Improving Family Communications How can I improve communications in my family?Here are a few important ways to build healthy communication - Be available: Make time in everyone's busy schedule to stop and talk about things. Even 10 minutes a day without distractions for you and your child to talk can make a big difference in forming good communication habits. Turn off the television or radio. Give your undivided attention to your child. Sit down and look at your child while you talk. Those few minutes a day can be of great value.
- Be a good listener : When you listen to your child, you help your child feel loved and valued. Ask your child about his feelings on a subject. If you are not clear about what your child is saying, repeat what you are hearing to be sure that you understand what your child is trying to say. You do not have to agree with what your child is saying to be a good listener. Sharing his thoughts with you helps your child calm down, so later he can listen to you.
- Show empathy: This means tuning in to your child's feelings and letting him know you understand. If your child is sad or upset, a gentle touch or hug may let him know that you understand those sad or bad feelings. Do not tell your child what he thinks or feels. Let him express those feelings. And be sure not to minimize these feelings by saying things like, "It's silly to feel that way," or "You'll understand when you get older." His feelings are real to him and should be respected.
- Be a good role model: Remember, children learn by example. Use words and tones in your voice that you want your child to use. Make sure that your tone of voice and what you do send the same message. For example, if you laugh when you say, "No, don't do that," the message will be confusing. Be clear in your directions. Once you get the message across, do not wear out your point. If you use words to describe your feelings, it will help your child to learn to do the same. When parents use feeling words, such as, "It makes me feel sad when you won't do what I ask you to do," instead of screaming or name calling, children learn to do the same.
More Tips To Improve Communication- Give clear, age-appropriate directions such as, "When we go to the store I expect you to be polite and stay with me." Make sure your child understands what you have said. Sometimes children do not fully understand the meanings of words they hear and use.
- Praise your child whenever you can.
- Calmly communicate your feelings.
- Be truthful.
- Listen carefully to what your child says.
- Use your talking times as teachable moments – do not miss opportunities to show your child healthy communication.
- Model what you want your child to do – practice what you preach.
- Make sure that when you are upset with your child, she knows that it is her behavior that is the problem, not the child herself.
- Give broad, general instructions such as, "You'd better be good!"
- Name call or blame. "You are bad" should be replaced with "I don't like the way you are acting."
- Yell or threaten.
- Lie or tell your child half-truths.
- Use silence to express strong feelings. Long silences frighten and confuse children.
Keeping Your CoolThere are times when all parents feel that they are out of patience. However, it is always important to find ways to help your child to behave without hurting her feelings. Here are a few ways to calm yourself when you feel stressed, before you try to talk with your child. - Take a few deep breaths very slowly.
- Wait 5 minutes before starting to talk to your child.
- Try to find a word to label what you are feeling (such as "disappointment"). Say it to yourself and be sure that it is appropriate for you child.
- Share your feelings of frustration with your spouse or a friend.
- Do not hold grudges. Deal only with the present.
- Seek professional help if you feel that you have lost control.
Healthy communication with your child is one of the most important and rewarding skills that you can develop as a parent. It also makes the tough parts of parenting (such as disciplining your child) much easier and more effective.  (432) 620-0255 Call us today. Help is available 24/7. The Effects of Poor Family CommunicationCommunication is key component in a successful working family. You communicate with members of the family not just with your words but using language and behavior. If you use negative methods to communicate or avoid communicating at all, this can make matters worse through adulthood and even affect who we become as adults. Poor family communication can include yelling, holding grudges, keeping secrets, blaming, giving the silent treatment, using ultimatums or threats, labeling someone bad instead of the behavior, and bringing harm. If these problems continue, you will never feel close to your family anymore. The way parents talk to their kids or how siblings talk to each other can impact their positive development when they are kids, teens, or young adults. Young people can also get anxiety and depression if there are still ill feelings that never left them. Kids can also develop behavioral problems when they do not respect authority or deal with at-risk behavior like criminal activity and substance abuse. Improper communication leads to false assumptions, feeling you can read their minds, or always jumping to conclusions. When you do not know what is going on with people in your family, it can lead to unnecessary worrying, fear, and concern that can lead to stress. Arguments will start more easily. Your self-esteem could suffer and you will not feel comfortable to talking to anyone in your family. If this disconnection continues to go on, no one will have a care or concern for the other and your family will be broken. The best way to improve family communication is to take some time away from your busy schedule to have a talk with your family members. Make sure it is in a private atmosphere with no distractions like the television or your phone. Listen to what the other person is saying and ask how the other person is feeling. Repeat back what the other person says if you are having trouble understanding. Show that you understand how they feel by giving a gentle touch or a hug. Do not minimize the person’s feelings by saying they are being dramatic or wrong for feeling how they feel. Otherwise, they will not talk to you again. Speak the way that you would want someone to speak to you. It is important to keep that line of communication going so that you will always have your family in your life. Located in downtown Midland, The Springboard Center’s mission is to offer programs and services to treat alcohol and drug addiction treatment using an evidence based curriculum, 12 step programs, diet, nutrition, exercise, emotional, mental and spiritual development for a long recovery. For more information, please call us at 432-620-0255 as we are open 24 hours a day, 7 days a week. Related Posts How Should I Prepare for Rehab? 5 Ways to Keep a New Year’s Resolution in Recovery 28 Recovery Quotes That Will Brighten Your Day- Family & Relationship Issues
Communication Challenges with Family and FriendsNatalie Staats Reiss, Ph.D. is a licensed Psychologist in the state of Ohio (License #6083). She received her Ph.D. in Clinical Psychology from ...Read More Most of us assume that because we have spent a lot of time with a spouse, other family members, or close friends, our communication with them should be relatively easy and effortless. Our thinking probably goes something like this: "my spouse/parent/sibling/best friend knows me very well, so he or she should know what I am thinking and feeling, as well as what I mean." We are often surprised and annoyed when people who are close to us misunderstand what we are talking about. Although it’s tempting to blame the other person, the problem also begins with us. Dr. Boaz Keysar, of the University of Chicago, has spent a career studying interpersonal communication, and has found that communicating with people we know very well is actually more difficult than communicating with people we hardly know at all. His research suggests that problems communicating with our loved ones and friends come from several different factors. First, most people seriously overestimate their ability to communicate effectively. Keysar’s studies suggest that nearly 50% of the time when we think we are understood, we are actually wrong. Because we assume we are being understood, we don’t take the time to check whether our family and friends receive the correct message. Because we communicate with our friends and family frequently, there are multiple opportunities for being misunderstood. Second, we tend to think that our knowledge is transparent, or known by other people. Because of the mental effort that speaking requires, it is often difficult to take another person’s perspective while we are talking. We forget that people, even those who spend a lot of time with us, might not know what we are discussing. For example, you might think that your spouse knows many of the same things as you do (because you have shared many similar experiences) and will therefore automatically follow your conversation. How many times have you said to your spouse, "I thought I told you this already?" Therapists are Standing By to Treat Your Depression, Anxiety or Other Mental Health NeedsExplore Your Options Today Third, because we communicate with family and friends frequently, there are times when our intended message is subtle (e.g., messages that are ambiguous, sarcastic, or meant to convey emotion). Unfortunately, conveying subtle messages is usually difficult. The more subtle the message, the more likely we are to miscommunicate. Worse, the more subtle the message, the less likely we are catch a miscommunication that occurs. For example, if your best friend apologizes for being busy, and you respond "It’s hard to be a good friend", you could mean anything from "You are not being a good friend", to "I understand that you have a lot going on right now". Or, if you tell your spouse "I am happy to take care of it", you could be serious or sarcastic, depending on your intended message. If you combine the above factors, the most challenging situations involve communicating new, subtle information to our loved ones and friends. In these situations, we often use short, ambiguous messages suggesting that the other person already knows what we are talking about. According to Dr. Keysar, it may be difficult to completely eliminate these communication "bad habits", but being aware of our behavior can help. He recommends that we err on the side of assuming that messages we are sending are complicated and likely to be misunderstood. Particularly in an argument or an emotional discussion, check frequently with the other person to make sure that she or he is actually receiving the message that you are intending to send. - Introduction
- How People Change
- Family Secrets
- What Is Freedom?
- Getting Through The Holidays
- For College
- Making Peace With Elderly Parents
- Impact Of Recession On Marriage
- Mixed Or Blended Families
- New Extended Family
- Perfect Family
- Personality Disorder Or Just A Horrible Person
- Husband Jealous Of My Friends And Family
- Is It Just A Name?!
- She's Lied About Everything
- My Family Is Ruining My Relationship With My Boyfriend
- My Boyfriend's Children Won't Accept Me....
- Does My Boyfriend Have Feelings For His Ex Wife?
- I Have Bulimia
- Arranged Marriage
- When Is Enough, Enough?
- Breaking Up
- Soon To Be 15 Year Old Step Daughter Who Is Physically Abusive To Family Members
- I Have Everything I Ever Wanted. Why Am I So Miserable?
- Should I Stay Or Should I Go?
- Is My Sister A Pathological Liar?
- Need Help In Building The Bridges
- Lack Of Affection And Intimacy
- Is He Seeing Someone?
- Marriage Question
- Respect + Anger Managment
- My Husband With Daughter......
- Resentment-Controlling Wife/Passive-Agressive Husband
- Getting Married, Stepsons With Awful Tempers
- Adult Son Interferes With Our Relationship
- Can My Marriage Be Saved?
- On And Off Relationship For Almost 10yrs
- I'm His 2nd Wife. Am I Destined To Play Second Fiddle To His Daughter Forever?
- How Do I Get My Husband To The Psychiatrist?
- Is It Inappropriate To Call My Daughter...
- Trying To Save 37 Years Of Marriage With My Bipolar Husband
- Alcoholism And Family
- Bipolar Obsessive Thoughts And False Memories
- Crazy Mother In Law Ruining Our Mental Health And Relationship
- Caught In The Middle Caring For Elderly Parent
- I Am A Newlywed And Need Help
- Husband's Relationship With His Children
- Substance Abuse
- Chronically Ill Non-Compliant 19 Year Old
- Child With Possible Oppositional Defiant Disorder (ODD)
- Obsession Or Excuse
- The Marriage Corner: How Can I Move Past This?
- The Marriage Corner: Do You Think My Marriage Can Be Repaired?
- I Am Only 26 Years Old
- My Boyfriend Saved A Picture Of A Girl He Slept With In Case We Split Up?
- Adoptive Mother Of 3 Children - SunFlower
- How To Handle My Mothers State Of Mind?
- Should I Fight For My Marriage?
- Why Does My Wife's Old Boyfriend Bother Me?
- How Do We Get Her To Accept Us As Part Of The Family?
- Another Woman
- Boyfriends Daughter
- How Do I Cope With A Parent Who Is Trying To Ruin Me?
- Worried About 4-year-old With Depression
- Same Views On So Much, But Can't Get Along As A Couple
- It's Me Or It's My Mother?
- Considering Divorce After Several Deaths In The Family
- Schizophrenia
- Please Help Me..
- My 19 Year Old Daughter Is Out Of Control
- My 19 Year Old Son
- I Desperately Want To Make This Work
- Marraige Life Of My Parents
- Is This Abuse And What Should I Do?
- My Girlfriend's Family Is Ruining Our Relationship
- I Feel Like I Have Failed - - May 20th 2010
- Relationship With My Bipolar And ADHD Girlfriend
- Huge Disapointment With My Husband
- I Don't Really Care About Anything. What Should I Do?
- What Should I Do?
- My Father, The Sociopath...
- What Is Wrong?
- What Should I Do With My 19 Year-Old Daughter's Anger Issue?
- Dominating Mother
- How To Help Our College Age Son With Depression And Addiction
- Personal Hygiene
- Help Me Please. What Is Going On With Me?
- Parenting A Bipolar Child, Not Quite A Child, Not Quite An Adult
- Am I Being Used?
- Is This Jealous Behaviour Normal In A Child?
- Grandson Behavior
- Husband's Addiction
- Help Or Do Nothing?
- Pregnant Again
- Are My Past Sexual Fantasies Dangerous And Unusual?
- It Is Finally An Emergency. We Need Help. Please.
- Trauma And Drama: Why Are Friends And Family Rejecting Me?
- Why Is My Mom Following Me Around To Take Over My Life?
- Does My Husband Have Bipolar Although The Doctors Said He Doesn't?
- How To Ask If The Pics Are Her?
- Did I Push Them Too Much?
- How Do You Turn Your Back On Your 19 Year Old Daughter?
- What To Do With A Dysfunctional Past
- SHOULD GRANDPARENTS INSIST ON SEEING A GRANDCHILD
- My Husband Wants To Leave Me
- My Husband No Longer Believes
- My Son's Problem
- Why Do I Beat Myself Up Over What They Think?
- Bipolar Sister, Narcissist Boyfriend
- Understanding My Son
- Worried About My Son
- Child Jealous Of Moms Relationship With Her New Husband
- This Guy I Bully
- Is There Help Out There? Lonely Mother Of Three
- Am I Depressed?
- Should I Give Up On This Marriage?
- Dealing With Demanding Mother
- Can You Give Me Some Advice Please?
- 17 Year Old Running The House
- My Needy Son Hates My Boyfriend. How Can I Avoid Choosing One Over The Other?
- Two Intelligent Adults Who Feel They Don't Have Friends
- 19 Year Old Daugter--Out Of Control
- 17 Yr Old Refuses Help With Bi-polar Disorder
- Teen In Full Retreat
- Out Of Control 16 Year Old Nephew
- I Need Help With My Sister
- Get Supported
- Forgotten Or Just Ignored?
- Dealing With A Family Member's Complete Personality Change
- Mother Showering & Sleeping In Same Bed With 5 Year Old
- Zoloft - Good Or Bad
- My Little Sister
- Unattractive Regardless, Why Bother?
- Coping With Narcissistic Behavior
- How To Deal With The Loss Of Family
- Husband's Anger
- Did I Love My Husband And Still Abuse Him Emotionally
- I Have A Hard Time Making Friends With Other Guys
- How To Communicate To A 'feeler'
- How Can I Control Morbid Jealousy
- How Can I Open Up And Become My Old Self Again?
- Advice For My Unhappily Married Friend
- How Can I Tell The Difference?
- Cannot Support Old Friend In Her Affair
- Is Something Wrong With Her?
- Need To Find A Reason For The Abuse
- Mom's Unlisted Number
- How To Help A Womanizing Friend?
- 'Extremely Controling' Wife And Passive Husband
- A Habitual Liar's Lament
- The Way Out Is Through The Door
- Drug Addict Son
- Angry At Ex-Boyfriend
- Violent Sister
- A Marriage Outside The Caste
- Seeing A Married Man
- A Mean, Verbally Abusive Woman
- Mom's Protector
- Busted By A 5-Year-Old
- Getting Along With Narcissistic Relatives
- Possibly Molested Daughter
- Dirty Niece
- Congenital Laziness
- Is Anxiety A Hereditary Factor?
- Abusive Father
- Self-Abusive Step-Daughter
- Paranoid Depression
- (Wo)man In The Middle
- Dysfunctional Family
- My Mother Is Ruining My Life
- Cowardly Stepdad
- Daughter's Violent Marriage
- My Father Dislikes Him
- Histrionic Sister-in-Law
- Personality Disordered Grandmother
- Mom's Venting
- Unhappy In An Arranged Marriage
- Toxic Parents
- Boarding School Blues
- A Situation For Tough Love?
- Depression Affects The Entire Family
- Internet Relationship
- I Want To Leave, But For The Children ...
- Public Menace
- Self-Injuring Sister
- Family Boundaries
- Dealing With Divorce
- Blossoming Paranoia?
- Trashed House
- What To Treat First?
- Love Triangle
- Problematic Parents
- Managing Priorities
- Mommy's New Boyfriend
- Busy And Wanting
- He's Not Himself
- Jealous Of My Fiance's Family
- Different Religions
- My Dad The Dictator
- My Children Aren't Speaking..
- Dogs Instead Of Children?
- My Wife Is Depressed
- Problems With My Daughter
- Anorexia Impacts The Whole Family
- Family Therapy Near Me - How To Find A Family Therapist
- Love Means Knowing How To Say You're Sorry
- Until Next Time: The Benefit Of Healthy Goodbyes
- Improve Your Relationships In Two Minutes
- When Is It Time To End A Relationship With A Lover, Friend Or Family Member?
- Learning To Navigate In-law Relationships As Newlyweds
- Working With Siblings Toward Caregiving Solutions - Part II
- When Caregiving Creates Tension Among Siblings - Part I
- Managing Tense Family Relationships During The Holidays - Part II
- Managing Tense Family Relationships During The Holidays - Part I
- What Is A Family "System?"
- Redefining The Idea Of "Relationship"
- Challenges Increase For Family Caregivers When Cognitive And Behavioral Issues Are Present
- What Keeps A Family Together?
- The Cultural Dimensions Of Family
- Cultivating Healthy Relationships Take Practice; Lots Of It
- Four Traits Of A Healthy Family
- Eight Tips For Talking To Your Aging Parents About Important Issues
- Establishing Healthy Family Relational Boundaries
- Helping Adult Children Affects Well-Being Of Older Parents
- Can You Really Multitask?
- Toxic Families: Navigating The Challenges Of Being A Family Scapegoat
- Holidays And Family Conflict
- Facing Grief And Loss During The Holidays
- The Holidays And The Meaning Of Giving
- The Problem Of Children And Blended Families
- When A Family Is Dysfunctional, The Deadlock In Washington
- The Elderly, Terminally Sick And Assisted Suicide
- Parents, The Empty Nest And Grads At Home
- The Emotional Needs Of Older Adults
- Parents Who Cannot Let Go
- Celebrating The Ordinary
- Family Life: Some Thoughts About The Role Of The Father
- Does Parental Longevity Impact Children's Personality?
- Roles In Relationships
- Creative Couple/Family Counseling: Discovering The Paradoxical Pass In The Impasse
- Dementia Affects The Whole Family
- Imago Relationship Therapy
- Marriage And "That Seven Year Itch"
- The Family: Its Stories And Myths
- Acceptable, Cute Aggression
- Childhood Television Viewing And Violent Behavior
- Making Your Relationship Work
- 5 Habits Of Emotionally Intelligent Families
- Own Being Responsible? -- Absolutely, Make Others Responsible? -- You Must Be Kidding!
- Nagging...or Motivational Speaking?
- A Lighthearted Response To Holiday Family Dysfunction
- Grieving My Father's Death: 46 Years Later
- When The Holidays Aren't So Jolly - Tips For Coping
- Don't Rain On The Parade
- Men, Women And Dysfunctional Relating
- Marriage, Are You Afraid Of Emotional Intimacy?
- Warning: Child Centered Is Not Child Friendly!
- Should I Divorce My Parents Or Forgive Them?
- "Love And Logic" Principles Of Parenting
- Independence Day, The Importance Of Democracy
- On Laughing And Laughter
- Is Your Partner Still Relating To His/Her Ex?
- Families And Groups With Rigid Boundaries
- Adoption, Finding The Birth Parents
- My Mother/Father Has Alzheimer's Disease
- Moving Back Home Again
- Boundaries And The Addicted Family
- Family Boundaries And The Parentified Child
- Am I Ugly? A Discussion Of The Young Teenager In Trouble
- Parents, Students, Teachers And Academic Performance - Everyone Plays A Role
- The Impact Of Divorce On Families
- Bipolar Disorder, Receiving The Diagnosis
- Catch A "Wild Pitch?" You Must Be Kidding!
- Why Do Couples Divorce?
- Admit Fault And Move On
- Divorce And Remarriage, The Blending Of Families
- Why Do People Marry?
- Violence Within Marriage
- How To Have A Happy Marriage
- A Requiem For A "Last Angry Man"
- Violence Against Women
- Impulse Control, Wanting...Waiting...Savoring
- The Substance Abuser And Multi Family Systems Therapy, Part One
- "On Being Certain," A Wonderful Book By Robert A. Burton, MD
- Mental Illness, A Failure To Understand
- The Only And Correct Way To Parent
- Work And Family, Are Boundaries Fading?
- The Impact Of Divorce On...
- Fathers And Father's Day
- When Life Gives You Lemons, Make Lemonade: Coping With Depression As A Result Of Economic Stress
- Revisiting Your Childhood Home, "Remembrance Of Things Past"
- April 15th: What Are You Worth?
- Some Reflections On Successful Marriages
- Teenagers, Technology And Parents
- Stepfamily Success: How Do You Know When You Can Relax?
- Anger Throughout The Generations
- Family Dinner, Do Families Interact And Talk To Each Other Any Longer?
- Step Dads, Don't Expect To Bring Order Into Your New Family
- He Doesn't Feel The Same Way About Me...
- Of Marriage, Money And Lies
- Strategies For Success For Stepmothers
- "That's Not Fair,...."
- Narcissistic Vs. Antisocial Or Sociopathic Personality Disorders
- Marriage, Family, Stress And Finances
- How To Protect Your Marriage In A Step Family
- It's About Relationships, Not Food!
- Stepfamily, Blended Family, Remarried Family Or Married With Baggage Family?
- Grandparents Raising Their Grandchildren
- A Debate Rages Over Education And Parenting
- Things I Learned From My Father's Dying
- Choosing To Be Childless, Is It Selfish?
- Setting Healthy Limits--It Can Be An All-Win!
- Managing Holiday Stress: Families + Holidays Do Not Always = Warm And Fuzzy Times
- Student Academic Performance
- Life, Death And Relationships
- The Pleasure, Beauty And Power Of Music
- Coping With People Who Are "Difficult"
- "My Mother Is Ruining My Life"
- Of Babies And Kisses And Hugs
- Empathy Vs. Blame
- A Legacy Of Two Elders
- Common And Mature Defenses, And Beyond
- Narcissism And What's Underneath
- Child Abuse And The Role Of Parental Denial
- Women Who Love Too Much, Are You One Of Them?
- Some Thoughts About Perception, Communication And Disagreement:
- Teenagers And Depression: Their Families And Psychotherapy
- On Demeaning, Devaluing And Bullying: Discussions Of Points Of View
- Married 40 Years....And We Never Had ONE Fight
- Family Therapy: A Different Approach To Psychotherapy
- On The Family As A System And The Problem Of Triangulation
- Arguing And Marriage: Go Together Like A Horse And Carriage
- Depression And Marriage
- How Do You Cope When A Loved One Has An Addiction?
- Handling The Stress Of The 2008 Holiday Season
- On Loneliness, Warmth And Making Friends
- Birthdays, Graduations And Other Celebrations:
- Infidelity, Why Do People Cheat?
- The Influence Of Culture On The Expression Of Depression
- Some Thoughts About Multiple Births
- On Fathers On Father's Day
- Summer Vacation, Children And Adolescents
- Teenage Self Injury
- "I Owe, I Owe, So Off To Work I Go," Spending, Debt And Stress
- Memories: Who Is Correct?
- Denial: The Good And Bad Of This Defense Mechanism For Relationships
- Transference: The Patient's Love For The Therapist And An Answer To A Graduate Student's Question
- Involving Fathers In The Treatment Of Children With ADHD
- On The Importance Of Fathers
- Couples And Quarrelling
- The End Of Vacation, Back To School And Work
- The Empty Nest, Or Is It?
- Addiction And The Family
- In The Middle
- Mother's Influence On Psychological And Physical Health Extends To Old Age
- Adult ADHD: The Importance Of Learning Social Skills
- Interfaith Dating And Marriage
- Money And Marriage
- Communication Challenges With Family And Friends
- If Not Now, When?
- "But You Can Choose Your Friends"
- Eating Disorders And Family Boundaries
- Can Men And Women Be Friends?
- Codependent And Enabling Behaviors
- Marriage And Friendship
- Points Of View
- Non Verbal Communication
- Bulimia Nervosa
- "Why Didn't I?"
- Stuffing It: The Culture Of Not Speaking
- Single And Satisfied: Is Marriage Still In?
- Lonliness Leads To High Blood Pressure ...
- Family Squabbles Can Derail Recovery From Cancer Surgery
- Sibling Bullies May Leave Lasting Effects
- Family Troubles Tied to Poorer Dental Health, Study Discovers
- Family Meals May Defuse Cyberbullying's Impact, Study Says
- When Parents Need Care, Daughters Carry the Burden: Study
- Health Tip: Avoiding Parental Burnout
- Spats, Conflicts Can Raise a Woman's Blood Pressure
- Frequent Arguments Might Be the Death of You
- How You Parent Is Partly Genetic, Study Suggests
- Life Issues
- Oppositional Defiant Disorder
- Mens Health
- What Is Addiction?
- Signs, Symptoms, & Effects Of Addiction
- What Causes Addiction?
- Mental Health, Dual-Diagnosis, & Behavioral Addictions
- Addiction Treatment
- Addiction Recovery
- Information On Specific Drugs
- Homosexuality And Bisexuality
- Internet Addiction
- Childhood Mental Disorders
- ADHD: Attention Deficit Hyperactivity Disorder
- Anxiety Disorders
- Bipolar Disorder
- Depression: Major Depression & Unipolar Varieties
- Eating Disorders
- Childhood Mental Disorders And Illnesses
- Dissociative Disorders
- Impulse Control Disorders
- Internet Addiction And Media Issues
- Intellectual Disabilities
- Obsessive-Compulsive Spectrum Disorders
- Post-Traumatic Stress Disorder
- Somatic Symptom And Related Disorders
- Tourettes And Other Tic Disorders
- Physical Mental Illness Flipbook
- Suicide Rates Vector Map
- Alzheimers Disease And Other Cognitive Disorders
- Chronic Obstructive Pulmonary Disease
- Colds And Flu
- Crohns Disease / Irritable Bowel
- Heart Disease
- High Blood Pressure
- Memory Problems
- Men's Health
- Sexually Transmitted Diseases
- Sleep Disorders
- Women's Health
- Anger Management
- Mindfulness
- Stress Reduction And Management
- Weight Loss
- Disabilities
- Domestic Violence And Rape
- Grief & Bereavement Issues
- Pain Management
- Relationship Problems
- Self Esteem
- Terrorism & War
- Health Insurance
- Health Policy & Advocacy
- Health Sciences
- Mental Health Professions
- Alternative Mental Health Medicine
- Medications
- Psychological Testing
- Psychotherapy
- Virtual Outpatient Eating Disorder Treatment
- Child Development And Parenting: Infants
- Child Development And Parenting: Early Childhood
- Sexuality & Sexual Problems
- Homosexuality & Bisexuality
- Aging & Geriatrics
- Death & Dying
- Physical Development: Motor Development
- Vygotsky's Social Developmental Emphasis
- Bullying & Peer Abuse
- Family And Relationship Issues
- Grief And Bereavement
 - People Directory
- Safety at UD
 Fact Sheets And Publications- Families and Relationships
- Financial Health
- Health Insurance 4 U
- Mindfulness
- Mental Wellness & Prevention (ROTA)
- Ag-We’ve Got Your Back
- Physical Activity
- Food Safety
- Community Health
- Request a Program
- Animal Science
- Beginning Farmer Program
- Lima Bean Breeding Program
- Production Recommendations
- Variety Trial Results
- Small Grains
- Pest and Disease Database
- Sustainable Landscapes
- Irrigated Corn Research Project
- Soybean Irrigation Response Study
- Irrigated Lima Bean Yield & Quality
- Subsurface Drip Irrigation
- Irrigation Research Projects and Studies
- Moths and Snap Pea Processing
- Silk Stage Sweet Corn - Action Thresholds
- IPM Hot Topics
- Alfalfa Pest Management
- Field Corn: Pest Management
- Small Grains: Pest Management
- Soybeans: Pest Management
- Commercial Field Crop Disease Management
- Commercial Fruit & Vegetable Crop Pest Management
- EIPM Implementation Projects
- Pollinators
- Research and Extension Demonstration Results
- Brown Marmorated Stink Bug (BMSB) Management, Research, and Resources
- Certified Crop Advisor Program
- Publications
- Applicators and Educators
- UD Plant Diagnostic Clinic
- Weed Science
- Disease Management
- Variety Trials
- Crop Production
- Registration Help
- Delaware 4-H Staff Directory
- New Castle County 4-H
- Kent County 4-H
- Sussex County 4-H
- Delaware 4-H Foundation
- Shooting Sports
- Civil Engagement and Leadership
- Volunteering
- Club Management
- 4-H Afterschool
- Delaware Military 4-H
- Citizenship
- Statewide Drug Prevention & Lifeskills Program
- Resources for Teachers
- MyPI Delaware
- The STEAM Team!
- Leadership Opportunities
- Scholarships & Awards
- 4-H by County
- Become a 4-H Volunteer
- Delaware State Fair
- Farm Succession and Estate Planning
- Building Farm and Farm Family Resilience
- Legal Resources for the Delaware Agriculture Community
- Farm Business Management
- Farm Vitality and Health Project
- Personal Financial Management Initiatives
- Climate Variability and Change
- General Information on what, how, why and where soil is tested
- Soil Testing Program Forms
- Nutrient Recommendations
- New to Delaware
- Grow Your Own Food
- Backyard Composting
- A Day in the Garden
- Become a Master Gardener
- Garden Workshops
- Gardener Helplines
- Garden Smart, Garden Easy
- Junior Gardener Program
- Kent County Scholarships
- Garden Advice Program
- Demonstration Gardens
- Master Naturalist Program
- Nutrient Management Certification
- Continuing Education for Nutrient Management
- Nutrient Management Planning Resources
- Commercial Nutrient Handler Resources
- Poultry Litter and Manure Management
- Turf Management
- Agriculture Notebook
- Horticulture Handbook
- Agriculture & Horticulture Handbooks
- Soil Fertility
- Delaware Climate Change Coordination Initiative (DECCCI)
- Salt Impacted Agricultural Lands
 Communication Skills for Your FamilyCommunication is the basic building block of our relationships. It is through communication that we convey our thoughts, feelings, and connection to one another. - Developing good communication skills is critical for successful relationships, whether parent, child, spouse, or sibling relationship.
- We all have had experiences where (1) we have felt heard and understood and we’ve all had experiences (2) where we have felt misunderstood and even ignored.
- Generally, when we feel heard, we are less angry, stressed, and more open to resolving problems than when we feel misunderstood. Feeling heard and understood also develops trust and caring between people.
Communication is a two-way process. - For communication to happen there must be (1) a sender—who conveys a message—and (2) a receiver—to whom the message is sent.
- In successful communication the sender is clear and accurately conveys the message she is trying to send. Also, the receiver clearly understands the message.
- Miscommunication occurs if the sender does not send a clear message and/or the receiver does not understand the message sent by the sender.
Many things can get in the way of good communication. For example: - When we assume we know what others are thinking, or that they should know what we are thinking.
- When we focus on what we want to say while others are talking—instead of listening to them.
- When we bring up other problems and issues unrelated to the topic at hand.
- When we assume we know what is right for others and try to convince them of this.
All of these things either keep us from sending a clear message or keep us from receiving the message the other person is trying to send. Communicating well takes practice and effort. It is not something that comes naturally for most of us. Below are some keys to good communication. These skills and techniques may seem strange and awkward at first. But if you stick with them, they will become natural in time. As an added bonus, you will improve all of your communication with others (inside and outside your family). Active Listening Active listening is a way of listening to others that lets them know you are working to understand the message they are sending. - Make sure your body language conveys to them that you are interested and listening. You can make eye contact with them, turn your body toward them, and nod as they are talking to let them know you are listening.
- Reduce any distractions that will keep you from focusing on their message. Try to stop whatever you are doing that may distract you from their message—such as watching television or trying to read while the person is talking to you. You may need to tell them, “I will be better able to listen to you once I am done with ____. “ Trying to listen while doing other tasks usually does not allow one to clearly hear the message.
- Listen for the content and the feelings behind the words. Do not just listen to the content of what is being said. Listen for the feeling that the person is trying to convey to you. Are they expressing joy, sadness, excitement, or anger—either through their words or body language?
- When the person has finished talking, paraphrase back to them what you heard them saying. “What I am hearing from you is......”“It sounds like ..... was very upsetting for you.”
- Do not offer advice to the person. When we offer advice—especially when it was not asked for—this often shuts down communication. The person first needs to know that you have understood them and that they have sent their message clearly to you.
You will be surprised at how your conversations and relationships change when you focus on listening to the other person— rather than thinking of your next response. Teaching Children to Communicate Children have to learn how to express themselves clearly and how to listen to others. - From the moment children begin to utter sounds, they are learning how to communicate. They are learning how to get the attention of others and how to get their message across. They are also learning that communication is a two-way process.
- Children learn their skills from how we respond to them and how we communicate with them.
One of the first steps in teaching our children is for us to listen actively to them. - When we actively listen to children, we are letting them know that they can send a message and that their message is important to us. As noted before, it is important that we give them our full attention—listening for the feelings as well as the content of their message. We must restrain from offering advice right away.
Second, we need to actively teach children how to listen. - The child needs to focus on the person who is talking—again eliminating as many distractions as possible. This may mean turning off the television, asking them to look at you, or having them come in the same room with you while you talk with them.
- Just as we give them our attention, we need to teach youngsters to give their attention to others.
- To be sure they have understood your message, ask youngsters to repeat back to you—in their own words—what they heard from you. In this way, you are teaching them to paraphrase what they have heard.
- Children can also be asked what feeling they are picking up from you. Are you happy, irritated, or sad? In this way they can begin to connect feeling and content.
- If the child does not repeat the message back clearly, this offers a time for clarification and another opportunity to teach that good communication takes effort —and that we sometimes don’t get it right the first time.
Finally, children learn the most by communicating with us and by watching how adults communicate with each other. - We need to be sure to be good role models and to take the time to listen and clearly send our own messages.
Family Communication More people = more complex communication. - When two people are involved, there is the opportunity for one relationship.
- When three people are involved, there is the opportunity for three relationships.
- With four, there are six possible relationships.
- With five, there are ten possible relationships, and so on.
- all family members can feel heard and understood and
- conflicts can be resolved.
Families are faced with balancing the needs and wants of many different people. Naturally conflicts are going to arise. - It is impossible for everyone’s needs to be met all the time.
- Compromise does not mean that there is a winner and a loser—but rather that a “new solution” has been found.
- Generating “win/win solutions” challenges us to be creative in developing solutions to problems—rather than focusing on our own needs or wants.
- To come up with “win/win solutions,” family members need good communication skills—so that everyone’s point of view and suggestions are expressed clearly and heard by the other family members.
Here are some ways to come up with “win/win” solutions: - It is important that all persons experiencing the conflict be included—even if this means calling a 10-minute “time out” so people can calm down. (Set the kitchen timer, and have people run around the block—or use some similar positive way to help people cool down.)
- Use neutral language. This means that family members may not name-call or pass judgment on other’s ideas or needs.
- Each person’s request needs to be considered. Each person’s opinion needs to be heard.
- Everyone needs to use their active listening skills (outlined before)—paraphrasing the points of view of other family members.
- Once everyone feels heard and understood, then the process can move to generating new solutions to resolve the conflict.
- The group should generate as many new solutions to the problem as they can— focusing on how to resolve the problem, not just how to meet one’s own needs.
- Keep a list of all the solution ideas that are generated.
- Some of the solutions can be silly and outrageous. Humor helps us relax our minds, which can help us do our best thinking.
- When all the possible solutions have been generated, go through each idea and discuss it. Would this solve the problem? Could we actually do it? How hard or easy would it be to do this?
- The group can vote on the best solution. If only 2 people are involved, then they must agree on a solution before the issue is considered resolved.
UD Cooperative Extension This institution is an equal opportunity provider. In accordance with Federal law and U.S. Department of Agriculture policy, Cooperative Extension is prohibited from discriminating on the basis of race, color, national origin, sex, age, or disability. College of Agriculture & Natural Resources Cooperative Extension- Health & Well-being
- Agricultural Programs
- 4-H, Personal & Economic Development
- Environmental Stewardship
 Additional Links- Faculty & Staff Resources
531 South College Avenue Newark, DE 19716 (302) 831-2501  An official website of the United States government The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site. The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely. - Publications
- Account settings
Preview improvements coming to the PMC website in October 2024. Learn More or Try it out now . - Advanced Search
- Journal List
- HHS Author Manuscripts
 Communicating with Patients and Families Around Difficult Topics in Cancer Care Using the COMFORT Communication CurriculumElaine wittenberg. Department of Communication Studies, California State University, Los Angeles, CA. City of Hope Comprehensive Cancer Center, Duarte, CA. Elisa KanterChapman University, Department of Communication, Orange, CA. Objectives:To examine nurse communication in cancer care and offer communication strategies for quality palliative care nursing. Data Sources:Communication strategies offered are based on the COMFORT Communication curriculum, an evidence-based communication training program. Conclusion:Whole-patient assessment, a major component of palliative care, involves communication that includes eliciting the patient’s story, addressing health literacy needs, being mindful of burnout, and relating to the patient and family. Implications for Nursing Practice:Quality communication skills are essential to oncology nursing, especially given their vital role in cancer care. Communication between nurse, patient, and family members involves more than just providing information. It includes discussing a range of topics, encouraging the sharing of feelings and fears about the illness, treatment, and prognosis, and helping patients and family members find a sense of control and a search for meaning and life purpose. 1 Nurses with strong communication skills have been shown to positively influence cancer patients’ satisfaction, improve overall well-being, and influence patients’ experiences. 2 – 5 However, oncology nurses rarely receive formal instruction on communication as part of their clinical training. 6 Nurse communication training is still relatively new and few training programs provide comprehensive skill training for palliative care. Existing programs have focused on discussions about fertility, 7 self-efficacy in responding empathically, 8 and discussing death, dying, and end-of-life goals of care, 9 and have not included vital palliative care communication training skills such as ways to include family members, discussing social, psychological and spiritual care topics, and team-based delivery of care. 1 Overall, palliative care communication training tends to be physician-focused, with only a smaller amount of work devoted to nurses specifically. However, the nurse’s role is inherently different than the physician’s role and involves talking with patients and families once they have received bad news, discussing spiritual and religious concerns, and talking with physicians and the oncology team about patients and family members. 10 Often excluded when information is provided to the patient and family, nurses report discomfort, lack of role definition, a fear of taking away hope, and a lack of time for participating in discussions with cancer patients and their families. 6 Communication barriers result in compromised psychosocial care for patient and family because nurses lack experience with screening tools and do not know how to approach sensitive topics. 11 Several barriers to effective communication for oncology nurses have been identified, including poor communication among the interprofessional team, 11 differing expectations among clinical staff, lack of skills for providing empathic care to patients and family members, the challenge of assessing patient expectations, how to initiate discussions about end of life, and explaining palliative care. 12 By its nature, oncology nursing demands more attention to palliative care communication because it attends to both the patient and family and serves to coordinate many factions across a potential of multiple care settings. Patients and family members expect nurses to be honest when sharing information and answering inquires, to ask about the patient’s values and goals, take time to listen, and to collaborate with health care team members. 13 Given the frequency of interaction between oncology nurses and patients and their families, it is crucial that oncology nurses possess strong palliative care communication skills to provide quality cancer care. 14 This article will offer communication strategies based on the COMFORT Communication curriculum (Comfort Communication Project, Los Angeles, CA), program funded by the National Cancer Institute. 15 COMFORT Communication CurriculumCOMFORT is an acronym that stands for the seven communication (C-Communication, O-Orientation and options, M-Mindful communication, F-Family, O-Openings, R-Relating, T-Team). Table 1 shows an overview of the curriculum and content of each module. Communication research based on clinical observations of terminal prognosis meetings with dying patients, hospice and palliative care team meetings, semi-structured interviews with palliative care team members, and extensive longitudinal research of patients and families from the point of diagnosis through death and bereavement 1 gave shape to the identification of the seven modules. 16 By integrating communication theory into clinical research, the curriculum was detailed in a volume on communication in palliative nursing. 17 Overview of the COMFORT Communication Curriculum | |
|---|
| Module | Communication processes |
|---|
| ommunication | Understanding the patient’s story
Recognizing task and relationship practices | | rientation and Options | Gauging health-literacy levels
Understanding cultural humility | | indful communication | Engaging in active listening
Understanding nonverbal communication
Being aware of self-care needs | | amily | Observing family communication patterns
Recognizing caregiver communication patterns
Responding to the varying needs of family caregivers | | penings | Identifying pivotal points in patient/family care
Finding common ground with patients/families | | elating | Realizing the multiple goals for patients/families
Linking care to quality-of-life domains | | eam | Developing team processes
Cultivating team structures
Distinguishing successful collaboration from group
cohesion |
Source: The COMFORT Communication Project developed by Elaine Wittenberg, PhD and Joy Goldsmith, PhD ( www.CommunicateComfort.com ), revised 2016. 15 With funding from the National Cancer Institute, the nurse communication curriculum was created for a 2-day training course for implementing evidence-based palliative care communication skills into practice. Clinical nursing faculty and communication researchers were brought together to teach the curriculum. To date, COMFORT communication training has been provided nationwide to 269 oncology nurses who have trained an additional 6863 other health care professionals at their home institutions. COMFORT has shown to improve clinician self-efficacy, attitudes toward communication, and reduce providers’ apprehension about communication. 18 – 20 Subsequent research with the curriculum has shown improvement in nurses’ attitudes, comfort levels, and perceived self-efficacy regarding palliative care conversations 21 and improvements in nurse-perceived confidence in initiating difficult communication topics with family caregivers. 22 Highlighted below are summaries of the four most popular modules of the curriculum (modules C, O, M, R), derived from a culmination of a review of the literature, efficacy research, concepts grounded in communication theory, and feedback from nationwide nursing audiences and expert clinical faculty. C-Communication (Clinical Narrative Practice)Fundamental to the goal of palliative care in providing holistic, comprehensive care focused on the patient’s quality of life, nurse communication should involve clinical narrative practice to capture an awareness of the patient/family life experience and incorporate that experience into communication about cancer. Clinical narrative practice is about narratuves or the stories of our patients’s lives. It is defined as being with and relating to others while honoring the patient’s voice and lived experience. When gathering information about the patient/family, nurses should ask the patient/family to recall the cancer story. Storytelling is a natural form of human interaction and stories of illness reveal how health is defined, how symptoms and concerns are managed, and how care is evaluated. Stories also reveal understanding about the cause of cancer and personal risk of cancer, 23 help patients and families make meaning and manage identity, and reveal perceptions of reality. 24 The patient’s story reveals his/her account of events and understanding, the circumstances of the illness in terms of heredity and life events, their living environment and occupation, and personality. Stories provide insight not gained through routine assessments. 25 Clinical narrative practice involves understanding the illness story 26 and tailoring communication to help the patient/family take control and find “alternative ways of being ill.” 27 Frank 27 defines this as the quest narrative, when the story of illness is viewed as a journey from which something will be gained. As oncology nurses hear the patient’s story, they should engage in relational communication by practicing active listening strategies. Each patient/family has a unique life story and a unique illness story. 28 Focus on gaps, ambiguities, and conflicting plots within the story. The patient’s history can reveal common forms of self-blame (life decisions/actions that led up to the illness, feelings of guilt for poor decisions, and the desire to cure at all costs). Encourage reflection on loss and the changes cancer has brought to everyday living. 29 Table 2 provides example questions to ask patients that promote reflection on life and can aid in helping the patient identify values and goals for care. Questions to Promote Reflection on Life | • “How has your illness (or his/her illness) affected your life and your relationships?” | | • “How do you think ignoring this will affect your life?” | | • “How does your illness (or his/her illness) reflect on you as a person?” | | • “How do you see the future?” | | • “How are you affected by others’ opinions?” | | • “What do you think influences this experience?” |
By learning the patient’s story, nurses can help families consider all dimensions of quality of life, create new solutions and plans, and explore alternative hopes for the future. Nurses can help the patient/family make meaning of what is happening, promote understanding and acceptance, and encourage reflection on how the illness has impacted daily life. To accomplish this, statements should explicitly recognize the patient’s life, elaborate on how illness impacts the patient’s life, and acknowledge the loss/change in life. In this manner, information is incorporated into important aspects of the patient’s life to promote understanding, as in the following example: A 74-year-old woman, Lois, with newly diagnosed non–small cell lung cancer was introduced to the palliative care team to discuss management of her dyspnea and goals of care. She had smoked 1 pack of cigarettes per day for 40 years but had recently quit; she has significant COPD and limited activity because of impaired pulmonary reserve. Her husband of 50 years has dementia and Lois cares for him in their home; he is verbal and capable of some self-care activities. One daughter lives nearby and assists with shopping and other errands, although she is employed full time and has a family. A son lives at a distance with his family and has limited financial means to visit frequently. The patient has approximately an 18-month prognosis and will undergo chemotherapy. Explicit Recognition of the Patient’s Life“Fifty years of marriage is a very special life accomplishment, and so is quitting smoking. Congratulations on this achievement. You must have a lot on your mind with his care and your difficulty breathing.” Elaboration of the Illness in the Context of the Patient’s Life“Your cancer can be treated with chemotherapy, but it will be very hard on you, making it more difficult for you to care for Wendell, and it will not get rid of the cancer. Over time, it will not be possible for you to take care of Wendell. How are you feeling about all of this?” Acknowledgement of the Loss/Change in Life“After caring for him and being together for so long, we understand that your inability to care for Wendell will be a major loss. You will need a lot of support.” O-Orientation and OptionsOncology nurses bridge the divide between the language of medicine and the language of everyday life. They do this by helping patients and their families understand health within the context of daily living, translating medical words by using metaphors and adjectives, and conveying to the team what the patient and family understand and do not understand. When communicating about cancer, it is important that nurses provide orientation to the cancer stage by describing the big picture of a diagnosis (orientation) and summarizing the disease path (options). Nurses must explain options that have been provided to the patient and their family, and tailor the format and modality of information presentation. For patient/family, the words used in everyday life make sense of health and illness. Body parts and functions are identified using plain language like-- puke, shaky, weak. Illness is understood by how it impacts work, family needs and expectations, and social relationships. On the other hand, providers, institutions, and online/printed material use the voice of medicine---nausea, malaise, activities of daily living. Medical terms, jargon, acronyms, and medical-speak identify parts of the body, procedures, and tests. 30 These are foreign and disorienting for a sick person and his/her family. Oncology nurses play a critical role during cancer care because they are often asked to translate medical terms, answer questions about the disease, diagnosis, and prognosis, and explain treatment and side effects. Conversations about cancer need to match the health literacy of the patient family. Health literacy is different than ‘literacy,’ in that it requires more communication skills than reading. For example, collecting and selecting the best and most useful information and then acting on the information demands more than simply reading a set of instructions. Family and patient must be able to receive, acquire, understand , and use information to be health literate. Health literacy includes the language you use when communicating with patients/family (face-to-face or otherwise), the context of the interaction (are you in the ICU, ER, multiple patient room), culture (do you and the patient/family have the same cultural background), communication skill levels, and technology . Matching the health literacy abilities of a patient/family is central to delivering quality care. 31 The case of Mr K demonstrates the many components of health literacy to consider when providing care: The primary treating team and ICU team have arranged for a discussion about goals of care with first- and second-generation family members of Mr K, a 63-year-old gentleman of Asian descent who has been in the ICU for 7 days. He remains ventilated and unresponsive, without evidence of being able to be weaned from the ventilator. The need for tracheostomy placement versus revision to the plan of care is the focus for the meeting. A conference room has been reserved because the patient is intubated and unable to participate in the conversation. A pre-meeting is held among the health care providers, at which time the oncology nurse who has worked closely with the patient informs the other providers of the importance of this family’s cultural background. In particular, he notes that if options are provided, the family will always choose whatever the doctor recommends, because doing otherwise would reflect disrespect, even if they know that the patient would disagree with the doctor’s recommendation. Health Literacy ComponentsIt will be important to provide a thorough introduction of each provider and his or her role. Family members will be confused by meeting three sets of providers (oncology treating team, ICU team, and palliative care team). The meeting should begin by orienting the family to the three services and how they work together. A pictorial chart or visual aid should be used to explain. The conference room should be large enough, so that all family members can sit down. Team members should be aware of where they sit; the team should not sit opposite the family. Team members should disperse and sit among the family to demonstrate partnership-building and decrease authority and hierarchy. Family members and health care team members should silence pagers and cellular phones to reduce interruptions. A translator may be needed. The pre-meeting huddle by the team should include a discussion of any language barriers for this family. A team member should be designated to ask the family about cultural needs regarding care. Communication SkillsIn a large family meeting, it is likely that communication skills among family members will vary. It is also likely that there is a member of the health care team that has already established a relationship with this family. The team should give careful consideration to who should lead the family meeting. A patient and family’s cultural and social background are also important aspects in orienting patient and family about cancer. Thirty-six percent of all Americans have basic or below-basic health literacy, with older Americans and women aged 50–79 from all ethnic groups having the most difficulty communicating with providers. 32 There are several cultural and social factors that contribute to a patient’s health literacy level, including their level of acculturation and language, limited English proficiency, the use of translators in explaining options, a lack of available educational materials in languages other than English, and their individual health beliefs. 33 – 35 Cultural factors may affect a patient’s treatment and result in a limited desire or ability to participate in care, a misunderstanding of cancer stage/stage awareness, less desire/need for cancer information, inaccurate assessments of risk and fewer questions asked to health care providers. Oncology nurses should use plain language as a strategy to reduce the gap between provider and patient/family health literacy levels. Using plain language includes using an active voice (eg, “Use your inhaler”) rather than a passive voice (eg, “After you have used your inhaler”). Plain language also involves speaking in the second person, limiting jargon, and defining new words (eg, everyday talk vs. health care talk). When using plain language, most sentences should have 15 words or less, limiting the information provided at one time. A list of tools for developing plain language materials can be found in Table 3 and includes a clear communication index for help translating medical terms as well as Web sites for evaluating the readability of written materials. Finally, the Plain Language Planner for Palliative Care (PLP) is a recommended resource for practicing plain language. The PLP is a tool for communicating about medications and symptoms in plain language at the 6 th grade level. The PLP translates common medications and symptoms in palliative care and oncology treatment and side effects and includes English and Spanish translations. The PLP is part of the Health Communication iPhone smartphone app and is available for free download in the iTunes store. Tools for Developing Plain Language Materials ∘ Health Literacy Measurement Tools (revised)
| ∘ Check the Readability Level of writing
| ∘ Health Literacy Toolkit for Providers
| ∘ Training by CDC for Practicing and Teaching Health Literacy
| ∘ CDC Clear Communication Index
| ∘ CDC Developing Materials Using Plain Language
|
M-Mindful CommunicationMindful communication in palliative care includes reducing self-talk, avoiding judgment about patient and family or how an interaction will proceed, and the ability to adapt to changes in the interaction. A nurse can be in the moment with patient and family by avoiding pre-determined scripts and engaging in mindful self-monitoring of the inner experience. 36 The inner experience of nursing also involves being mindful of the toll of care, which can erode mindful communication practices overtime. Nurses often begin careers with motivation to practice effective communication with patients and families, yet may experience compassion fatigue from too little sleep and not enough time to meet demanding clinical tasks. 37 As a result, disconnection is communicated through interactions with patients and families. Repetition of ineffective communication experiences, such as the non-patient–centered delivery of bad news, can lead to diminished mindful communication. There are specific communication stressors for nurses working in palliative care that can impact the ability to be mindful. For example, patients and families expect availability, access, competency, empathy, and patience from nurses. There are also specific factors that can affect the patient/family–nurse relationship. These factors include attachment, similarities, emotional balance, nurse mortality, and challenging spiritual beliefs. 15 All of these factors may contribute to burnout, which can lead to severe negative consequences, such as early retirement, unprofessional behavior, and an increased risk of medical errors. Consider the following example of Sylvia: After a decade of working as an oncology provider, Sylvia joined the palliative care team about 6 months ago. She is passionate about her work and is a strong team member. As usual, the team’s case load remains high and the past month has included high-intensity s, consisting of two to three family meetings, often involving lawyers, caring for a patient who was an oncology provider that worked with Sylvia, and a newly diagnosed Alzheimer’s patient who keeps referring to Sylvia as her daughter. Sylvia has been short-tempered and is neglecting her personal appearance. She has constant fatigue, feels overworked, and is questioning whether or not palliative care is the right clinical setting for her. She feels like her efforts go unnoticed by her colleagues. She is just ‘going through the motions’ at work, trying to find enthusiasm to return to work each day. She has witnessed so much suffering over the last 6 months and feels like she is ‘failing’ as a health care provider. Sylvia may be experiencing burnout. Burnout can be described as an adverse psychological state characterized by emotional exhaustion, depersonalization, cynicism, and a low perception of personal accomplishment. 38 , 39 Predictors of burnout among health care providers who work in palliative care include: working over 50 hours per week, working on weekends, less experience, isolation from peers, lack of confidence in regards to communication skills, time constraints that hamper successful communication, communicating bad news, addressing pain/suffering/death, working in smaller organizations, being under 50 years old, tensions between non-specialists and palliative care specialists, and regulatory issues. 38 – 40 Burnout also has detrimental effects on personal physical and emotional health, as well as relationships. 39 It has been suggested that increased burnout among oncology providers is associated with feelings of not being trained properly in cancer communication skills and having a desire to change communication with patients. 40 , 41 Table 4 summarizes indicators of stress at work that signify diminished ability to be mindful, which can result in poor quality of care, reduced patient trust and satisfaction, malpractice lawsuits, poor decision making, lower productivity, and emotional detachment from patients. 41 – 46 Indicators of Stress at Work | ∘ Withdrawing from patients/colleagues | | ∘ Ignoring or delaying patient/family requests | | ∘ Quick emotional responses to others | | ∘ Overreactions to colleagues | | ∘ Calling in sick to avoid feelings | | ∘ Keeping busy with work, ignoring emotions |
To prevent burnout, it is crucial for oncology nurses to create opportunities for self-care. For example, nurses should create ways to share difficult patient-family situations with colleagues. This can be done by seeking advice, confirming action, and sharing emotions. An activity that can be extremely helpful is journaling, which can aid in reflection. Journaling allows for the processing of emotions and feelings about events, and can aid in making meaning of situations. 47 Nurses can journal with other team members after the loss of a patient and share their writing with each other. They may also write a letter to a patient/family or to a colleague. 15 Self-care is critical for nurses because neglecting self-care may not only have detrimental personal effects, but may also be detrimental for their patients/families and colleagues. Relating involves being aware of the patient’s/family member’s understanding of the disease and its probable course and being willing to meet patients and families where they are in accepting the change brought by serious illness. In relating to patient and family, nurses should recognize that medical information such as prognosis and treatment option may need to be repeated numerous times to help patient and family reach awareness and understanding. Relating to the patient and family involves being aware of the multiple goals that can exist when talking about uncertainty and learning what hope means to the patient. Multiple goals exist because task and relational communication impact how our words are received and interpreted. Simply, task communication imparts the content of the message, whereas relational communication includes the nonverbal components of the interaction. This communication approach is predicated upon the axiom that every message (verbal or nonverbal) conveys both content (verbal message) and relationship (nonverbal communication). 48 Multiple goals can exist through the direct (verbal) and indirect (nonverbal) actions of words. For example, the way a patient or family members says “I’m worried” can reveal multiple concerns depending upon how it is said alongside nonverbal cues. Nonverbal communication can convey why they are worried, what they are worried about, how relationships influence worry, and whether or not they feel comfortable expressing worry to provider. It is essential for oncology nurses to learn how multiple goals are present for patient and family. Relating to patient/family involves building trust and establishing a relationship. Trust depends on the interpersonal and technical competence of the health care provider 49 and is gained by patient’s perceived emotional support, ability to share personal feelings, whether or not multiple discussions have taken place, and collaboration with family. 50 It is established over time, not just in one visit, 49 and includes understanding patient/family preferences, values, and priorities. Encouraging patients to ask questions and actively participate in their care is one way to elicit preferences. 51 Question prompt list is a communication tool that can facilitate difficult discussions and stimulate questions so that the clinician can understand the patient’s most important concerns. 51 – 54 A coaching intervention using the question prompt list in breast cancer survivors prompted questions regarding symptoms and recurrence and resulted in improved breast cancer self-efficacy. 53 An intervention with gynecologic cancer survivors included reflection and symptom sheets to facilitate communication during the nurse telephone coaching sessions. 54 Sessions focused on assessing challenges, symptom education, and problem-solving strategies. The intervention group scored higher on quality-of-life and physical well-being subscales compared with the usual care group. 54 Relating to patient/family also involves exploring feelings of uncertainty that cause worry. Nurses can help patients manage uncertainty by framing information in terms of what is known and unknown and acknowledging that some uncertainty in unavoidable. 37 The ability to speak to nurses between follow-up visits can provide reassurance regarding the meaning of symptoms and may decrease anxiety. 55 Peer support groups and lay navigators are resources that can provide emotional and tangible support. 56 Cancer survivors who express ongoing anxiety, uncertainty, and fear of recurrence may benefit from cognitive-behavioral and cognitive-existential therapies, mindfulness-based strategies, and coaching and communication interventions. 57 , 58 Dean and Street 59 describe a three-stage model for clinicians to help patients navigate emotional distress and difficult feelings: a) recognition; b) exploration; and c) therapeutic action. Recognizing distress requires cognitive and communication strategies. Rapport building, listening, asking about patient concerns, and avoiding interruptions are strategies to help nurses recognize emotional concerns. 59 In the exploration phase, nurses can validate and normalize emotions using open-ended questions and empathic phrases. Even if the nurse is uncertain how to respond, listening and demonstrating caring behaviors can be therapeutic. In the therapeutic action phase, nurses can provide clear information about symptoms and follow-up care, and referrals to assist survivors in managing uncertainty. 59 Brief screening tools to assess distress and symptoms should be integrated with electronic medical records. For example, PROMIS instruments can be used to assess anxiety, depression, and quality of life and can help to identify psychosocial concerns. 57 , 58 Consider the following case: Mrs Rogers recently completed treatment for stage III ovarian cancer and returns for her initial follow-up visit. Nurse Carol J. sits next to Mrs Rogers and asks if she has any questions or concerns she’d like to discuss during the visit. Mrs Rogers responds “I’m really not sure about what symptoms I should report or be concerned about. I’m also feeling anxious waiting for my CA-125 test result.” The nurse mentions that the transition to follow-up care can be stressful for many women and asked Mrs Rogers to tell her more about her concerns. Looking at the floor, Mrs Rogers explains: “I can’t stop thinking about the possibility that my cancer may come back. My husband gets upset if I try to talk with him about it.” The nurse responds “It must be difficult for you and your husband to deal with everything you have gone through in the past several months. Tell me about how he has helped you during your care and treatment. Do you think he is worried about the cancer returning?” The nurse quietly listens as Mrs Rogers shares about her relationship with her husband. The nurse provides education about common physical and emotional symptoms that survivors experience, suggesting that Mrs Rogers share these with her husband. The nurse reassures her that she will be available by phone if questions arise. She also mentions some support services that other women have found helpful and asks Mrs Rogers her thoughts on these options. The nurse ggests that she invite her husband to participate in the discussion with the oncologist arding surveillance and follow-up care. In this case study, the nurse uses communication strategies based on principles from the Dean and Street 59 and COMFORT models. She asks about and actively listens to Mrs Rogers’ concerns (Recognition). The nurse uses an open-ended clarifying question and acknowledges how difficult this must be. The nurse discusses options and seeks the patient’s preference for possible support services (Exploration). The nurse provides education regarding symptoms to reduce uncertainty; reassurance that she will be available; and identifies possible resources (Therapeutic action). Using the COMFORT principle of R-relating, the nurse encourages Mrs Rogers to discuss her concerns to further explore her feelings. She recognizes that Mrs Rogers’ worry about her cancer returning is connected to a lack of communication about cancer with her husband. Moreover, Mrs Rogers is looking at the ground when she makes this statement (nonverbal cue), revealing that this is also a difficult topic for her to discuss with the nurse. To further explore how Mrs Roger’s relationship with her husband influences her anxiety, she asks Mrs Rogers to recall how her husband has participated in her care and to imagine how he must be feeling. Addressing the partners’ uncertainty and concerns will promote well-being because the partner’s and survivor’s adjustment are interdependent. 60 Fostering healing relationships is a key communication task to help facilitate trust and relate to patient and family. Finally, the nurse builds trust by emphasizing that she is available by phone if questions arise. A major component of palliative care is whole-patient assessment that includes the impact of the patient’s illness on quality of life. Quality communication skills are essential to cancer nursing, enabling nurses to learn the patient’s story, address patient and family health literacy needs, discuss patient uncertainty and emotional distress, and be mindful of the need for self-care. Engaging in difficult or sensitive conversations requires trust, compassion, and self-awareness. 37 Palliative care communication training for oncology nurses is needed, especially given their vital role in cancer care. The COMFORT Communication model offers a nursing curriculum for teaching palliative care communication. AcknowledgmentsResearch reported in this publication was partially supported by the National Cancer Institute of the National Institutes of Health under award number R25CA174627. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health. Publisher's Disclaimer: This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final citable form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain. Contributor InformationElaine Wittenberg, Department of Communication Studies, California State University, Los Angeles, CA. Anne Reb, City of Hope Comprehensive Cancer Center, Duarte, CA. Elisa Kanter, Chapman University, Department of Communication, Orange, CA. Two Communication Rules in My Family Essay- To find inspiration for your paper and overcome writer’s block
- As a source of information (ensure proper referencing)
- As a template for you assignment
Family communication is important in fostering intimacy and accumulating resources. They also help in raising children as independent people capable of interacting with other human systems. The family communication rules are guidelines that govern what is to be expected of all communication in the family, what is allowed and what is prohibited under given circumstances. The rules are closely knit into the family culture and are transferred to newer generations by the senior members of the family. The rules dictate the emotional interdependence among family members and therefore family members directly affect each other emotionally, as well in their thoughts, feelings and actions (Le Poire, 2005). In my family, there is a non-written rule that young members of the family should not question the elder members. The rule further implied that the young should always execute orders or requests by the older members of the family without seeking to know why they have been specifically chosen to perform those tasks. This rule has been very significant in shaping the relationships among the members of my family. They were formulated mainly in order to govern the child to parent and parent to child communication and prevent incidents of children talking back to their parents when it is not desirable. As long as the communication rules have been observed, children have always been quiet when they are in the sight of their parents unless spoken to. The effects of this rule include; the relationship among brothers and sisters is not very mutual. The elder children dominate the communication with the younger children. The rules have also made it impossible for the young in the family to air their grievances to parents since it is expected that they feel aggrieved because of their own mistake of failing to listen or act as commanded by their elder brothers or sisters. The rule has therefore been a major source of fearful respect to elders. Even among adult members of the family the rule has made dispute resolution in favour of the much older members unless the situation is very clear that they are on the wrong. The rule has elevated the oldest member of the family to be the position of head of family since because of their age, their decisions are unquestionable. Apart from elders, the rule also places wives under their husbands in the age hierarchy. When it comes to family business, important decisions are taken by the head of the family with or without consultations with other members. As a result, success of the family majorly becomes dependent on the wisdom of the head of the family. Positive impacts of the rule have been that the family relations has been tight and there has always been general agreements on the direction taken by the family as siblings have no reason to debate among themselves on who is right. The rule has also checked on family rivalry. Another family rule is that bad or sensitive news cannot be told to children. This was informed by the need not to disrupt children’s upbringing by informing them about events that might be too big for them to handle emotionally. The rule has created the effect of ignorance of basic meanings in life, and has become an obstacle for children who want to learn about their family history and traditions. For example, in my family children cannot be informed of death of a family member including their parents and instead they are given excuses to explain the disappearance. While the rule serves to insulate children from emotional baggage, it also becomes a source of contention when children grow up and discover that important facts that could have shaped their lives had been hidden from them. A lot of disagreements and breakups have happened in my family because of the non-disclosure rule. To sum up, communication serves as vehicle that family members use to develop and maintain intimate relations (Vangelisti, 2004). Rules that govern this communication in the family are responsible for how well the communication serves to hold the family together and lead it to prosperity. The rules also significantly affect individual’s view of each other among the family. Le Poire, B. A. (2005). Family communication: nurturing and control in a changing world. Southern Oaks, CA: Sage Publications. Vangelisti, A. L. (2004). Handbook of family communication. Mahwah, NJ: Lawrence Erlbaum Associates Inc Publishers. - Good Parent-Children Relationship
- Concept and Treatment of the Alzheimer Disorder
- Denver and Abu Dhabi Airports: Baggage-Handling System
- AeroShield Market Research
- Taylor Swift & Bon Iver’s Exile (Indie Folk Song)
- Instruction Manual: How to Apply Kinesio Tape®
- Ethics in the Healthcare Delivery
- Medical Ethics: Arguments for Medical Dishonesty
- Alcoholism Disease or Self Will
- Classification of Water-Related Diseases
- Chicago (A-D)
- Chicago (N-B)
IvyPanda. (2018, August 21). Two Communication Rules in My Family. https://ivypanda.com/essays/two-communication-rules-in-my-family/ "Two Communication Rules in My Family." IvyPanda , 21 Aug. 2018, ivypanda.com/essays/two-communication-rules-in-my-family/. IvyPanda . (2018) 'Two Communication Rules in My Family'. 21 August. IvyPanda . 2018. "Two Communication Rules in My Family." August 21, 2018. https://ivypanda.com/essays/two-communication-rules-in-my-family/. 1. IvyPanda . "Two Communication Rules in My Family." August 21, 2018. https://ivypanda.com/essays/two-communication-rules-in-my-family/. Bibliography IvyPanda . "Two Communication Rules in My Family." August 21, 2018. https://ivypanda.com/essays/two-communication-rules-in-my-family/.  How parents can promote positive sibling relationships Postdoctoral Research Fellow, Department of Psychology, University of Calgary  Professor, Canada Research Chair in Determinants of Child Development, Owerko Centre at the Alberta Children’s Hospital Research Institute, University of Calgary Disclosure statementMarissa Nivison receives funding from the Social Sciences and Humanities Research Council of Canada. Sheri Madigan receives funding from the Social Sciences and Humanities Research Council, the Canadian Institutes of Health Research, the Alberta Children's Hospital Foundation, an anonymous donor, and the Canada Research Chairs program. University of Calgary provides funding as a founding partner of The Conversation CA. University of Calgary provides funding as a member of The Conversation CA-FR. View all partners Sibling relationships are some of the longest-lasting relationships we have in our lives . Half of Canadians and around 80 per cent of people worldwide have at least one sibling. Sibling relationships are unique from all other relationships because siblings often grow up together and share family history. Biological siblings even share genetics. In childhood, children spend more time with their siblings than anyone else, including their parents . A longitudinal study found that the quality of sibling relationships in young adulthood was one of the strongest predictors of well-being at age 65 . Sibling relationships change as we grow. In early adulthood, maintaining the sibling relationship becomes a matter of choice, although most sibling relationships last a lifetime . In childhood, parents have important roles to play setting the stage for life-long positive sibling relationships. As developmental and clinical psychologists, we recognize the profound impact siblings can have on development, especially having personally experienced the benefits, and sometimes the frustrations, within our own sibling relationships.  Sibling relationships and child developmentNot only is the sibling relationship unique, but it also serves an important role in a child’s development. Children with siblings tend to develop better relationships with their peers, engage in more creative play and have higher empathy and a better understanding of others’ thoughts and feelings . They often develop social skills much earlier than children without siblings, which helps them form friendships when they start school . Some studies have shown that positive sibling relationships also serve as a protective factor during difficult times, like high levels of life stress and marital conflict between parents . It is not surprising that siblings can have a large impact on an individual’s development. For example, children may adjust their personalities to avoid conflict and competition with their sibling . Additionally, just knowing they have a sibling can positively affect a child . Sibling conflicts, rivalryWhen we are kids, sibling relationships can be full of rivalry. In adolescence, sibling relationships tend to drift as we explore new relationships with peers and our own identity. It is probably no surprise that a major topic in research on sibling relationships is conflict. Sibling conflict is quite common and, to some extent, can actually be good for children’s development . The sibling relationship offers a unique context for children to resolve conflict because, unlike friendships, the sibling relationship cannot just end after a quarrel. Through navigating conflict with siblings, children can learn valuable skills such as understanding others’ perspectives, developing empathy, improving listening skills, setting boundaries and standing up for their own self interests.  However, there is a fine line between small disagreements and conflict being the main feature of the sibling relationship. It is normal for siblings to feel rivalry and competition, but when this becomes the defining feature of the relationship, it can create a negative environment. Specifically, children can become jealous and start to resent their sibling when they feel the need to compete for their parents’ attention and approval . How parents can navigate sibling conflictAlthough most parents say they don’t play favourites among siblings, up to 85 per cent of children believe their parents had a favourite. One of the biggest predictors of sibling conflict is differential treatment by parents — including perceived differences in parenting. This means that even if a parent believes they are treating all children equally, a child often feels they are being treated differently . For example, if both children are running through the house on separate occasions and one child receives a time out while the other is not allowed to go to a friend’s birthday party, the second child may perceive this as unfair, and naturally it creates tension in the sibling relationship. Parents should strive to be as fair as possible in their parenting by ensuring consistent consequences for similar misbehaviours among siblings. Another key factor is for parents to recognize the individual strengths of each child and avoid unhealthy competition between siblings. For example, if one child does well in math, and the other does well in science, recognize their individual abilities and accomplishments and avoid comparing one sibling’s strength with the other’s weakness. Promoting positive sibling relationshipsThere are science-backed ways parents can promote positive sibling relationships. Encourage positive engagement : Choose activities and interests that all siblings can enjoy together. Identify what’s going well: Recognize when siblings support, co-operate and help each other. Engage in shared experiences : Highlight each sibling’s unique strengths during activities that require teamwork. Regulate emotions : Help children identify and process their emotions during difficult times. Facilitate social and emotional understanding : Teach children about how to share their own feelings and understand and respect feelings of siblings. Manage undesirable behaviours : Address negative behaviours like bossiness towards siblings. Help children learn to consider the actions of their siblings, without assuming these actions are directed at them : It is important for children to understand that accidents happen and their siblings often do not have malicious intent toward them. For example, a parent might see a sibling accidentally knock over the toy tower. Manage conflict : Parents can mediate conflict between children to help resolve situations fairly. Examine parental differential treatment : Talk with children about instances when they feel they are being treated unfairly. Ask them to explain why they think something is “not fair” and discuss it together. By implementing these strategies, parents can help build strong, positive and supporting relationships between siblings, which can support their well-being throughout their lifetimes. - Child development
- Sibling rivalry
- Starting school
- Parent-child relationships
- Family relationships
 Service Delivery Consultant Newsletter and Deputy Social Media Producer College Director and Principal | Curtin College Head of School: Engineering, Computer and Mathematical Sciences Educational DesignerThere is less communication between family members today than in the past. Do you agree or disagree?Unauthorized use and/or duplication of this material without express and written permission from this site’s author and/or owner is strictly prohibited. Excerpts and links may be used, provided that full and clear credit is given to Writing9 with appropriate and specific direction to the original content. IELTS says that you should write a minimum of 250 words in writing task 2. If you go under word count you will lose marks in task response. A very long essay will not give you a higher band score. Aim for between 260 to 290 words in writing task 2. This will ensure a concise essay and will be realistic in terms of time management. You have only 40 minutes to write the essay and you need around 10 minutes of planning time, so you will not be able to write a long essay in 30 minutes. Discover more tips in The Ultimate Guide to Get a Target Band Score of 7+ » — a book that's free for 🚀 Premium users. - Check your IELTS essay »
- Find essays with the same topic
- View collections of IELTS Writing Samples
- Show IELTS Writing Task 2 Topics
In some countries, more and more people are becoming interested in finding out about the history of the house or building they live in. What are the reasons for this? How can people research this? Give reasons for your answer and include any relevant examples from your own knowledge or experience.Some people think that advertisements aimed at children should be banned. to what extent do you agree or disagree, prevention is better than cure. out of a country’s health budget, a large proportion should be diverted from treatment to spending on health education and preventive measure. to what extent do you agree or disagree, your neighbours have recently written to you to complain about the noise from your house flat. write a letter to your neighbour's. in your letter explain the reasons for the noise apologies describe what action you will take write at least 150 words., children at secondary school are often taken on visits to museums,zoos and concerts and sometimes even to other countries.what do you think the advantages and disadvantages of such visits are.  |







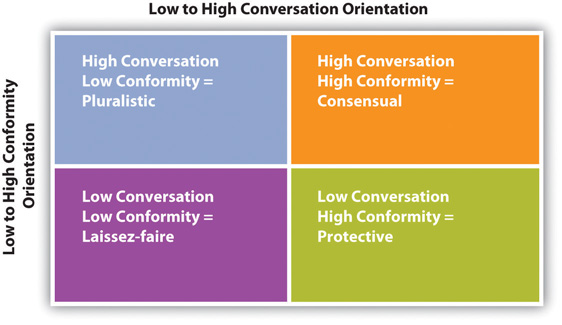


















IMAGES
VIDEO
COMMENTS
According to Graham, "In order for effective communication to take place within families, individual family members must be open and honest with on another" (1996, p. 24). Trust creates strong relationships among family members. Family Communication: Essay on My Family's Survival: As narrated by my mother
Communication between my family and me is based on the following special and unique principles. Our relationship is based on mutual interaction and cooperation, verbal and nonverbal methods of transmitting information, and dynamic interaction (Pace). Primarily, the connections between members of my family and me are directly conditioned by ...
Summary. Through the years, the concept of family has been studied by family therapists, psychology scholars, and sociologists with a diverse theoretical framework, such as family communication patterns (FCP) theory, dyadic power theory, conflict, and family systems theory. Among these theories, there are two main commonalities throughout its ...
Family relationships offer a unique source of emotional support. Within the familial circle, individuals find comfort, understanding, and empathy. Family members provide a safe haven where vulnerabilities can be shared without judgment. This support creates a sense of security and belonging that nurtures emotional well-being and encourages open ...
Nurturing family members entails providing basic care and support, both emotional and financial. Socializing family members refers to teaching young children how to speak, read, and practice social skills. Transactional definitions of family focus on communication and subjective feelings of connection.
This introductory essay attempts to accomplish the following: (1) discuss the importance of talk regarding death; (2) highlight the formative role of family interactions on the death and dying process; and (3) outline the articles in this special issue. Scholars contributing to this special issue on "Family Communication at the End of Life ...
Summary. Families shape individuals throughout their lives, and family communication is the foundation of family life and functioning. It is through communication that families are defined and members learn how to organize meanings. When individuals come together to form family relationships, they create a system that is larger and more complex ...
Pathways Linking Family Relationships to Well-Being. A life course perspective draws attention to the importance of linked lives, or interdependence within relationships, across the life course (Elder, Johnson, & Crosnoe, 2003).Family members are linked in important ways through each stage of life, and these relationships are an important source of social connection and social influence for ...
Be available: Make time in everyone's busy schedule to stop and talk about things. Even 10 minutes a day without distractions for you and your child to talk can make a big difference in forming good communication habits. Turn off the television or radio. Give your undivided attention to your child. Sit down and look at your child while you talk.
Abstract. Each stage of the human life course is characterised by a distinctive pattern of social relations. We study how the intensity and importance of the closest social contacts vary across the life course, using a large database of mobile communication from a European country. We first determine the most likely social relationship type ...
Family Relationship, Childhood Delinquency, Criminality. In regard to the relationship between the effect of various factors involved in a child's upbringing and the likelihood of becoming a criminal during adulthood, varied findings were made. Modality of Family Faith and Meanings and Relationships in Family Life.
Family communication patterns. Koerner and Fitzpatrick (Citation 2006) family communication patterns theory (FCP) suggests family communication schemata are defined by conversation and conformity orientations; as such, FCP provides a useful framework for understanding whether individuals disclose health information.Conversation orientation refers to how freely family members express ideas ...
Communication is found to be the most important factor for cohesion in families and sustainability of family wealth. Statistics show that more than 70% of families are unsuccessful at multi-generational wealth transfer and further, that 65% of the time this failure is attributed to lack of communication and trust within the family.*. The ...
You communicate with members of the family not just with your words but using language and behavior. If you use negative methods to communicate or avoid communicating at all, this can make matters worse through adulthood and even affect who we become as adults. Poor family communication can include yelling, holding grudges, keeping secrets ...
His research suggests that problems communicating with our loved ones and friends come from several different factors. First, most people seriously overestimate their ability to communicate effectively. Keysar's studies suggest that nearly 50% of the time when we think we are understood, we are actually wrong.
Communication is the basic building block of our relationships. It is through communication that we convey our thoughts, feelings, and connection to one another. Developing good communication skills is critical for successful relationships, whether parent, child, spouse, or sibling relationship. We all have had experiences where (1) we have ...
The objective of this study is to examine interpersonal communication and spoken skills. This work will examine communication skills using the theories of Pragmatic Perspective, Psychological Perspective, Social Constructionist, and social responsibility theory. Trenholm (2008) states that communication "is very important to everyone.
Based on the facts I furnished above, I strongly believe the communication gap between the family members is increased compared to the past decade. Submitted by tahsin291287 on Mon Apr 05 2021. ... A great argument essay structure may be divided to four paragraphs, in which comprises of four sentences (excluding the conclusion paragraph, which ...
Communication between nurse, patient, and family members involves more than just providing information. It includes discussing a range of topics, encouraging the sharing of feelings and fears about the illness, treatment, and prognosis, and helping patients and family members find a sense of control and a search for meaning and life purpose. 1 Nurses with strong communication skills have been ...
Get a custom essay on Two Communication Rules in My Family. The rules are closely knit into the family culture and are transferred to newer generations by the senior members of the family. The rules dictate the emotional interdependence among family members and therefore family members directly affect each other emotionally, as well in their ...
In this modern contemporary era, where technology has played a crucial role in the development of methods where people can easily communicate, commute and get the information at their door-steps. It is observed that the interaction among family members has been drastically reduced compared to the olden days | Band: 8
time. with their family which,accounts for less communication between family. For instance. ,the survey conducted at a university showed that because of less. time. spent between the families they less interaction between family members. In conclusion,due to the introduction of electronic gadgets and the modern ,era people become less ...
Strong, positive and supporting relationships between siblings can support people's well-being throughout their lifetimes, and parenting approaches matter.
A very long essay will not give you a higher band score. Aim for between 260 to 290 words in writing task 2. This will ensure a concise essay and will be realistic in terms of time management. You have only 40 minutes to write the essay and you need around 10 minutes of planning time, so you will not be able to write a long essay in 30 minutes.
PNSB Palau Fellowship Award Recipients Discuss Studying abroad and internships | August 7, 2024 | EPFM Studio