Privacy Policy .

How to Write a Nursing Reflective Essay (Guide for Nurse Students)

If you are a nursing or medicine student, you are aware that you will come across or have already come across assignments requiring you to write a nursing reflection essay. At first, such a task always appears challenging, but given the understanding of the steps, things flat out, and you can write reflective essays and get better grades.
Reflective practice is highly encouraged in nursing. Reflection entails making sense of situations, events, actions, and phenomena in the workplace.
As a nursing student, you will be asked to write a reflective essay on your clinical placement, practicum, shadowing experience, shadow health DCE activities, personal nursing philosophy, why you want to become a nurse, nursing program, ethical dilemma, knowledge, skills, and abilities, systems, and processes.
The easiest way to complete the reflective essay assignment is by first determining what reflective writing entails, its significance, its steps, and some of the best tips that form the core of this ultimate guide.
Basics of Reflective Writing in Nursing
Reflective writing is an analytical writing practice where the writer describes a real or imaginary event, scene, phenomenon, occurrence, or memory, including their takeaway. It entails the critical analysis of an experience, including recording how it has impacted you and what you intend to do with the new knowledge or how to act when such an occurrence recurs.
As you document the encounter, you can use first-person pronouns and write subjectively and objectively. This means that you can decide to either use personal experiences alone or support these experiences using citations from scholarly sources.
When writing a reflective essay in nursing, you must recount the events and give critical detail of how the events shaped your knowledge acquisition. Reflection helps nursing students develop skills in self-directed learning, which is directly associated with high motivation and improved quality of care .
In most cases, reflection occurs on what went well and what went wrong. It could be a successful operation, a thank you note from a patient, a patient who regained their health faster, or a new nursing care plan that worked. However, it can also be about adverse events such as death, postoperative complications, death of an infant at birth, dissatisfied patient, medical error, or a failed procedure.
As a nursing student, when you learn to reflect on situations, you grow to become a professional nurse who diligently does their noble duty.
When writing a reflective essay, you begin by setting the scene (explaining what, where, how, and who-the situation), detailing how you felt (emotional state), why it happened (making sense of the situation), critical review and development of insights, a note on what was learned, and strategies to address future recurrence.
Your professor may ask you to write a nursing reflective paper about various topics in your course or your experience working in a group, how you solved a problem, a healthcare issue, or clinical practice. Consider the following example of a reflective statement in nursing; in my clinical practices, I realized I focused more on the technical aspects but failed to explain what it was doing to improve their health. I would like to understand more about listening to patience and their concerns to better care for them.
As you will notice later, these reflective stages are structured into different reflective models and frameworks that we will explore in-depth. So, with the understanding of what comprises reflective writing and its importance in nursing, let's now get solid on the structure.
Related Reading:
- Philosophy of Nursing Example.
- Ideas and topics for nursing capstone or project papers
- How to write a SOAP note paper
- Top nursing debate topics
- Nursing Theories and Theorists.
Structure of a Reflective Essay in Nursing
A reflective essay is an analytical writing piece describing and evaluating encounters or experiences. When asked to write one, you should know that an excellent reflective essay consists of different parts, just like a typical academic essay. It comprises the cover or title page, introduction, body paragraphs, conclusions, and a references page.
The title page contains information about the assignment. If you are writing the reflective essay in APA, include these on the title page:
- Title of the reflective essay
- Course code and name
- Instructors name
- Name of your institution
- Date of submission
When writing in Harvard format, the title or the cover page will consist of the following:
- Title of the essay in title case and the page number (upper right margin),
- Title of the essay in CAPS,
- Name of class or course,
- Name of the instructor,
- Name of your school,
- City and state where your school is located and,
- The date of submission.
Introduction
The introduction begins with an attention grabber or a hook sentence to attract readers' attention. It should then explain the essay's purpose and signpost the ideas that will come later in the essay. The introduction also has a thesis statement at the end of the paragraph- the last sentence. The thesis is concise, clear, and relatable and should reflect your position.
Body Paragraphs
The body paragraphs of a reflective essay can be three or more, depending on the length of the essay. Essentially, the body comprises 80% of the total word count.
The first paragraph is where you describe the situation, including the events, why they occurred, how they occurred, and those involved.
The second paragraph entails your personal feelings or reaction to the situation and how it made you feel.
The third paragraph can include making sense of the situation. You have to think about why things happened the way they did. You should also critically review and develop insights based on the situation. Finally, think of the factors that could have influenced the situation.
The next paragraph should explain how the event or situation will change your practice, approach, decisions, perspective, or perception. This is where you evaluate the experience by detailing the knowledge and skills you took from the experience.
The last body paragraph should entail a critical reflection on the learning opportunities. First, describe the situation and what it made you learn. Next, elaborate on how you intend to make yourself better poised to address such situations.
Mostly, you should structure the body of your essay as per the preferred nursing reflective model.
After everything else falls into place, you need to summarize the information you presented in the essay. Then, finally, restate your thesis and have a call to action to bring a sense of closure to your readers.
Steps for Writing a Nursing Reflection Essay � The Guide
When assigned to write a reflective essay for your nursing class, here are the surefire steps to get you to success.
Read the instructions
The first step after receiving an assignment is to begin reading the instructions. as you read, note what your instructor or professor expects in the paper you will submit for marking.
Reading instructions helps you to get informed on the scope of the paper, word count, number of references and pages, and the formatting style to use.
Besides, you also get to plan your paper with the deadline highlighted in the instructions.
You need to get a conducive environment where you can start writing.
The first step of writing is to brainstorm about situations during your clinical hours when you were shadowing a Nurse Practitioner or one you have read about.
Assess whether the situation or scenario you have thought, encountered, or chosen can help you write a reflective essay that meets the requirements.
Research and Plan
After choosing a scenario, the next step is researching the best reflective model.
You can use your class text, the instructions, the college library, course readings, and online nursing journals to get articles and resources with information about specific reflective models.
Select the best reflective model and take notes on the steps it entails.
As you research, write down notes on how to address your paper based on your selected framework or model of reflection . Additionally, research nursing journal articles with information you can use when critically analyzing a situation.
Plan how you will handle the paper as well. For instance, as you research, develop a thesis statement that grounds your entire paper, then draft an outline on how to develop the thesis.
Write an Outline
Outlining is a crucial aspect of writing. It helps you envision how you will meet the objective of writing a reflective essay. As an essential part of the essay writing process, outlining helps create a good flow of ideas and can come in handy in helping you overcome writer's block. Your outline should comprise the following:
- The hook or attention grabber
- Thesis statement
- Main points of each body paragraph (topic sentence, evidence, examples, illustrations, etc.)
- Conclusion (restated thesis and call-to-action)
With the outline done, you should take a break and resume writing your first draft of the nursing reflection essay. Writing with an outline helps avoid mistakes and also helps you write faster.
Describe the Experience
Once you have identified the relevant experience, begin describing it chronologically.
Describe the experience that prompted you to consider nursing your ideal career goal. Think of this experience's key elements, such as the setting, patient demographics, and significant events that impacted you.
Show how these events changed your perspective on life. Ensure you are as descriptive as possible to paint a clear picture for readers.
Consider the following questions to come up with a good description:
- What happened?
- Was there someone involved? If yes, what part did they play?
- Where did the event take place?
- What actions did you take?
Set the context of this experience by giving relevant background information. Ensure you are objective and pay attention to the facts.
Provide a Reflection
Talk about your feelings and thoughts concerning the particular experience you went through. You have to be honest and open up about your initial expectations and challenges you faced at each stage of the experience. The following questions can help you come up with a good reflection:
- What was I trying to achieve?
- What prompted me to act the way I did?
- Are there any consequences for my actions? If yes, what are they?
- How did I feel about this event as it was happening?
- How did those around me react to it?
- How do I know how those around me felt about it?
Analyze the Experience
Description of an experience is essential, but so is analysis. You have to move beyond the surface and give a critical analysis of your experience.
State your actions, and your overall experience will give insights into your experience. Think of how the experience has impacted your actions, feelings, and thoughts.
Give an Evaluation
Evaluate the skills and knowledge you got from the experience. Show how you can apply these skills and knowledge in your nursing practice. Also, state the actions and interventions you took during the nursing experience.
State whether you achieved the desired outcome and if there are any specific areas that you need to improve on.
Talk about how you built or improved skills like communication, teamwork, and critical thinking.
As you evaluate the experience, identify what you believe to be your strengths and weaknesses in the nursing experience. What have you learned from the experience? State the areas where you excelled and what abilities contributed to your success.
Talk about how those you were with during the clinical experience complimented you. Similarly, acknowledge your weaknesses.
What kind of mistakes did you make, and how did you improve them? Talk about the tasks that drain you most during the experience.
Illustrate Learning
Demonstrate elements of deeper thought and reflection levels. This is a great point to include nursing theories in your reflection essay to support analysis of your experience.
Relate your experiences to the theoretical frameworks you were taught in class. This is effective learning and will demonstrate your ability to apply knowledge to real-life nursing situations.
Doing this will also show that you can effectively deduce different things from observations made during the reflection process.
Ensure you also demonstrate a change in perspective, as this will prove that you learned something from the experience.
Write Your Conclusion
Conclude by summarizing your points and highlighting the lessons learned.
The lessons you reached as part of your reflection should support your overall conclusion.
Also, restate your thesis statement.
Come Up with an Action Plan
Now that you have learned from your reflection develop an action plan for future nursing practice.
This part should contain all the details you have learned and actions needed to improve when faced with a similar situation. Consider the following questions:
- What would I change if faced with a similar situation?
- How can I develop the necessary skills needed to face this situation?
- How can I act differently in a similar situation?
Ensure you identify areas to improve and set realistic goals to enhance your nursing skills. Discuss how you intend to seek additional education, training, or mentorship to address your shortcomings.
Finally, end the essay with a happy note so readers know you learned something from the experiences.
Proofread, Edit, and Polish
After doing your first draft, take a break to relax and get out of the writing mood - it helps you to become objective.
You can then resume reading out loud to yourself, make necessary tweaks, and ensure that every part you include meets the rubric requirements.
Edit for grammar, punctuation, tenses, voice, spelling, and use of language. You should also proofread the essay to adhere to the style, organization, and presentation requirements.
Ensure that all the in-text citations are accounted for in the reference list and are up-to-date. You are good to go when you have an essay that meets all the instructions.
Finally, you can submit the paper for grading.
Writing is not everyone's cup of tea. For that reason, you can hire a nursing reflection essay writer from our website to assist you in crafting a top-grade paper. In addition, we have nursing writers whose forte is writing various nursing papers.
Choosing the suitable Reflective Model or Framework
As you can see above, many reflective models are used for your reflective essay. We have not exhaustively listed and expounded on all of them. Other reflective models and frameworks you can also consider when writing a reflective essay in nursing include:
- Bouds Reflective Model
- Brookfield Reflective Model
- Pender's Health Promotion Model
- Roper Logan and Tierney Model
- Driscoll Reflective Model
- The Johari window model
Note that most nursing instructors will often suggest the models they prefer for you to use in your essay.
For example, in most nursing reflective essays. Whichever the case, readily available information expands on each model to make it easier to write a reflection essay on a specific aspect of nursing education or practice.
Read the assignment rubric and instructions to understand the specific model. If it is unclear, ask for clarification from your instructor early enough.
Tips for Writing a Good Nursing Reflective Essay
As you try to figure out how to write a nursing reflective essay, keep the following tips in mind.
Choose the Right Topic
If the instructions from your professors involve choosing a topic for the reflective essay, you must select one that is meaningful to you.
This will ensure you can easily write and easily develop relevant elements about the topic. Therefore, take time to pick a topic that you find interesting.
As you write, ensure you stay on topic, whether sharing a one-off event or a recurrent story.
Use the Right Tone
A reflective essay is more personal, unlike other types of academic essays. This means you don't need a strict or formal tone.
Since this is about your experiences, use personal pronouns such as I and Me.
Be Vulnerable
You must be extremely vulnerable to learn how to write a reflective essay in nursing.
Be open about your thoughts, feelings, and beliefs about something you went through that sparked an interest in nursing.
It's okay to share mistakes or things you did wrong that eventually led you to this career path.
Choose the Right Focus
A reflection essay is all about narrating your experience during the nursing experience.
While including other people in your experience is okay, please let them not be the center of your reflection.
This is your essay, so you should be the focus of attention.
Keep it Brief
A good nursing reflection essay should be between 300 and 800 consciously written words. Because of this length, you must only write relevant information about your reflection. Refrain from lengthy reflections, as they make it difficult to pass your points across.
Convey Your Information Wisely
Even though a nursing reflection essay is about your personal experiences, it doesn't mean you should reveal everything about yourself. Ask yourself whether something is appropriate before including it in your paper.
Mistakes to Avoid When Writing a Reflection Essay in Nursing
A good reflection essay involves reflecting on your nursing studies and practices throughout school and career to demonstrate your competence. For this reason, there are certain mistakes you should be aware of when writing an essay.
Not including a Personal Story
Like food tastes bland without salt, so does a reflection essay without a personal story. At the center of a reflection essay is You. This means the essay should focus on your personal story that led you to want a nursing career. A lot of times, students miss out on this instead of talking about their story. You need more than just the personal qualities you think will be a great fit for the nursing program; you must also share a story that shows how well you contributed to nursing care.
Failing to Share Your Experience
You will lose points when you fail to include nursing-related experiences in your reflection essay. Mentioning that you want to be a nurse is great, but failing to show specific events that led to the desire will cost you a great point.
Plagiarizing Your Essay
Plagiarism is a serious academic offense because it is considered taking other people's ideas and using them as your own without crediting the author. So, provide relevant citations and references for any ideas that aren't your own. Also, an AI will not write your essay as a human writer would.
Related Readings:
- How to write a student nurse resume with no experience.
- PICOT examples and guides
Sample of a Nursing Reflective Essay
The following is a sample of a nursing Reflective essay using Gibb's Model of Reflection. Use this sample to guide you when writing your own.
Introduction Communication is an important element in healthcare practice as it determines patient satisfaction and treatment outcomes. This essay will focus on reflecting on an experience I went through with a 40-year-old diabetic patient who also had a foot infected with an ulcer. When I approached the patient to sign the consent form, I noticed that he wasn't happy because of the news given to him about his health. I concluded that there must be a communication dilemma. I will reflect on the experience using Gibb's Model of Reflection. Using this model, I will identify and discuss the actions taken to resolve the issue. Description This incident happened a few months ago when I was working as a wound nurse in a Methodist hospital in my hometown. I was part of a care team handling the case of a 40-year-old male patient with diabetes and an infected diabetic foot ulcer. After careful examination, a team comprising various specialists concluded that his leg needed amputation below the knee. After making this decision, the team left, and I was asked to give the patient a consent form to sign. When I came back from retrieving the form, I noticed the patient looked sorrowful because of the news given to him. Feelings As soon as I saw the patient, I knew what he was going through. He perceived the situation to be irreparable, but I wasn't sure whether to console the patient or not. I was powerless and couldn't imagine what he was going through. At the same time, I was startled that the team left without showing any compassion. They could have handled the situation more delicately. I, on the other hand, could have relayed the information better. I wasn't sure whether my approach would be acceptable or appropriate. Evaluation I always go back to that particular situation and wonder whether I could have acted better. The situation helped me better understand the importance of good communication in patient care, particularly in therapeutic care. Before the incident, I didn't acknowledge the role of nurses play in caring for patient's emotional needs. I realized nurses must show compassion and console patients in their low moments. Analysis Most healthcare professionals do not know how to deliver bad news to patients. They find the process extremely challenging and always feel psychologically unprepared. This has a negative impact on patients and could lead to bad health outcomes. Furthermore, how information is relayed could impact a patient's adherence to treatment. Because of these effects, multiple protocols and approaches were developed to help with communicating bad news to patients. One of the approaches that was proposed is emotion-centered. This proposes that a healthcare provider acknowledges how sad the patient is and builds a professional relationship based on empathy and sympathy. Action Plan I now understand the essence of communicating bad news with compassion. The experience allowed me to look closely at different aspects of my professional development that needed more improvement. Thus, I plan to be more empathetic and speak up in support of patient's emotional and psychological well-being, especially when presented with traumatic news about their health. Additionally, I now understand I am not powerless when dealing with a sorrowful patient. I believe I have learned from my experience, and I'm not able to communicate well with patients any more. Conclusion The experience allowed me to value good communication in nursing and the need to incorporate it into daily nurse-patient interaction. Nurses must learn how to deliver bad news and manage patient's sorrow. This has been and will continue to be my biggest priority in patient care. References Street Jr, R. L., Makoul, G., Arora, N. K., & Epstein, R. M. (2009). How does communication heal? Pathways linking clinicianpatient communication to health outcomes. Patient education and counselling, 74(3), 295-301. Buckman, R. (1992). Breaking bad news: why is it still so difficult? BMJ: British Medical Journal, 304(6842), 886. Ptacek, J. T., & Eberhardt, T. L. (1996). Breaking bad news: a review of the literature. The Journal of the American Medical Association, 276(6), 496-502.
Writing is not everyone's cup of tea. For that reason, you can hire a nursing reflection essay writer from NurseMyGrade to assist you in crafting a top-grade paper. In addition, we have nursing writers whose forte is writing various nursing papers. Just place an order , and we will get back to you ASAP.
Struggling with
Related Articles

How to Make SOAP Notes for a Nursing Class Assignment

Writing an Engaging Disusion Post/Response in Nursing School

Best Nursing Topics and Ideas for Presentations
NurseMyGrades is being relied upon by thousands of students worldwide to ace their nursing studies. We offer high quality sample papers that help students in their revision as well as helping them remain abreast of what is expected of them.
- LOGIN / FREE TRIAL

‘The challenges facing nurse education must be tackled’
STEVE FORD, EDITOR
- You are here: Students
‘Reflect on the importance of your words and actions’
14 January, 2022 By Chloe Hawkins

Development of communication skills is always an ongoing and ever-changing process, which all student nurses go through and continue with into qualified status.
The development of our communication skills is vital to ensure patient safety, allowing us to work within the remits of the Nursing and Midwifery Council (NMC) code. Without essential communication skills, how can we conduct complex and clinical tasks with our patients?
Communication skills are a core skill for any health professional. However, communicating with patients who may have severe communication difficulties can be difficult if the patient is unfamiliar to you.
Documents such as communication passports or hospital passports are a great tool to overcome barriers that may affect the effectiveness of the communication between yourself and your patient. When used, they are a valuable tool to enhance our understanding of the patient’s needs. Not to mention, the importance that family and carers hold within these situations – for example families and carers are best placed to recognise discomfort, pain and changes to the individual.
"Being able to appropriately communicate allows us to focus on our holistic approach and clinical interventions"
I take this opportunity to reflect on the opportunities I have had, to learn new communication skills and how they have broadened my skills and given me valuable opportunities to connect with patients. The experiences I have had to date have allowed me to build on my skills and recognise how I need to adapt for each individual patient. I was fortunate enough to undertake some Makaton training, which again has enhanced my ability to communicate with people and their families.
As a student nurse, being able to develop a rapport with both patients and their families and carers is a vital part of our learning experiences. Often, we learn new skills and gain new knowledge from these interactions.
Being able to appropriately communicate allows us to focus on our holistic approach and clinical interventions. Our experiences as students ultimately shape the knowledge and skills we develop upon as we transition into qualified nurse status, taking into account the NMC code and all relevant legislation and policies.
The importance of simulation learning for students also gives additional opportunity to practice and build upon our skills when communicating; it enhances our experiences on clinical placement and allows us to explore our own styles of communication. Simulation provides us with a structured and controlled environment to learn and develop.
My experiences of simulation to date have also allowed me to learn from others and have allowed me to develop in a way that allows me to appropriately reflect following this to enhance skills for the future. The support that students receive during simulation sessions helps shape and build our experiences and make for safe and positive learning experiences.
Understanding the importance of our words and our actions, and the impacts that they can have on people is a great area to reflect upon.
Chloe Hawkins is a second-year learning disability nursing student, Northumbria University and 2021-22 Nursing Times student editor
- Add to Bookmarks
Related articles

‘I know that this new chapter will bring new challenges’
Student editor Carly Davis reflects on her time at university as her time as a student midwife comes to an end.

‘The open meeting illuminated the dynamics of leadership and collective action’
Student editor Devansh Chiralayath Njalil Baburaj reflects on attending an open meeting at the Nursing and Midwifery Council.

‘Student nurses are struggling and something needs to be done’
Student editor Lucy Allen on the pressures that students face at the moment.
‘We can be part of the change to reduce the incidence of birth trauma’
Student editor Carly Davis on the recent inquiry investigating birth trauma.
One comment
Chloe Hawkins is very intelligent young lady. i always read her articles. well done Chloe it wouldn’t be long before you become band 8.
Have your say
Sign in or Register a new account to join the discussion.

How to Write a Nursing Reflective Essay as a BSN Nursing Student
- November 29, 2023
Welcome to NursingWriters.net, your go-to resource for expert information and guidance on writing nursing essays. In this article, we will provide you, as a BSN nursing student , with a comprehensive guide on how to write a compelling nursing reflective essay. Reflective essays are a personal reflection on your experiences in the nursing profession, and we are here to help you navigate this writing challenge.
As a busy nursing student, we understand that you may have limited time to spare. That’s where NursingWriters.net comes in, empowering you to excel in your BSN program by providing expert guidance on different writing and comprehension challenges you may face. Let’s dive into the world of nursing reflective essays and discover how you can effectively express your thoughts and insights.
Key Takeaways:
- Reflective essays allow nursing students to reflect on their experiences and personal growth in the profession.
- A nursing reflective essay is different from a personal statement, focusing on self-reflection rather than academic achievements.
- Key elements to include in a nursing reflective essay are the inciting incident, personal reflections, vivid details, and actions taken.
- The introduction should grab the reader’s attention and provide a clear thesis statement.
- The body paragraphs should delve into the writer’s reflections and emotions with specific examples and anecdotes.
What Is a Reflective Essay in Nursing?
A reflective essay in nursing is a powerful tool that allows nursing students to analyze their experiences, emotions, and actions related to their nursing practice. It provides an opportunity for self-reflection, critical thinking, and personal growth. Reflective writing can help nurses develop a deeper understanding of their own practice, improve patient care, and enhance their professional development.
Reflective essays in nursing differ from personal statements in that they focus on specific experiences and their impact on the writer’s growth and development. These essays require the writer to critically reflect on their actions, emotions, and thoughts, and identify ways to improve their practice. By examining their experiences and applying reflective frameworks, nursing students can gain valuable insights into their strengths, weaknesses, and areas for growth.
When writing a reflective essay in nursing , it is important to follow a structured approach. This includes describing the incident or experience, analyzing personal thoughts and feelings, exploring the actions taken, and reflecting on the outcomes and implications. By structuring the essay effectively, nursing students can communicate their reflections in a clear and organized manner.
| Key Takeaways: |
|---|
| – Reflective essays in nursing allow nursing students to analyze their experiences and emotions in relation to their practice. |
| – These essays focus on specific incidents or experiences and their impact on the writer’s growth and development. |
| – When writing a , it is important to follow a structured approach to effectively communicate reflections. |
Key Elements to Include in a Nursing Reflective Essay
When writing a nursing reflective essay, it is important to include key elements that will make your essay comprehensive and impactful. These elements will help you convey your thoughts and experiences clearly, allowing the reader to gain a deeper understanding of your reflections on nursing practice.
Inciting Incident or Event
The first key element to include in your nursing reflective essay is the inciting incident or event. This is the moment or experience that triggered your reflection and made a significant impact on your practice. It could be a challenging patient encounter, an ethical dilemma, or a personal realization. By describing this event in detail, you set the stage for your reflective journey.
Personal Reflections
Your nursing reflective essay should also include personal reflections on the experience. This is where you delve into your thoughts, feelings, and emotions related to the inciting incident. Reflect on how the event made you feel, what you learned from it, and how it has influenced your growth as a nursing professional. Be honest and vulnerable in your reflections, as this will allow the reader to connect with your experience on a deeper level.
Vivid Setting and Descriptive Details
To create a vivid and engaging narrative, include specific details that paint a picture of the setting and the people involved. Describe the physical environment, the interactions between healthcare professionals and patients, and any other relevant details that contribute to the overall context of the experience. This will help the reader visualize the situation and understand the complexities of the event.
Actions Taken
Finally, it is important to describe the actions you took in response to the inciting incident. Discuss how you applied your nursing knowledge and skills to address the challenges or opportunities presented by the event. Reflect on the effectiveness of your actions and whether there were any areas for improvement. This demonstrates your ability to critically analyze your own practice and make informed decisions.
By including these key elements in your nursing reflective essay, you can create a comprehensive and impactful piece of writing that showcases your growth and development as a nursing professional.
How to Write the Introduction of a Nursing Reflective Essay
The introduction of a nursing reflective essay plays a crucial role in capturing the reader’s attention and setting the tone for the entire essay. It should provide a concise overview of the main points that will be discussed and create a sense of curiosity and engagement. Here are some tips to help you write an effective introduction for your nursing reflective essay:
- Start with an intriguing opening line: Begin your introduction with a captivating statement or anecdote that relates to the topic of your essay. This will grab the reader’s attention and make them eager to continue reading.
- Provide context and background information: Give a brief overview of the event or experience that you will be reflecting on in your essay. This will help the reader understand the context and significance of your reflections.
- Present a clear thesis statement: Your thesis statement should clearly state the main purpose of your essay and the specific points or themes that you will be exploring. This will give the reader a preview of what to expect in the body of the essay.
By following these tips, you can craft an introduction that captivates the reader and sets the stage for a compelling nursing reflective essay.
“As I walked into the busy hospital ward on my first day of clinical rotation, I couldn’t help but feel a mix of excitement and nervousness. Little did I know that this experience would become a pivotal moment in my nursing journey, shaping my understanding of empathy, communication, and patient-centered care. In this reflective essay, I will delve into the details of this encounter and explore the personal and professional growth that resulted from it.”
With an attention-grabbing opening, providing context, and presenting a clear thesis statement, your introduction will set the stage for a compelling nursing reflective essay that captures the reader’s attention and lays the foundation for your reflections.
Nursing Reflection Essay Tips and Examples
Writing a nursing reflective essay requires careful consideration and thoughtful analysis. Here are some tips to help you craft an impactful and meaningful reflection essay as a BSN nursing student . Additionally, we will provide examples to illustrate how these tips can be applied.
Tips for Writing a Nursing Reflection Essay:
- Start by choosing a specific experience or event that had a significant impact on your nursing practice. This could be a challenging patient encounter, a critical incident, or a personal realization that transformed your perspective.
- Reflect on the experience and consider how it affected your emotions, thoughts, and actions. What did you learn from the experience? How has it shaped your growth as a nursing professional?
- Focus on the key aspects of the experience that were particularly impactful or meaningful to you. Avoid including unnecessary details or deviating from the main message of your reflection.
- Use specific examples, anecdotes, or patient scenarios to support your reflections. This will make your essay more engaging and relatable to the reader.
- Consider the ethical implications of the experience and reflect on how it has influenced your approach to patient care and decision-making.
- End your essay with a reflection on the implications of your learning for future nursing practice. How will you apply the lessons learned to provide better care and improve patient outcomes?
Now, let’s take a look at two examples of nursing reflective essays to further illustrate these tips:
“During my clinical rotation in the Intensive Care Unit (ICU), I encountered a complex patient case that challenged my critical thinking skills and decision-making abilities. The patient was a middle-aged woman who had undergone a complicated surgery and experienced numerous post-operative complications. This experience taught me the importance of collaboration within the healthcare team and the significance of advocating for the patient’s best interests…”
“One of the most significant experiences during my nursing education was my time spent in the pediatric oncology unit. Witnessing the resilience and bravery of children facing life-threatening illnesses had a profound impact on my perspective as a nurse. It taught me the importance of providing holistic care, not only addressing physical needs but also supporting emotional well-being and promoting a positive environment for healing…”
These examples demonstrate how personal reflections, specific details, and professional insights can be incorporated to create a compelling nursing reflective essay. Remember to structure your essay in a clear and organized manner, ensuring that your reflections flow logically and coherently.
| Key Elements | Example 1 | Example 2 |
|---|---|---|
| Inciting Incident | Complex patient case in the ICU | Experience in pediatric oncology unit |
| Reflections | Importance of collaboration and advocacy | Focusing on holistic care and emotional well-being |
| Specific Details | Complications post-surgery | Resilience of children facing life-threatening illnesses |
| Professional Insights | Importance of critical thinking and decision-making | Promoting positive healing environment |
By following these tips and utilizing examples, you can create a compelling nursing reflective essay that showcases your growth and development as a nursing professional.
How to Conclude a Nursing Reflective Essay
The conclusion of a nursing reflective essay serves as the final reflection on the writer’s growth and learning from the experience. It is an essential part of the essay that summarizes the main points discussed and leaves a lasting impression on the reader. The reflective essay conclusion should bring closure to the essay by restating the thesis statement and highlighting the key takeaways from the essay.
To write a strong and impactful conclusion, start by restating the thesis statement in a clear and concise manner. This reminds the reader of the main focus of the essay and reinforces its significance. Next, summarize the key points discussed in the body paragraphs, highlighting the most important insights and reflections. This helps to reinforce the main ideas and ensures that they are not overlooked in the final reflection.
In addition to summarizing the main points, a thought-provoking statement or future outlook can be included to provide a sense of closure and leave the reader with something to ponder. This can be a reflection on how the experience has influenced the writer’s future practice or a call to action for continued personal and professional growth. By ending the essay on a strong and meaningful note, the conclusion enhances the overall impact of the nursing reflective essay.
A well-crafted conclusion is essential for a nursing reflective essay as it reinforces the main ideas, leaves a lasting impression on the reader, and provides a sense of closure. By following these tips, nursing students can create a powerful and impactful conclusion that enhances the overall effectiveness of their reflective essays.
Tips for Writing a Nursing Reflective Essay
Writing a nursing reflective essay can be a challenging task, but with the right approach, it can also be a rewarding experience. Here are some helpful tips and strategies to guide nursing students in their essay writing process:
- Start early: Give yourself plenty of time to brainstorm ideas, reflect on your experiences, and write and revise your essay. Starting early will help you avoid last-minute stress and allow for a more thoughtful and polished essay.
- Conduct thorough self-reflection: Before you begin writing, take the time to reflect on your experiences and emotions related to your nursing practice. Consider how these experiences have shaped your growth and development as a nurse, and what lessons you have learned along the way.
- Organize your thoughts and ideas: Create an outline or a rough structure for your essay to ensure a logical flow of ideas. Group similar thoughts and reflections together to create cohesive paragraphs, and use headings or subheadings to further organize your essay.
- Seek feedback: Share your essay with trusted peers or instructors and ask for their feedback. They can offer valuable insights, provide constructive criticism, and help you refine your essay to make it stronger and more impactful.
Additionally, it is important to pay attention to the technical aspects of your essay:
- Grammar and spelling: Proofread your essay carefully to ensure it is free of any grammatical or spelling errors. Use grammar and spell-check tools, and consider asking someone else to review your essay for a fresh perspective.
- Coherent writing style: Use clear and concise language to convey your thoughts and reflections. Avoid excessive jargon or technical terms, and focus on communicating your ideas effectively.
- Formatting guidelines: Follow any formatting guidelines provided by your instructor or institution. Pay attention to font style, size, spacing, and citation style if required.
By following these tips and strategies, nursing students can approach their reflective essay writing with confidence and produce compelling and insightful essays that showcase their growth and development in the nursing profession.
Reflective Tools and Models for Nursing Reflective Essays
Reflective tools and models can provide structure and guidance for nursing students when writing reflective essays. These tools help organize thoughts and experiences, allowing for a more comprehensive and meaningful reflection. By utilizing reflection models , nursing students can enhance their reflective writing skills and deepen their understanding of their own growth and development as healthcare professionals.
Gibbs’ Reflective Model
“Reflective practice is both an art and a science that requires ongoing commitment and practice.” – Gibbs
Gibbs’ Reflective Model is a widely used reflection framework in nursing. It consists of six stages: description, feelings, evaluation, analysis, conclusion, and action plan. This model encourages a structured approach to reflection, allowing the writer to systematically explore their thoughts and emotions, analyze the situation, and identify areas for improvement or further development.
Dewey’s Reflective Thinking Model
“We do not learn from experience, we learn from reflecting on experience.” – Dewey
Dewey’s Reflective Thinking Model focuses on the importance of reflection as a tool for learning and growth. It emphasizes the need to actively engage with experiences, thoughts, and emotions, and to critically evaluate them in order to gain deeper insights and understanding. This model encourages nursing students to think analytically and develop a continuous learning mindset.
Kolb Reflective Model
“Knowledge results from the combination of grasping experience and transforming it.” – Kolb
The Kolb Reflective Model is based on the concept of experiential learning. It consists of four stages: concrete experience, reflective observation, abstract conceptualization, and active experimentation. This model encourages nursing students to engage in a cyclical process of learning, where they actively participate in experiences, reflect on them, conceptualize their insights, and apply their learning in real-life situations.
Schön Reflective Model
“Reflection-in-action is the heart of the learning process.” – Schön
Schön Reflective Model emphasizes the importance of reflection in the midst of action. It focuses on the ability to think and adapt in real-time, making decisions based on professional knowledge and experiences. This model encourages nursing students to develop a reflective mindset that allows them to learn and grow while actively engaging in their practice.
| Name | Key Concepts | Stages |
|---|---|---|
| Gibbs’ Reflective Model | Structured reflection, comprehensive analysis | Description, Feelings, Evaluation, Analysis, Conclusion, Action Plan |
| Dewey’s Reflective Thinking Model | Active engagement, critical evaluation | Experience, Reflection, Interpretation, Evaluation |
| Kolb Reflective Model | Experiential learning, application of knowledge | Concrete Experience, Reflective Observation, Abstract Conceptualization, Active Experimentation |
| Schön Reflective Model | Reflection-in-action, adaptability | Reflection-in-Action, Reflection-on-Action |
Benefits of Reflective Writing in Nursing
Reflective writing plays a crucial role in nursing practice, offering numerous benefits for nursing students and professionals alike. By engaging in reflective writing, nurses can enhance their self-awareness, develop their critical thinking skills, and gain a deeper understanding of patient experiences. This section will explore the advantages of reflective writing in nursing and its significance in healthcare.
Enhanced Self-Awareness
Reflective writing fosters self-reflection, allowing nurses to examine their thoughts, emotions, and actions in various clinical situations. Through this process, they gain a deeper understanding of their strengths, weaknesses, and areas for improvement. This heightened self-awareness enables nurses to provide more effective and compassionate patient care, fostering a patient-centered approach.
Improved Critical Thinking
Reflective writing encourages nurses to think critically about their experiences and the impact of their actions. It requires them to analyze and evaluate the effectiveness of their decision-making and problem-solving skills. By reflecting on past experiences, nurses can identify areas where they can enhance their clinical practice and make informed decisions based on evidence and best practices.
Increased Empathy and Understanding
Through reflective writing, nurses develop a deeper empathy and understanding of patient experiences. By reflecting on their interactions with patients, nurses can recognize the emotions, fears, and challenges faced by individuals in their care. This increased empathy enables nurses to provide more holistic and patient-centered care, improving the overall healthcare experience for patients.
Continuous Professional Development
Reflective writing is an essential tool for nurses’ continuous professional development. It allows them to document their growth, learning, and achievements throughout their nursing career. By regularly engaging in reflective writing, nurses can identify areas for further development, set goals for improvement, and ensure they are providing the best possible care to their patients.
Overall, reflective writing in nursing is a powerful tool that empowers nurses to enhance their self-awareness, critical thinking skills, and empathy. By engaging in this practice, nurses can continuously improve their clinical practice, provide high-quality patient care, and contribute to the ongoing development of the nursing profession.
Nursing Reflective Essay Examples
Looking for inspiration for your nursing reflective essay? Here are some examples that showcase different experiences, reflections, and growth in the nursing profession.
| Topic | Key Reflections |
|---|---|
| Providing End-of-Life Care | The writer reflects on their emotions, challenges, and personal growth while caring for terminally ill patients. They explore the importance of empathy, communication, and self-care in delivering compassionate end-of-life care. |
| Topic | Key Reflections |
|---|---|
| Leadership in Nursing | The writer reflects on their experiences as a nurse leader, discussing effective leadership strategies, challenges faced, and the impact of their leadership style on the nursing team and patient outcomes. |
| Topic | Key Reflections |
|---|---|
| Dealing with Ethical Dilemmas | The writer reflects on a challenging ethical dilemma encountered in their nursing practice. They explore the ethical principles involved, their decision-making process, and the lessons learned from navigating complex ethical situations. |
These examples demonstrate how nursing reflective essays can provide valuable insights into personal experiences, reflections, and professional growth. They serve as excellent references to help nursing students develop their own reflective writing skills and gain a deeper understanding of the nursing profession.
Writing a Nursing Reflective Essay for Nursing School Application
A nursing reflective essay can be a powerful tool for nursing school applications. It allows applicants to showcase their self-awareness, critical thinking skills, and passion for the nursing profession. When writing a nursing reflective essay for a nursing school application, there are a few key tips to keep in mind.
Reflect on your passion for nursing
Start by reflecting on what drew you to the nursing profession and why you are passionate about it. Consider your personal experiences, such as volunteering or shadowing healthcare professionals, and how they have shaped your desire to become a nurse. Highlight your commitment to providing compassionate and quality patient care.
Share personal experiences in healthcare settings
Provide specific examples of your experiences in healthcare settings, such as clinical rotations or internships. Reflect on the challenges you faced, the lessons you learned, and how those experiences have impacted your growth and development as a future nurse. Discuss any significant interactions with patients, healthcare teams, or mentors that have shaped your understanding of the nursing profession.
Align with the nursing school’s values and mission
Research the nursing school’s values, mission, and educational philosophy. Ensure that your reflective essay aligns with these principles and demonstrates your commitment to the school’s mission. Use the nursing school’s prompts or essay questions as a guide to structure your essay and address the specific criteria they are looking for in applicants.
By following these tips, you can write a compelling nursing reflective essay that effectively conveys your passion for nursing, showcases your experiences, and aligns with the nursing school’s values. Remember to proofread your essay carefully for grammar and spelling errors and seek feedback from mentors or trusted individuals in the nursing profession to ensure your essay is clear, concise, and impactful.
| Nursing Reflective Essay for Nursing School Application Tips |
|---|
| Reflect on your passion for nursing |
| Share personal experiences in healthcare settings |
| Align with the nursing school’s values and mission |
(Table) Tips for Writing a Nursing Reflective Essay for Nursing School Application
Writing a nursing reflective essay can be a transformative experience for BSN nursing students. It allows them to gain valuable insight into their own growth and development as future healthcare professionals. Throughout this comprehensive guide, we have provided expert information and guidance on how to write a compelling nursing reflective essay.
By understanding the purpose of a reflective essay and the key elements to include, nursing students can effectively showcase their personal experiences and reflections. Incorporating reflection models such as Gibbs’ Reflective Model or Kolb Reflective Model can also provide structure and depth to their essays.
At NursingWriters.net, we are dedicated to empowering busy nurses and providing them with the tools they need to excel in their BSN programs. Whether it’s writing a reflective essay or any other writing challenge, we are here to support and guide nursing students towards success.
What is a nursing reflective essay?
A nursing reflective essay is a personal essay where the writer reflects on their own experiences and how those experiences have shaped their growth and development in the nursing profession.
How is a reflective essay in nursing different from a personal statement?
While a reflective essay in nursing focuses on the writer’s personal experiences and reflections, a personal statement is more of a formal document that highlights the writer’s qualifications, achievements, and future goals in the nursing profession.
What are the key elements to include in a nursing reflective essay?
The key elements to include in a nursing reflective essay are the inciting incident or event, personal reflections on the experience, specific details to create a vivid setting, and a description of the actions taken by the writer. It is important to avoid including academic details and excessive focus on emotions.
How should I write the introduction of a nursing reflective essay?
To write an engaging and informative introduction for a nursing reflective essay, you can grab the reader’s attention with an intriguing opening line, provide context and background information, and present a clear thesis statement. Focus on the specific event or experience that will be the main focus of the essay.
How should I structure the body paragraphs of a nursing reflective essay?
The body paragraphs of a nursing reflective essay should have a clear structure. Use the first paragraph to present the thesis statement and provide background information on the event. Use subsequent paragraphs to explore your reflections, emotions, and actions taken. Use specific examples and anecdotes to make the essay more engaging.

How should I conclude a nursing reflective essay?
To write a strong conclusion for a nursing reflective essay, you can summarize the main points discussed in the essay, provide a final reflection on your growth and learning from the experience, restate the thesis statement, and leave the reader with a thought-provoking statement or future outlook.
What are some tips for writing a nursing reflective essay?
Some tips for writing a nursing reflective essay include starting early, conducting thorough self-reflection, organizing your thoughts and ideas, and seeking feedback from peers or instructors. Pay attention to proper grammar and spelling, coherent writing style, and adhere to any formatting guidelines provided.
How can reflective tools and models help with nursing reflective essays?
Reflective tools and models provide structure and guidance for nursing students when writing reflective essays. Models such as Gibbs’ Reflective Model, Dewey’s Reflective Thinking Model, Kolb Reflective Model, and Schön Reflective Model can be used as frameworks for organizing thoughts and experiences in a nursing reflective essay.
What are the benefits of reflective writing in nursing?
Reflective writing in nursing offers benefits such as enhanced self-awareness, improved critical thinking skills, increased empathy and understanding of patient experiences, and continuous professional development. It promotes lifelong learning and helps improve patient care.
Where can I find nursing reflective essay examples?
You can find nursing reflective essay examples that showcase different experiences, reflections, and growth. These examples incorporate personal reflections, specific details, and professional insights into nursing practice. They demonstrate the diversity of topics and experiences that can be explored in nursing reflective essays.
How can I write a nursing reflective essay for nursing school applications?
To write a nursing reflective essay for nursing school applications, reflect on your passion for nursing, personal experiences in healthcare settings, and future goals in the nursing profession. Address specific prompts and align the content with the nursing school’s values and mission.
How can writing a nursing reflective essay benefit BSN nursing students?
Writing a nursing reflective essay allows BSN nursing students to gain insight into their own growth and development as future healthcare professionals. It helps improve critical thinking skills, self-awareness, and understanding of patient experiences. It also promotes continuous professional development.
Have a subject expert Write for You Now
Have a subject expert finish your paper for you, edit my paper for me, have an expert write your dissertation's chapter, table of contents.
- Our Guarantees
- Client Reviews
- Privacy Policy
- Terms and Conditions
Knowledge Base
- All Writing Guides
- Nursing Essay Writing Guides
- Topics Ideas
- Nursing Guides
- Nursing Exemplar Papers
- DNP Nursing Paper Examples
- MSN Nursing Paper Writing
Nursing Writers Service
- Write My Nursing Paper
- Nursing Paper Writers
- Nursing Assignment Writers
- Nursing research paper writers
- Nursing Paper Writing Services
- Online Nursing Papers
- Personal Nursing Philosophy Paper
- Nursing Paper Writing Services reviews
- Nursing School Paper Writing Service
- Nursing Research Paper Writing Service
- Nursing Paper Writing Service
- Research Paper Writing Service nurses
- Paper Writing Service Nursing
- Paper Writing Service Reddit nursing
- Paper Writing Service chamberlain nursing
Writing Tools
- Citation Generator
- Topic Generator
- Thesis Generator
- Sentence Rewriter
- Title Page Generator
- Research Paper Title Generator
Use our resources and guides to write perfect papers. You can use our writing service and order customized sample papers without plagiarism!
Disclaimer
NursingWriters.net helps students cope with college assignments and write papers on various topics. We deal with academic writing, creative writing, and non-word assignments.
All the materials from our website should be used with proper references. All the work should be used per the appropriate policies and applicable laws.
Our samples and other types of content are meant for research and reference purposes only. We are strongly against plagiarism and academic dishonesty.

✍️ Nursing Writers
Typically replies within minutes
Hey! 👋 Need help with an assignment?
WhatsApp Us
🟢 Online | Privacy policy
WhatsApp us
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now .
- Advanced Search
- Journal List
- J Caring Sci
- v.8(2); 2019 Jun
The Effect of Reflection on Nurse-Patient Communication Skills in Emergency Medical Centers
Bahman pangh.
1 Department of nursing, Faculty of Nursing and Midwifery, Golestan University of Medical Sciences, Gorgan, Golesatn, Iran
Leila Jouybari
2 Department of Family and Community Medicine, Faculty of Medicine, Golestan University of Medical Sciences, Gorgan, Golestan, Iran
Mohamad Ali Vakili
3 Department of Community Health Nursing, Nursing Research Center, Golestan University of Medical Sciences, Gorgan, Golestan, Iran
Akram Sanagoo
Aysheh torik.
4 Department of Women Affairs, Gomishan Government Office, Golestan, Iran
Introduction: Reflection is formed through deep reflection on the event or a certain clinical position. The aim of this study was to determine the effect of reflection on nurse-patient communication skills of nurses working in emergency departments.
Methods: This interventional study was conducted on intervention and control groups and with a pretest-posttest design. 142 nurses working in the emergency departments of hospitals affiliated to Golestan University of Medical Sciences were enrolled in the study in 2015, and randomly divided into two groups. During eight weeks of the study, the intervention group was asked to write their clinical experiences with regard to communication issues with their patients. Before the intervention, the communication skills of both groups were compared using a questionnaire. Data analysis was performed, using independent t-test, paired t-test, Mann-Whitney and Wilcoxon tests.
Results: Of the 142 nurses, 122 nurses had full participation. In the intervention group the mean scores of verbal communication skills, non-verbal communication skills, general communication skills and communication skills based on patient safety were statistically significant, but there was no significant difference in the control group.
Conclusion: The results showed that eight weeks of reflection by nurses is an effective intervention in dimensions of communication skills. We therefore suggest that a reflective writing be encouraged as a vital tool for improving communication competency among emergency department nurses.
Introduction
Communication skills are taught to nurses in the educational environment and are an important part of educational programs, but there are many concerns about communication weaknesses and lack of communication skills. 1 Some nursing experts believe that appropriate communication skills are the cornerstone of all nursing care activities, 2 resulting in improved patient care and professional development and personality growth of the nurses. 3
Effective communication has positive effects on the patients, including improved vital signs, decreased pain and anxiety, increased satisfaction, improved treatment outcomes, and enhanced participation in treatment programs. 4 The emergency room is the busiest and most serious part of any hospital. 5 And smooth and organized management of this department can save the lives of many patients. Therefore, in this environment, nurses should be equipped with different capabilities and skills to withstand the pressure and tension, among which communication skills are one of the most important. 6 Many qualitative and quantitative studies have evaluated the nurse-patient relationship. 7 In a study about nursing care in emergency units, communication has been introduced as one of the elements of care in the emergency room. Therefore, special attention should be paid to effective communication between nurses, patients, their companions, and other care providers in the emergency units. 6 Studies conducted in Iran show that the nurse-patient relationship is not quite effective and is even reported to be weak at times. 8 , 9
The art of reflection encourages the person to search for and evaluate solutions in equivocal and complicated situations. 10 The experience of utilizing the reflection process in a clinical setting causes a sense of ownership towards the created knowledge in nurses, because they achieve this knowledge through focusing on their own experience, using creative methods. 11 The process of reflection starts when the person refers to his/her own experience and recollects what has occurred, reconsiders the experience, and reevaluates it. 12 This effective strategy also improves critical thinking and problem-solving skills in nurses. 13 Reflection is regarded as a proof of professionalism and is used as a skill related to clinical performance and professional behavior. 14 Reflective thinking in recent years has been considered as a learning strategy for nursing students while not being used by novice nurses in practice. 15 Studies have suggested that reflective thinking as a skill should be learned and used continuously. 16 , 17 In general, nurses should know how to have reflection on their clinical performance and practice it regularly.Evidence suggests that nurses may not be able to recognize the effects of reflection thinking on their professional development. 18 It seems there are some organizational barriers to hinder the use of reflective thinking. 19 , 20 The study by Asselin and Fain on the effectiveness of a continuing education program using individual narratives and group discussion showed that many of the participants couldn’t complete the process of reflection process. 21 Kim and colleagues in their study about the effects of a work-based critical reflection program for novice nurses recommended doing similar research with larger and more diverse samples.
Considering the effect of reflection on enhancing clinical activities and the importance of communication skills in advancing the therapeutic objectives and patient satisfaction and because patients are in a state of suspension and abeyance in emergency units, the best of the staff should be employed in these wards. Since university students have been the main target group of the studies conducted in Iran, and there has been no empirical evidence on the outcomes of reflective thinking among nurses in the emergency department, in this research we aimed to evaluate the effect of reflection on nurse-patient communication skills in emergency units.
Materials and methods
This single-blind, randomized, controlled clinical trial was conducted in nurses working in Sayyad Shirazi and Panj-Azar educational hospitals and west healthcare centers (Aqqala Al Jalil Hospital, Bandar Torkaman Imam Khomeini Hospital, Kordkuy Amir-Al-Momenin Hospital, and Bandar-e Gaz Shohada Hospital) with two parallel arms in 2015. The protocol of the study was approved by the ethics Committee of Golestan University of Medical Sciences (code: R.GOUMS. REC. 1394.73) and registered in the Iranian Registry of Clinical Trials (IRCT201501277821N1). The inclusion criteria were a minimum of 6 months’ experience in the emergency units, holding B.Sc or M.Sc. Degrees in nursing, and a negative history of acute stressful events in the past six months (death of fist-degree relatives, use of drugs related to psychotic disorders).
Leaving the emergency units or working in other units for any reason during the study, acute physical or mental crisis during the study (death of relatives, divorce, hospitalization), and incomplete recording of the reflection notebook (less than 4 reflections) were regarded as the exclusion criteria of the study. The participants were given information on the protocol and aims of the study, data anonymity, and confidentiality of the results. Informed consent was obtained from all the participating nurses. The sample size of the study was calculated, using the following formula, considering a study conducted by Hemmati Maslakpak et al., 22 With regards to the above study and an estimate of 80-80% for desirable verbal and non-verbal communication in ICU nurses of Urmia (Iran), an increase of at least 20% in desirable verbal communication was expected to occur after the study. Therefore, considering P1=0.75 and P2=0.95, confidence interval of 95%, and power of 90%, 62 nurses were required in each group (a total of 124 nurses); however, all nurses were included in the study to increase the precision of the study. The participants were allocated to the intervention or control group, using random blocks with block sizes of 4 and 6 and an allocation ratio of 1:1. For allocation concealment, the type of intervention was written on a piece of paper, placed in dark envelopes and numbered sequentially.
The allocation sequencing was done by a person who was not involved in the recruitment, data collection, and analysis. If a participant met the inclusion criteria, his/her name was written on the envelope. The envelopes were opened by the researcher to allocate the participants to either the intervention or control group.
The census method was used to invite all eligible nurses (142 out of 158) who met the inclusion criteria to participate in the study. A random number table generated by the SPSS software was again used to allocate the nurses to intervention and control groups. After obtaining informed consents and before the intervention, the nurse-patient communication skills questionnaire developed by Hemmati Maslakpak et al., 22 was completed by the nurses in both groups. In their study the average content validity index (0.887) and reliability coefficient of the questionnaire (alpha-coronbach = 0.96) were confirmed. In the present study the total Cronbach's alpha coefficient of questionnaire was 0.919 and for different dimensions were as verbal: 0.884, non-verbal: 0.848, and patient-based safety skill: 96.03, which indicates an acceptable homogeneity.
The participants in both groups were requested to complete the questionnaire once more after eight weeks. Special notebooks were designed based on the Gibb’s reflective cycle, and were given to the intervention group for reflective writing. Code 0 was assigned to the control group (n=71) and code 1 was given to the intervention group (n=71). Blinding: This study was a single-blind trial; in other words, the research assistant who collected the questionnaires was not aware of the allocation. After coordination with the nursing office of the afore-mentioned health centers, the schedule of the rotating shifts of the nursing staff of emergency units was obtained and then a briefing session was held about the process of work. The participants completed the nurse-patient communication skills questionnaire. Nurses in the intervention group practiced reflection at least once a week for 8 weeks. Since the purpose of this study was not to analyze the participants' notes in detail, the handwritten notes were only checked for relevance in relation to the communication skills with patients. There was no specific guideline to determine the length of reflective writing and national and international studies have reported different periods, so their average was used in this study. In reflection, based on the Gibb’s model, although there is no need to require the participants to adopt a certain framework, the following guide may help a person organize their thoughts and feelings:
- What happened?
- What were your reactions and feelings?
- What was good or bad about the experience?
- What did you learn from this situation?
- What else could you do?
- What will you do if it occurs again? 23
According to the Gibb’s reflective cycle, the participants were asked to reflect on their clinical experiences and write their best and worst experience of communication with the patient and their companions, the most difficult moment, and the best moment. No intervention was applied in the control group. The participants completed the nurse-patient communication skills questionnaire before the study and also at the end of eight weeks, and then they were asked to complete the questionnaire. The collected data included demographic (age, sex, ethnicity, marital status) and occupational characteristics (work experience, type of employment, position, ward).
The questionnaire had three sections including verbal and non-verbal communication skills (21 questions) and patient safety-related communication skills (27 questions). The questions were scored, using a 5-point Likert scale as always (5 points), often (4 points), sometimes (3 points), rarely (2 points), and never (1 point).According to the total score, the verbal and non-verbal communication skills were categorized as weak (score: 21-48), moderate (score: 49-76), and good (score: 77-105), and patient safety-related communication skills were categorized as weak (score: 18-41), moderate (score: 42-65), and good (score: 66-90). A higher score indicated a better communication performance. The Cronbach’s alpha was 0.96 for the whole questionnaire, 0.87 for verbal communication section, 0.92 for non-verbal communication section, and 0.95 for patient safety-related communication section. 22 The SPSS software, version 13 (IBM, Armonk, NY, USA) was used for analysis. The Kolmogorov-Smirnov and Shapiro-Wilk tests were applied to evaluate data normality. To determine the difference between quantitative variables in each group, independent t-test and paired t-test were used if the data were distributed normally and Mann-Whitney and Wilcoxon tests were used if the data distribution was not normal. P- values less than 0.05 were considered significant
The present study was conducted from September 2015 until January 2016. Of 158 eligible nurses, 142 met the inclusion criteria of whom 71 were allocated to the intervention group and 71 were allocated to the control group. Finally, the data of 122 participants were analyzed ( Fig. 1 ). The mean age of the participants was 29.97 (6.14) years, with 64.5% of the nurses in the control group and 60% of the nurses in the intervention group being female. There was no significant difference in demographic characteristics between the two groups ( Table 1 ).

Flow chart of the participants through each
| | | ||
| Age | 29.93 (5.4) | 30.01 (6.83) | 0.64 |
| Work experience (yrs) | 6.24 (4.64) | 6.8 (5.74) | 0.96 |
| Work experience in emergency department (yrs) | 3.21 (2.89) | 4.03 (4.01) | 0.05 |
| Gender | 0.6 | ||
| Female | 36 (60) | 40 (64.5) | |
| Male | 22 (35.5) | 24 (40) | |
| Education | 0.99 | ||
| BSN | 59 (98.3) | 60 (96.8) | |
| MSN | 1 (1.17) | 2 (3.2) |
a Mean (SD), b Mann–Whitney U, c Chi square, d n (%), e Chi-square for trend, f Fisher's exact test
The Shapiro-Wilk test was used to evaluate the normal distribution of quantitative continuous variables. Age, total work experience in hospitals, work experience in the emergency units, and nurse-patient communication skills had a non-normal distribution (P>0.05). A significant difference was observed in the score of verbal communication skills before and after the intervention in the intervention group (P<0.001) while the difference was not significant in the control group (P<0.418).
The difference in the score of non-verbal communication skills before and after the intervention was significant in the intervention group (P<0.001) while no significant difference was observed in the control group (P<0.413).
Moreover, there was a significant difference in patient safety related communication skills before and after the intervention in the intervention group (P<0.001); however, the difference was not significant in the control group (P<0104).
In general, a significant difference was seen in the total score of communication skills before and after the intervention in the intervention group (P<0.001) while no significant difference was observed in the control group (P<0.872) ( Table 2 ).
| | | ||
| Verbal communication skill | |||
| Before intervention | 70.57 (12.97) | 80.30 (12.38) | 0.001 |
| After intervention | 91.25 (6.41) | 79.18 (10.63) | 0.001 |
| P | 0.001 | 0.41 | |
| Differences before and after the test | 20.67 (11.73) | -1.11 (10.78) | 0.001 |
| Non-verbal communication skills | |||
| Before intervention | 67.18 (14.92) | 77.62 (14.93) | 0.001 |
| After intervention | 89.21 (8.63) | 80.04 (11.12) | 0.001 |
| P | 0.001 | 0.24 | |
| Differences before and after the test | 22.03 (16.25) | 2.41 (16.51) | 0.001 |
| Communication skills based on patient safety | |||
| Before intervention | 65.34 (14.74) | 78.28 (12.01) | 0.001 |
| After intervention | 89.93 (6.61) | 75.89 (7.62) | 0.001 |
| P | 0.001 | 0.10 | |
| Differences before and after the test | 24.59 (16.14) | -2.8 (11.4) | 0.001 |
| Total communication skill | |||
| Before intervention | 69.28 (12.5) | 79.28 (12.18) | 0.001 |
| After intervention | 90.47 (6.22) | 79.51 (9.11) | 0.001 |
| P | 0.001 | 0.87 | |
| Differences before and after the test | 21.19 (12.04) | 0.23 (11.23) | 0.001 |
a Mann–Whitney U, b Wilcoxon
The main findings of this study show that the reflective writing had a positive effect on the nurses’ clinical communication abilities. A significant difference was observed in verbal, non-verbal, and patient safety-related communication skills before and after the intervention while the difference was insignificant in the control group.
This study assessed the effect of reflection on communication skills of clinical nurses for the first time in Iran. Most national studies on reflection, such as those conducted by Sedaghti et al., 24 Abedini et al., 25 and Dehghany et al., 26 have mainly been of observational types. Moreover, most of the studies investigating the nurses’ communication skills were descriptive or related to reflection in the students. The results of the present study are in line with previous research findings according to which work-based critical reflection program or reflective journaling by hospital nurses (through fellowship program) improved critical thinking skills, communication abilities, and job performance. 27 , 28
Fukui et al., showed that communication skills training improved the patients’ quality of life and increased the nurses’ job satisfaction. 29 With regards to weak communication skills in clinical environments and their potential effects on the nurses, interventions are required to enhance these skills. It seems that the traditional teaching methods are not effective enough. A study by Heaven et al., revealed that despite the effectiveness of educational workshop, it was comparatively less effective in clinical environment, indicating the need for more clinical supervision and intervention in practice. 29
Reflection enables the learners to search for their roles and responsibilities in an interdisciplinary context and enhance their verbal and teamwork skills. In the present study, among the three types of skills, verbal skills had the highest mean score after the intervention. Verbal communication skills are behaviors such as greetings, introducing to patients, and using open questions. It seems that the nurses had the highest score in their verbal skills because such behaviors are common in the practice.
The reflective writing helped nurses pay more attention to such apparently simple behaviors. Consequently, reflective thinking promoted positive social behaviors in communicating with their patients.
These findings are consistent with the results of a study by Lestander et al., in which the participants stated that their verbal communication skills with patients improved after three reflection sessions (two individual sessions and one group session), leading to their increased efficacy in the nursing profession. 30 A study by Pai et al., showed that simulated learning opportunities with feedback, debriefing, and guided reflection enhanced critical thinking, clinical judgment, verbal communication skills and caring skills. Therefore, self-reflection may play an effective role in improving the nurses’ verbal communication skills. 31 In that study, the participants also stated that reflective thinking helped them to use proper phrases to encourage patients to express their feelings or to try to provide training in plain and intelligible language. In a study by Abedini et al., on the effectiveness of reflection in clinical education, most of the students believed that reflection increased their communication and social skills. 25 Therefore, verbal skills are an important part of nurse-patient communication skills and accurate identification of factors affecting verbal skills is required to improve them. The results of the present study also showed the high score of non-verbal communication skills (such as proper eye contact with the patient, body gesture and head movements or listening to the patient) of the nurses working in the emergency rooms. In a study by Thomas et al., the majority of patients needed non-verbal communication. 32
Heinerichs et al., assessed the effect of non-verbal communication skills through videotaping and debriefing of clinical skills. The results showed non-verbal communication skills improved in 96% of the students and 98% of the students mentioned non-verbal communication skills as a proper means of communication. 33 Although, in the present study, before and after the intervention, the non-verbal communication skills of the nurses increased in the intervention and control groups, this difference was only significant in the intervention group, which could be due to the rethinking and contemplation of nurses in their daily experiences of communicate with patients. The results of the present study also showed that nurses had good patient safety-related communication skills. Similarly, the results of a study by Hemmati et al., showed that from the perspective of the nurses, patient safety was in a good level for most patients hospitalized in the intensive care units of educational hospitals. 22 However, some studies have reported contradictory results regarding patient safety. 33 , 34 The domain of patient safety-related communication skills has a direct association with clinical competency of the nurses and their professionalism, 27 which was significantly enhanced through reflection in our study. Pearson et al., noted that reflection by surgical residents improved their medical performance, communication, and professionalism. 35 Moghadami et al., evaluated the effect of reflection on nurse-patient communication skills in nursing students, but found no significant difference in the students’ therapeutic communication skills between the two groups. Although clinical reflection was associated with an increase in the mean score of therapeutic communication skills, the difference was not significant. 36 It is important for all nurses to possess communication abilities; therefore, those nurses working in the emergency unit are not exempt from this requirement. So, it is critical to help them improve their communication verbal and non-verbal abilities and patient safety through reflective writing, which is an easy and non-expensive approach.
The present study had certain limitations. Since the previous studies had not suggested a specific period for performing the narrative writing, a period of “eight weeks” was considered for the intervention based on the available evidence,. So it has to be admitted that a decrease or increase in this period could have been accompanied by other consequences not found in the present study. Due to mandatory rotating work shifts, the communication between the intervention and control groups was inevitable and there was a possibility of transmission of intervention into the control group. However, the fact that the participants had been selected from different hospitals (teaching hospitals, governmental hospitals), and from different cities of the same province can be considered as a strength of this research. Suggestions for further studies: It is suggested that in the future studies, the effect of group oral reflection on communication skills of nurses working in emergency units be investigated. Also, the effect of reflective narration on the patients’ safety and clinical errors and the other core clinical competencies can be studied. Exploring the effect of self-reflective narration through e-mail sounds interesting too. Implication for nursing: Every health care system should equip its nurses with good communication skills. Since reflective thinking leads to the development of critical thinking, it is expected that better decisions can be made by nurses in relation to patients, and better communications with patients can thus be established. It is, thus, recommended nurses’ administrators incorporate reflective writing into in-service training and use that as a tool for making sense in emergency units, learning and art in care practices.
The reflective writing not only had a positive effect on verbal, non-verbal and general communication skills, but also helped nurses to have better communication skills based on patient safety. In other words, reflection enables the nurses to support the patients more effectively in each stage and have a more prominent role in the health despite limitations in resources and the high work load. For these reasons, such a program could be considered an important tool for improving communication competency among nurses in emergency units. This educational approach emphasizes health, hopefulness, and positive thinking; therefore, it is consistent with the philosophy of nursing care and may be used in different situations like routine clinical care.
Acknowledgments
The authors wish to thank the education development center and deputy of Research, Golestan University of Medical Science, as well as the officials and emergency wards’ staff of the hospitals for their participations. This article was derived from a master thesis of at Golestan University of Medical Sciences, Gorgan, Iran.
Ethical issues
None to be declared.
Conflict of interest
The authors declare no conflict of interest in this study.
Citation: Pangh B, Jouybari L, Vakili MA, Sanagoo A, Torik A. The effect of reflection on nurse-patient communication skills in emergency medical centers. J Caring Sci 2019; 8 (2): 75-81. doi: 10.15171/jcs.2019.011 .
Nursing Reflective Essay: Examples + Useful Writing Tips [2024]
![student nurse reflective essay on communication Nursing Reflective Essay: Examples + Useful Writing Tips [2024]](https://studycorgi.com/wp-content/uploads/2022/04/medical-assistant-reading-book-elder-disabled-woman-nursing-home-senior-patient-sitting-wheelchair-receiving-assistance-support-from-nurse-as-entertainment-fun-activity-485x528.jpg)
Do you need to write a reflective nursing essay? Whether you are a nursing student or already working, we know that you may be too busy writing papers. We’ve prepared information for you about reflection models and nursing reflective essay examples, writing instructions, and templates for the outline. This article will teach everything you need to make writing your essay easier.
So, how do you write an academic reflective essay?
What Is a Reflective Essay?
15 best reflective essay topics: nursing, nursing reflective essay examples, reflective tools and models, reflective essay writing tips, reflective essay body paragraphs, how to conclude a reflective essay.
In a reflective essay, you express your thoughts based on your knowledge, beliefs, reflections, and experiences. A reflective essay is best described as an exceptional and personal essay: you will have a lot to think about, comprehend, and explain. You have to demonstrate the feelings that you have experienced before. It should be honest. If you have any opposing thoughts and feelings about the topic, you should write them.
| Criteria | Reflective essay | Analytical essay |
|---|---|---|
| Subject | Reflection on previous experiences | Analysis of a controversial topic |
| Writing style | Free and relaxed | Formal |
| Object | Personal experience | Depends on subject |
| Thesis statement | Focus on the narrative | Focus on the paper’s topic |
The peculiarity of a reflective essay, unlike an analytical one, is in the expression of thoughts based on personal experience.
How long does a reflective essay last? It’s simple. It depends on your topic and how you express your thoughts. But you have to remember that this is a highly brief type of essay, and you can do it with a few pages.
You can check out the 100% free essay samples to see it all.

What Is a Reflection in Nursing Essay?
Nursing involves many aspects of work, and reflection is one of the critical tools for developing professional competence and personal skills. In nursing, reflection is important because it provides all the prerequisites for further personal growth. It is a reflection that will allow you to take a broader look at your strengths and weaknesses and assess your prospects.
Think of your nursing reflective essay as a chance to reflect on your career, skills, and personality, which will lead to further improvement.
- Empathy and support in nursing.
- Communication with patients is one of a nurse’s most important tasks.
- Nursing is the art of caring for the patient during illness.
- The key is not to cause harm but to help afterward.
- Time management in nursing.
- The Patient’s Interests Come First.
- Why did I become a nurse?
- Doctor- patient confidentiality in nursing.
- The importance of enhancing soft skills for the nurse.
- Nursing knowledge should not be limited to narrowly professional information.
- Reflective essay on the internship .
- Nursing culture and ethics .
- Deontology of nursing and its synthesis with my personal experience.
- Nursing clinical reflection essay.
- Nursing issues for the elderly.
To better understand what reflexivity is, let’s look at examples based on these articles:
| The author considered the best competencies that fit her current and future goals. She discusses the skills acquired and draws conclusions. | |
| The author takes a reflection on the DNP course. Conclusions about specific skills support it. | |
| The author reflects on DNP Essentials, which is the author’s course. Reflection occurs in terms of its contribution to the author’s professional development. | |
| An example of the subject of leadership. The author took a course on reflective practice in nursing and discovered many new things. | |
| In this essay, the author reflects on her experiences and skills in the context of Capstone’s professional practice. The reflection occurs about oneself and concerning others involved in the practice. | |
| The author discusses the skills he learned while creating and launching his course for nurses. | |
| The author reflects on the experiences nurses have had due to taking his course and what is vital in nursing. | |
| The author reflects on her personal experience with the patient. Great for students who already have experience in the specialty. | |
| The author discusses the challenges nurses face and the ways to solve them. | |
| In this paper, the author discusses the goals, strategies, and other aspects of implementing artificial intelligence in nursing. | |
| This essay examines nursing philosophy and its relationship with individual values. | |
| In this essay, the author breaks down the benefits and disadvantages of introducing case management into nursing. | |
| The author explains how the Civil War in America changed the role of women in nursing. | |
| The author discusses the issue of bullying and violence in nursing and provides suggestions and reasons. | |
| This paper examines the functions such as hospital premises and toilet cleaning, which initially are not the responsibility of nurses, and other staff is to fulfill them. | |
| This evidence-based project presents data that aims to evaluate the efficiency of team-based anti-stress therapy sessions and compares it with standard self-care practices in a hospital setting. | |
| The author discusses the ways to reduce the pressure on nurses and reflects on personal experience. | |
| This paper breaks down the responsibilities of RNID. | |
| The author explains three strategies to create a well-developed portfolio for nurses. | |
| This short paper aims to discuss specific challenges and risks that nurses experience in work environments. |
Scientists from different fields of science invented many models to simplify the process of reflection. Below are reflection models you can use in your essay nursing writing practice.
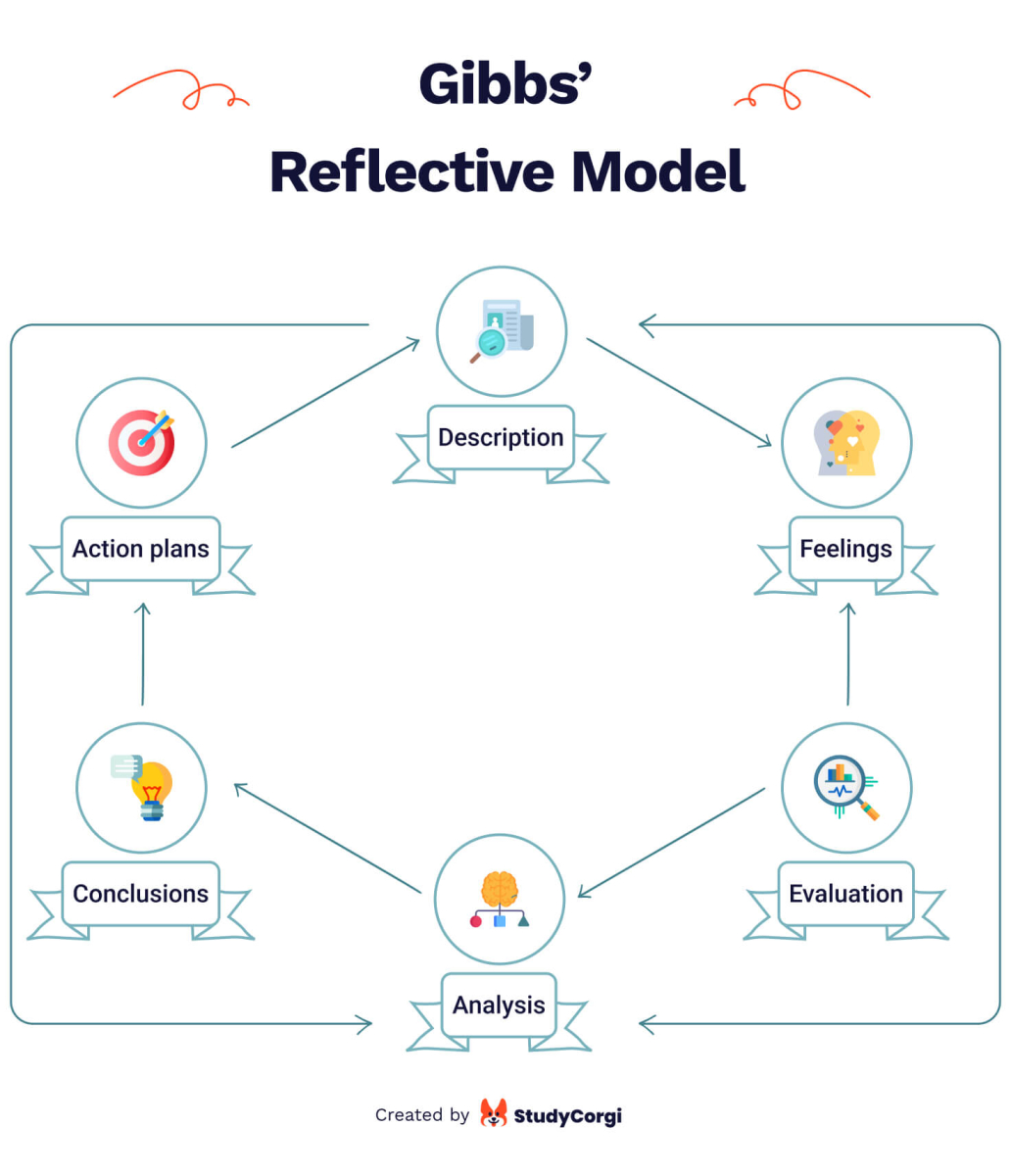
Gibbs’ Reflective Model
In 1998, Graham Gibbs introduced his reflexive model to the world. Gibbs’ model is a cycle and, therefore, excellent for analyzing repetitive experience.
It covers 6 stages:
- Description. What happened? Don’t judge or try to conclude yet; just describe.
- Feelings. What were your reactions and emotions? Again, don’t begin to analyze them yet.
- Evaluation. What was good or bad about the experience? Make value judgments.
- Analysis. Were different people’s experiences similar or different in importance?
- Conclusions. What conclusions can you draw in a general sense from this experience and your analysis? What conclusions can you draw about your particular, unique personal situation or way of working?
- Personal action plans. What steps are you going to take based on what you have learned? What are you going to do differently in this situation next time?
Dewey’s Reflective Thinking Model
John Dewey believed that reflective thinking is the active, persistent, and careful evaluation of a belief or assumed form of knowledge, the grounds for that knowledge, and the additional conclusions to which knowledge leads.
John Dewey’s Reflective Model was one of the first and has been the foundation for many other models. He identified five steps of reflective thinking:
- Step 1: Identify the problem.
- Step 2: Investigate the issue.
- Step 3: Generate several possible solutions.
- Step 4: Evaluate the options and select the best answer from the combination of solutions.
- Step 5: Test and implement the solution.
Kolb Reflective Model
The Kolb Reflective Model or “Kolb cycle” focuses on transforming information into knowledge. The basic four steps of the Kolb model are as follows:
- Concrete experience. Anyone should already have experience in the field or area they want to learn.
- Observation and reflection . This stage implies analyzing the person’s experience and knowledge .
- Forming abstract concepts . A model describing the information and expertise is built at this stage . Ideas are generated, interrelations are made, and new information is added concerning how everything works and is arranged.
- Testing in new situations . The last stage implies experimentation and testing the model’s applicability and concept . The result of this stage is a direct unique experience. Then the circle closes.
Schön Reflective Model
Donald Schön’s reflexive model was described in the book ‘ The Reflexive Practitioner .’ He explained how professionals solve problems with a kind of improvisation that is perfected through practice.
Schön’s reflective model , like his writings, is based in many ways on the Dewey we already know
- Action reflection involves reflecting on an experience you have already had or an action you have already taken. It involves considering what could have been done differently and the positive aspects of that interaction.
- Reflection in action involves reflecting on your efforts as you make them and considering issues such as best practices throughout the process.
Bouds Reflective Model
David Bouds paired with Schön to explore the limits of reflective practice. This model is based on learning by doing. By analyzing his own experience, the practitioner begins to understand better how to improve certain things.
Bouds suggests that by reflecting, a person may be unconsciously learning. In reassessing the events of his life, he systematizes and classifies emotions, ideas, and results, as well as results, and compares past goals with results.
Past experiences, experiences, and ideas require constant analysis attention to feelings. This leads to new perspectives, commitment to action overall positive changes in behavior.

Driscoll Reflective Model
John Driskoll proposed a simple model of reflection at the beginning of the 21st century. It involves reflection through extended answers to questions we are already familiar with. The scholar linked the three basic questions to the stages of the experiential learning cycle and then added trigger questions that must be answered to complete the process of reflection.
Step 1: What? Sets out to recall what happened as objectively as possible, without criticizing anything that happened
- What exactly happened?
- What exactly did you do?
- Was anyone else involved?
- Was it a good experience? Or a bad experience? Or both? And why?
Step 2: So what? It requires you to slow down and start looking for patterns or meaningful moments. The key here is to bring in concepts that help shed light on what is going on.
- How did you feel at that particular moment?
- How did you react?
- Why did you react that way?
- Did you feel the same way about the situation then as you do now?
- Did you experience conflict with your values?
- Do you think past cases influenced your experiences in this situation?
- Who else was involved in the situation? How did they feel? And how did they react? And why did they react that way?
Step 3: Now what? Encourages beginning to transfer new knowledge into future situations and other contexts.
- What did you learn from reflecting on this situation/experience/incident?
- Could you have prevented the negative consequences?
- And how might you have done so?
- What would you have done differently if a similar situation arose in the future?
- What could you have done to better prepare for it?
- Where did things go wrong last time, and what would you focus on now?
5R Framework
The 5R Framework was developed in 2002 by a group of scientists as a universal system of reflection, later modified.
It focuses on five basic steps, each addressing one aspect of reflection. Thinking through the five stages, an individual will engage all of the major reflection components, allowing you to create a critically meaningful review based on your experience.
- Report. What do you see and hear? Write it all down.
- React. What do you think is happening? What works well and what doesn’t? How do you feel about the situation you are reflecting on? What is it about this situation that makes you feel this way?
- Relate. How do my perceptions of this situation relate to my personal and professional experiences? How do they relate to my knowledge and skills? Through what “lens” do you view this situation? From the perspective of classroom management or collaborative learning? Do you need professional development in terms of content knowledge?
- Reason. Do you relate your point of view to someone else’s and how it affects the situation? Does sound practice support your strategies, or do you use different approaches? How does your point of view affect how you understand the problem? Could another point of view be helpful?
- Reconstruct. What did you learn from this observation, and how will it affect your practice?
CARL framework
The CARL framework of reflection involves going through four stages: context, action, results, and learning. The vastness of this model gives a lot of information, and even at the first stage, you can already get a lot of valuable data. But this is also its main disadvantage because it makes the model more complex.
The framework has four steps:
- Context : Description of the context of the experience.
- Action : Explanation of the action taken.
- Results : Explanation of what your actions led to.
- Learning : Identification of the experience and knowledge gained.
Now that we’ve covered the basic concepts let’s write a reflective nursing essay.
Reflective Essay Outline
How to make a reflective essay? First, write an outline.
Any reflective essay is a statement of thoughts about something, and the outline acts as a sketch in which you write them down. Creating it is the first step to creating high quality and vivid essay.
What would make a good outline structure for a reflection essay? Structure all your knowledge. Write what you want to see in the introduction, body, and conclusion.
Here is the reflective essay outline template:
- Hook: Use a catchy statement to set the tone and introduce the article.
- Mention the main points.
- Thesis statement: Include all the important points and ideas in one statement.
- Topic sentence: Carefully explain the first idea in one sentence.
- Proof of topic or idea: Use authoritative sources to support the idea.
- Idea analysis: Apply logic and rational thought to the idea and information from the source.
- Topic sentence: Carefully explain the second idea in one sentence.
- Topic sentence: Carefully explain the third idea in one sentence.
- Repeat the statement of the thesis.
- Review the main ideas
- Final, concluding sentence
Reflective Essay Thesis
A thesis statement is a condensed version of the paper in which you must briefly explain your position. The point is for your audience to read it and understand your work.
To make a good thesis statement for a reflective essay, you need to formulate your thought on paper. To begin with, think well about the problem, and develop your attitude toward it. That’s why the thesis statement should be created after writing the outline. It is unnecessary to give everything out in advance to the reader because later, you will unfold this thought more broadly.
After successfully developing the thesis statement, you can proceed to the actual writing.
And so, below, you can see examples of the reflective essay introduction and conclusion. Learn what its body of it is.
How to Start a Reflective Essay? Examples
You need to start any paper in the right way. How to write a reflective essay introduction? Check these examples:
- Practice and theory do not always agree. Not all of the medical reference books that I have been able to study are fully applicable in practice. John Kimble’s case is a testament that it is often necessary to rely on them and consider the specific situation. He complained of dizziness, and the doctors advised him to get a blood iron test. The test showed that there was nothing wrong. But as it turned out later, this was an erroneous result because Kimble had eaten redfish rich in iron the day before, which temporarily raised the iron in his blood.
- I had always dreamed of becoming a nurse, but my fear of blood robbed me of all desire to study. But still, my passion and ambition made me pull my will into a fist. I had to change and forget what fear of blood was. I lived my dream, which helped me overcome one of my fears.
- A few years ago, I went through a severe emotional crisis. I had always dreamed of going to the University of California, as it is one of the most prestigious medical universities in the United States. But unfortunately, I failed my entrance exams, so I had to study at the university in my hometown. My failure seemed like a disaster, but now I realize it was a real blessing.
The essay’s body carries arguments, explanations of the topic, and the main body of information.
Each paragraph should begin with short introductory sentences, and the body of the sections should be divided into several parts. This will help you better structure what you have written and help the reader navigate through the text.
It is worth remembering about argumentation. There should be several things that you rely on in your position. Describe each of them in detail in a separate paragraph. Observe the semantic sequence. A mistake, in this case, will be to repeat twice the same argument in different words. It will give the reader the impression that there is nothing to say.
You should also remember about transitions in a reflective essay. Move smoothly from one aspect to another and take your time.
How to end a reflective essay? In conclusion, you should focus on pulling together all of the material, summarizing all of the points made and what you have learned. Try to include a few moments about why and how your attitudes and behaviors changed. Here are some examples:
- Was the practice of volunteer nursing helpful to me? Absolutely! I was grateful for these weeks because I learned a lot. But most of all, I have learned my Soft skills, which will help me get used to my professional activities.
- At that moment, I thought about who would be the priority in that situation, and I still believe it was the patient. If the same problem were to arise again, I think I would do nothing but speak up and justify my decisions. I recognize and know that time management and prioritization are essential skills in nursing, and I hope that my skills will improve with practice.
- I reflected on how personal values can affect professional practice from the incident. Still, it is crucial to consider that the organization has its own set of values to follow, regardless of personal values. Finally, in reflecting on the incident, I was able to discuss the importance of quality assurance monitoring and health care evaluation both in general and during the incident, which allowed me to consider what conclusions were drawn from the incident and how to prevent similar situations occurring again.
So, now you have examples and an idea for writing a reflective nursing essay. Writing your paper will become many times easier and faster.
If this article was helpful, share it with your friends and colleagues!
❓ What Is the Purpose of Writing a Reflective Essay?
A reflective essay aims to express one’s thoughts about a previous experience, including how one changed in the process and what one learned. It is often described in a diary entry; they are intended to demonstrate how the author’s thoughts have changed over time.
❓ What Makes a Good Reflective Essay?
A reflective essay is a combination of both objective and subjective elements. We mix scholarly analysis with personal experiences. This type of paper should explain to readers how our experience influences our behavior and what lessons we learned.
❓ What Are the 3 Basic Parts of Reflection Paper?
An essay should have a clear structure and must contain three parts. It should have a clear introduction reflecting the problem, then the central part with an analysis of the causes, and the conclusion with possible solutions to the problem or how it affected the author.
❓ What Is the Best Reflective Model to Use in Nursing?
One of the best options for nurses is the Gibbs model. The model is accessible and extremely simple. Therefore it can be operated without any problems in any situation.
- Reflection toolkit: The University of Edinburgh
- Essay Conclusions: University of Maryland
- Thesis Statements: UNC Writing Center
- A short guide to reflective writing: University of Birmingham
- Outlining: Harvard College Writing Center
- Reflective Practice in Nursing: ZU
- Critical self-reflection for nurse education: NCBI
- Essay Structure: Harvard College Writing Center
- Essay Structure: UAGC Writing Center
- General tips for academic reflections: The University Of Edinburgh
- Reflective essays – ANU
- Writing An Essay Title – Illinois Valley Community College
- Nursing Essay Help: Medical Essay Writing Service in UK
Using Scholarly Articles as Sources: A How-to Guide
30 google search tips & tricks for students, learning to write shorthand: the complete guide for students, infographics for students: the complete guide, step-by-step guide on how to write an opinion essay + examples, coping with culture shock: a guide for international students.
The NMC website will be unavailable from 07:15 - 10:00 on Saturday 14 September whilst we carry out essential maintenance. NMC Online will be available as normal. Apologies for any inconvenience caused.
- Latest hearings
First year student nurse, Emma
Practice learning experience case scenario in an acute hospital setting
- Second year student nurse, Saima
- Third year student nurse, Darren
The focus of this scenario is the learning that Emma, a first-year student nurse undertook while on a shift during her fifth week of a ten-week placement on ward A.
Emma’s key objectives during this placement were:
- To develop effective communication and relationship management skills
- To acquire skills and knowledge for post-operative care, specifically pain management, vital signs, and fluid balance.
- To undertake wound care and assessment
This is Emma’s second placement, her first had been on a medical assessment unit.
Emma is joined on this shift by:
- Grace, a registered nurse (RN), practice supervisor to Darren, Saima and Emma
- Darren: a third-year student nurse who is coordinating the care on the bay and acting as practice supervisor for Saima under the supervision of Grace
- Saima, a second-year student nurse
- Colin: a Health Care Assistant (HCA)
Emma has a practice assessor Sarah, who is not on duty today
Planning for her shift
Emma was allocated to work with Janet, as she had cared for her during her last shift, in the immediate post-operative period.
Emma's patient
Female, aged 67
Total abdominal hysterectomy two days ago for cancer
Has a 10cm abdominal surgical wound, closed with clips, theatre dressing intact and due to be reviewed today
Urinary catheter removed earlier today
Lives at home and is a full-time carer to her husband, Robert, who has disabilities
Janet is experiencing a lot of pain and feeling nauseous
She is feeling extremely anxious and scared about both her diagnosis and how her husband is doing
Diagnosed with cancer only two weeks ago after experiencing weight loss and fatigue.
Emma introduced herself, asking Janet if she required assistance with her personal hygiene needs, and if she could look at her wound and dressing. Janet appeared appreciative of this request, and she readily accepted. Emma took careful consideration of Janet’s privacy and dignity and encouraged her to do as much as she could for herself.
While Emma is assisting her, Janet discloses that she is feeling anxious about her diagnosis and how her husband is coping at home. Emma also noticed that Janet was in considerable discomfort and that her dressing was soiled with exudate. Emma, documented her observations, recording information concerning nutrition, fluids and skin care. Grace agreed with Emma’s records.
Putting the proficiencies into practice
The Standards of proficiency for registered nurses list the knowledge, skills and behaviours that every nurse must have by the end of their programme.
The standards are set out in seven sections called 'platforms'.
There are two annexes in these standards that list the skills nurses must have, and the procedures they must be able to do when they join our register.
One focuses on communication and relationship skills, and the other on nursing procedures.
Through some examples see how Emma was able to demonstrate certain outcomes of these proficiencies through her learning experiences.
What Emma did
Emma recognised and acknowledged that Janet was in pain and a discussion took place with Grace regarding evidence-based medicines and options to reduce her pain. Emma reflected on the World Health Organisation (WHO) pain ladder and the ‘gate control theory’ of pain; specifically, around the part that anxiety plays in the pain experience. This informed the pain assessment she carried out and Emma took time to actively listen to Janet to understand her pain and the source of her anxieties.
Emma spent time getting to know Janet and with her involvement developed and agreed strategies to support her. She noticed that Janet communicated openly when she was being helped with a wash; recognising that the privacy and intimacy in this situation helped Janet trust Emma to talk about how she was feeling. She took her time assisting Janet and made sure that she continued to feel able to be open about her concerns.
With Grace’s support and with Janet’s agreement Emma contacted social services to discuss Janet’s husband Robert and to ensure that he was receiving the support and care that was sufficient to meet his needs and enable him to stay at home. Emma explored the possibility of Robert visiting Janet, she was aware that they had been married for 40 years and had never been apart. Emma suggested that this could take place at a mealtime so they could enjoy eating together. Janet had mentioned that one of her main concerns was that Robert was not eating properly when she wasn’t there.
During the multidisciplinary round Emma was able to contribute, reporting that Janet had passed urine since her catheter was removed and that the team would be reviewing Janet’s pain as she continued to have difficulties, especially when she moved. This was important and needed to be prioritised as it had the potential to affect her recovery and delay the plans for discharge (also see Annexe B below).
Emma and Grace discussed how many people with abdominal wounds are anxious about this when moving and walking; Grace asked Emma to reflect on the importance of mobility and showed her how to support Janet’s abdomen with a pillow and to take some deep breaths to improve her parasympathetic nervous system.
What this demonstrated
Emma applied her learning about person centred communication and pain management to support Janet. She developed a good rapport enabling Janet to trust Emma to disclose her anxieties. Emma was able draw on her knowledge and experiences, thinking critically about Janet’s care, putting her preferences and needs first.
Emma demonstrated knowledge and confidence to communicate and manage relationships effectively with Janet and in the multidisciplinary team.
Emma reflected on Janet’s recent diagnosis of cancer and how she had delayed seeking help for her symptoms as she was busy caring for her husband. She discussed this with her supervisor Grace and ensured that the Oncology clinical nurse specialist (CNS) visiting Janet was aware of this to make sure that her recovery and plans for returning home would not be similarly affected. Emma made a note to do some further reading and reflection on this subject. On Grace’s suggestion Emma also had a discussion with the Oncology CNS, Kevin, and planned for a shadow shift with him. Grace, Emma, and Kevin identified some learning outcomes for this experience, and he agreed to be her supervisor for the day.
Emma recognised that Janet had prioritised Robert’s care needs and that this had influenced her decision when she experienced symptoms. This prompted Emma to reflect on how a person’s individual circumstances are linked to help seeking behaviours and health outcomes. This showed an understanding of the contribution of psychosocial influences, behaviours, and lifestyle choices to health outcomes.
Emma took the opportunity to share with Grace her knowledge and understanding of the anatomy and physiology related to Janet’s surgery. They discussed the rationale for a total abdominal hysterectomy compared to a laparoscopic hysterectomy. Emma, as a first-year student, provided a basic knowledge of the surgery and how the tumour had been affecting Janet. With this awareness Emma helped Janet to set some goals around improving her mobility with the initial aim of walking, accompanied, to use the bathroom to wash and use the toilet rather than using facilities at the bedside.
Emma recognised that Janet was experiencing pain on movement that was not being relieved with her current medication and that she was extremely anxious about her husband being home alone. With support from Grace, she made referrals to the pain team and spoke to Kevin about Janet’s anxieties. Grace and Emma had a conversation about how Janet’s anxiety and pain might affect her recovery and discharge. Janet expressed some anxiety about her wound and felt hesitant to move, concerned that the clips may come undone. Grace reassured Janet that this was very unlikely, and Emma was able to show her how to take deep breaths using a pillow to support her abdomen.
Under Grace’s supervision Emma documented Janet’s’ agreed plan of care and the progress made to date.
Emma linked her knowledge of relevant anatomy and physiology to Janet’s surgery and recovery. She was able to apply this knowledge to contribute to a joint plan of care that was person-centred with agreed goals. Janet’s wound was healing nicely and Emma reflected on the importance of anxiety and how this may be influencing levels of pain; this informed the decision to refer Janet to the pain management team.
Emma monitored Janet’s fluid balance and encouraged her to take oral fluids and a light diet. Janet expressed concern about needing to pass urine frequently if she drunk more fluids; Emma explained the risk of urinary tract infection (UTI) with a restricted fluid intake and, with Emma’s support, Janet drank more fluid.
Emma regularly monitored the six physiological measurements recorded to calculate the National Early Warning Score (NEWS 2) for Janet. This included: respiration rate; oxygen saturation, systolic blood pressure; pulse rate; level of consciousness and temperature. At the beginning of the shift these were being recorded every two hours, Emma calculated Janet’s NEWS2 score to 3, this is considered low risk (aggregate score 1 to 4) and so Emma asked Grace if the frequency of assessment could be changed. As a response to this Grace advised that Janet’s monitoring to be changed to four hourly. Emma updated Janet on this positive outcome and progress which helped to reduce her overall anxiety. Grace and Emma discussed possible signs and actions should Janet’s condition deteriorate.
Emma demonstrated she was aware of the importance of an adequate fluid intake and the risk of UTI following gynecological surgery and catheterisation. She was able to effectively communicate and manage Janet’s expectations.
Emma showed that she was developing the knowledge and ability to identify and respond proactively to early signs and symptoms of deterioration and contribute towards sound clinical decisions.
When Emma referred Janet to the pain team, she made sure that the team had all the relevant information including the pain score, wound condition, NEWS2 score, and the exacerbating factors such as Janet’s anxiety about her husband at home and her new diagnosis.
Janet had also been referred to the oncology CNS prior to admission. When Kevin the CNS came to the ward for a follow up visit; Emma spoke to him explaining that Janet had disclosed to her that she does not fully understand the diagnosis she has been given and the treatment plan now she has had the hysterectomy.
Emma showed an understanding of the roles of both the oncology CNS and the acute pain team and effectively communicated Janet’s care needs with them, ensuring that they are fully informed of factors affecting her care and were able to provide continuity and collaborate with her to meet her needs.
Emma made sure that all relevant risk assessments were updated for Janet as she became more mobile. This included pressure ulcer risk assessments, moving and handing assessments, pain assessment, falls risk, wound assessments and nutrition risk score. She was able to explain to Grace the importance of these assessments and talked through the actions they may take depending on possible changes and outcomes.
Grace and Emma discussed how person centred data from risk assessments are used to inform clinical audits and how this supports overall quality improvement in key aspects of the care people receive post operatively and through their care journey/pathway. Grace invited Emma to the next ward quality improvement meeting so she could see how this works and the implications for her future practice.
Emma showed she can accurately undertake risk assessments for an individual in an acute care setting and demonstrated an awareness of the importance of doing so. She also knew how to escalate concerns if Janet’s health deteriorated. In addition, Emma continues to develop an awareness of the impact of individual risk assessments on audit activity and quality improvement strategies.
While assisting Janet with her personal hygiene needs, Emma gained important information around her home circumstances. This included information about her husband’s care needs. Janet had made arrangements for Robert in preparation for her hospital admission; Emma gained Janet’s permission to explore the possibilities of continuing with the extra support when Janet returns home to help with her recovery. Emma acted as Janet’s advocate by documenting their discussion and shared her longer-term care needs and priorities with the multidisciplinary team.
Emma was able to effectively contribute towards jointly planning Janet’s discharge in line with her needs, wishes and preferences. She recognised that planning for discharge would need to take account of both Janet’s care needs as well as her husband’s showing an awareness of the principles and processes involved in facilitating safe discharge.
Annexe A: Communication and relationship management skills
What Emma did:
Emma reflected on the rapport, relationship, and communication she had with Janet and thought about the strategies that she used to help Janet feel comfortable in expressing her anxieties. Emma reflected on the communication techniques she has learned and the importance of working in partnership. She actively listened to Janet and helped her to talk about her anxieties gently probing, asking open questions and being non-judgmental.
For Emma these conversations were difficult at times as she had little experience of talking with people who have cancer; however, she recognised that Janet trusted her and felt comfortable talking to her. Emma felt very shy and lacking in confidence around difficult conversations and found it helpful to talk this through with Grace. She was sensitive and understanding but also recognised her limitations as she was not equipped to give specialist advice and should involve other members of the team. Aware that the oncology CNS, Kevin, was visiting Janet, Emma spoke to him about the nurse specialist role and continued to listen, aware that she did not want Janet to feel ‘fobbed off’.
Emma engaged in appropriate dialogue with Janet and during Kevin’s visit, sat with her, listened, and recognised the value of staying with her and holding her hand providing support in the absence of a family member. She then ensured that the outcomes of the conversations were accurately documented and communicated to Grace.
Emma showed that she was working towards the communication and relationship management skills outlined in Annexe A. She demonstrated active listening including responding to non-verbal cues (1.1) using prompts and verbal and non-verbal reinforcement (1.2). Emma showed that she understood the importance of non-verbal communication, specifically touch, when she sat with Janet during the Oncology CNS visit (1.3). In addition, she made use of open and closed questions and caring conversation techniques (1.4 and 1.5). In recording the outcome of her discussion with Janet she showed that she can write accurate, clear, legible records (1.8).
By engaging in a difficult conversation with Janet, Emma displayed that she has begun to work towards this skill (2.9). She conveyed compassion and sensitivity to Janet who at times was feeling extremely anxious.
Annexe B: Nursing procedures
Emma undertook and recorded vital signs for Janet and calculated the early warning score. She took the opportunity to use the ‘manual’ sphygmomanometer to record Janet’s blood pressure as she was keen to consolidate the skill she had learnt in simulation at her university. The fluid balance chart was updated to record that Janet had passed urine since her catheter was removed. Working closely with Janet throughout, Emma completed a pain assessment and escalated her concerns about her level of pain when she moved. The nutritional risk assessment was updated, and Emma helped Janet select healthy meals from the menu.
Emma had a discussion with Janet about how much help she may need to wash. She was keen for Janet to maintain her independence but also wanted to make sure she felt cared for. Janet was able to wash herself with some assistance from Emma who ensured that she had clean bedding, her table was nearby and decluttered and the call-bell was accessible. While being assisted with a wash, Janet became distressed, Emma understood the importance of recognising anxieties and the impact this may have on her feeling safe, her recovery and plans for safe discharge. Emma made sure this was documented and appropriately communicated to the team.
As Janet’s pain became controlled, she was able to walk to the bathroom with Emma’s assistance finding this more comfortable than using a commode at the bedside. Emma updated Janet’s mobility and falls risk assessments to reflect her increased mobility.
Emma noticed that Janet’s surgical wound dressing had become soiled with exudate. She asked Grace to review the wound as she was concerned about this. Grace asked Emma what she knew about wound healing, and they explored the types of exudate that can be seen. They reviewed the wound together and concluded that the liquid seen on the dressing was serosanguinous drainage as it was thin, pink, and watery in presentation. Emma was able to explain that purulent drainage is milky, typically thicker in consistency, and can be grey, green, or yellow in appearance and if fluid becomes very thick, this can be a sign of infection. They were able to reassure Janet that the liquid seen on the dressing did not indicate an infection and was part of the healing process. She let Janet know the wound was healing nicely and emphasised the importance of keeping it clean and dry. Emma re-dressed the wound using an aseptic technique and documented the condition of the wound including the type of exudate seen.
In all care interventions with Janet, Emma was observed to act in accordance with local infection prevention and control policy and was able to articulate to Grace the rationale behind these.
Emma showed that she is working towards the nursing procedures outlined in Annexe B. She showed that she was able to recognise signs of emotional distress (1.1.1) as well as symptoms and signs of physical ill health (1.2.1). She demonstrated that she was able to recognise symptoms and signs of deterioration and sepsis (1.2.3) and articulated how this is being monitored by taking, recording, and interpreting vital signs manually and via technological devices (2.1).
In assisting Janet, Emma showed that she can use appropriate bed making techniques for those with limited mobility (3.2) and she endeavored to ensure privacy and dignity at all times (3.4). Emma also took appropriate actions with Janet to reduce or minimise discomfort (3.5).
While helping Janet to meet her care needs and support with hygiene and skin integrity Emma showed that she was able to observe, assess and optimise skin and hygiene status and determine the need for support (4.1, 4.3).
By redressing Janet’s surgical wound, Emma demonstrated the use of an aseptic technique when undertaking wound care (4.6, 9.3). In addition, she observed infection prevention measures including standard precaution protocols (9.1), using appropriate personal protection equipment (9.4) and safely disposed of waste (9.8).
Emma updated Janet’s nutrition risk score and thereby showed that she is using contemporary nutritional assessment tools (5.2). Furthermore, she recorded fluid intake and output (5.4) and observed Janet’s level of urinary continence and assisted her with toileting (6.1). Recognising that it was important to record that Janet had passed urine since her catheter was removed, Emma showed that she was developing an awareness in the assessment of bladder patterns and urinary retention (6.4).
Janet’s mobility was initially impaired following her surgery and Emma showed that she was observing and using evidence-based risk assessments to determine need for support and intervention to optimise mobility and safety and to identify and manage risk of falls (7.1).
With respect to best evidence-based practice with medicines administration and optimisation, Emma showed she was working towards gaining procedural competencies to exercise professional accountability in ensuring the safe administration of medicines to those receiving care (11.6) and administering medicines using a range of routes (11.9).
Test your understanding
Questions to prompt reflection and discussion
For Emma to achieve her objectives in relation to medicines management and optimisation, and discharge planning identify two proficiencies that Emma still needs to work on and what learning opportunities would you consider might be available for her in your area to achieve this?
For example, Emma could spend time with the departmental pharmacist, who could act as her practice supervisor to work towards Annexe B, 11.2 “recognise the various procedural routes under which medicines can be prescribed, supplied, dispensed and administered; and the laws, policies, regulations and guidance that underpin them” and Annexe B 11.11 “undertake safe storage, transportation and disposal of medicinal products.
For discharge planning Emma could attend the multidisciplinary (MD) meeting to discuss discharge plans and thereby work towards Platform 7, 7.10 “understand the principles and processes involved in planning and facilitating the safe discharge and transition of people between caseloads, settings and services”.
Emma will be spending a day with Kevin the oncology CNS, what objectives could be set for Emma to achieve while Kevin is her supervisor for this experience? If you were Emma’s practice assessor, what feedback would you ask Kevin to provide?
If you are a registered nurse, you may wish to use this scenario and your reading as part of your continuing professional development (CPD) for your revalidation .
- Last updated: 06/12/2022
This website is intended for healthcare professionals

- { $refs.search.focus(); })" aria-controls="searchpanel" :aria-expanded="open" class="hidden lg:inline-flex justify-end text-gray-800 hover:text-primary py-2 px-4 lg:px-0 items-center text-base font-medium"> Search
Search menu
Alberti R, Emmons M. Your perfect right. Assertiveness and equality in your life and relationships, 10th edn. Samnta Clarita (CA): Impact Publishing; 2017
Akinbode A. Teaching as lived experience: the value of exploring the hidden and emotional side of teaching through reflective narrative. Studying Teacher Education. 2013; 1:(9)62-73 https://doi.org/10.1080/17425964.2013.771574
Beauvais AM, Brady N, O'Shea ER, Griffin MTQ. Emotional intelligence and nursing performance among nursing students. Nurse Educ Today. 2011; 31:(4)396-401 https://doi.org/10.1016/j.nedt.2010.07.013
Begley AM. On being a good nurse: reflections on the past and preparing for the future. Int J Nurs Pract. 2010; 16:(6)525-532 https://doi.org/10.1111/j.1440-172X.2010.01878.x
Bishop S. Develop your assertiveness, 3rd edn. London: Kogan Page; 2013
Butler-Kisber L, Poldma T. The power of visual approaches in qualitative inquiry: the use of collage making and concept mapping in experiential research. Journal of Research Practice. 2010; 2:(6)1-16
Care Quality Commission. Raising a concern with CQC. A quick guide for health and care staff about whistleblowing. 2017. https://tinyurl.com/mr3s3c84 (accessed 23 June 2022)
Cohen L, Manion L, Morrison K. Research methods in education, 6th edn. London: Routledge; 2007
Contreras JA, Edwards-Maddox S, Hall A, Lee MA. Effects of reflective practice on baccalaureate nursing students' stress, anxiety and competency: an integrative review. Worldviews Evid Based Nurs. 2020; 17:(3)239-245 https://doi.org/10.1111/wvn.12438
de Souza Pereira S, Bastos Teixeira CA, Reisdorfer E, da Silva Gherardi-Donato EC, Juruena MF, Cardoso L. Burnout in nursing professionals: associations with early stress. British Journal of Mental Health Nursing. 2015; 6:(4)267-275 https://doi.org/10.12968/bjmh.2015.4.6.267
Duffy K, McCallum J, Ness V, Price L. Whistleblowing and student nurses - Are we asking too much?. Nurse Educ Pract. 2012; 12:(4)177-178 https://doi.org/10.1016/j.nepr.2012.04.002
Edwards S, Lee M, Sluman K. Student-led simulation: preparing students for leadership. Nurs Manage. 2018; 25:(5)28-34 https://doi.org/10.7748/nm.2018.e1778
Ekebergh M. Lifeworld-based reflection and learning: a contribution to the reflective practice in nursing and nursing education. Reflective Pract. 2007; 8:(3)331-343 https://doi.org/10.1080/14623940701424835
Ferguson LM. From the perspective of new nurses: what do effective mentors look like in practice?. Nurse Educ Pract. 2011; 11:(2)119-23 https://doi.org/10.1016/j.nepr.2010.11.003
Fook J, Askeland GA. Challenges of critical reflection: ’nothing ventured, nothing gained.’. Social Work Education. 2007; 5:(26)520-533 10.1080/02615470601118662
Fuster Linares P, Rodriguez Higueras E, Martin-Ferreres ML, Cerezuela Torre MÁ, Wennberg Capellades L, Gallart Fernández-Puebla A. Dimensions of leadership in undergraduate nursing students. Validation of a tool. Nurse Educ Today. 2020; 95 https://doi.org/10.1016/j.nedt.2020.104576
Goleman D. Working with emotional intelligence.London: Bloomsbury; 1998
Greenwood J. The role of reflection in single and double loop learning. J Adv Nurs. 1998; 27:(5)1048-1053 https://doi.org/10.1046/j.1365-2648.1998.t01-1-00579.x
Hudek K. Finding Voice. AORN J. 2012; 95:(5)648-652 https://doi.org/10.1016/j.aorn.2012.02.011
Hutchison JS. Anti-oppressive practice and reflexive lifeworld-led approaches to care: a framework for teaching nurses about social justice. Nurs Res Pract. 2015; 2015:1-5 https://doi.org/10.1155/2015/187508
Ion R, Smith K, Moir J, Nimmo S. Accounting for actions and omissions: a discourse analysis of student nurse accounts of responding to instances of poor care. J Adv Nurs. 2016; 72:(5)1054-64 https://doi.org/10.1111/jan.12893
Johns C. Becoming a reflective practitioner, 4th edn. Chichester: Wiley-Blackwell; 2013
Kaihlanen AM, Lakanmaa RL, Salminen L. The transition from nursing student to registered nurse: the mentor's possibilities to act as a supporter. Nurse Educ Pract. 2013; 13:(5)418-422 https://doi.org/10.1016/j.nepr.2013.01.001
Keeling J, Templeman J. An exploratory study: student nurses' perceptions of professionalism. Nurse Educ Pract. 2013; 13:(1)18-22 https://doi.org/10.1016/j.nepr.2012.05.008
Krueger RA. Analyzing and reporting focus group results.London: Sage; 1998
Larijani TT, Aghajani M, Baheiraei A, Neiestanak NS. Relation of assertiveness and anxiety among Iranian University students. J Psychiatr Ment Health Nurs. 2010; 17:(10)893-839 https://doi.org/10.1111/j.1365-2850.2010.01607.x
Law BYS, Chan EA. The experience of learning to speak up: a narrative inquiry on newly graduated registered nurses. J Clin Nurs. 2015; 24:(13-14)1837-1848 https://doi.org/10.1111/jocn.12805
Levett-Jones T, Lathlean J. ‘Don't rock the boat’: Nursing students' experiences of conformity and compliance. Nurse Educ Today. 2009; 29:(3)342-349 https://doi.org/10.1016/j.nedt.2008.10.009
Malik D, Wilkinson D, Henwood S. Practical leadership in nursing and health care. In: Henwood S (ed). London: CRC Press; 2014
Moon J. Using story in higher education and professional development, 1st edn. London: Routledge; 2010
Mooney M. Professional socialization: the key to survival as a newly qualified nurse. Int J Nurs Pract. 2007; 13:(2)75-80 https://doi.org/10.1111/j.1440-172X.2007.00617.x
Nursing and Midwifery Council. Future nurse: Standards of proficiency for registered nurses. 2018a. https://tinyurl.com/2x2nbpdr (accessed 1 August 2022)
Nursing and Midwifery Council. The Code. 2018b. https://www.nmc.org.uk/standards/code/ (accessed 24 June 2022)
Nursing and Midwifery Council. Standards framework for nursing and midwifery education. 2019. https://tinyurl.com/ru573f7t (accessed 1 August 2022)
Oxtoby K. Make yourself heard. Nurs Stand. 2015; 30:(15) https://doi.org/10.7748/ns.30.15.63.s53
Por J, Barriball L, Fitzpatrick J, Roberts J. Emotional intelligence: its relationship to stress, coping, well-being and professional performance in nursing students. Nurse Educ Today. 2011; 31:(8)855-860 https://doi.org/10.1016/j.nedt.2010.12.023
Poroch D, McIntosh W. Barriers to assertive skills in nurses. Aust N Z J Ment Health Nurs. 1995; 4:(3)113-123
Punch KF. Introduction to social research: quantitative and qualitative approaches, 3rd edn. London: Sage; 2014
Royal College of Nursing. Informed consent in health and social care research. RCN guidance for nurses. 2011. https://tinyurl.com/4kjy3tze (accessed 1 August 2020)
Siviter B. The student nurse handbook, 3rd edn. London: Balliére-Tindall/Elsevier; 2013
Smith JA, Osborn M. Interpretive phenomenological analysis. In: Smith JA (ed). London: Sage; 2003
Stanley D. Clinical leadership characteristics confirmed. Journal of Research in Nursing. 2014; 19:(2)118-128 https://doi.org/10.1177/1744987112464630
Timmins F, McCabe C. Nurses' and midwives' assertive behaviour in the workplace. J Adv Nurs. 2005; 51:(1)38-45 https://doi.org/10.1111/j.1365-2648.2005.03458.x
Tomietto M, Sartor A, Mazzocoli E, Palese A. Paradoxical effects of a hospital-based, multi-intervention programme aimed at reducing medication round interruptions. J Nurs Manag. 2012; 20:(3)335-343 https://doi.org/10.1111/j.1365-2834.2012.01329.x
Wadensten B, Engström M, Häggström E. Public nursing home staff 's experience of participating in an intervention aimed at enhancing their self-esteem. J Nurs Manag. 2009; 17:(7)833-842 https://doi.org/10.1111/j.1365-2834.2009.00968.x
Developing collective leadership for health care. 2014. https://bit.ly/3xLToLA (accessed 24 June 2022)
Willis Commission. Quality with compassion: the future of nursing education. Report of the Willis Commission. 2012. https://tinyurl.com/2p8r5a3m (accessed 24 June 2022)
Students' experience of the challenges of using assertive communication
Claire Keates
Senior lecturer, Adult nursing, University of Hertfordshire, Hatfield
View articles · Email Claire

Assertive communication is a skill that many nurses, particularly nursing students, find challenging. This article describes the findings of phenomenological study that set out to explore third-year student nurses' experiences of using assertive communication in the clinical setting. A narrative enquiry approach reviewed six reflective written accounts of their experiences. In addition, seven students took part in an in-depth semi-structured group discussion of their clinical experiences. Data were analysed using a hybrid interpretive phenomenological analysis and discourse analysis framework. Three key themes emerged: a sense of responsibility/duty and a sense of failure when this is not upheld, the importance of mentors in promoting self-confidence and self-esteem, and a sense of belonging on placement. The students responded well to positive role models and were able to identify negative role models. Accurate, constructive feedback and support was important to help students reflect appropriately.
Nursing has historically been a submissive profession within health care. Today, changes in healthcare policy, the evolving nursing role and negative healthcare events publicised in the media, have made it essential for contemporary nurses to be leaders within the clinical environment, using assertive communication styles in their exchanges with patients, relatives and other healthcare staff. Individuals in leaderships positions motivate others, set clear goals and make decisions, using listening skills and articulating clearly. The Nursing and Midwifery Council (NMC) (2018a ; 2019 ) standards consider that leadership principles, such as assertiveness, are an integral component in the delivery of high-quality care and there is an expectation that students will engage with this from the start of their education.
The Willis Commission (2012) recognised that nurse educators and qualified nurses are in a unique position to lead nursing as a competent and compassionate workforce. Nursing students must be proficient in recognising, challenging and reporting poor care, working as equal partners alongside other health professionals ( NMC, 2018b ). This is consistent with Cumming and Bennett's (2012) position that leadership must exist at every level, with each individual viewing themselves as a leader who role models compassion in day-to-day care and who is committed to speaking up when things are wrong.
Register now to continue reading
Thank you for visiting British Journal of Nursing and reading some of our peer-reviewed resources for nurses. To read more, please register today. You’ll enjoy the following great benefits:
What's included
Limited access to clinical or professional articles
Unlimited access to the latest news, blogs and video content
Signing in with your registered email address
Home — Essay Samples — Nursing & Health — Nursing — Communication Style Reflection for Effective Nursing Practice
Communication Style Reflection for Effective Nursing Practice
- Categories: Effective Communication Interpersonal Communication Nursing
About this sample

Words: 1105 |
Published: Aug 4, 2023
Words: 1105 | Pages: 2 | 6 min read
Table of contents
Introduction, strengths in communication style, weaknesses in communication style, works cited.
- Balzar Riley, J. (2008). Potter and Perry Canadian Fundamentals of Nursing, 5th edition.
- Arnold, E. C., & Boggs, K. U. (2020). Interpersonal Relationships: Professional Communication Skills for Nurses. Elsevier.

Cite this Essay
To export a reference to this article please select a referencing style below:
Let us write you an essay from scratch
- 450+ experts on 30 subjects ready to help
- Custom essay delivered in as few as 3 hours
Get high-quality help

Verified writer
- Expert in: Sociology Nursing & Health

+ 120 experts online
By clicking “Check Writers’ Offers”, you agree to our terms of service and privacy policy . We’ll occasionally send you promo and account related email
No need to pay just yet!
Related Essays
1 pages / 517 words
2 pages / 1039 words
4 pages / 1732 words
3 pages / 1478 words
Remember! This is just a sample.
You can get your custom paper by one of our expert writers.
121 writers online
Still can’t find what you need?
Browse our vast selection of original essay samples, each expertly formatted and styled
Related Essays on Nursing
Nurse burnout has become a pressing issue in the healthcare industry, with detrimental effects on both nurses and patient care. Understanding the causes and effects of burnout, as well as implementing strategies for prevention, [...]
Advocating for patients' need for basic care and comfort is pivotal in nursing practice. Healthcare professionals should ensure that patients are not harmed in the healthcare setting as it is supposed to provide healing and [...]
Altman, M., & Rosa, W. (2015). Redefining “time” to meet nursing’s evolving demands. Nursing Management, 46(5), 46–50. doi:http://dx.doi.org.libaccess.fdu.edu/10.1108/DLO-02-2017-0009
The social justice in nursing essay delves into the critical role of nurses in promoting equitable and fair healthcare for all individuals. Social justice, a fundamental principle of nursing, emphasizes the importance of [...]
Nursing plays a pivotal role in healthcare, and effective management and leadership are essential to ensure the delivery of high-quality care. Nurses, irrespective of their levels, have the opportunity to display leadership [...]
The role of a nurse is often seen as one of care and compassion, providing support and medical treatment to those in need. However, there is another aspect to nursing that is equally important but often overlooked - that of the [...]
Related Topics
By clicking “Send”, you agree to our Terms of service and Privacy statement . We will occasionally send you account related emails.
Where do you want us to send this sample?
By clicking “Continue”, you agree to our terms of service and privacy policy.
Be careful. This essay is not unique
This essay was donated by a student and is likely to have been used and submitted before
Download this Sample
Free samples may contain mistakes and not unique parts
Sorry, we could not paraphrase this essay. Our professional writers can rewrite it and get you a unique paper.
Please check your inbox.
We can write you a custom essay that will follow your exact instructions and meet the deadlines. Let's fix your grades together!
Get Your Personalized Essay in 3 Hours or Less!
We use cookies to personalyze your web-site experience. By continuing we’ll assume you board with our cookie policy .
- Instructions Followed To The Letter
- Deadlines Met At Every Stage
- Unique And Plagiarism Free
Nursing Reflective Essay: Example Outline and Guide
Are you a nursing student? Then, you will definitely have an assignment to compose a nursing reflective essay. This task might be quite tough and challenging. But don’t stress out! Our professionals are willing to assist you.
First and foremost, let’s figure out what’s reflective writing. In a few words, such essays are based on your experiences, feelings, views on something, etc. For nursing students, reflective papers help to practice their skills and expand their knowledge.
In case you are wondering how to master nursing essay writing, you are on the right page. This article will provide tips that will help you write an outstanding student nurse reflection: examples of what to include in it, what to avoid, and what reflection ideas to use.
- ✒️ Analytical Essay
- ✒️ Reflective Essay
⭕ Outline and Draft
- ⭕ Revise and Edit
- ❓ Reflecting
- ❗ Essential Parts
- ⚠️ Mistakes to Avoid
- 💡 Additional Tips
🔗 References
🆚 analytical vs. reflective nursing essay.
Basically, nursing essays can be divided into different types.
The most common ones are analytical and reflective essays. These two styles are the most suitable for nursing papers. They either argue a particular perspective (analytical) or base the narration on previous experiences (reflective).
This focus is what differentiates one type of essay from another, as both analytical and reflective nursing essays can be quite similar stylistically.
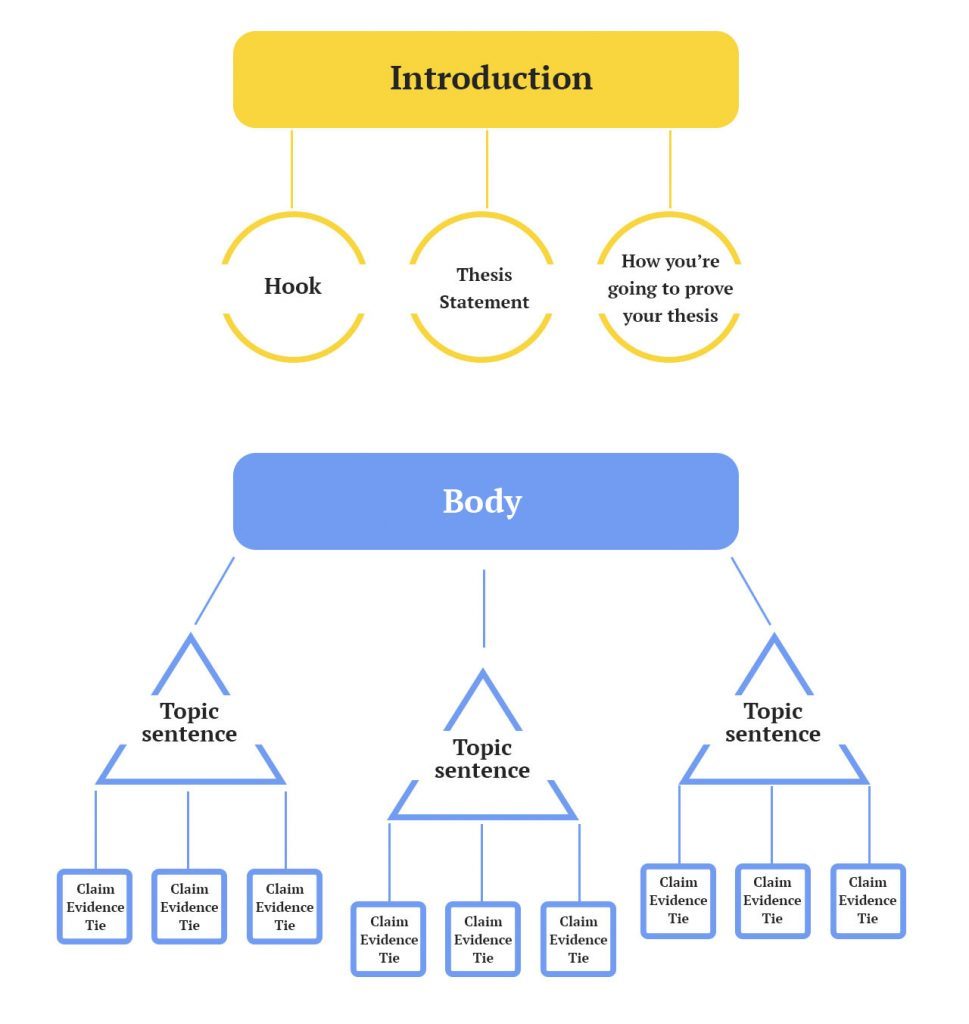
✒️ Nursing: Analytical Essay
Speaking of structural parts, the basic outline for an analytical essay on nursing can look like this:
- Introduction. The introduction is your first paragraph, which usually consists of two parts. First, you have to capture the reader’s attention. Then, you aim to create a clear thesis statement to demonstrate your position.
- Providing evidence. Each of your arguments should have at least one piece of evidence. If you have more to share, it’s even better. However, you have to keep the word count in mind. So, make strong points to keep your essay concise.
- Practical use of evidence. There’s no point in providing evidence that wouldn’t have any real use in practice.
- The judgment of evidence. Here, you’ll demonstrate your critical thinking abilities. Prove that your evidence is indeed strong and valid.
- Conclusion. First, summarize what’s been said in your essay. Then give your own opinion on it.
✒️ Nursing: Reflective Essay
A reflective nursing essay usually consists of the following elements:
- Introduction. It explains the whole purpose of the essay and tells readers what to expect. The most crucial part of the introduction is the thesis statement. Usually, it’s the last sentence of the intro. Your thesis should be concise and clearly reflect your position.
- Description of the situation. Since a reflective essay is based on previous experiences, describing those events is the core part of the paper. Again, this section should contain only the most important and valuable details.
- Sharing of personal feelings. The section demonstrates how you react to situations and how you’re able to gain control over those emotions.
- Evaluation of experience. This part is a summary of what skills and knowledge did you get from experience.
- Reflection and opportunities for learning. The part is closely connected to the previous one. While previously you were just giving a summary, here you’ll describe what this situation made you understand. Also, elaborate on your future path of self-development.
- Conclusion. This one is simple. Just summarize all the information you discussed in your essay.
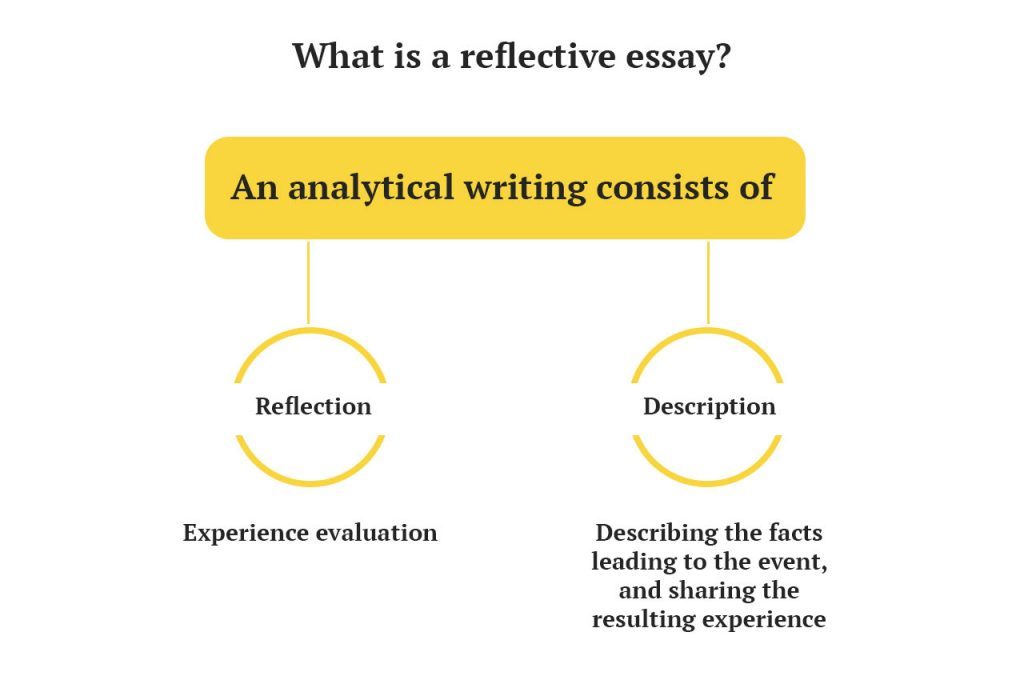
We’ll now tell you about the writing preparation process.
✍️ Reflective Nursing Essay Writing Guide
Creating a nursing reflection essay is a long and challenging journey that requires total concentration on a task. That’s why it is essential to turn your “study mode” on and devote yourself to the essay writing process.
No doubts, you might get too overwhelmed by the amount of work you have to get done. But don’t worry! We know how to avoid anxiety. Just follow out tips and write an outstanding nursing reflection paper!
⭕ Remove the Distractions
Yes, it’s as simple as that. Ironically, most of the major problems usually happen at this initial stage. So, you just need to know how to overcome them right away.
- Turn all the gadgets off (yes, even your cell phone).
- Make sure to get rid of anything around you that could potentially catch your attention and distract you from writing.
- Get earplugs if necessary.
Then, get in your “ study mood .”
- Go through all your pre-game rituals — visit the bathroom, eat, drink, meditate, etc.
- Get fun out of the way. Dedicate some time for yourself so that you won’t have the temptation later.
- Prepare the essentials — open your notebook or create a Word document and make sure you have all the necessary notes and resources ready.
After you create perfect conditions, make another significant step to start writing. Research is an essential part of any academic work, even if you’re telling your personal story.
Here’s where you can start your search for brilliant ideas:
- your college library;
- your course readings;
- scholar.google.com ;
- online nursing journal articles;
And no matter what topic you’re going to discuss, don’t forget that most nursing essays use a similar pattern:
You still need to remember what we talked about in the very beginning—your story has to be unique. Use these questions as a framework, and fill the essay with unique content. If you’ve answered most of these questions, you’re halfway to your excellent grade.
No wonder outlining is a vital part of the essay writing process. It helps to reach the logical flow of ideas and organize all the arguments and examples in the right order. Also, you can easily edit a well-developed structure if something seems wrong. It’s always better to change the part of an outline rather than rewriting the entire paragraph.
Your reflective essay outline should look approximately like this:
- Point 1 (evidence, examples, other supportive details)
- Point 2 (evidence, examples, other supportive details)
- Point 3 (evidence, examples, other supportive details)
- Restatement of thesis statement
- Final memorable statement
After creating an outline, it would be a great idea to write the rough draft of your nursing reflective essay. This step will help you to avoid all the possible mistakes before submitting the paper.
⭕ Proofread and Revise
Polishing your essay is the last but not the least step of the writing process. So, take it seriously and don’t waste your chance to submit a flawless work. Revise your rough draft, make sure your ideas are coherent and supporting evidence is logical, and then create a final version of the essay.
We created the checklist of what you should take into consideration while revising your nursing reflective essay. Don’t hesitate to use it!
- make sure you meet the writing style requirements;
- check whether all in-text citations have the corresponding reference list entry;
- make sure you followed the proper structure (introduction, three body paragraphs, conclusion);
- get rid of all grammar and punctuation mistakes;
- double-check whether your ideas are clear and the supporting details are logical.
📝 Reflective Essay: Nursing School Application
Although people say there is a lack of nurses in the United States and a high demand for good specialists with a stellar education, it is not that easy to pass a nursing school admission.
What’s the reason for this?
It seems like nursing schools are looking for outstanding students, who have made a firm decision to become a nurse and will contribute to the community of the school and the field of healthcare in general.

You need to showcase this capability in your nursing application essay, where you reflect on your goals or experience. In the following sections, we’ll explain how to write it.
❓ Reflecting on Your Goals
Here’s a question you should ask yourself.
“Why do I want to become a nurse?”
As curious as it may sound, some students do not have that answer. If you are one of them, you might want to reconsider your decision.
Being a nurse is stressful. It requires dedication, a strong philosophy, and stable mental health. And if you’re unsure about your choice — try to make up your mind as soon as possible. Getting a nursing education is a serious step in your life. So, be confident about your choice not to regret it later. The video below will give you an idea of what a day in the life of a nurse is like.
If your intentions are firm and you’re sure about your career goals, then we’re here to help you cope with all those “Why I chose nursing” essays.
- Know where to begin with your nursing essay. A good idea would be to find several nursing essay examples first. You will see that many students do not try to be creative. The same boring stories can be found in numerous essays. And it seems that those stories are taken from the same articles. This does not sound impressive at all. Repeating familiar stories is quite a critical mistake, and you should avoid it. We’ll talk more about common errors in nursing essay writing later, so keep on reading. Look through nursing paper examples and try to make your essay on nursing career different. Make it stand out from the crowd.
- Base your essay on a true story. Think about any situation from your clinical placement, which your reflective nursing essay will be based on. Describe what happened, who was involved in the case, why it impressed you, etc. By doing this, you’ll demonstrate a complete understanding of the situation. Your essay will show that you’re able to comprehend what’s happening and make the right decisions, even in critical cases. These are skills that every nurse should have.
- Write a personal essay. Now, proceed to describe your feelings. Follow these three questions: How did you feel in that situation? Why? What were your actions, actions of other personnel? Be sure to tell how much you care about what happened. It’s a great way to show how sympathetic you can be.
- Evaluate the event. Another stage of writing the reflective nursing essay is an evaluation of your experience. Why do you think it is a valuable experience for you? How did it contribute to your personal and professional development? Self-development is among the most important aspects of professionalism for a nurse. And you must not forget to show that you have this capability.
- Choose the right focus. It’s common for students to concentrate on a story that deals with the nursing profession. This is a strategy that you too can follow when writing your nursing essay. Make sure that the narrative focuses on you instead of other nurses or patients. It is your essay, so be sure to write about your personal experience. You have to tell the reader about all the lessons you have learned and explain how it helped you come up with a decision to become a nurse.
- Allow yourself to fantasize. There’s another critical subtopic you should cover in your nursing essay. Tell what other actions you could take and whether you would repeat them if you are to face the same situation.
Next, we’re going to talk about the parts that make up a well-written nursing essay. So, stay with us!
❗ Essential Application Essay Parts
You probably know that competition in nursing schools is especially severe compared to other educational institutions.
Your paper should be outstanding if you want to be accepted. Below, you’ll find a list of the most significant parts of any nursing admission essay. These parts contain all relevant info that the admission officers want to know about an applicant.
- Is there someone who influenced your decision?
- Was there an event that had an impact on your choice of a career?
- Do you know what particular kind of nursing you want to do?
These are essential questions to answer in the nursing school essay. You do double-duty by responding to these questions. Not only will you explain how you decided to become a nurse, but you’ll also make sure that your intentions are truly firm.
- Show what you’re worth. You need to tell about your experience in the nursing field. This is a job where you need at least some background experience. If you have never seen a syringe in your life, your nursing essay will hardly convince anybody. So, make a personal statement. And make it strong.
- Prove that you’re ready. You need to show that you are prepared to be a nurse and ready for all nursing hardships. Nursing is emotionally and physically exhausting. That’s why you need to demonstrate the best of your personal and professional values. Prove to the admission counselors that you are capable of completing the nursing job.
⚠️ Nursing Reflective Essay: Mistakes to Avoid
As we have mentioned before, the competition is going to be tough. It is not easy to enter a nursing school even with the best scores and a high GPA. So, your essay should be of the highest quality!
One of the best ways to ensure your works’ flawlessness is to learn the most common mistakes and avoid them in your paper. Below, you will find the list of the most critical errors for a nursing application essay. Investigate them here:
- Not including your own nursing story. Without a real-life story, a nursing application essay seems very weak. Listing personal qualities that a nurse should possess is not enough. Tell a story that will show the admission officers how helpful you were while providing care to somebody.
- Not sharing your experiences. Your nursing application essay will undoubtedly lose a couple of points if you do not mention some nursing-related experiences. A strong intention to become a nurse is great, of course. However, if you have no idea what nursing is all about, your essay will not be convincing.
- Not providing sufficient reasons to support your intentions. It is ridiculous to remind about that, but some students still fail to mention why they want to enter a certain school. Make sure to avoid this mistake in your nursing application essay.
- Plagiarizing. Plagiarism can cause you to fail your paper or be rejected by the schools you’re applying for. More importantly, plagiarizing isn’t ethical. To avoid any potential issues, make sure to cite all your sources and provide an authentic and unique story.
- Repeating yourself. This problem is widespread in the introduction and conclusion. If you need to connect the first and the last paragraphs, don’t just rewrite the info from the introduction into a conclusion. Rather synthesize your thoughts and finish your essay dynamically.
💡 Nursing Reflective Essay: Additional Tips
We’ve come to the point where you can go ahead and start writing your nursing essay. But there’s one more thing…
The process of writing a nursing essay has its own tips and tricks. So, we simply couldn’t let you go without sharing a few of them.
Hopefully, you’ll find these nursing school essay tips useful:
- Always start working on your student nurse essay with studying assignment instructions. It is the best way to find out what exactly will be assessed in your paper.
- Do not hesitate to ask your tutors for help and advice. Whether you believe it or not, but they do not want you to fail student nurse assignments and essays.
- To prepare a good student nurse essay, you will have to find and read quite a lot of nursing literature. Mind that it usually takes a lot of time. So, start researching early.
- Student nurse essays have a standard structure. Thus, make sure you have all the necessary paragraphs. Do not forget about specific terminology that should be used in your works. Also, remember about the proper formatting of your paper (e.g., MLA, Chicago, or APA format).
- How to summarize an article without plagiarizing ? Keep your text balanced. When looking through your draft, pay attention not only to the logic of your narration. Also, check how much of the paper consists of your own thoughts and what percentage is a review of other people’s work.
With these tips in mind, it’s now your time to shine!
Nursing Reflective Essay Topics
- Strengths and weaknesses of nursing professionals.
- Analyze the methods clinical nurses use to deal with moral distress.
- Examine the types of errors in nursing.
- Describe the role of technology in nursing care.
- The role of the nursing professional in patient advocacy.
- Peculiarities and importance of nursing interventions in the pre-op period.
- The crucial role of communication in nursing.
- Is MSN course worth studying?
- Examine the importance of cultural competency in nursing practice.
- What is the best nursing recruitment strategy and why?
- The critical role of QSEN competencies in becoming a better nurse.
- Collaboration and communication issues in nursing practice .
- Personal integrity and accountability in nursing practice.
- Describe the aims and key concepts of nursing care delivery model.
- Analyze the basic nursing theories.
- Discuss the occupational health and safety risks of practicing nurses.
- How to reduce the rate of workplace burnouts in nursing profession.
- Advantages and disadvantages of becoming a clinical nurse leader.
- Analyze the main reasons for nursing shortage.
- Describe the challenges of family nurse practitioner and the ways to overcome them.
- The importance of nurses providing care for elderly at home .
- Examine the elements that the nurses should take into account to improve the care of diabetic patients.
- Why knowledge and application of psychological theories are vital for nursing practice.
- Why is it necessary to integrate cultural competence in nursing practice?
- Do Christian values play an important role in nursing practice?
- Discuss the significance of evidence-based practice to nursing.
- Explain how a nurse can use a personal digital assistant to enhance performance.
- The challenges of language barrier and cultural diversity in nursing practice.
- Cultural sensitive approach in nursing and health care.
- Describe ethical and moral dilemmas of nursing.
- Why strategic management is important to a trained nurse.
- Discuss the issues of combining a nursing job and Jewish traditions.
- The issue of aging of the nursing population.
- Analyze the peculiarities of Cuban-American culture and its influence on nursing practice.
- The role of nurses in healthcare delivery.
- The issue of applying theory to practice to manage stress in nursing.
- Describe the advantages and disadvantages of different leadership styles in nursing.
- Examine the specifics of women’s nursing.
- The leadership role of nurses in the healthcare system.
- Explain how a nurse can be a cultural broker of the community.
- Why do people choose to become nurses?
- The types and benefits of technologies used in nursing profession.
- Analyze why a mandatory overtime in nursing profession is a controversial solution.
- Describe the reasons of burnout in nursing profession.
- How to resolve the nursing shortage problem.
- Discuss the effective strategies to improve nursing ratios.
- Psychological effects of COVID-19 that result in hospital nursing shortage.
- Compare and analyze the specifics of the community virtual ward model with the inpatient nursing care model.
- The importance of clear vision to nursing leaders.
- Discuss whether the use of social media can violate ethical nursing practices.
Writing a nursing essay doesn’t have to seem so difficult anymore. So, go forth and do it. Make it flawless because it’s your very first step on the way to success.
Also, don’t hesitate to share your thoughts! Did we miss something? Want to add more helpful info? Write about it in the comments below!
Further reading:
- How to Write an Expository Essay in Simple Steps
- Essay on Dengue Fever: How to Write + Free Examples
- Objective Essay Writing: How to Write, Topics and Examples
- French Essay Writing: How-to Guide and Examples
🤔 Reflective Essay in Nursing FAQ
A good essay of this kind is a reflection of personal feelings, impressions, and motivation. It should be based on a real-life example. Describe an unusual situation you’ve faced during the clinical placement program. Analyze the emotions it provoked, what could have been improved, etc.
Before you start writing, focus on your personal impressions provoked by a certain event or topic. Then put them down and organize cohesively. Do not forget about an appropriate introduction and a memorable conclusion.
If you are to write a good application essay to progress your career as a nurse, start with formulating your personal motivation to pursue this occupation. Draft the arguments and relevant examples, and then distill the right wording to make your paper persuasive and impressive.
It is a good idea to read some examples of reflective essay conclusions, but make sure that your own version is personal and sincere. A reflective essay is all about your own thoughts and perceptions, so you may simply paraphrase and summarize them.
- Ten Terrific Tips for New Nurses Dealing with Difficult Patients
- Volunteer Nursing Abroad
- Ten Ways How to Get in and Gain Experience in Nursing
- Critical Thinking and Writing for Nursing Students
- Learning Opportunities in Adolescent Nursing
- Clinical Nursing Resources
- The NHS Constitution for England
- The National League for Nursing Core Values
- Reflective Writing: About Gibbs Reflective Cycle
- Nursing Reflection Essays
- Share to Facebook
- Share to LinkedIn
- Share to email
![student nurse reflective essay on communication Remembering an Event Essay: Examples and Guidelines [Free]](https://custom-writing.org/blog/wp-content/uploads/2020/12/businessman-touching-eyeglasses-is-using-digital-tablet-284x153.jpg)
Throughout our life, we meet plenty of people and participate in various events. If some of them are just regular, the other people or occasions play a critical role in our fates. Your life-changing experience might become a perfect ground for creating a remembering essay.
![student nurse reflective essay on communication Environment vs. Development Essay: Tips & Topics [2024]](https://custom-writing.org/blog/wp-content/uploads/2020/12/storage-tanks-284x153.jpg)
Environment vs. development is a multifaceted present days’ dilemma. On the one hand, environmental problems are increasing year after year. We have more polluted areas on our planet, more polluted rivers, fewer trees that produce oxygen. On the other hand, can we stop development and progress in various fields? Is...

What does an essay look like? At a glance, the answer is obvious. An essay looks like a mere piece of paper (one page or several pages) with an organized text. It’s generally divided into five paragraphs, though there may be more. The essential essay structure includes: Yet, will this...

Some students find writing literary analysis papers rather daunting. Yet, an English class cannot go without this kind of work. By the way, writing literary analysis essays is not that complicated as it seems at a glance. On the contrary, this work may be fascinating, and you have a chance...

These days, leadership and ability to work in a team are the skills that everybody should possess. It is impossible to cope with a large educational or work project alone. However, it can also be challenging to collaborate in a team. You might want to elaborate on importance and difficulties...

Racial profiling is not uncommon. It’s incredibly offensive and unfair behavior that causes most of the protests in support of people of color. It occurs when people are suspected of committing a crime based on their skin color or ethnicity. Unfortunately, most people are unaware that racial profiling is an everyday...

Without a doubt, a natural disaster essay is a tough paper to write. To begin with, when people encounter a disaster risk, it’s a tragedy. Emergency situations can affect hundreds, thousands, and millions of people. These are the crises and events that change people’s lives drastically. So, disaster and emergency...

“You are not only responsible for what you say, but also for what you do not say”Martin Luther There are a lot of other good quotations that can serve as a good beginning for your essay on responsibility and provide good ideas for writing.

Exemplification essays, which are also called illustration essays, are considered one of the easiest papers to write. However, even the easiest tasks require some experience and practice. So, if you are not experienced enough in writing exemplification essays, you will face certain challenges.

You push the snooze button once again and finally open your eyes. It is already 8:50, and your classes start at 9. “I’m going to be late again!”— you think, already in full panic mode. In a minute, you rush out the door half-dressed, swallowing your sandwich on the go....

An essay about Harriet Tubman is to focus on the biography and accomplishments of a famous American abolitionist and political activist of the 19th century. Harriet Tubman was born into slavery, escaped it herself, and helped others escape it. She changed many jobs throughout her lifetime, being a housekeeper, a...

What is a documented essay and what is the purpose of it? It is a type of academic writing where the author develops an opinion relying on secondary resources. A documented essay can be assigned in school or college. You should incorporate arguments and facts from outside sources into the...
You’re awesome! Thanks for these nursing reflective essay writing tips! Thanks! Thanks! Thanks!
Thanks for your nursing reflective essay guide. It really helped me cope with my reflective essay in nursing.

IMAGES
VIDEO
COMMENTS
Communication is a vital part of the nurse's role. Theorists such as Peplau (1952), Rogers (1970) and King (1971) all emphasise therapeutic communication as a primary part of nursing and a major focus of nursing practice. Long (1992) further suggests that communication contains many components including presence, listening, perception, caring ...
I have chosen to reflect on this account as I found the communication a challenging experience. There are several models that can be used in the reflection of practice for example Gibb's Reflective Cycle (1988), Johns Model of structured reflection (1994) and Borton's Reflective Framework (1970). The communication reflection is structured ...
Gibbs model reflection essay reflective practice essay on reflection effective communication effective communication and collaboration improve care. contents ... As a Nursing Associate student, I will continue to develop my understanding of the NMC's Professional Code (NMC, 2018a) and I will achieve the necessary proficiencies by the end of ...
This essay aims to critically reflect on an encounter with a service user in a health care setting. The Gibbs' Reflective Cycle will be used as this is a popular model of reflection. Reflection is associated with learning from experience. It is viewed as an important approach for professionals who embrace lifelong learning (Jasper, 2013).
Communication is a fundamental element in nursing practice. This element can possibly determine patients' satisfaction and even the outcomes of their treatment (Lotfi et al., 2019). The situation described in the paper will exemplify the potential role of communication, which is why it will serve as a Gibbs Reflective Cycle nursing example.
Although reflective writing does improve self-awareness, in health care, focusing attention on something besides the self is critically important. Nurses must be able to observe, listen, and empathize. Reflection offers students the opportunity to shift the focus away from self and encourage objectivity (Kerr, 2010).
1 EXAMPLE REFLECTIVE ESSAY FOR Critical Thinking and Writing for Nursing Students Bob Price and Anne Harrington This example of a reflective essay is presented in association with Price, B and Harrington, A (2013) Critical Thinking and Writing for Nursing Students, London, Learning Matters.
The hook or attention grabber. Thesis statement. Main points of each body paragraph (topic sentence, evidence, examples, illustrations, etc.) Conclusion (restated thesis and call-to-action) With the outline done, you should take a break and resume writing your first draft of the nursing reflection essay.
Understanding the importance of our words and our actions, and the impacts that they can have on people is a great area to reflect upon. Chloe Hawkins is a second-year learning disability nursing student, Northumbria University and 2021-22 Nursing Times student editor. 'The open meeting illuminated the dynamics of leadership and collective ...
The key elements to include in a nursing reflective essay are the inciting incident or event, personal reflections on the experience, specific details to create a vivid setting, and a description of the actions taken by the writer. It is important to avoid including academic details and excessive focus on emotions.
Writing a reflective essay in nursing is a journey into personal experiences, emotions, and insights within the context of your nursing practice. It demands sincerity, self-examination, and an eagerness to learn and evolve. Even though the journey can present challenges, it is an invaluable instrument for personal and professional growth.
Action Plan. In future, I will aim to develop my assertive skills when working with colleagues, in order to ensure that the well-being of clients is maintained. In my next placement, I will make this a goal for my learning, and will discuss this with my mentor to work out strategies for how I can achieve this. *******************.
This manuscript has been submitted to Journal of Nursing Education. Learner Objectives. The learner will: Understand the benefits of reflective writing for nursing students and educators. Recognize the role of the nurse educator in student reflection. Identify the essential components of reflective writing assignments.
Abstract. Introduction: Reflection is formed through deep reflection on the event or a certain clinical position. The aim of this study was to determine the effect of reflection on nurse-patient communication skills of nurses working in emergency departments. Methods: This interventional study was conducted on intervention and control groups ...
15 Best Reflective Essay Topics: Nursing. Empathy and support in nursing. Communication with patients is one of a nurse's most important tasks. Nursing is the art of caring for the patient during illness. The key is not to cause harm but to help afterward. Time management in nursing.
The focus of this scenario is the learning that Emma, a first-year student nurse undertook while on a shift during her fifth week of a ten-week placement on ward A. Emma's key objectives during this placement were: To develop effective communication and relationship management skills. To acquire skills and knowledge for post-operative care ...
Reflection is a highly beneficial tool (Oelofsen, 2012), one that has played a key role in the author's ongoing examination of her practice. In this context, reflection enables a personal insight into the communication process and highlights the inherent challenges of communication and their pertinence to patient care and clinical practice outcomes (Bramhall, 2014).
Abstract. Assertive communication is a skill that many nurses, particularly nursing students, find challenging. This article describes the findings of phenomenological study that set out to explore third-year student nurses' experiences of using assertive communication in the clinical setting. A narrative enquiry approach reviewed six ...
The paper will show emphasise based on communication. This reflection has been chosen to highlight the need for nurses to have therapeutic communication skills in order to provide holistic care and encourage a good nurse-patient relationship. Gibbs (1988) reflective cycle has been chosen as a framework for this paper.
1920927077. Sample Reflective journal. The following are extracts from a Reflective journal written for the course, Reflective Nursing Practice 1 by a first year student, Chrissy Poulos: ALOUR COMMENTSExcerpt from Wee. IDefining nursing is a tough one. I am not su.
Introduction. Communication is defined as a lifelong learning process for nurses, who are intimately involved with clients and their families from birth to death (Balzar Riley, 2008, as cited in Potter and Perry Canadian Fundamentals of Nursing 5th edition, p. 242).
Disclaimer: This essay has been written by a student and not our expert nursing writers. ... Self Reflection on Communication in Nursing. Info: 2130 words (9 pages) Nursing Essay Published: 12th Feb 2020. ... Example Reflective Essay using Rolfe Reflective Model.
Point 1 (evidence, examples, other supportive details) Point 2 (evidence, examples, other supportive details) Point 3 (evidence, examples, other supportive details) Conclusion. Restatement of thesis statement. Final memorable statement. After creating an outline, it would be a great idea to write the rough draft of your nursing reflective essay.