- Resources Home 🏠
- Try SciSpace Copilot
- Search research papers
- Add Copilot Extension
- Try AI Detector
- Try Paraphraser
- Try Citation Generator
- April Papers
- June Papers
- July Papers


The Craft of Writing a Strong Hypothesis

Table of Contents
Writing a hypothesis is one of the essential elements of a scientific research paper. It needs to be to the point, clearly communicating what your research is trying to accomplish. A blurry, drawn-out, or complexly-structured hypothesis can confuse your readers. Or worse, the editor and peer reviewers.
A captivating hypothesis is not too intricate. This blog will take you through the process so that, by the end of it, you have a better idea of how to convey your research paper's intent in just one sentence.
What is a Hypothesis?
The first step in your scientific endeavor, a hypothesis, is a strong, concise statement that forms the basis of your research. It is not the same as a thesis statement , which is a brief summary of your research paper .
The sole purpose of a hypothesis is to predict your paper's findings, data, and conclusion. It comes from a place of curiosity and intuition . When you write a hypothesis, you're essentially making an educated guess based on scientific prejudices and evidence, which is further proven or disproven through the scientific method.
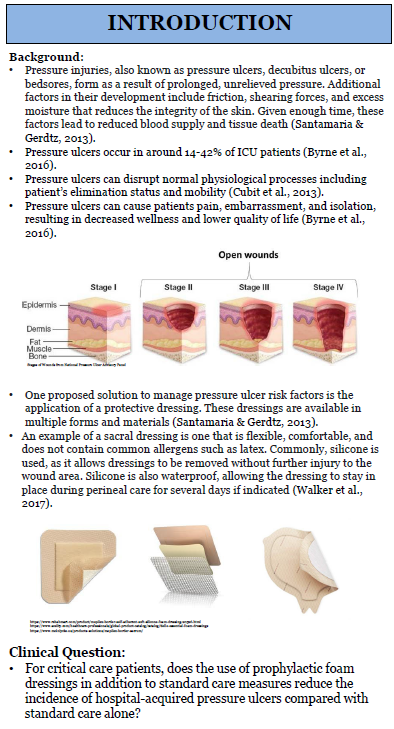
The reason for undertaking research is to observe a specific phenomenon. A hypothesis, therefore, lays out what the said phenomenon is. And it does so through two variables, an independent and dependent variable.
The independent variable is the cause behind the observation, while the dependent variable is the effect of the cause. A good example of this is “mixing red and blue forms purple.” In this hypothesis, mixing red and blue is the independent variable as you're combining the two colors at your own will. The formation of purple is the dependent variable as, in this case, it is conditional to the independent variable.
Different Types of Hypotheses

Types of hypotheses
Some would stand by the notion that there are only two types of hypotheses: a Null hypothesis and an Alternative hypothesis. While that may have some truth to it, it would be better to fully distinguish the most common forms as these terms come up so often, which might leave you out of context.
Apart from Null and Alternative, there are Complex, Simple, Directional, Non-Directional, Statistical, and Associative and casual hypotheses. They don't necessarily have to be exclusive, as one hypothesis can tick many boxes, but knowing the distinctions between them will make it easier for you to construct your own.
1. Null hypothesis
A null hypothesis proposes no relationship between two variables. Denoted by H 0 , it is a negative statement like “Attending physiotherapy sessions does not affect athletes' on-field performance.” Here, the author claims physiotherapy sessions have no effect on on-field performances. Even if there is, it's only a coincidence.
2. Alternative hypothesis
Considered to be the opposite of a null hypothesis, an alternative hypothesis is donated as H1 or Ha. It explicitly states that the dependent variable affects the independent variable. A good alternative hypothesis example is “Attending physiotherapy sessions improves athletes' on-field performance.” or “Water evaporates at 100 °C. ” The alternative hypothesis further branches into directional and non-directional.
- Directional hypothesis: A hypothesis that states the result would be either positive or negative is called directional hypothesis. It accompanies H1 with either the ‘<' or ‘>' sign.
- Non-directional hypothesis: A non-directional hypothesis only claims an effect on the dependent variable. It does not clarify whether the result would be positive or negative. The sign for a non-directional hypothesis is ‘≠.'
3. Simple hypothesis
A simple hypothesis is a statement made to reflect the relation between exactly two variables. One independent and one dependent. Consider the example, “Smoking is a prominent cause of lung cancer." The dependent variable, lung cancer, is dependent on the independent variable, smoking.
4. Complex hypothesis
In contrast to a simple hypothesis, a complex hypothesis implies the relationship between multiple independent and dependent variables. For instance, “Individuals who eat more fruits tend to have higher immunity, lesser cholesterol, and high metabolism.” The independent variable is eating more fruits, while the dependent variables are higher immunity, lesser cholesterol, and high metabolism.
5. Associative and casual hypothesis
Associative and casual hypotheses don't exhibit how many variables there will be. They define the relationship between the variables. In an associative hypothesis, changing any one variable, dependent or independent, affects others. In a casual hypothesis, the independent variable directly affects the dependent.
6. Empirical hypothesis
Also referred to as the working hypothesis, an empirical hypothesis claims a theory's validation via experiments and observation. This way, the statement appears justifiable and different from a wild guess.
Say, the hypothesis is “Women who take iron tablets face a lesser risk of anemia than those who take vitamin B12.” This is an example of an empirical hypothesis where the researcher the statement after assessing a group of women who take iron tablets and charting the findings.
7. Statistical hypothesis
The point of a statistical hypothesis is to test an already existing hypothesis by studying a population sample. Hypothesis like “44% of the Indian population belong in the age group of 22-27.” leverage evidence to prove or disprove a particular statement.
Characteristics of a Good Hypothesis
Writing a hypothesis is essential as it can make or break your research for you. That includes your chances of getting published in a journal. So when you're designing one, keep an eye out for these pointers:
- A research hypothesis has to be simple yet clear to look justifiable enough.
- It has to be testable — your research would be rendered pointless if too far-fetched into reality or limited by technology.
- It has to be precise about the results —what you are trying to do and achieve through it should come out in your hypothesis.
- A research hypothesis should be self-explanatory, leaving no doubt in the reader's mind.
- If you are developing a relational hypothesis, you need to include the variables and establish an appropriate relationship among them.
- A hypothesis must keep and reflect the scope for further investigations and experiments.
Separating a Hypothesis from a Prediction
Outside of academia, hypothesis and prediction are often used interchangeably. In research writing, this is not only confusing but also incorrect. And although a hypothesis and prediction are guesses at their core, there are many differences between them.
A hypothesis is an educated guess or even a testable prediction validated through research. It aims to analyze the gathered evidence and facts to define a relationship between variables and put forth a logical explanation behind the nature of events.
Predictions are assumptions or expected outcomes made without any backing evidence. They are more fictionally inclined regardless of where they originate from.
For this reason, a hypothesis holds much more weight than a prediction. It sticks to the scientific method rather than pure guesswork. "Planets revolve around the Sun." is an example of a hypothesis as it is previous knowledge and observed trends. Additionally, we can test it through the scientific method.
Whereas "COVID-19 will be eradicated by 2030." is a prediction. Even though it results from past trends, we can't prove or disprove it. So, the only way this gets validated is to wait and watch if COVID-19 cases end by 2030.
Finally, How to Write a Hypothesis

Quick tips on writing a hypothesis
1. Be clear about your research question
A hypothesis should instantly address the research question or the problem statement. To do so, you need to ask a question. Understand the constraints of your undertaken research topic and then formulate a simple and topic-centric problem. Only after that can you develop a hypothesis and further test for evidence.
2. Carry out a recce
Once you have your research's foundation laid out, it would be best to conduct preliminary research. Go through previous theories, academic papers, data, and experiments before you start curating your research hypothesis. It will give you an idea of your hypothesis's viability or originality.
Making use of references from relevant research papers helps draft a good research hypothesis. SciSpace Discover offers a repository of over 270 million research papers to browse through and gain a deeper understanding of related studies on a particular topic. Additionally, you can use SciSpace Copilot , your AI research assistant, for reading any lengthy research paper and getting a more summarized context of it. A hypothesis can be formed after evaluating many such summarized research papers. Copilot also offers explanations for theories and equations, explains paper in simplified version, allows you to highlight any text in the paper or clip math equations and tables and provides a deeper, clear understanding of what is being said. This can improve the hypothesis by helping you identify potential research gaps.
3. Create a 3-dimensional hypothesis
Variables are an essential part of any reasonable hypothesis. So, identify your independent and dependent variable(s) and form a correlation between them. The ideal way to do this is to write the hypothetical assumption in the ‘if-then' form. If you use this form, make sure that you state the predefined relationship between the variables.
In another way, you can choose to present your hypothesis as a comparison between two variables. Here, you must specify the difference you expect to observe in the results.
4. Write the first draft
Now that everything is in place, it's time to write your hypothesis. For starters, create the first draft. In this version, write what you expect to find from your research.
Clearly separate your independent and dependent variables and the link between them. Don't fixate on syntax at this stage. The goal is to ensure your hypothesis addresses the issue.
5. Proof your hypothesis
After preparing the first draft of your hypothesis, you need to inspect it thoroughly. It should tick all the boxes, like being concise, straightforward, relevant, and accurate. Your final hypothesis has to be well-structured as well.
Research projects are an exciting and crucial part of being a scholar. And once you have your research question, you need a great hypothesis to begin conducting research. Thus, knowing how to write a hypothesis is very important.
Now that you have a firmer grasp on what a good hypothesis constitutes, the different kinds there are, and what process to follow, you will find it much easier to write your hypothesis, which ultimately helps your research.
Now it's easier than ever to streamline your research workflow with SciSpace Discover . Its integrated, comprehensive end-to-end platform for research allows scholars to easily discover, write and publish their research and fosters collaboration.
It includes everything you need, including a repository of over 270 million research papers across disciplines, SEO-optimized summaries and public profiles to show your expertise and experience.
If you found these tips on writing a research hypothesis useful, head over to our blog on Statistical Hypothesis Testing to learn about the top researchers, papers, and institutions in this domain.
Frequently Asked Questions (FAQs)
1. what is the definition of hypothesis.
According to the Oxford dictionary, a hypothesis is defined as “An idea or explanation of something that is based on a few known facts, but that has not yet been proved to be true or correct”.
2. What is an example of hypothesis?
The hypothesis is a statement that proposes a relationship between two or more variables. An example: "If we increase the number of new users who join our platform by 25%, then we will see an increase in revenue."
3. What is an example of null hypothesis?
A null hypothesis is a statement that there is no relationship between two variables. The null hypothesis is written as H0. The null hypothesis states that there is no effect. For example, if you're studying whether or not a particular type of exercise increases strength, your null hypothesis will be "there is no difference in strength between people who exercise and people who don't."
4. What are the types of research?
• Fundamental research
• Applied research
• Qualitative research
• Quantitative research
• Mixed research
• Exploratory research
• Longitudinal research
• Cross-sectional research
• Field research
• Laboratory research
• Fixed research
• Flexible research
• Action research
• Policy research
• Classification research
• Comparative research
• Causal research
• Inductive research
• Deductive research
5. How to write a hypothesis?
• Your hypothesis should be able to predict the relationship and outcome.
• Avoid wordiness by keeping it simple and brief.
• Your hypothesis should contain observable and testable outcomes.
• Your hypothesis should be relevant to the research question.
6. What are the 2 types of hypothesis?
• Null hypotheses are used to test the claim that "there is no difference between two groups of data".
• Alternative hypotheses test the claim that "there is a difference between two data groups".
7. Difference between research question and research hypothesis?
A research question is a broad, open-ended question you will try to answer through your research. A hypothesis is a statement based on prior research or theory that you expect to be true due to your study. Example - Research question: What are the factors that influence the adoption of the new technology? Research hypothesis: There is a positive relationship between age, education and income level with the adoption of the new technology.
8. What is plural for hypothesis?
The plural of hypothesis is hypotheses. Here's an example of how it would be used in a statement, "Numerous well-considered hypotheses are presented in this part, and they are supported by tables and figures that are well-illustrated."
9. What is the red queen hypothesis?
The red queen hypothesis in evolutionary biology states that species must constantly evolve to avoid extinction because if they don't, they will be outcompeted by other species that are evolving. Leigh Van Valen first proposed it in 1973; since then, it has been tested and substantiated many times.
10. Who is known as the father of null hypothesis?
The father of the null hypothesis is Sir Ronald Fisher. He published a paper in 1925 that introduced the concept of null hypothesis testing, and he was also the first to use the term itself.
11. When to reject null hypothesis?
You need to find a significant difference between your two populations to reject the null hypothesis. You can determine that by running statistical tests such as an independent sample t-test or a dependent sample t-test. You should reject the null hypothesis if the p-value is less than 0.05.
You might also like

Consensus GPT vs. SciSpace GPT: Choose the Best GPT for Research

Literature Review and Theoretical Framework: Understanding the Differences

Types of Essays in Academic Writing - Quick Guide (2024)

What Is A Research (Scientific) Hypothesis? A plain-language explainer + examples
By: Derek Jansen (MBA) | Reviewed By: Dr Eunice Rautenbach | June 2020
If you’re new to the world of research, or it’s your first time writing a dissertation or thesis, you’re probably noticing that the words “research hypothesis” and “scientific hypothesis” are used quite a bit, and you’re wondering what they mean in a research context .
“Hypothesis” is one of those words that people use loosely, thinking they understand what it means. However, it has a very specific meaning within academic research. So, it’s important to understand the exact meaning before you start hypothesizing.
Research Hypothesis 101
- What is a hypothesis ?
- What is a research hypothesis (scientific hypothesis)?
- Requirements for a research hypothesis
- Definition of a research hypothesis
- The null hypothesis
What is a hypothesis?
Let’s start with the general definition of a hypothesis (not a research hypothesis or scientific hypothesis), according to the Cambridge Dictionary:
Hypothesis: an idea or explanation for something that is based on known facts but has not yet been proved.
In other words, it’s a statement that provides an explanation for why or how something works, based on facts (or some reasonable assumptions), but that has not yet been specifically tested . For example, a hypothesis might look something like this:
Hypothesis: sleep impacts academic performance.
This statement predicts that academic performance will be influenced by the amount and/or quality of sleep a student engages in – sounds reasonable, right? It’s based on reasonable assumptions , underpinned by what we currently know about sleep and health (from the existing literature). So, loosely speaking, we could call it a hypothesis, at least by the dictionary definition.
But that’s not good enough…
Unfortunately, that’s not quite sophisticated enough to describe a research hypothesis (also sometimes called a scientific hypothesis), and it wouldn’t be acceptable in a dissertation, thesis or research paper . In the world of academic research, a statement needs a few more criteria to constitute a true research hypothesis .
What is a research hypothesis?
A research hypothesis (also called a scientific hypothesis) is a statement about the expected outcome of a study (for example, a dissertation or thesis). To constitute a quality hypothesis, the statement needs to have three attributes – specificity , clarity and testability .
Let’s take a look at these more closely.
Need a helping hand?
Hypothesis Essential #1: Specificity & Clarity
A good research hypothesis needs to be extremely clear and articulate about both what’ s being assessed (who or what variables are involved ) and the expected outcome (for example, a difference between groups, a relationship between variables, etc.).
Let’s stick with our sleepy students example and look at how this statement could be more specific and clear.
Hypothesis: Students who sleep at least 8 hours per night will, on average, achieve higher grades in standardised tests than students who sleep less than 8 hours a night.
As you can see, the statement is very specific as it identifies the variables involved (sleep hours and test grades), the parties involved (two groups of students), as well as the predicted relationship type (a positive relationship). There’s no ambiguity or uncertainty about who or what is involved in the statement, and the expected outcome is clear.
Contrast that to the original hypothesis we looked at – “Sleep impacts academic performance” – and you can see the difference. “Sleep” and “academic performance” are both comparatively vague , and there’s no indication of what the expected relationship direction is (more sleep or less sleep). As you can see, specificity and clarity are key.

Hypothesis Essential #2: Testability (Provability)
A statement must be testable to qualify as a research hypothesis. In other words, there needs to be a way to prove (or disprove) the statement. If it’s not testable, it’s not a hypothesis – simple as that.
For example, consider the hypothesis we mentioned earlier:
Hypothesis: Students who sleep at least 8 hours per night will, on average, achieve higher grades in standardised tests than students who sleep less than 8 hours a night.
We could test this statement by undertaking a quantitative study involving two groups of students, one that gets 8 or more hours of sleep per night for a fixed period, and one that gets less. We could then compare the standardised test results for both groups to see if there’s a statistically significant difference.
Again, if you compare this to the original hypothesis we looked at – “Sleep impacts academic performance” – you can see that it would be quite difficult to test that statement, primarily because it isn’t specific enough. How much sleep? By who? What type of academic performance?
So, remember the mantra – if you can’t test it, it’s not a hypothesis 🙂

Defining A Research Hypothesis
You’re still with us? Great! Let’s recap and pin down a clear definition of a hypothesis.
A research hypothesis (or scientific hypothesis) is a statement about an expected relationship between variables, or explanation of an occurrence, that is clear, specific and testable.
So, when you write up hypotheses for your dissertation or thesis, make sure that they meet all these criteria. If you do, you’ll not only have rock-solid hypotheses but you’ll also ensure a clear focus for your entire research project.
What about the null hypothesis?
You may have also heard the terms null hypothesis , alternative hypothesis, or H-zero thrown around. At a simple level, the null hypothesis is the counter-proposal to the original hypothesis.
For example, if the hypothesis predicts that there is a relationship between two variables (for example, sleep and academic performance), the null hypothesis would predict that there is no relationship between those variables.
At a more technical level, the null hypothesis proposes that no statistical significance exists in a set of given observations and that any differences are due to chance alone.
And there you have it – hypotheses in a nutshell.
If you have any questions, be sure to leave a comment below and we’ll do our best to help you. If you need hands-on help developing and testing your hypotheses, consider our private coaching service , where we hold your hand through the research journey.

Psst... there’s more!
This post was based on one of our popular Research Bootcamps . If you're working on a research project, you'll definitely want to check this out ...
17 Comments
Very useful information. I benefit more from getting more information in this regard.
Very great insight,educative and informative. Please give meet deep critics on many research data of public international Law like human rights, environment, natural resources, law of the sea etc
In a book I read a distinction is made between null, research, and alternative hypothesis. As far as I understand, alternative and research hypotheses are the same. Can you please elaborate? Best Afshin
This is a self explanatory, easy going site. I will recommend this to my friends and colleagues.
Very good definition. How can I cite your definition in my thesis? Thank you. Is nul hypothesis compulsory in a research?
It’s a counter-proposal to be proven as a rejection
Please what is the difference between alternate hypothesis and research hypothesis?
It is a very good explanation. However, it limits hypotheses to statistically tasteable ideas. What about for qualitative researches or other researches that involve quantitative data that don’t need statistical tests?
In qualitative research, one typically uses propositions, not hypotheses.
could you please elaborate it more
I’ve benefited greatly from these notes, thank you.
This is very helpful
well articulated ideas are presented here, thank you for being reliable sources of information
Excellent. Thanks for being clear and sound about the research methodology and hypothesis (quantitative research)
I have only a simple question regarding the null hypothesis. – Is the null hypothesis (Ho) known as the reversible hypothesis of the alternative hypothesis (H1? – How to test it in academic research?
this is very important note help me much more
Hi” best wishes to you and your very nice blog”
Trackbacks/Pingbacks
- What Is Research Methodology? Simple Definition (With Examples) - Grad Coach - […] Contrasted to this, a quantitative methodology is typically used when the research aims and objectives are confirmatory in nature. For example,…
Submit a Comment Cancel reply
Your email address will not be published. Required fields are marked *
Save my name, email, and website in this browser for the next time I comment.
- Print Friendly
Have a language expert improve your writing
Run a free plagiarism check in 10 minutes, generate accurate citations for free.
- Knowledge Base
Methodology
- How to Write a Strong Hypothesis | Steps & Examples
How to Write a Strong Hypothesis | Steps & Examples
Published on May 6, 2022 by Shona McCombes . Revised on November 20, 2023.
A hypothesis is a statement that can be tested by scientific research. If you want to test a relationship between two or more variables, you need to write hypotheses before you start your experiment or data collection .
Example: Hypothesis
Daily apple consumption leads to fewer doctor’s visits.
Table of contents
What is a hypothesis, developing a hypothesis (with example), hypothesis examples, other interesting articles, frequently asked questions about writing hypotheses.
A hypothesis states your predictions about what your research will find. It is a tentative answer to your research question that has not yet been tested. For some research projects, you might have to write several hypotheses that address different aspects of your research question.
A hypothesis is not just a guess – it should be based on existing theories and knowledge. It also has to be testable, which means you can support or refute it through scientific research methods (such as experiments, observations and statistical analysis of data).
Variables in hypotheses
Hypotheses propose a relationship between two or more types of variables .
- An independent variable is something the researcher changes or controls.
- A dependent variable is something the researcher observes and measures.
If there are any control variables , extraneous variables , or confounding variables , be sure to jot those down as you go to minimize the chances that research bias will affect your results.
In this example, the independent variable is exposure to the sun – the assumed cause . The dependent variable is the level of happiness – the assumed effect .
Prevent plagiarism. Run a free check.
Step 1. ask a question.
Writing a hypothesis begins with a research question that you want to answer. The question should be focused, specific, and researchable within the constraints of your project.
Step 2. Do some preliminary research
Your initial answer to the question should be based on what is already known about the topic. Look for theories and previous studies to help you form educated assumptions about what your research will find.
At this stage, you might construct a conceptual framework to ensure that you’re embarking on a relevant topic . This can also help you identify which variables you will study and what you think the relationships are between them. Sometimes, you’ll have to operationalize more complex constructs.
Step 3. Formulate your hypothesis
Now you should have some idea of what you expect to find. Write your initial answer to the question in a clear, concise sentence.
4. Refine your hypothesis
You need to make sure your hypothesis is specific and testable. There are various ways of phrasing a hypothesis, but all the terms you use should have clear definitions, and the hypothesis should contain:
- The relevant variables
- The specific group being studied
- The predicted outcome of the experiment or analysis
5. Phrase your hypothesis in three ways
To identify the variables, you can write a simple prediction in if…then form. The first part of the sentence states the independent variable and the second part states the dependent variable.
In academic research, hypotheses are more commonly phrased in terms of correlations or effects, where you directly state the predicted relationship between variables.
If you are comparing two groups, the hypothesis can state what difference you expect to find between them.
6. Write a null hypothesis
If your research involves statistical hypothesis testing , you will also have to write a null hypothesis . The null hypothesis is the default position that there is no association between the variables. The null hypothesis is written as H 0 , while the alternative hypothesis is H 1 or H a .
- H 0 : The number of lectures attended by first-year students has no effect on their final exam scores.
- H 1 : The number of lectures attended by first-year students has a positive effect on their final exam scores.
| Research question | Hypothesis | Null hypothesis |
|---|---|---|
| What are the health benefits of eating an apple a day? | Increasing apple consumption in over-60s will result in decreasing frequency of doctor’s visits. | Increasing apple consumption in over-60s will have no effect on frequency of doctor’s visits. |
| Which airlines have the most delays? | Low-cost airlines are more likely to have delays than premium airlines. | Low-cost and premium airlines are equally likely to have delays. |
| Can flexible work arrangements improve job satisfaction? | Employees who have flexible working hours will report greater job satisfaction than employees who work fixed hours. | There is no relationship between working hour flexibility and job satisfaction. |
| How effective is high school sex education at reducing teen pregnancies? | Teenagers who received sex education lessons throughout high school will have lower rates of unplanned pregnancy teenagers who did not receive any sex education. | High school sex education has no effect on teen pregnancy rates. |
| What effect does daily use of social media have on the attention span of under-16s? | There is a negative between time spent on social media and attention span in under-16s. | There is no relationship between social media use and attention span in under-16s. |
If you want to know more about the research process , methodology , research bias , or statistics , make sure to check out some of our other articles with explanations and examples.
- Sampling methods
- Simple random sampling
- Stratified sampling
- Cluster sampling
- Likert scales
- Reproducibility
Statistics
- Null hypothesis
- Statistical power
- Probability distribution
- Effect size
- Poisson distribution
Research bias
- Optimism bias
- Cognitive bias
- Implicit bias
- Hawthorne effect
- Anchoring bias
- Explicit bias
Receive feedback on language, structure, and formatting
Professional editors proofread and edit your paper by focusing on:
- Academic style
- Vague sentences
- Style consistency
See an example

A hypothesis is not just a guess — it should be based on existing theories and knowledge. It also has to be testable, which means you can support or refute it through scientific research methods (such as experiments, observations and statistical analysis of data).
Null and alternative hypotheses are used in statistical hypothesis testing . The null hypothesis of a test always predicts no effect or no relationship between variables, while the alternative hypothesis states your research prediction of an effect or relationship.
Hypothesis testing is a formal procedure for investigating our ideas about the world using statistics. It is used by scientists to test specific predictions, called hypotheses , by calculating how likely it is that a pattern or relationship between variables could have arisen by chance.
Cite this Scribbr article
If you want to cite this source, you can copy and paste the citation or click the “Cite this Scribbr article” button to automatically add the citation to our free Citation Generator.
McCombes, S. (2023, November 20). How to Write a Strong Hypothesis | Steps & Examples. Scribbr. Retrieved August 12, 2024, from https://www.scribbr.com/methodology/hypothesis/
Is this article helpful?
Shona McCombes
Other students also liked, construct validity | definition, types, & examples, what is a conceptual framework | tips & examples, operationalization | a guide with examples, pros & cons, "i thought ai proofreading was useless but..".
I've been using Scribbr for years now and I know it's a service that won't disappoint. It does a good job spotting mistakes”

The First Step: Ask; Fundamentals of Evidence-Based Nursing Practice
In this module, we will learn about identifying the problem, start the “Ask” process with developing an answerable clinical question, and learn about purpose statements and hypotheses.
Content includes:
- Identifying the problem
- Determining the Population, Intervention, Comparison, and Outcome (PICO)
- Asking a Research/Clinical Question (Based on PICO)
Statements of Purpose
Objectives:
- Describe the process of developing a research/practice problem.
- Describe the components of a PICO.
- Identify different types of PICOs.
- Distinguish function and form of statements of purpose.
- Describe the function and characteristics of hypotheses.
Development of a Research/Practice Problem
Practice questions frequently arise from day-to-day problems that are encountered by providers (Dearholt & Dang, 2012). Often, these problems are very obvious. However, sometimes we need to back up and take a close look at the status quo to see underlying issues. The basis for any research project is indeed the underlying problem or issue. A good problem statement or paragraph is a declaration of what it is that is problematic or what it is that we do not know much about (a gap in knowledge) (Polit & Beck, 2018).
The process of defining the practice/clinical problem begins by seeking answers to clinical concerns. This is the first step in the EBP process: To ask . We start by asking some broad questions to help guide the process of developing our practice problem.
- Is there evidence that the current treatment works?
- Does the current practice help the patient?
- Why are we doing the current practice?
- Should we be doing the current practice this way?
- Is there a way to do this current practice more efficiently?
- Is there a more cost-effective method to do this practice?
Problem Statements:
For our EBP Project, we will need to ask these broad questions and then develop our problem that exists. This establishes the “background” of the issue we want to know more about.
For example, if we are choosing a clinical question based on wanting to know if adjunct music therapy helps decrease postoperative pain levels than just pharmaceuticals alone, we might consider the underlying problems of:
- Postoperative pain is not adequately managed in greater than 80% of patients in the US, although rates vary depending on such factors as type of surgery performed, analgesic/anesthetic intervention used, and time elapsed after surgery (Gan, 2017).
- Poorly controlled acute postoperative pain is associated with increased morbidity, functional and quality-of-life impairment, delayed recovery time, prolonged duration of opioid use, and higher health-care costs (Gan, 2017).
- Multimodal analgesic techniques are widely used but new evidence is disappointing (Rawal, 2016).
In the above examples, we are establishing that poorly managed postoperative pain is a problem. Thus, looking at evidence about adjunctive music therapy may help to address how we might manage pain more effectively. These are our problem statements. This would be our introduction section on the EBP poster. For the sake of our EBP poster, you do not need to list these on the poster references. A heads up: The sources used to help develop our research/clinical program should not be the same resources that we use to answer our upcoming clinical question. In essence, we will be conducting two literature reviews: One, to establish the underlying problem; and, two: To find published research that helps to answer our developed clinical question.
Here is the introduction to the article titled, “The relationships among pain, depression, and physical activity in patients with heart failure” (Haedtke et al, 2017). You can read that the underlying problem is multifocal: 67% of patient with heart failure (HF) experience pain, depression is a comorbidity that affects 22% to 42% of HF patients, and that little attention has been paid to this relationship in patients with HF. The researchers have established the need for further research and why further research is needed.

Here is another example of how the clinical problem is addressed in an EBP poster that wants to appraise existing evidence related to dressing choice for decubitus ulcers.
When trying to communicate clinical problems, there are two main sources (Titler et al, 1994, 2001):
- Problem-focused triggers : These are identified by staff during routine monitoring of quality, risk, adverse events, financial, or benchmarking data.
- Knowledge-focused triggers : There are identified through reading published evidence or learning new information at conferences or other professional meetings.
Sources of Evidence-Based Clinical Problems:
| Triggers | Sources of Evidence |
| Problem-focused |
|
| Knowledge-focused |
Most problem statements have the following components:
- Problem identification: What is wrong with the current situation or action?
- Background: What is the nature of the problem or the context of the situation? (this helps to establish the why)
- Scope of the problem: How many people are affected? Is this a small problem? Big problem? Potential to grow quickly to a large problem? Has been increasing/decreasing recently?
- Consequences of the problem: If we do nothing or leave as the status quo, what is the cost of not fixing the issue?
- Knowledge gaps: What information about the problem is lacking? We need to know what we do not know.
- Proposed solution: How will the information or evidence contribute to the solution of the problem?
If you are stumped on a topic, ask faculty, RNs at local facilities, colleagues, and key stakeholders at local facilities for some ideas! There is usually “something” that the nursing field is concerned about or has questions about.
Components of a PICO Question
After we have asked ourselves some background questions, we need to develop a foreground (focused) question. A thoughtful development of a well-structured foreground clinical/practice question is important because the question drives the strategies that you will use to search for the published evidence. The question needs to be very specific, non-ambiguous , and measurable in order to find the relevant evidence needed and also increased the likelihood that you will find what you are looking for.
In developing your clinical/practice question, there is a helpful format to utilize to establish the key component. This format includes the Patient/Population, Intervention/Influence/Exposure, Comparison, and Outcome (PICO) (Richardson, Wilson, Nishikawa, & Hayward, 1995).
Let’s dive into each component to better understand.
P atient, population, or problem: We want to describe the patient, the population, or the problem. Get specific. We will want to know exactly who we are wanting to know about. Consider age, gender, setting of the patient (e.g. postoperative), and/or symptoms.
I ntervention: The intervention is the action or, in other words, the treatment, process of care, education given, or assessment approaches. We will come back to this in more depth, but for now remember that the intervention is also called the “Independent Variable”.
C omparison: Here we are comparing with other interventions. A comparison can be standard of care that already exists, current practice, an opposite intervention/action, or a different intervention/action.
O utcome: What is that that we are looking at for a result or consequence of the intervention? The outcome needs to have a metric for actually measuring results. The outcome can include quality of life, patient satisfaction, cost impacts, or treatment results. The outcome is also called the “Dependent Variable”.
The PICO question is a critical aspect of the EBP project to guide the problem identification and create components that can be used to shape the literature search.

Let’s watch a nice YouTube video, “PICO: A Model for Evidence-Based Research”:
“PICO: A Model for Evidence Based Research” by Binghamton University Libraries. Licensed CCY BY .
Great! Okay, let’s move on and discuss the various types of PICOs.
Types of PICOs
Before we start developing our clinical question, let’s go over the various types of PICOs and the clinical question that can result from the components. There are various types of PICOs but we are concerned with the therapy/treatment/intervention format of PICO for our EBP posters.
Let’s take a look at the various types of PICOs:
| Type of Question | PICO Template |
| Therapy/Intervention/Treatment (We will use this type for our EBP Posters) | In _________ (Population), what is the effect of ___________ (Intervention) in comparison to ___________(Comparison) on __________ (Outcome)? Or Does _________ (Intervention) compared to __________ (Comparison) decrease/increase ______________ (Outcome) in ____________ (Population)?
|
| Diagnosis/Assessment | For _________ (Population), does __________ (Identifying tool/procedure) yield more accurate or more appropriate diagnostic/assessment information than __________ (Comparative tool/procedure) about __________ (Outcome)?
|
| Prognosis | For ______ (Population), does _______ (Exposure to disease or condition), relative to _______ (Comparative disease or condition) increase the risk of ________ (Outcome)?
|
| Etiology/Harm | Does (Influence, exposure, or characteristic) increase the risk of ________ (Outcome) compared to ________ (Comparative influence, exposure, or condition) in ________ (Population)?
|
| Description (Prevalence/Incidence) | These questions vary from the typical PICO in that explicit comparisons are not typical (except to compare population). In ______ (Population), how prevalent is ________ (Outcome)?
|
| Meaning or Process | Explicit comparisons are not typical in these types of questions. These are qualitative questions and are used to elicit narrative, subjective responses. What is it like for ________ (Population) to experience _________ (situation, condition, circumstance)?
|
The first step in developing a research or clinical practice question is developing your PICO. Well, we’ve done that above. You will select each component of your PICO and then turn that into your question. Making the EBP question as specific as possible really helps to identify specific terms and narrow the search, which will result in reducing the time it times searching for relevant evidence.
Once you have your pertinent clinical question, you will use the components to begin your search in published literature for articles that help to answer your question. In class, we will practice with various situations to develop PICOs and clinical questions.
Many articles have the researcher’s statement of purpose (sometimes referred to as “aim”, “goal”, or “objective”) for their research project. This helps to identify what the overarching direction of inquiry may be. You do not need a statement of purpose/aim/goal/objective for your EBP poster. However, knowing what a statement of purpose is will help you when appraising articles to help answer your clinical question.

The following statement of purpose was written as an aim. The population (P) was identified as patients with HF, the interventions (I) included physical activity/exercise, and the outcomes (O) included pain, depression, total activity time, and sitting time as correlated with the interventions.

In the articles above, the authors made it easy and included their statements of purpose within the abstract at the beginning of the article. Most articles do not feature this ease, and you will need to read the introduction or methodology section of the article to find the statement of purpose, much like within article 3.1.
In qualitative studies, the statement of purpose usually indicates the nature of the inquiry, the key concept, the key phenomenon, and the population.

Function and Characteristics of Hypotheses.
A hypothesis (plural: hypothes es ) is a statement of predicted outcome. Meaning, it is an educated and formulated guess as to how the intervention (independent variable – more on that soon!) impacts the outcome (dependent variable). It is not always a cause and effect. Sometimes there can be just a simple association or correlation. We will come back to that in a few modules.
In your PICO statement, you can think of the “I” as the independent variable and the “O” as the dependent variable . Variables will begin making more sense as we go. But for now, remember this:
Independent Variable (IV): This is a measure that can be manipulated by the researcher. Perhaps it is a medication, an educational program, or a survey. The independent variable enacts change (or not) onto the independent variable.
Dependent Variable (DV): This is the result of the independent variable. This is the variable that we utilize statistical analyses to measure. For instance, if we are intervening with a blood pressure medication (our IV), then our DV would be the measurement of the actual blood pressure.
Most of the time, a hypothesis results from a well-worded research question. Here is an example:
Research Question : “Does sexual abuse in childhood affect the development of irritable bowel syndrome in women?”
Research Hypothesis : Women (P) who were sexually abused in childhood (I) have a higher incidence of irritable bowel syndrome (O) than women who were not abused (C).
You may note in that hypothesis that there is a predicted direction of outcome. One thing leads to something.
But, why do we need a hypothesis? First, they help to promote critical thinking. Second, it gives the researcher a way to measure a relationship. Suppose we conducted a study guided only by a research question. Take the above question, for example. Without a hypothesis, the researcher is seemingly prepared to accept any result (Polit & Beck, 2021). The problem with that is that it is almost always possible to explain something superficially after the fact, even if the findings are inconclusive. A hypothesis reduces the possibility that spurious results will be misconstrued (Polit & Beck, 2021).

Not all research articles will list a hypothesis. This makes it more difficult to critically appraise the results. That is not to say that the results would be invalidated, but it should ignite a spirit of further inquiry as to if the results are valid.
Hypotheses (also called alternative hypothesis) can be stated as:
- Directional or nondirectional
- Simple or complex
- Research or Null
Simple hypothesis : Statement of causal (cause and effect) relationship – one independent variable (intervention) and one dependent variable (outcome).
Example : If you stay up late, then you feel tired the next day.
Complex hypothesis : Statement of causal (cause and effect) or associative (not causal) between two or more independent variables (interventions) and/or two or more dependent variables (outcomes).
Example : Higher the poverty, higher the illiteracy in society, higher will be the rate of crime (three variables – two independent variables and one dependent variable).
Directional hypothesis : Specifies not only the existence but also the expected direction of the relationship between the dependent (outcome) and the independent (intervention) variables. You will also see this called “One-tailed hypothesis”.
Example : Depression scores will decrease following a 6-week intervention.
Nondirectional hypothesis : Does not specify the direction of relationship between the variables. You will also see this called “Two-tailed hypothesis”.
Example : College students will perform differently from elementary school students on a memory task (without predicting which group of students will perform better).

Null hypothesis : The null hypothesis assumes that any kind of difference between the chosen characteristics that you see in a set of data is due to chance. Now, the null hypothesis is why the plain old hypothesis is also called alternative hypothesis. We don’t just assume that the hypothesis is true. So, it is considered an alternative to something just happening by chance (null).
Example : Let’s say our research question is, “Do teens use cell phones to access the internet more than adults?” – our null hypothesis could state: Age has no effect on how cell phones are used for internet access.

And then, further develop the problem and background through finding existing literature to help answer the following questions:
- Knowledge gaps: What information about the problem is lacking? We need to know what we do not know.
With the previous example of pain in the pediatric population, here is an example of an Introduction section from a past student poster:

- What was the research problem? Was the problem statement easy to locate and was it clearly stated? Did the problem statement build a coherent and persuasive argument for the new study?
- Does the problem have significance for nursing?
- Was there a good fit between the research problem and the paradigm (and tradition) within which the research was conducted?
- Did the report formally present a statement of purpose, research question, and/or hypotheses? Was this information communicated clearly and concisely, and was it placed in a logical and useful location?
- Were purpose statements or research questions worded appropriately (e.g., were key concepts/variables identified and the population specified?
- If there were no formal hypotheses, was their absence justified? Were statistical tests used in analyzing the data despite the absence of stated hypotheses?
- Were hypotheses (if any) properly worded—did they state a predicted relationship between two or more variables? Were they presented as research or as null hypotheses?
References & Attribution
“ Green check mark ” by rawpixel licensed CC0 .
“ Light bulb doodle ” by rawpixel licensed CC0 .
“ Magnifying glass ” by rawpixel licensed CC0
“ Orange flame ” by rawpixel licensed CC0 .
Chen, P., Nunez-Smith, M., Bernheim, S… (2010). Professional experiences of international medical graduates practicing primary care in the United States. Journal of General Internal Medicine, 25 (9), 947-53.
Dearholt, S.L., & Dang, D. (2012). Johns Hopkins nursing evidence-based practice: Model and guidelines (2nd Ed.). Indianapolis, IN: Sigma Theta Tau International.
Gan, T. (2017). Poorly controlled postoperative pain: Prevalence, consequences, and prevention. Journal of Pain Research, 10, 2287-2298.
Genc, A., Can, G., Aydiner, A. (2012). The efficiency of the acupressure in prevention of the chemotherapy-induced nausea and vomiting. Support Care Cancer, 21 , 253-261.
Haedtke, C., Smith, M., VanBuren, J., Kein, D., Turvey, C. (2017). The relationships among pain, depression, and physical activity in patients with heart failure. Journal of Cardiovascular Nursing, 32 (5), E21-E25.
Pankong, O., Pothiban, L., Sucamvang, K., Khampolsiri, T. (2018). A randomized controlled trial of enhancing positive aspects of caregiving in Thai dementia caregivers for dementia. Pacific Rim Internal Journal of Nursing Res, 22 (2), 131-143.
Polit, D. & Beck, C. (2021). Lippincott CoursePoint Enhanced for Polit’s Essentials of Nursing Research (10th ed.). Wolters Kluwer Health.
Rawal, N. (2016). Current issues in postoperative pain management. European Journal of Anaesthesiology, 33 , 160-171.
Richardson, W.W., Wilson, M.C., Nishikawa, J., & Hayward, R.S. (1995). The well-built clinical question: A key to evidence-based decisions. American College of Physicians, 123 (3), A12-A13.
Titler, M. G., Kleiber, C., Steelman, V.J. Rakel, B. A. Budreau, G., Everett,…Goode, C.J. (2001). The Iowa model of evidence-based practice to promote quality care. Critical Care Nursing Clinics of North America, 13 (4), 497-509.
Evidence-Based Practice & Research Methodologies Copyright © by Tracy Fawns is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License , except where otherwise noted.
Share This Book

The P value: What it really means
As nurses, we must administer nursing care based on the best available scientific evidence. But for many nurses, critical appraisal, the process used to determine the best available evidence, can seem intimidating. To make critical appraisal more approachable, let’s examine the P value and make sure we know what it is and what it isn’t.
Defining P value
The P value is the probability that the results of a study are caused by chance alone. To better understand this definition, consider the role of chance.
The concept of chance is illustrated with every flip of a coin. The true probability of obtaining heads in any single flip is 0.5, meaning that heads would come up in half of the flips and tails would come up in half of the flips. But if you were to flip a coin 10 times, you likely would not obtain heads five times and tails five times. You’d be more likely to see a seven-to-three split or a six-to-four split. Chance is responsible for this variation in results.
Just as chance plays a role in determining the flip of a coin, it plays a role in the sampling of a population for a scientific study. When subjects are selected, chance may produce an unequal distribution of a characteristic that can affect the outcome of the study. Statistical inquiry and the P value are designed to help us determine just how large a role chance plays in study results. We begin a study with the assumption that there will be no difference between the experimental and control groups. This assumption is called the null hypothesis. When the results of the study indicate that there is a difference, the P value helps us determine the likelihood that the difference is attributed to chance.
Competing hypotheses
In every study, researchers put forth two kinds of hypotheses: the research or alternative hypothesis and the null hypothesis. The research hypothesis reflects what the researchers hope to show—that there is a difference between the experimental group and the control group. The null hypothesis directly competes with the research hypothesis. It states that there is no difference between the experimental group and the control group.
It may seem logical that researchers would test the research hypothesis—that is, that they would test what they hope to prove. But the probability theory requires that they test the null hypothesis instead. To support the research hypothesis, the data must contradict the null hypothesis. By demonstrating a difference between the two groups, the data contradict the null hypothesis.
Testing the null hypothesis
Now that you know why we test the null hypothesis, let’s look at how we test the null hypothesis.
After formulating the null and research hypotheses, researchers decide on a test statistic they can use to determine whether to accept or reject the null hypothesis. They also propose a fixed-level P value. The fixed level P value is often set at .05 and serves as the value against which the test-generated P value must be compared. (See Why .05?)
A comparison of the two P values determines whether the null hypothesis is rejected or accepted. If the P value associated with the test statistic is less than the fixed-level P value, the null hypothesis is rejected because there’s a statistically significant difference between the two groups. If the P value associated with the test statistic is greater than the fixed-level P value, the null hypothesis is accepted because there’s no statistically significant difference between the groups.
The decision to use .05 as the threshold in testing the null hypothesis is completely arbitrary. The researchers credited with establishing this threshold warned against strictly adhering to it.
Remember that warning when appraising a study in which the test statistic is greater than .05. The savvy reader will consider other important measurements, including effect size, confidence intervals, and power analyses when deciding whether to accept or reject scientific findings that could influence nursing practice.
Real-world hypothesis testing
How does this play out in real life? Let’s assume that you and a nurse colleague are conducting a study to find out if patients who receive backrubs fall asleep faster than patients who do not receive backrubs.
1. State your null and research hypotheses
Your null hypothesis will be that there will be no difference in the average amount of time it takes patients in each group to fall asleep. Your research hypothesis will be that patients who receive backrubs fall asleep, on average, faster than those who do not receive backrubs. You will be testing the null hypothesis in hopes of supporting your research hypothesis.

2. Propose a fixed-level P value
Although you can choose any value as your fixed-level P value, you and your research colleague decide you’ll stay with the conventional .05. If you were testing a new medical product or a new drug, you would choose a much smaller P value (perhaps as small as .0001). That’s because you would want to be as sure as possible that any difference you see between groups is attributed to the new product or drug and not to chance. A fixed-level P value of .0001 would mean that the difference between the groups was attributed to chance only 1 time out of 10,000. For a study on backrubs, however, .05 seems appropriate.
3. Conduct hypothesis testing to calculate a probability value
You and your research colleague agree that a randomized controlled study will help you best achieve your research goals, and you design the process accordingly. After consenting to participate in the study, patients are randomized to one of two groups:
- the experimental group that receives the intervention—the backrub group
- the control group—the non-backrub group.
After several nights of measuring the number of minutes it takes each participant to fall asleep, you and your research colleague find that on average, the backrub group takes 19 minutes to fall asleep and the non-backrub group takes 24 minutes to fall asleep.
Now the question is: Would you have the same results if you conducted the study using two different groups of people? That is, what role did chance play in helping the backrub group fall asleep 5 minutes faster than the non-backrub group? To answer this, you and your colleague will use an independent samples t-test to calculate a probability value.
An independent samples t-test is a kind of hypothesis test that compares the mean values of two groups (backrub and non-backrub) on a given variable (time to fall asleep).
Hypothesis testing is really nothing more than testing the null hypothesis. In this case, the null hypothesis is that the amount of time needed to fall asleep is the same for the experimental group and the control group. The hypothesis test addresses this question: If there’s really no difference between the groups, what is the probability of observing a difference of 5 minutes or more, say 10 minutes or 15 minutes?
We can define the P value as the probability that the observed time difference resulted from chance. Some find it easier to understand the P value when they think of it in relationship to error. In this case, the P value is defined as the probability of committing a Type 1 error. (Type 1 error occurs when a true null hypothesis is incorrectly rejected.)
4. Compare and interpret the P value
Early on in your study, you and your colleague selected a fixed-level P value of .05, meaning that you were willing to accept that 5% of the time, your results might be caused by chance. Also, you used an independent samples t-test to arrive at a probability value that will help you determine the role chance played in obtaining your results. Let’s assume, for the sake of this example, that the probability value generated by the independent samples t-test is .01 (P = .01). Because this P value associated with the test statistic is less than the fixed-level statistic (.01 < .05), you can reject the null hypothesis. By doing so, you declare that there is a statistically significant difference between the experimental and control groups. (See Putting the P value in context.)
In effect, you’re saying that the chance of observing a difference of 5 minutes or more, when in fact there is no difference, is less than 5 in 100. If the P value associated with the test statistic would have been greater than .05, then you would accept the null hypothesis, which would mean that there is no statistically significant difference between the control and experimental groups. Accepting the null hypothesis would mean that a difference of 5 minutes or more between the two groups would occur more than 5 times in 100.
Putting the P value in context
Although the P value helps you interpret study results, keep in mind that many factors can influence the P value—and your decision to accept or reject the null hypothesis. These factors include the following:
- Insufficient power. The study may not have been designed appropriately to detect an effect of the independent variable on the dependent variable. Therefore, a change may have occurred without your knowing it, causing you to incorrectly reject your hypothesis.
- Unreliable measures. Instruments that don’t meet consistency or reliability standards may have been used to measure a particular phenomenon.
- Threats to internal validity. Various biases, such as selection of patients, regression, history, and testing bias, may unduly influence study outcomes.
A decision to accept or reject study findings should focus not only on P value but also on other metrics including the following:
- Confidence intervals (an estimated range of values with a high probability of including the true population value of a given parameter)
- Effect size (a value that measures the magnitude of a treatment effect)
Remember, P value tells you only whether a difference exists between groups. It doesn’t tell you the magnitude of the difference.
5. Communicate your findings
The final step in hypothesis testing is communicating your findings. When sharing research findings (hypotheses) in writing or discussion, understand that they are statements of relationships or differences in populations. Your findings are not proved or disproved. Scientific findings are always subject to change. But each study leads to better understanding and, ideally, better outcomes for patients.
Key concepts
The P value isn’t the only concept you need to understand to analyze research findings. But it is a very important one. And chances are that understanding the P value will make it easier to understand other key analytical concepts.
Selected references
Burns N, Grove S: The Practice of Nursing Research: Conduct, Critique, and Utilization. 5th ed. Philadelphia: WB Saunders; 2004.
Glaser DN: The controversy of significance testing: misconceptions and alternatives. Am J Crit Care. 1999;8(5):291-296.
Kenneth J. Rempher, PhD, RN, MBA, CCRN, APRN,BC, is Director, Professional Nursing Practice at Sinai Hospital of Baltimore (Md.). Kathleen Urquico, BSN, RN, is a Direct Care Nurse in the Rubin Institute of Advanced Orthopedics at Sinai Hospital of Baltimore.

NurseLine Newsletter
- First Name *
- Last Name *
- Hidden Referrer
*By submitting your e-mail, you are opting in to receiving information from Healthcom Media and Affiliates. The details, including your email address/mobile number, may be used to keep you informed about future products and services.
Test Your Knowledge
Recent posts.

Interpreting statistical significance in nursing research

Introduction to qualitative nursing research

Navigating statistics for successful project implementation

Nurse research and the institutional review board
Research 101: Descriptive statistics

Research 101: Forest plots

Understanding confidence intervals helps you make better clinical decisions

Differentiating statistical significance and clinical significance

Differentiating research, evidence-based practice, and quality improvement
Are you confident about confidence intervals?

Making sense of statistical power
- Subscribe to journal Subscribe
- Get new issue alerts Get alerts
Secondary Logo
Journal logo.
Colleague's E-mail is Invalid
Your message has been successfully sent to your colleague.
Save my selection
Hypothesis Testing
Yarandi , Hossein
HOSSEIN N. YARANDI teaches biostatistics and health economics at the University of Florida, Gainesville, Florida. He received his BS in economics and statistics from Tehran University and his MA in economics and PhD in econometrics from Indiana University, Bloomington, Indiana. He has taught statistics, macro and microeconomics, finite math, calculus, operations research, statistical methods in research, mathematical statistics with computer applications, multivariate statistics, design and analysis of experiment, and health economics at Indiana University-Purdue University at Indianapolis, State University of New York at Fredonia, and the University of Florida .
HYPOTHESIS TESTING IS the process of making a choice between two conflicting hypotheses. The null hypothesis, H 0 , is a statistical proposition stating that there is no significant difference between a hypothesized value of a population parameter and its value estimated from a sample drawn from that population. The alternative hypothesis, H 1 or H a , is a statistical proposition stating that there is a significant difference between a hypothesized value of a population parameter and its estimated value. When the null hypothesis is tested, a decision is either correct or incorrect. An incorrect decision can be made in two ways: We can reject the null hypothesis when it is true (Type I error) or we can fail to reject the null hypothesis when it is false (Type II error). The probability of making Type I and Type II errors is designated by α and β, respectively. The smallest observed significance level for which the null hypothesis would be rejected is referred to as the p -value. The p -value only has meaning as a measure of confidence when the decision is to reject the null hypothesis. It has no meaning when the decision is that the null hypothesis is true.
Full Text Access for Subscribers:
Individual subscribers.

Institutional Users
Not a subscriber.
You can read the full text of this article if you:
- + Favorites
- View in Gallery
An official website of the United States government
The .gov means it’s official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you’re on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- My Bibliography
- Collections
- Citation manager
Save citation to file
Email citation, add to collections.
- Create a new collection
- Add to an existing collection
Add to My Bibliography
Your saved search, create a file for external citation management software, your rss feed.
- Search in PubMed
- Search in NLM Catalog
- Add to Search
Trends in hypothesis testing and related variables in nursing research: a retrospective exploratory study
Affiliation.
- 1 Northern Illinois University, DeKalb, IL, USA. [email protected]
- PMID: 21560925
- DOI: 10.7748/nr2011.04.18.3.38.c8462
Aim: To compare the inclusion and the influences of selected variables on hypothesis testing during the 1980s and 1990s.
Background: In spite of the emphasis on conducting inquiry consistent with the tenets of logical positivism, there have been no studies investigating the frequency and patterns of hypothesis testing in nursing research
Data sources: The sample was obtained from the journal Nursing Research which was the research journal with the highest circulation during the study period under study. All quantitative studies published during the two decades including briefs and historical studies were included in the analyses
Review methods: A retrospective design was used to select the sample. Five years from the 1980s and 1990s each were randomly selected from the journal, Nursing Research. Of the 582 studies, 517 met inclusion criteria.
Discussion: Findings suggest that there has been a decline in the use of hypothesis testing in the last decades of the 20th century. Further research is needed to identify the factors that influence the conduction of research with hypothesis testing.
Conclusion: Hypothesis testing in nursing research showed a steady decline from the 1980s to 1990s. Research purposes of explanation, and prediction/ control increased the likelihood of hypothesis testing.
Implications for practice: Hypothesis testing strengthens the quality of the quantitative studies, increases the generality of findings and provides dependable knowledge. This is particularly true for quantitative studies that aim to explore, explain and predict/control phenomena and/or test theories. The findings also have implications for doctoral programmes, research preparation of nurse-investigators, and theory testing.
PubMed Disclaimer
Similar articles
- A descriptive study of research published in scientific nursing journals from 1985 to 2010. Yarcheski A, Mahon NE, Yarcheski TJ. Yarcheski A, et al. Int J Nurs Stud. 2012 Sep;49(9):1112-21. doi: 10.1016/j.ijnurstu.2012.03.004. Epub 2012 Apr 6. Int J Nurs Stud. 2012. PMID: 22483613
- Nursing research in Italy. Zanotti R. Zanotti R. Annu Rev Nurs Res. 1999;17:295-322. Annu Rev Nurs Res. 1999. PMID: 10418662 Review.
- The research evidence published in high impact nursing journals between 2000 and 2006: a quantitative content analysis. Mantzoukas S. Mantzoukas S. Int J Nurs Stud. 2009 Apr;46(4):479-89. doi: 10.1016/j.ijnurstu.2008.12.016. Epub 2009 Feb 1. Int J Nurs Stud. 2009. PMID: 19187934
- Incorporating multiculturalism into oncology nursing research: the last decade. Phillips J, Weekes D. Phillips J, et al. Oncol Nurs Forum. 2002 Jun;29(5):807-16. doi: 10.1188/02.ONF.807-816. Oncol Nurs Forum. 2002. PMID: 12058155 Review.
- [Analysis of research papers published in the Journal of the Korean Academy of Nursing-focused on research trends, intervention studies, and level of evidence in the research]. Shin HS, Hyun MS, Ku MO, Cho MO, Kim SY, Jeong JS, Jeong GH, Seomoon GA, Son YJ. Shin HS, et al. J Korean Acad Nurs. 2010 Feb;40(1):139-49. doi: 10.4040/jkan.2010.40.1.139. J Korean Acad Nurs. 2010. PMID: 20220290 Korean.
- Search in MeSH
LinkOut - more resources
Full text sources.
- Ovid Technologies, Inc.
Miscellaneous
- NCI CPTAC Assay Portal
- Citation Manager
NCBI Literature Resources
MeSH PMC Bookshelf Disclaimer
The PubMed wordmark and PubMed logo are registered trademarks of the U.S. Department of Health and Human Services (HHS). Unauthorized use of these marks is strictly prohibited.
Nursing Research
- First Online: 24 January 2019
Cite this chapter

- Lars-Petter Jelsness-Jørgensen 3 , 4
1675 Accesses
Nurses play an increasingly active role in clinical research in IBD. By reviewing existing literature on the topic, this chapter provides a brief overview of some main concepts related to research in nursing. In addition, the chapter provides some general advice in relation to implementing evidence-based practice, as well as carrying out independent research.
This is a preview of subscription content, log in via an institution to check access.
Access this chapter
Subscribe and save.
- Get 10 units per month
- Download Article/Chapter or eBook
- 1 Unit = 1 Article or 1 Chapter
- Cancel anytime
- Available as PDF
- Read on any device
- Instant download
- Own it forever
- Available as EPUB and PDF
- Durable hardcover edition
- Dispatched in 3 to 5 business days
- Free shipping worldwide - see info
Tax calculation will be finalised at checkout
Purchases are for personal use only
Institutional subscriptions
Similar content being viewed by others

Ethics and Integrity in Nursing Research

Case Study in Nursing
Abrandt Dahlgren M, Higgs J, Richardson B (2004) Developing practice knowledge for health professionals. Butterworth-Heinemann, Edinburgh
Google Scholar
Bager P, Befrits R, Wikman O, Lindgren S, Moum B, Hjortswang H et al (2011) The prevalence of anemia and iron deficiency in IBD outpatients in Scandinavia. Scand J Gastroenterol 46(3):304–309
Article Google Scholar
Bager P, Befrits R, Wikman O, Lindgren S, Moum B, Hjortswang H et al (2012) Fatigue in out-patients with inflammatory bowel disease is common and multifactorial. Aliment Pharmacol Ther 35(1):133–141
Article CAS Google Scholar
Coenen S, Weyts E, Vermeire S, Ferrante M, Noman M, Ballet V et al (2017) Effects of introduction of an inflammatory bowel disease nurse position on the quality of delivered care. Eur J Gastroenterol Hepatol 29(6):646–650
Czuber-Dochan W, Ream E, Norton C (2013a) Review article: description and management of fatigue in inflammatory bowel disease. Aliment Pharmacol Ther 37(5):505–516
Czuber-Dochan W, Dibley LB, Terry H, Ream E, Norton C (2013b) The experience of fatigue in people with inflammatory bowel disease: an exploratory study. J Adv Nurs 69(9):1987–1999
Czuber-Dochan W, Norton C, Bassett P, Berliner S, Bredin F, Darvell M et al (2014a) Development and psychometric testing of inflammatory bowel disease fatigue (IBD-F) patient self-assessment scale. J Crohns Colitis 8(11):1398–1406
Czuber-Dochan W, Norton C, Bredin F, Darvell M, Nathan I, Terry H (2014b) Healthcare professionals’ perceptions of fatigue experienced by people with IBD. J Crohns Colitis 8(8):835–844
Dibley L, Norton C (2013) Experiences of fecal incontinence in people with inflammatory bowel disease: self-reported experiences among a community sample. Inflamm Bowel Dis 19(7):1450–1462
Dibley L, Bager P, Czuber-Dochan W, Farrell D, Jelsness-Jorgensen LP, Kemp K et al (2017) Identification of research priorities for inflammatory bowel disease nursing in Europe: a Nurses-European Crohn’s and Colitis Organisation Delphi Survey. J Crohns Colitis 11(3):353–359
PubMed Google Scholar
Dicenso A, Bayley L, Haynes RB (2009) Accessing pre-appraised evidence: fine-tuning the 5S model into a 6S model. Evid Based Nurs 12(4):99–101
Domecq JP, Prutsky G, Elraiyah T, Wang Z, Nabhan M, Shippee N et al (2014) Patient engagement in research: a systematic review. BMC Health Serv Res 14:89
Elwyn G, Edwards A, Thompson R (2016) Shared decision making in health care: achieving evidence-based patient choice, 3rd edn. Oxford University Press, Oxford
Book Google Scholar
Jaghult S, Larson J, Wredling R, Kapraali M (2007) A multiprofessional education programme for patients with inflammatory bowel disease: a randomized controlled trial. Scand J Gastroenterol 42(12):1452–1459
Jaghult S, Saboonchi F, Johansson UB, Wredling R, Kapraali M (2011) Identifying predictors of low health-related quality of life among patients with inflammatory bowel disease: comparison between Crohn’s disease and ulcerative colitis with disease duration. J Clin Nurs 20(11–12):1578–1587
Jelsness-Jorgensen LP (2015) Does a 3-week critical research appraisal course affect how students perceive their appraisal skills and the relevance of research for clinical practice? A repeated cross-sectional survey. Nurse Educ Today 35(1):e1–e5
Jelsness-Jorgensen LP, Moum B, Bernklev T (2011a) Worries and concerns among inflammatory bowel disease patients followed prospectively over one year. Gastroenterol Res Pract 2011:492034
Jelsness-Jorgensen LP, Bernklev T, Henriksen M, Torp R, Moum BA (2011b) Chronic fatigue is associated with impaired health-related quality of life in inflammatory bowel disease. Aliment Pharmacol Ther 33(1):106–114
Jelsness-Jorgensen LP, Bernklev T, Henriksen M, Torp R, Moum BA (2011c) Chronic fatigue is more prevalent in patients with inflammatory bowel disease than in healthy controls. Inflamm Bowel Dis 17(7):1564–1572
Jelsness-Jorgensen LP, Bernklev T, Henriksen M, Torp R, Moum B (2012a) Chronic fatigue is associated with increased disease-related worries and concerns in inflammatory bowel disease. World J Gastroenterol 18(5):445–452
Jelsness-Jorgensen LP, Bernklev T, Henriksen M, Torp R, Moum B (2012b) Is patient reported outcome (PRO) affected by different follow-up regimens in inflammatory bowel disease (IBD)? A one year prospective, longitudinal comparison of nurse-led versus conventional follow-up. J Crohns Colitis 6(9):887–894
Lindberg A, Ebbeskog B, Karlen P, Oxelmark L (2013) Inflammatory bowel disease professionals’ attitudes to and experiences of complementary and alternative medicine. BMC Complement Altern Med 13:349
Melnyk BM, Fineout-Overholt E, Stillwell SB, Williamson KM (2010) Evidence-based practice: step by step: the seven steps of evidence-based practice. Am J Nurs 110(1):51–53
Norton C, Dibley L (2013) Help-seeking for fecal incontinence in people with inflammatory bowel disease. J Wound Ostomy Continence Nurs 40(6):631–638; quiz E1-2
O’Connor M, Bager P, Duncan J, Gaarenstroom J, Younge L, Detre P et al (2013) N-ECCO consensus statements on the European nursing roles in caring for patients with Crohn’s disease or ulcerative colitis. J Crohns Colitis 7(9):744–764
Opheim R, Fagermoen MS, Bernklev T, Jelsness-Jorgensen LP, Moum B (2014a) Fatigue interference with daily living among patients with inflammatory bowel disease. Qual Life Res 23(2):707–717
Opheim R, Fagermoen MS, Jelsness-Jorgensen LP, Bernklev T, Moum B (2014b) Sense of coherence in patients with inflammatory bowel disease. Gastroenterol Res Pract 2014:989038
Oxelmark L, Magnusson A, Lofberg R, Hilleras P (2007) Group-based intervention program in inflammatory bowel disease patients: effects on quality of life. Inflamm Bowel Dis 13(2):182–190
Oxelmark L, Lindberg A, Lofberg R, Sternby B, Eriksson A, Almer S et al (2016) Use of complementary and alternative medicine in Swedish patients with inflammatory bowel disease: a controlled study. Eur J Gastroenterol Hepatol 28(11):1320–1328
Polit DF, Beck CT (2017) Nursing research: generating and assessing evidence for nursing practice, 10th edn. Wolters Kluwer, Philadelphia
Sackett DL, Rosenberg WM (1995) The need for evidence-based medicine. J R Soc Med 88(11):620–624
CAS PubMed PubMed Central Google Scholar
Sackett DL, Rosenberg WM, Gray JA, Haynes RB, Richardson WS (1996) Evidence based medicine: what it is and what it isn’t. BMJ (Clinical Research Ed) 312(7023):71–72
Williams B, Perillo S, Brown T (2015) What are the factors of organisational culture in health care settings that act as barriers to the implementation of evidence-based practice? A scoping review. Nurse Educ Today 35(2):e34–e41
Woodward S, Dibley L, Coombes S, Bellamy A, Clark C, Czuber-Dochan W et al (2016) Identifying disease-specific distress in patients with inflammatory bowel disease. Br J Nurs (Mark Allen Publishing) 25(12):649–660
Younge L, Norton C (2007) Contribution of specialist nurses in managing patients with IBD. Br J Nurs (Mark Allen Publishing) 16(4):208–212
Download references
Author information
Authors and affiliations.
Østfold University College, Department of Health Science, Halden, Norway
Lars-Petter Jelsness-Jørgensen
Østfold Hospital Trust, Department of Gastroenterology, Grålum, Norway
You can also search for this author in PubMed Google Scholar
Corresponding author
Correspondence to Lars-Petter Jelsness-Jørgensen .
Editor information
Editors and affiliations.
DRK Kliniken Berlin Westend, Department of Gastroenterology, Berlin, Germany
Andreas Sturm
Gastroenterology Level 5, John Radcliffe Hospital, Oxford, UK
Lydia White
Rights and permissions
Reprints and permissions
Copyright information
© 2019 Springer Nature Switzerland AG
About this chapter
Jelsness-Jørgensen, LP. (2019). Nursing Research. In: Sturm, A., White, L. (eds) Inflammatory Bowel Disease Nursing Manual. Springer, Cham. https://doi.org/10.1007/978-3-319-75022-4_42
Download citation
DOI : https://doi.org/10.1007/978-3-319-75022-4_42
Published : 24 January 2019
Publisher Name : Springer, Cham
Print ISBN : 978-3-319-75021-7
Online ISBN : 978-3-319-75022-4
eBook Packages : Medicine Medicine (R0)
Share this chapter
Anyone you share the following link with will be able to read this content:
Sorry, a shareable link is not currently available for this article.
Provided by the Springer Nature SharedIt content-sharing initiative
- Publish with us
Policies and ethics
- Find a journal
- Track your research
International Journal of Nursing Science Practice and Research
- Other Journals
- For Readers
- For Authors
- For Librarians
- Announcements
- JournalsPub Home Page
- Editorial Board
- Publication Ethics & Malpractice Statement
Hypothesis Types and Research
Dennis F. Polit. Nursing Research: Generating and Assessing Evidence for Nursing Practice, 9th edition. New Delhi: Lippincott Williams and Wilkins; 2012, 58–93p.
Nursing Research society of India, Nursing research and statistics, 1st edition. India: Pearson Publication; 2013, 48–51p.
Polit DF, Hungler BP. Nursing Research Principles and Methods. Philadelphia: Lippincott; 1999.
- There are currently no refbacks.
Warning: The NCBI web site requires JavaScript to function. more...
An official website of the United States government
The .gov means it's official. Federal government websites often end in .gov or .mil. Before sharing sensitive information, make sure you're on a federal government site.
The site is secure. The https:// ensures that you are connecting to the official website and that any information you provide is encrypted and transmitted securely.
- Publications
- Account settings
- Browse Titles
NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health.
Institute of Medicine (US) Division of Health Care Services. Nursing and Nursing Education: Public Policies and Private Actions. Washington (DC): National Academies Press (US); 1983.

Nursing and Nursing Education: Public Policies and Private Actions.
- Hardcopy Version at National Academies Press
Appendix 8 Nursing Research: Definitions and Directions
In order to provide further insight into the need for, philosophy, and scope of nursing research this appendix presents a position statement issued by the Commission on Nursing Research of the American Nurses' Association. It is quoted here in its entirety: 1
Recent years have seen a growing awareness among the public that valuable resources are finite and their use must be carefully considered. In this context, increasing attention is being given to the relative cost of various strategies for utilizing health care resources to meet the present and emerging needs of the nation. Concurrently, nurses are assuming increased decision-making responsibility for the delivery of health care, and they can be expected to continue to assume greater responsibility in the future. Therefore, the timeliness and desirability of identifying directions for nursing research that should receive priority in funding and effort in the 1980s is apparent.
The priorities identified below were developed by the Commission on Nursing Research of the American Nurses' Association, a nine-member group of nurses actively engaged in research whose backgrounds represent considerable diversity in preparation and experience. The priorities represent the consensus of the commissioners, developed through a process of thoughtful discussion and careful deliberation with colleagues.
Accountability to the public for the humane use of knowledge in providing effective and high quality services is the hallmark of a profession. Thus, the preeminent goal of scientific inquiry by nurses is the ongoing development of knowledge for use in the practice of nursing; priorities are stated in that context. Other guiding considerations were the present and anticipated health problems of the population; a historic appreciation of the circumstances in which nursing action has been most beneficial; nursing's philosophical orientation, in which emphasis is on a synthesis of psychosocial and biomedical phenomena to the end of promoting health and effective functioning; and projections regarding the types of decisions nurses will be making in the last decades of the twentieth century. New, unanticipated problems will undoubtedly confront the health care resources of the country; yet it is clear that many of the problems of the future are already manifest today. New knowledge is essential to bring about effective solutions. Nursing research directed to clinical needs can contribute in a significant way to development of those solutions.
- Definition of Nursing Research
Nursing research develops knowledge about health and the promotion of health over the full lifespan, care of persons with health problems and disabilities, and nursing actions to enhance the ability of individuals to respond effectively to actual or potential health problems.
These foci of nursing research complement those of biomedical research, which is primarily concerned with causes and treatments of disease. Advancements in biomedical research have resulted in increased life expectancies, including life expectancies of those with serious injury and those with chronic or terminal disease. These biomedical advances have thus led to growth in the numbers of those who require nursing care to live with health problems, such as the frail elderly, the chronically ill, and the terminally ill.
Research conducted by nurses includes various types of studies in order to derive clinical interventions to assist those who require nursing care. The complexity of nursing research and its broad scope often require scientific underpinning from several disciplines. Hence, nursing research cuts across traditional research lines, and draws its methods from several fields.
- Directions for Research
Priority should be given to nursing research that would generate knowledge to guide practice in:
Promoting health, well-being, and competency for personal care among all age groups;
Preventing health problems throughout the life span that have the potential to reduce productivity and satisfaction;
Decreasing the negative impact of health problems on coping abilities, productivity, and life satisfaction of individuals and families;
Ensuring that the care needs of particularly vulnerable groups are met through appropriate strategies;
Designing and developing health care systems that are cost-effective in meeting the nursing needs of the population.
Examples of research consistent with these priorities include the following:
- Identification of determinants (personal and environmental, including social support networks) of wellness and health functioning in individuals and families, e.g. avoidance of abusive behaviors such as alcoholism and drug use, successful adaptation to chronic illness, and coping with the last days of life.
- Identification of phenomena that negatively influence the course of recovery and that may be alleviated by nursing practice, such as, for example, anorexia, diarrhea, sleep deprivation, deficiencies in nutrients, electrolyte imbalances, and infections.
- Development and testing of care strategies to do the following: Facilitate individuals' ability to adopt and maintain health enhancing behaviors (e.g. alterations in diet and exercise). Enhance patients' ability to manage acute and chronic illness in such a way as to minimize or eliminate the necessity of institutionalization and to maximize well-being. Reduce stressful responses associated with the medical management of patients (e.g. surgical procedures, intrusive examination procedures, or use of extensive monitoring devices). Provide more effective care to high-risk populations (e.g. maternal and child care service to vulnerable mothers and infants, family planning services to young teenagers, services designed to enhance self-care in the chronically ill and the very old). Enhance the care of clients culturally different from the majority (e.g. Black Americans, Mexican-Americans, Native Americans) and clients with special problems (e.g. teenagers, prisoners, and the mentally ill), and the underserved (the elderly, the poor, and the rural).
- Design and assessment, in terms of effectiveness and cost, of models for delivering nursing care strategies found to be effective in clinical studies.
All of the foregoing are directly related to the priority of developing the knowledge and information needed for improvement of the practice of nursing.
While priority should be given to this form of clinical research, there is no intent to discourage other forms of nursing research. These would include such investigations as those utilizing historical and philosophical modes of inquiry, and studies of manpower for nursing education, practice, and research, as well as studies of quality assurance for nursing and those for establishment of criterion measures for practice and education.
American Nurses' Association. Research priorities for the 1980s: Generating a scientific basis for nursing practice (Publication No. D-68). Kansas City, Mo.: American Nurses' Association, 1981.
- Cite this Page Institute of Medicine (US) Division of Health Care Services. Nursing and Nursing Education: Public Policies and Private Actions. Washington (DC): National Academies Press (US); 1983. Appendix 8, Nursing Research: Definitions and Directions.
- PDF version of this title (2.7M)
In this Page
Recent activity.
- Nursing Research: Definitions and Directions - Nursing and Nursing Education Nursing Research: Definitions and Directions - Nursing and Nursing Education
Your browsing activity is empty.
Activity recording is turned off.
Turn recording back on
Connect with NLM
National Library of Medicine 8600 Rockville Pike Bethesda, MD 20894
Web Policies FOIA HHS Vulnerability Disclosure
Help Accessibility Careers
Free Al Office Suite with PDF Editor
Edit Word, Excel, and PPT for FREE.
Read, edit, and convert PDFs with the powerful PDF toolkit.
Microsoft-like interface, easy to use.
Windows • MacOS • Linux • iOS • Android
- Articles of Word
How to Write a Hypothesis? [Tips with Examples]
Click here if you have ever found yourself in the position of having to wrestle with the development of a hypothesis for your research paper. As an expert writer, I have seen that this is where most students begin to sweat. It is a potpourri of theory and practice, hence rather intimidating. But not to worry because I have got your back. This guide is a pool of tips and tricks for writing a hypothesis to set the stage for compelling research.
What is a Hypothesis?
A hypothesis is a tentative statement, usually in the form of an educated guess, that provides a probable explanation for something either a phenomenon or a relationship between variables. This will, therefore, form a basis for conducting experiments and research studies, hence laying down the course of your investigation and mainly laying the ground for your conclusion.
A good hypothesis should be:
Specific and clear
Testable and falsifiable
Based upon existing knowledge
Logically consistent
Types of Hypothesis
There are different kinds of hypotheses used in research, all of which serve different purposes depending on the nature of the study. Here are eight common types:
1. The null hypothesis (H0): asserts that there is no effect or relationship between variables. This forms a baseline for comparison. Example: "There is no difference in test scores for students who study music and for those who do not."
2. Alternative Hypothesis (H1): The hypothesis that postulates some effect or relationship between variables; it is, therefore, the opposite of the null hypothesis. For instance, "Students who study with music have different test scores than those who study in silence."
3. Simple Hypothesis: The hypothesis that states a relationship between two variables: one independent and one dependent. For example, "More sunlight increases plant growth."
4. Complex Hypothesis: This hypothesis involves the relationship of more than one variable. For example, "More sunlight and water increase plant growth."
5. Directional Hypothesis: The hypothesis which specifies the direction of the effect between variables. For instance, "Students who study with music will have higher test scores than students who study in silence."
6. Non-Directional Hypothesis: This is a hypothesis used where the relationship is indicated, but the direction is not specified. For example, "There is a difference in test scores between students who study with music and those who study in silence."
7. Associative Hypothesis: This hypothesis merely states that the change in one variable is associated with a change in another. It does not indicate cause and effect. For example: "There is a relationship between study habits and academic performance."
8. Causal Hypothesis: This hypothesis states that one variable causes a change in another. For example: "Increased study time results in higher test scores."
Understanding such types of hypotheses will help in the selection of the correct hypothesis for your research and in making your analysis clear and effective.
5 Steps to Write a Good Hypothesis [With Examples]
An excellent hypothesis provides a backbone to any scientific research. Leave some help behind in writing one? Follow this easy guide:
Step 1: Ask a Question
First, you must understand what your research question is. Suppose you want to carry out an experiment on plant growth. Your question can be, "How does sunlight affect plant growth?"
Use WPS AI to help when you get stuck. Feed it a topic, and it will come up with related questions to ask.
Step 2: Do Preliminary Research
Do some research to see what's already known about your topic. That way, you can build upon existing knowledge.
Research information in journals, books and credible websites. Then summarize what you read. This will help you formulate your hypothesis.
Step 3: Define Variables
Identify your variables:
Independent Variable: What you manipulate. For example, the amount of sun.
Dependent Variable: What you measure. For example, plant growth rate.
Clearly defining these makes your hypothesis specific and testable.
Step 4: State Your Hypothesis
State your question in the form of a hypothesis. Here are some examples:
If then: "If plants receive more sunlight, then they will grow faster."
Comparative statements: "Plants receiving more sunlight grow faster than plants receiving less."
Correlation statements: "There is positive correlation between sunlight and plant growth." This kind of pattern makes your hypothesis easy to test.
Step 5: Refine Your Hypothesis
Revise your hypothesis to be clear and specific, and elicit feedback to improve it.
You will also need a null hypothesis, which says that there is no effect or relationship between variables. An example would be, "Sunlight has no effect on the growth of plants."
With these steps, you are now bound to come up with a testable hypothesis. WPS AI can help you in this process more efficiently.
Characteristics of a Good Hypothesis
A good hypothesis is seen as the backbone of doing effective research. Following are some key characteristics that define a good hypothesis:
A good hypothesis has to be testable either by experimentation or observation. The hypothesis should clearly predict what can be measured or observed. For example, "If it receives more sunlight, the plant will grow taller" is a testable hypothesis since it states what can be measured.
Falsifiable
A hypothesis has to be falsifiable: it should be able to prove it wrong. This feature is important because it accommodates testing in science. For example, the statement "All swans are white" is falsifiable since it just takes one black swan to disprove the claim.
A good hypothesis should be grounded in current knowledge and should be properly reasoned. It should be broad or reasonable within existing knowledge. For example, "Increasing the amount of sunlight will boost plant growth" makes sense, in that it tallies with generally known facts about photosynthesis.
Specific and Clear
What is needed is clarity and specificity. A hypothesis has to be brief, yet free from ambiguity. For instance, "Increased sunlight leads to taller plants" is clear and specific whereas "Sunlight affects plants" is too vague.
Built upon Prior Knowledge
A good hypothesis is informed by prior research and existing theories. The available knowledge enlightens it to build on what is known to find new relationships or effects. For example, "Given photosynthesis requires sunlight, increasing sunlight will enhance plant growth" is informed by available scientific understanding.
Ethical Considerations
Finally, a good hypothesis needs to consider the ethics involved. The research should not bring damage to participants or the environment. For instance, "How the new drug will affect a human when tested without testing it on animals" may present an ethical concern.
Checklist for Reviewing Your Hypothesis
To be certain that your hypothesis has the following characteristics, use this checklist to review your hypothesis:
1. Is the hypothesis testable through experimentation or observation?
2. Can the hypothesis be proven false?
3. Is the hypothesis logically deduced from known facts?
4. Is your hypothesis clear and specific?
5. Does your hypothesis relate to previous research or theories?
6. Will there be any ethical issues with the proposed research?
7. Are your independent and dependent variables well defined?
8. Is your hypothesis concise and ambiguity free?
9. Did you get feedback to help in refining your hypothesis?
10. Does your hypothesis contain a null hypothesis for comparison?
By making sure that your hypothesis has these qualities, you are much more likely to set yourself on the course of higher-quality research and larger impacts. WPS AI can help fine-tune a hypothesis to ensure it is well-structured and clear.
Using WPS to Perfect your Hypothesis
Drafting a good hypothesis is the real inception of any research project. WPS AI, with its advanced language functions, can very strongly improve this stage of your study. Here's how WPS AI can help you perfect your hypothesis:
Check Grammar and Syntax
Grammar and punctuation errors can make your hypothesis weak. WPS AI checks and corrects this with the assurance that your hypothesis is as clear as possible and professional in its presentation. For example, when your hypothesis is written, "If the temperature increases then plant growth will increases", WPS AI can correct it to "If the temperature increases, then plant growth will increase."
Rewrite Your Hypothesis for Clarity
There needs to be a clear hypothesis. WPS AI can suggest ways to reword your hypothesis so that it makes sense. If your original hypothesis is, "More sunlight will result in more significant plant growth due to photosynthesis," WPS AI can suggest, "Increased sunlight will lead to greater plant growth through enhanced photosynthesis."
Automatic Content Expansion
Sometimes, your hypothesis or the related paragraphs may require more detail. WPS AI's [Continue Writing] feature can help enlarge the content. For example, after having written, "This study will examine the effects of sunlight on plant growth", using [Continue Writing] it can enlarge it to, "This research paper is going to study how sunlight affects the growth of plants by measuring their height and their health under different amounts of sunlight over a period of six weeks."
WPS AI is a great tool that can help you in drafting a good hypothesis for your research. It will help you check grammar, syntax, clarity, and completeness. Using WPS AI , you will be assured that the results of your hypothesis will be well-written and clear to understand.
What is the difference between a hypothesis and a theory?
The hypothesis is one single testable prediction regarding some phenomenon. The theory is an explanation for some part of the natural world which is well-substantiated by a body of evidence, together with multiple hypotheses.
What do I do if my hypothesis isn't supported by my data?
If your results turn out not to support your hypothesis, analyze the data again to see why your result rejects your hypothesis. Do not manipulate the observations or experiment so that it leads to your hypothesis.
Can there be more than one hypothesis in a research study?
Yes, there may be more than one hypothesis, especially when one research study is examining several interrelated phenomena or variables. Each hypothesis has to be separately and clearly stated and tested.
Correct formulation of a strong, testable hypothesis is one of the most critical steps in the application of the scientific method and within academic research. The steps provided in this article will help you write a hypothesis that is clear, specific, and based on available knowledge. Give the tools and tips a try to elevate your academic writing and kick your research up a notch.
- 1. How to Write a Cover Letter [Tips with Examples]
- 2. How to Write a Cover Letter for Teaching Positions [Tips with Examples]
- 3. How to Write a Bibliography [Tips with Examples]
- 4. How to Write a Call to Action - Steps with Examples
- 5. How to Write Modern Resume Examples Free 2022
- 6. How to Write a Book Review [Tips with Examples]

15 years of office industry experience, tech lover and copywriter. Follow me for product reviews, comparisons, and recommendations for new apps and software.

- Allergy & Immunology
- Anesthesiology
- Critical Care
- Dermatology
- Diabetes & Endocrinology
- Emergency Medicine
- Family Medicine
- Gastroenterology
- General Surgery
- Hematology - Oncology
- Hospital Medicine
- Infectious Diseases
- Internal Medicine
- Multispecialty
- Ob/Gyn & Women's Health
- Ophthalmology
- Orthopedics
- Pathology & Lab Medicine
- Plastic Surgery
- Public Health
- Pulmonary Medicine
- Rheumatology
- Transplantation
- Today on Medscape
- Business of Medicine
- Medical Lifestyle
- Science & Technology
- Medical Students
- Pharmacists
Vision Loss a New Dementia Risk Factor? What Do the Data Say?
Megan Brooks
August 15, 2024
In 2019, 57 million people worldwide were living with dementia, a figure expected to soar to 153 million by 2050. A recent Lancet Commission report suggests that nearly half of dementia cases could be prevented or delayed by addressing 14 modifiable risk factors, including impaired vision.
The report's authors recommend that vision-loss screening and treatment be universally available. But are these recommendations warranted? What is the evidence? What is the potential mechanism? And what are the potential implications for clinical practice?
Worldwide, the prevalence of avoidable vision loss and blindness in adults aged 50 years or older is estimated to hover around 13%.
"There is now overwhelming evidence that vision impairment in later life is associated with more rapid cognitive decline and an increased risk of dementia," Joshua Ehrlich, MD, MPH, associate professor in ophthalmology and visual sciences, the Institute for Social Research at the University of Michigan, Ann Arbor, told Medscape Medical News .
The evidence includes a meta-analysis of 14 prospective cohort studies with roughly 6.2 million older adults who were cognitively intact at baseline. Over the course of up to 14 years, 171,888 developed dementia. Vision loss was associated with a pooled relative risk (RR) for dementia of 1.47.
A separate meta-analysis also identified an increased risk for dementia (RR, 1.38) with visual loss. When broken down into different eye conditions, an increased dementia risk was associated with cataracts and diabetic retinopathy but not with glaucoma or age-related macular degeneration.
A US study that followed roughly 3000 older adults with cataracts and normal cognition at baseline for more than 20 years found that those who had cataract extraction had significantly reduced risk for dementia compared with those who did not have cataract extraction (hazard ratio, 0.71), after controlling for age, race, APOE genotype, education, smoking, and an extensive list of comorbidities.
Causation or Coincidence?
The mechanisms behind these associations might be related to underlying illness, such as diabetes, which is a risk factor for dementia; vision loss itself, as might be suggested by a possible effect of cataract surgery; or shared neuropathologic processes in the retina and the brain.
A longitudinal study from Korea that included roughly 6 million adults showed that dementia risk increased with severity of visual loss, which supports the hypothesis that vision loss in itself might be causal or that there is a dose-response effect to a shared causal factor.
Ehrlich told Medscape Medical News , "work is still needed to sort out" exactly how visual deficits may raise dementia risk, although several hypotheses exist.
For example, "decreased input to the brain via the visual pathways may directly induce brain changes. Also, consequences of vision loss, like social isolation, physical inactivity, and depression , are themselves risk factors for dementia and may explain the pathways through which vision impairment increases risk," he said.
Is the link causal? "We'll never know definitively because we can't randomize people to not get cataract surgery versus getting cataract surgery, because we know that improving vision improves quality of life, so we'd never want to do that. But the new evidence that's come in over the last 5 years or so is pretty promising," Esme Fuller-Thomson, PhD, director of the Institute for Life Course and Aging and professor, Department of Family and Community Medicine and Faculty of Nursing, at the University of Toronto, Ontario, Canada, told Medscape Medical News.
She noted that results of two studies that have looked at this "seem to indicate that those who have cataract surgery are not nearly as high risk of dementia of those who have cataracts but don't have the surgery. That's leaning towards causality."
A study published last month suggests that cataracts increase dementia risk through vascular and non– Alzheimer's disease mechanisms.
Clear Clinical Implications
Ehrlich told Medscape Medical News evidence for an association between untreated vision loss and dementia risk and potential modification by treatment has clear implications for care.
"Loss of vision impacts so many aspects of people's lives beyond just how they see the world and losing vision in later life is not a normal part of aging. Thus, when older adults experience vision loss, this should be a cause for concern and prompt an immediate referral to an eye care professional," he noted.
Fuller-Thomson agrees.
"Addressing vision loss will certainly help people see better and function at a higher level and improve quality of life, and it seems probable that it might decrease dementia risk so it's a win-win," she said.
In her own research, Fuller-Thomson has found that the combination of hearing loss and vision loss is linked to an eightfold increased risk for cognitive impairment.
"The idea is that vision and/or hearing loss makes it harder for you to be physically active, to be socially engaged, to be mentally stimulated. They are equally important in terms of social isolation, which could lead to loneliness, and we know that loneliness is not good for dementia," she said.
"With dual sensory impairment, you don't have as much information coming in — your brain is not engaged as much — and having an engaged brain, doing hobbies, having intellectually stimulating conversation, all of those are factors are associated with lowering risk of dementia," Fuller-Thomson said.
The latest Lancet Commission report noted that treatment for visual loss is "effective and cost-effective" for an estimated 90% of people. However, across the world, particularly in low- and middle-income countries, visual loss often goes untreated.
"A clear opportunity for dementia prevention exists with treatment of visual loss," the report concluded.
Ehrlich and Fuller-Thomson have no relevant conflicts of interest.
Send comments and news tips to [email protected] .
TOP PICKS FOR YOU
- Perspective
- Drugs & Diseases
- Global Coverage
- Additional Resources
- Vision Screening at Well-Child Visits Cost-Effective for Detecting Amblyopia
- 'Tunable' Lenses Offer New Way to Correct Presbyopia
- Primary Care Physician's Next Frontier: Palliative Care
- news How to Safely Discontinue Multiple Myeloma Maintenance Care
- news Primary Care Vision Testing Rates in Children Low
- news Vision Impairment Tied to Isolation, Depression
- news Semaglutide Linked to Cause of Vision Loss
- Inherited Retinal Diseases: Early Signs and Advances in Treatment
- Treating Exudative or Wet Age-Related Macular Degeneration
- Fast Five Quiz: Can You Properly Address Cataracts?
- Fast Five Quiz: Type 2 Diabetes Key Aspects
- Optimizing Prognosis and Treatment Outcomes in Exudative or Wet Age-Related Macular Degeneration
- Fast Five Quiz: Exudative (Wet) Age-Related Macular Degeneration Presentation and Diagnosis
- Fighting Vision Loss With Food
- How to Safely Discontinue Multiple Myeloma Maintenance Care
- Primary Care Vision Testing Rates in Children Low
- Vision Impairment Tied to Isolation, Depression

Title Page Setup
A title page is required for all APA Style papers. There are both student and professional versions of the title page. Students should use the student version of the title page unless their instructor or institution has requested they use the professional version. APA provides a student title page guide (PDF, 199KB) to assist students in creating their title pages.
Student title page
The student title page includes the paper title, author names (the byline), author affiliation, course number and name for which the paper is being submitted, instructor name, assignment due date, and page number, as shown in this example.
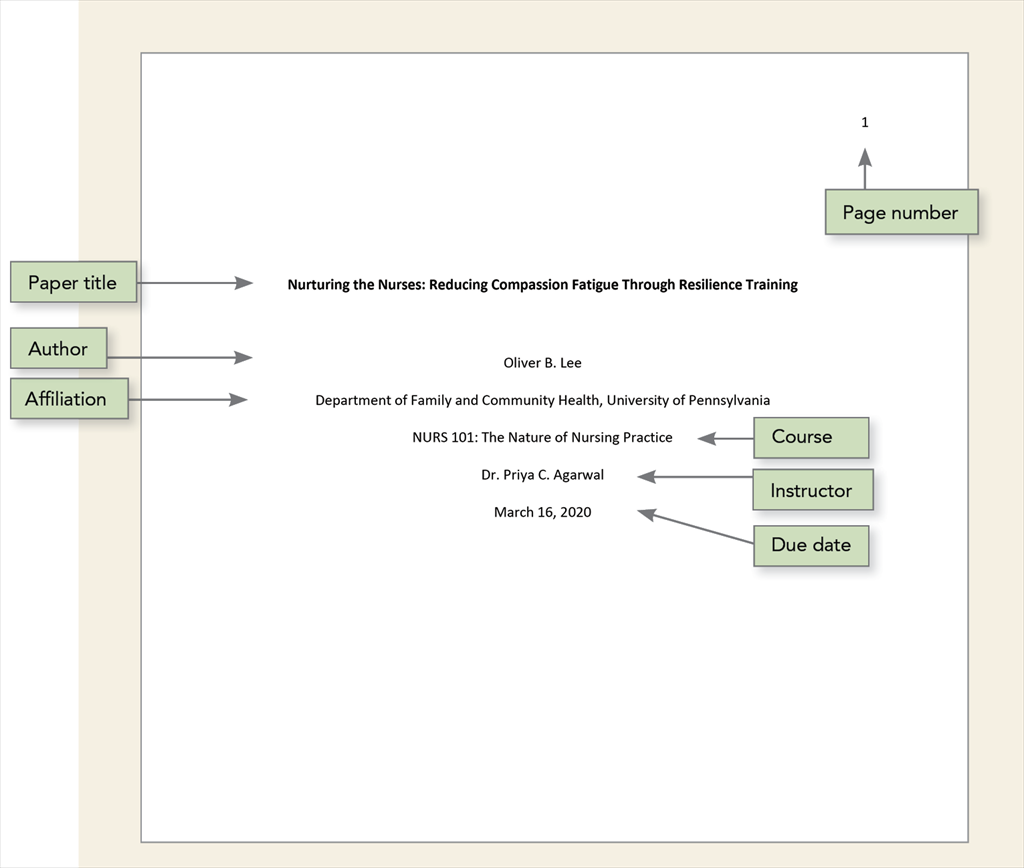
Title page setup is covered in the seventh edition APA Style manuals in the Publication Manual Section 2.3 and the Concise Guide Section 1.6
Related handouts
- Student Title Page Guide (PDF, 263KB)
- Student Paper Setup Guide (PDF, 3MB)
Student papers do not include a running head unless requested by the instructor or institution.
Follow the guidelines described next to format each element of the student title page.
|
|
|
|
|---|---|---|
| Paper title | Place the title three to four lines down from the top of the title page. Center it and type it in bold font. Capitalize of the title. Place the main title and any subtitle on separate double-spaced lines if desired. There is no maximum length for titles; however, keep titles focused and include key terms. |
|
| Author names | Place one double-spaced blank line between the paper title and the author names. Center author names on their own line. If there are two authors, use the word “and” between authors; if there are three or more authors, place a comma between author names and use the word “and” before the final author name. | Cecily J. Sinclair and Adam Gonzaga |
| Author affiliation | For a student paper, the affiliation is the institution where the student attends school. Include both the name of any department and the name of the college, university, or other institution, separated by a comma. Center the affiliation on the next double-spaced line after the author name(s). | Department of Psychology, University of Georgia |
| Course number and name | Provide the course number as shown on instructional materials, followed by a colon and the course name. Center the course number and name on the next double-spaced line after the author affiliation. | PSY 201: Introduction to Psychology |
| Instructor name | Provide the name of the instructor for the course using the format shown on instructional materials. Center the instructor name on the next double-spaced line after the course number and name. | Dr. Rowan J. Estes |
| Assignment due date | Provide the due date for the assignment. Center the due date on the next double-spaced line after the instructor name. Use the date format commonly used in your country. | October 18, 2020 |
|
| Use the page number 1 on the title page. Use the automatic page-numbering function of your word processing program to insert page numbers in the top right corner of the page header. | 1 |
Professional title page
The professional title page includes the paper title, author names (the byline), author affiliation(s), author note, running head, and page number, as shown in the following example.
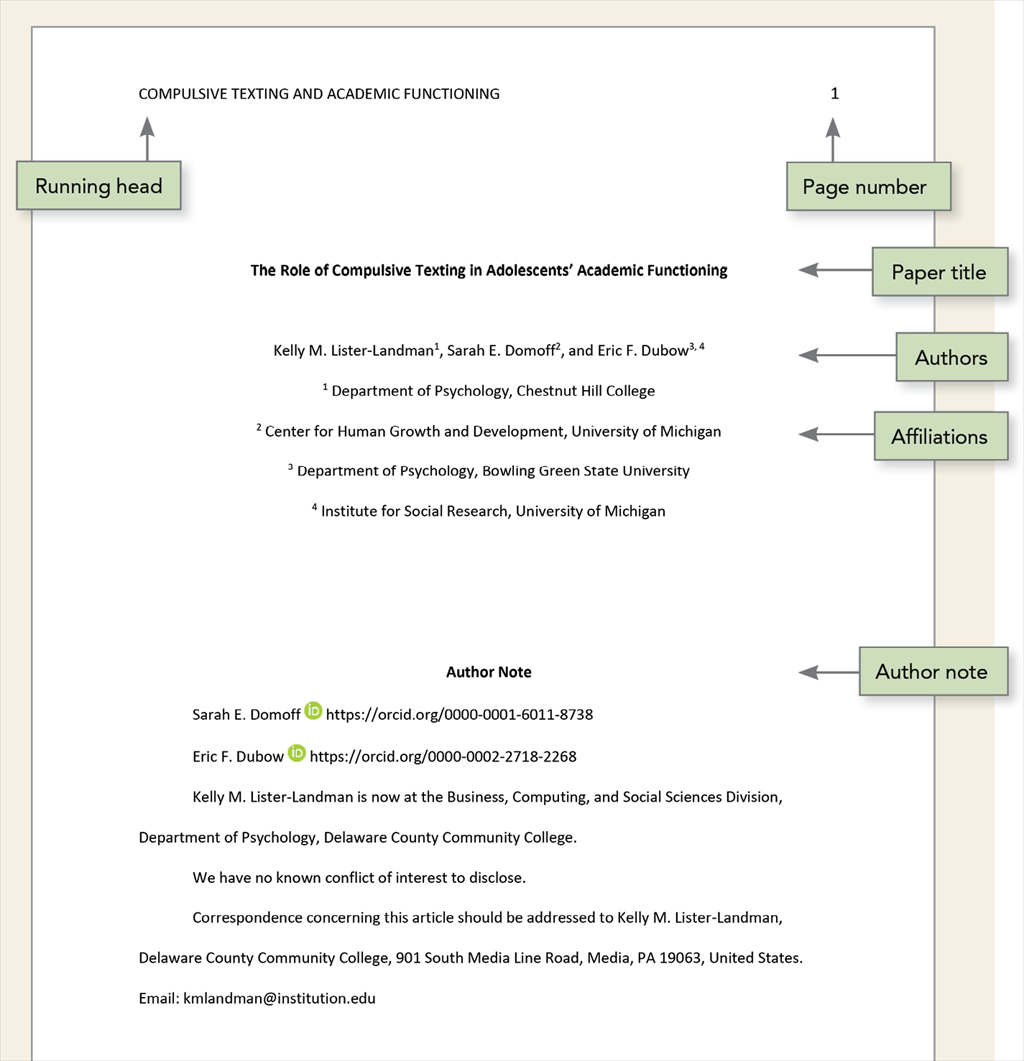
Follow the guidelines described next to format each element of the professional title page.
|
|
|
|
|---|---|---|
| Paper title | Place the title three to four lines down from the top of the title page. Center it and type it in bold font. Capitalize of the title. Place the main title and any subtitle on separate double-spaced lines if desired. There is no maximum length for titles; however, keep titles focused and include key terms. |
|
| Author names
| Place one double-spaced blank line between the paper title and the author names. Center author names on their own line. If there are two authors, use the word “and” between authors; if there are three or more authors, place a comma between author names and use the word “and” before the final author name. | Francesca Humboldt |
| When different authors have different affiliations, use superscript numerals after author names to connect the names to the appropriate affiliation(s). If all authors have the same affiliation, superscript numerals are not used (see Section 2.3 of the for more on how to set up bylines and affiliations). | Tracy Reuter , Arielle Borovsky , and Casey Lew-Williams | |
| Author affiliation
| For a professional paper, the affiliation is the institution at which the research was conducted. Include both the name of any department and the name of the college, university, or other institution, separated by a comma. Center the affiliation on the next double-spaced line after the author names; when there are multiple affiliations, center each affiliation on its own line.
| Department of Nursing, Morrigan University |
| When different authors have different affiliations, use superscript numerals before affiliations to connect the affiliations to the appropriate author(s). Do not use superscript numerals if all authors share the same affiliations (see Section 2.3 of the for more). | Department of Psychology, Princeton University | |
| Author note | Place the author note in the bottom half of the title page. Center and bold the label “Author Note.” Align the paragraphs of the author note to the left. For further information on the contents of the author note, see Section 2.7 of the . | n/a |
|
| The running head appears in all-capital letters in the page header of all pages, including the title page. Align the running head to the left margin. Do not use the label “Running head:” before the running head. | Prediction errors support children’s word learning |
|
| Use the page number 1 on the title page. Use the automatic page-numbering function of your word processing program to insert page numbers in the top right corner of the page header. | 1 |
Antibodies From Long COVID Patients Provide Clues to Autoimmunity Hypothesis
BY ISABELLA BACKMAN August 5, 2024

Promising new research supports that autoimmunity—in which the immune system targets its own body—may contribute to Long COVID symptoms in some patients.
As covered previously in this blog, researchers have several hypotheses to explain what causes Long COVID, including lingering viral remnants, the reactivation of latent viruses, tissue damage, and autoimmunity.
Now, in a recent study , when researchers gave healthy mice antibodies from patients with Long COVID, some of the animals began showing Long COVID symptoms—specifically heightened pain sensitivity and dizziness. It is among the first studies to offer enticing evidence for the autoimmunity hypothesis. The research was led by Akiko Iwasaki, PhD , Sterling Professor of Immunobiology at Yale School of Medicine (YSM).
“We believe this is a big step forward in trying to understand and provide treatment to patients with this subset of Long COVID,” Iwasaki said.
Iwasaki zeroed in on autoimmunity in this study for several reasons. First, Long COVID’s persistent nature suggested that a chronic triggering of the immune system might be at play. Second, women between ages 30 and 50, who are most susceptible to autoimmune diseases, are also at a heightened risk for Long COVID. Finally, some of Iwasaki’s previous research had detected heightened levels of antibodies in people infected with SARS-CoV-2.
Mice given antibodies show signs of Long COVID symptoms
Iwasaki’s team isolated antibodies from blood samples obtained from the Mount Sinai-Yale Long COVID study . They transferred these antibodies into mice and then conducted multiple experiments designed to look for changes in behavior that may indicate the presence of specific symptoms. For many of these experiments, mice that received antibodies [the experimental group] behaved no differently than mice that had not [the control group].
However, a few experiments revealed striking changes in the behavior of the experimental mice. These included:
- Pain sensitivity test: Some experimental mice were quicker to react after being placed on a heated plate.
- Coordination and balance test: Some experimental mice struggled to balance on a rotarod (rotating rod) compared to control mice.
- Grip strength test: Some of the experimental mice applied less force with their paws.
Among the mice that showed behavioral changes, the researchers identified which patients their antibodies came from and what symptoms they had experienced. Interestingly, of the mice that showed heightened pain, 85% received antibodies from patients that reported pain as one of their Long COVID symptoms. Additionally, 89% of mice that had demonstrated loss of balance and coordination on the rotarod test had received antibodies from patients who reported dizziness. Furthermore, 91% of mice that showed reduced strength and muscle weakness received antibodies from patients who reported headache and 55% from patients who reported tinnitus. More research is needed to better understand this correlation.
The autoimmunity hypothesis has recently been further supported by a research group in the Netherlands led by Jeroen den Dunnen, DRS , associate professor at Amsterdam University Medical Center, which also found a link between patients’ Long COVID antibodies and corresponding symptoms in mice.
Treatments for autoimmunity may help some Long COVID patients
Diagnosing and treating Long COVID requires doctors to understand what causes the disease. The new study suggests that treatments targeting autoimmunity, such as B cell depletion therapy or plasmapheresis, might alleviate symptoms in some patients by removing the disease-causing antibodies.
Intravenous immunoglobulin (IVIg) is another therapy used for treating autoimmune diseases like lupus in which patients receive antibodies from healthy donors. While its exact mechanism is still unclear, the treatment can help modulate the immune system and reduce inflammation. Could this treatment help cases of Long COVID that are caused by autoimmunity?
A 2024 study led by Lindsey McAlpine, MD , instructor at YSM and first author, and Serena Spudich, MD , Gilbert H. Glaser Professor of Neurology at YSM and principal investigator, found that IVIg might help improve small fiber neuropathy—a condition associated with numbness or painful sensations in the hands and feet—caused by Long COVID. Iwasaki is hopeful that future clinical trials might reveal the benefits of this treatment in helping some of the other painful symptoms of the diseases.
Other drugs are also in the pipeline, such as FcRn inhibitors. FcRn is a receptor that binds to antibodies and recycles them. Blocking this receptor could help bring down levels of circulating antibodies in the blood. An FcRn receptor was recently approved by the FDA for treating myasthenia gravis, another kind of autoimmune disease.
The study could also help researchers create diagnostic tools for evaluating which patients have Long COVID induced by autoimmunity so that doctors can identify who is most likely to benefit from treatments such as these.
Iwasaki plans to continue researching why and how autoantibodies might cause Long COVID, as well as conduct randomized clinical trials on promising treatments. She is also conducting similar antibody transfer studies in other post-acute infection syndromes, such as myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS).
In the meantime, she is excited about her team’s promising results. “Seeing this one-to-one correlation of antibodies that cause pain from patients who reported pain is really gratifying to me as it suggests a causal link,” she says. “It’s a first step, but I think it’s a big one.”
Isabella Backman is associate editor and writer at Yale School of Medicine.
The last word by Lisa Sanders, MD:
I am very excited by this research, which suggests that at least some of the symptoms of Long COVID are driven by autoimmunity. If so, then this suggests that there may be a way to test for some versions of Long COVID. And if we could identify the patients who have an autoimmune-driven disease, we have treatments to try that have been used with success in other autoimmune diseases. Many of the autoimmune diseases are treated with medications that suppress the immune system. These are powerful medicines that can leave an individual at risk for infection, so they must be thoughtfully applied to patients with evidence of immune system involvement.
I feel as though every blog post here ends with the possibility of better testing and better treatment, but what makes this different is that it points in a very specific direction and leads to the kind of specific questions that help get to useful answers. Which antibodies are involved? Which cells? And finally, can we develop treatments that are specific to those antibodies or to their targets? These are exciting questions, which will, I hope, lead to useful answers.
Read other installments of Long COVID Dispatches here .
If you’d like to share your experience with Long COVID for possible use in a future post (under a pseudonym), write to us at: [email protected]
Information provided in Yale Medicine content is for general informational purposes only. It should never be used as a substitute for medical advice from your doctor or other qualified clinician. Always seek the individual advice of your health care provider for any questions you have regarding a medical condition.
More news from Yale Medicine

College of Nursing and Health Innovation
- Academic Programs
- Alumni & Giving
News & Events
- Student Resources
- Request Information
Graduate Nursing Students Embark on an Educational Journey to Switzerland and France
Wednesday, Aug 14, 2024

This summer, Graduate Nursing students from multiple MSN and DNP programs had the unique opportunity to expand their horizons and deepen their understanding of healthcare through a study abroad trip to Switzerland and France. The weeklong trip was part of a Spring 2024 elective course.
The trip focused on experiential learning, allowing students to apply their classroom knowledge in real-world settings and engage with healthcare professionals from around the globe.
Highlights of the Trip included:
-United Nations Visit: CONHI students attended a United Nations meeting focused on the human rights of indigenous peoples from around the world. This session provided an eye-opening perspective on global health issues and human rights advocacy.
-Red Cross Museum and World Health Organization Tour: The students toured the Red Cross Museum and the World Health Organization, gaining insights into the history and current efforts in global health and humanitarian work.
-University of Geneva: During their visit to the University of Geneva, the students had the privilege of meeting with Professors Catherine Ludwig and Alexia Bourgeois. These discussions enriched their understanding of international healthcare systems and academic collaborations.
-Médecins Sans Frontières Lecture: A lecture from Médecins Sans Frontières (Doctors Without Borders) offered students a deeper understanding of global health crises and the critical role of emergency medical response.
-Air Glacier Complex Tour: The tour of the Air Glacier complex was a highlight, where students learned about air mountain rescues and trauma care. This hands-on experience demonstrated the challenges and innovations in emergency medical services in rural mountainous regions.
-Cultural Immersion: In addition to the educational components, students immersed themselves in the rich cultures of Switzerland and France, experiencing local traditions, cuisine, and history.
The trip provided graduate nursing students with unparalleled opportunities to apply theoretical knowledge in real-world settings, network with international healthcare professionals, and ultimately, gain a global perspective on nursing and healthcare.
Looking Forward

Study abroad travel plans for 2025 are already in the works, including a spring break trip to Italy. Graduate nursing students interested in participating are encouraged to keep an eye out for additional information.
- Recent News
- Dream Makers
- Publications
- Share Your Story
411 S. Nedderman Drive Box 19407, Arlington, Texas 76019-0407 P: 817-272-2776 | F: 817-272-5006
- Request Info

IMAGES
COMMENTS
Issues of Concern Without a foundational understanding of hypothesis testing, p values, confidence intervals, and the difference between statistical and clinical significance, it may affect healthcare providers' ability to make clinical decisions without relying purely on the research investigators deemed level of significance. Therefore, an overview of these concepts is provided to allow ...
Developing a research problem and hypothesis: Nursing Videos, Flashcards, High Yield Notes, & Practice Questions. Learn and reinforce your understanding of Developing a research problem and hypothesis: Nursing.
The development of research questions and the subsequent hypotheses are prerequisites to defining the main research purpose and specific objectives of a study. Consequently, these objectives determine the study design and research outcome. The development ...
A research hypothesis is an assumption or a tentative explanation for a specific process observed during research. Unlike a guess, research hypothesis is a calculated, educated guess proven or disproven through research methods.
A research hypothesis (also called a scientific hypothesis) is a statement about the expected outcome of a study (for example, a dissertation or thesis). To constitute a quality hypothesis, the statement needs to have three attributes - specificity, clarity and testability.
HYPOTHESIS TESTING. A clinical trial begins with an assumption or belief, and then proceeds to either prove or disprove this assumption. In statistical terms, this belief or assumption is known as a hypothesis. Counterintuitively, what the researcher believes in (or is trying to prove) is called the "alternate" hypothesis, and the opposite ...
A hypothesis is a statement that can be tested by scientific research. If you want to test a relationship between two or more variables, you need to write hypotheses before you start your experiment or data collection.
Abstract Editor's note: This is the 16th article in a series on clinical research by nurses. The series is designed to be used as a resource for nurses to understand the concepts and principles essential to research. Each column will present the concepts that underpin evidence-based practice—from research design to data interpretation.
Editor's note: This is the 16th article in a series on clinical research by nurses. The series is designed to be used as a resource for nurses to understand the concepts and principles essential to research. Each column will present the concepts that underpin evidence-based practice-from research de …
The research/clinical question is in the "background" planning phases of research projects. Meaning, the eventual hypothesis is developed from the research question and/or statement of purpose after a literature review is performed to determine what evidence already exists and establishing the research problem. Hot Tip!
In every study, researchers put forth two kinds of hypotheses: the research or alternative hypothesis and the null hypothesis. The research hypothesis reflects what the researchers hope to show—that there is a difference between the experimental group and the control group. The null hypothesis directly competes with the research hypothesis.
The research question should address a relevant issue in the nursing field and reflect your aim to add to the body of nursing science. A hypothesis is an accurate prediction of the relationship of the variables in your research question.
A hypothesis (from the Greek, foundation) is a logical construct, interposed between a problem and its solution, which represents a proposed answer to a research question. It gives direction to the investigator's thinking about the problem and, therefore, facilitates a solution. Unlike facts and assumptions (presumed true and, therefore, not ...
The focus of this inaugural column is how to start the research process, which involves the identification of the topic of interest and the development of a well-defined research question. This article also discusses how to formulate quantitative and qualitative research questions.
Hypothesis. • A hypothesis is a formal statement of the expected relationship between two or more variables in a specified population. • The hypothesis translates the research problem and purpose into a clear explanation or prediction of the expected results or outcomes of the study.
Abstract. HYPOTHESIS TESTING IS the process of making a choice between two conflicting hypotheses. The null hypothesis, H 0, is a statistical proposition stating that there is no significant difference between a hypothesized value of a population parameter and its value estimated from a sample drawn from that population.
Further research is needed to identify the factors that influence the conduction of research with hypothesis testing. Conclusion: Hypothesis testing in nursing research showed a steady decline from the 1980s to 1990s. Research purposes of explanation, and prediction/ control increased the likelihood of hypothesis testing.
A hypothesis is a statement of the researcher's expectation or prediction about relationship among study variables. The research process begins and ends with the hypothesis.
Nurses play an increasingly active role in clinical research in IBD. By reviewing existing literature on the topic, this chapter provides a brief overview of some main concepts related to research in nursing. In addition, the chapter provides some general advice in...
Figures Process of formulating the hypothesis Hypothesis a forerunner for a research problem and many a times is encircled as an enquiry or question.
A hypothesis is a statement of the researcher's expectation or prediction about relationship among study variables. The research process begins and ends with the hypothesis.
Definition of Nursing Research Nursing research develops knowledge about health and the promotion of health over the full lifespan, care of persons with health problems and disabilities, and nursing actions to enhance the ability of individuals to respond effectively to actual or potential health problems.
Learn how to formulate a good, testable hypothesis for your research paper or science project, with real examples and practical advice. Enhance your academic writing with WPS AI.
About the University of Miami School of Nursing and Health Studies: The University of Miami School of Nursing and Health Studies (SONHS) transforms lives and health care through education, research, innovation, and service across the hemisphere. Established in 1948 as South Florida's first collegiate nursing program, SONHS is a world-class ...
A longitudinal study from Korea that included roughly 6 million adults showed that dementia risk increased with severity of visual loss, which supports the hypothesis that vision loss in itself ...
Employing novel high-frequency data we examine what effect the absence of nursing staff has on inpatient mortality and other outcomes associated with nursing care. We find significant adverse mortality impacts of shortages of nurses with degree-level qualifications but no effect of shortages of less qualified nursing assistants.
The student title page includes the paper title, author names (the byline), author affiliation, course number and name for which the paper is being submitted, instructor name, assignment due date, and page number, as shown in this example.
The autoimmunity hypothesis has recently been further supported by a research group in the Netherlands led by Jeroen den Dunnen, DRS, associate professor at Amsterdam University Medical Center, which also found a link between patients' Long COVID antibodies and corresponding symptoms in mice.
Additionally, it has the No. 1-ranked nursing B.S.N program in Florida in 2024, according to U.S. News & World Report. The mom and daughter got the chance to enjoy the unusual moment because Albanese-O'Neill is a College of Nursing Alumni Council member. The council hosts the pinning ceremonies and members historically pin the graduates.
This summer, Graduate Nursing students from multiple MSN and DNP programs had the unique opportunity to expand their horizons and deepen their understanding of healthcare.